Published online Dec 26, 2021. doi: 10.12998/wjcc.v9.i36.11400
Peer-review started: June 13, 2021
First decision: June 25, 2021
Revised: June 29, 2021
Accepted: November 15, 2021
Article in press: November 15, 2021
Published online: December 26, 2021
Processing time: 192 Days and 22.3 Hours
Acute appendicitis with mesenteric vein thrombosis (MVT) is an uncommon condition and usually lacks specific clinical manifestations, which leads to a high rate of misdiagnosis or delayed diagnosis, especially when it is accompanied by other abdominal diseases. Prompt and accurate recognition is vital for treatment and prognosis.
A 37-year-old woman had a history of acute metastatic right lower abdominal pain, nausea, and fever. A contrast-enhanced computed tomography (CT) scan showed a filling defect in the mesenteric vessels. The patient was diagnosed with acute appendicitis complicated by MVT and was treated with anticoagulation and intravenous antibiotics. The follow-up CT scan showed full resolution of the thrombosis and inflammation.
Clinical awareness is essential for recognizing MVT, especially when it is accompanied by other common acute abdominal diseases, such as acute appendicitis. Contrast-enhanced CT is helpful for the diagnosis of MVT and is recommended for patients with acute abdominal diseases.
Core Tip: The article presents an uncommon clinical case of mesenteric vein thrombosis (MVT) complicated by acute appendicitis in a patient with no obvious risk factors for thrombosis. The patient was diagnosed correctly at an early stage and finally recovered after receiving anticoagulation and antibiotics. MVT is rare and difficult to recognize when it occurs with other acute abdominal diseases. Contrast-enhanced computed tomography is vital to its diagnosis. Therefore, clinicians should fully consider the possibility of this disease when treating patients with acute abdominal diseases and use appropriate diagnostic tests.
- Citation: Yang F, Guo XC, Rao XL, Sun L, Xu L. Acute appendicitis complicated by mesenteric vein thrombosis: A case report. World J Clin Cases 2021; 9(36): 11400-11405
- URL: https://www.wjgnet.com/2307-8960/full/v9/i36/11400.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v9.i36.11400
Acute appendicitis is common in emergency departments but is rarely accompanied by mesenteric vein thrombosis (MVT). Numerous retrospective studies have revealed that acute MVT accounts for approximately 2%-10% of the total number of acute intestinal ischemia cases. The incidence rate in Europe and the United States is approximately 0.1%. Risk factors usually include tumors, infection, thrombosis history, inflammatory bowel disease, thrombophilia, cirrhosis, etc. Pathogenic factors comprise any conditions that may cause vascular endothelial injury, blood flow obstruction, or hypercoagulability[1]. MVT is more frequent in elderly individuals, although it could still happen in the young. The prognosis largely depends on prompt detection and intervention, while delayed diagnosis and treatment may lead to serious consequences, with mortality rates as high as 60%-80%[2]. The outcome of early simple acute appendicitis is good, but the presence of MVT poses an increased likelihood of adverse outcomes, such as intestinal necrosis, septic shock, or short bowel syndrome. MVT lacks specific clinical and laboratory manifestations in the early stage. The application of contrast-enhanced computed tomography (CT) can greatly improve the recognition of MVT and reduce the mortality of this disease[3].
A 37-year-old woman was admitted to the emergency department due to metastatic right lower abdominal pain, fever, and nausea present for 4 d.
The patient developed pain around the belly button 4 d ago, and the pain migrated to the right lower abdominal pain within 1 d with concomitant fever and nausea.
The patient had been treated with levofloxacin for acute gastroenteritis for 3 d prior but still had not improved.
The patient had no special history.
The patient's vital signs were normal, and the only discovery was tenderness of the right McBurney's point.
The laboratory tests performed on the day that the patient was admitted showed an increased neutrophil count of 13.11 × 109/L and a decreased platelet count of 73 × 109/L; the fibrin-degradation-product and D-dimer levels were slightly higher.
A plain CT scan was routinely performed and suggested appendicitis with adjacent peritonitis. The radiologist suspected mesenteric ischemia and consequently scheduled the patient to receive contrast-enhanced CT, from which we noticed that the embolus was probably blocking the ileocolic vein.
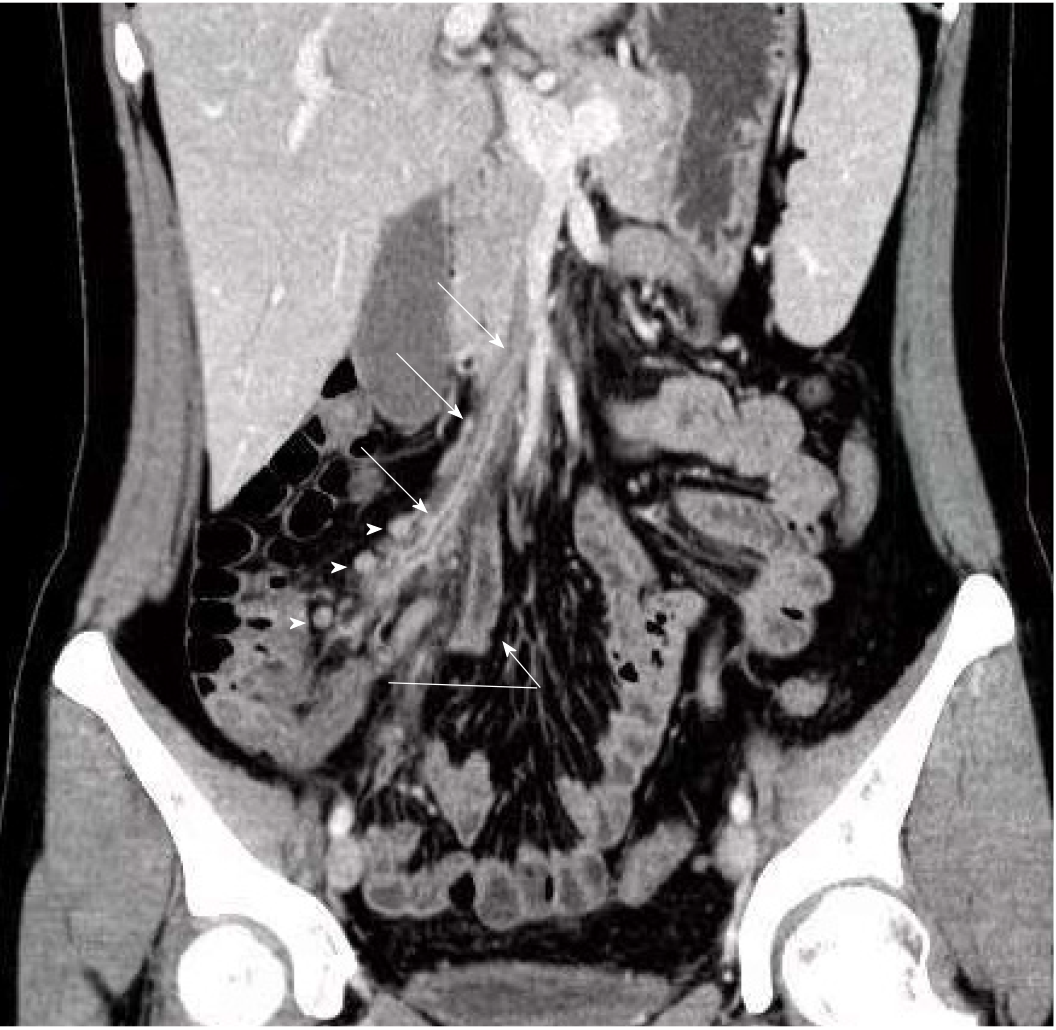
Subsequently, the patient underwent another CT scan on the sixth day in the hospital, and the images showed less severe inflammation and exudation than before; however, the thrombus was still present in her ileocolic vein (Figure 1).
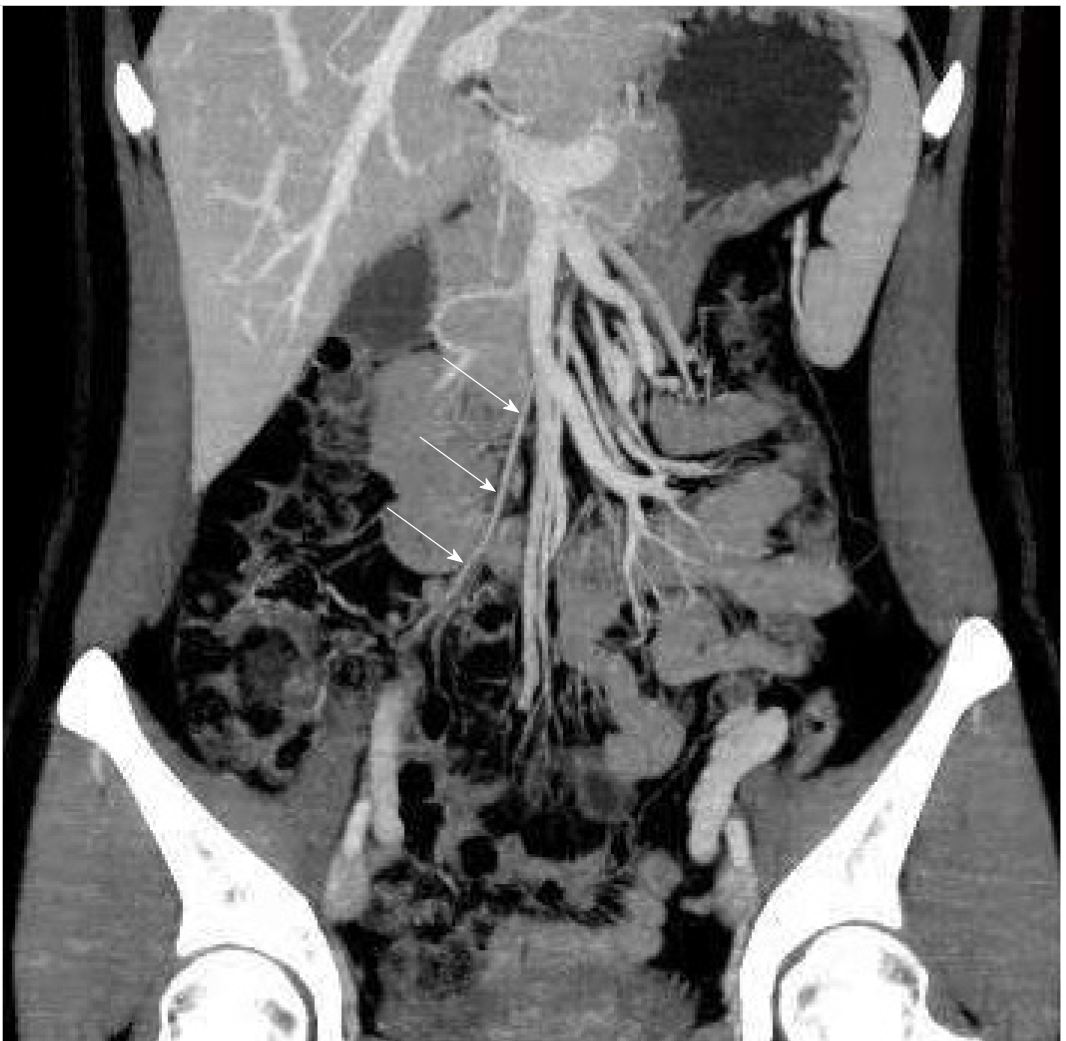
One month after discharge from the hospital, the patient received another CT scan (Figure 2), which showed that the inflammation and the embolized ileocolic vein had both resolved.
The final diagnosis of the presented case was acute appendicitis complicated by MVT.
After admission, the patient received antibiotics and low-molecular-weight heparin (LMWH) as well as underwent fasting. Her temperature returned to normal on the second day, and her abdominal pain was relieved. The only complaint was a small amount of reddish-brown broken tissue excreted in her stool. Considering that the CT scan on her sixth day in the hospital showed a better result, she was allowed to gradually return to a regular diet on the seventh day, then placed on oral rivaroxaban instead of LMWH injection and finally discharged from the hospital on the tenth day.
The physician instructed the patient to stop rivaroxaban 3 d after discharge from the hospital and to receive another CT scan 1 mo later (Figure 2); this scan showed that the inflammation and the embolized ileocolic vein had both resolved. In subsequent follow-up to date, the patient has not complained of any other discomfort.
We present a female patient with no significant risk factors or history predisposing to thrombosis. She had a good prognosis after anticoagulation therapy due to accurate diagnosis by contrast-enhanced CT. MVT is rare, and its cause is not clear. Although patients may have a variety of possible pathogenic factors or none of the risk factors, approximately 75% of these patients with MVT have identifiable potential etiologic factors[4]. Other similar cases that have been reported suggest that acute appendicitis may induce MVT by causing local blood hypercoagulability, mesenteric phlebitis, or mesenteric perivascular inflammation, among others[5,6]. Since our case did not undergo surgery, we were unable to obtain a pathological diagnosis. However, the CT scan showed that the appendix and mesenteric perivascular inflammation occurred during the onset of the disease. The other CT scan 1 mo after the onset of illness indicated that the involved vein was completely occluded and that collateral circulation was established. Thus, we consider that the angiitis and periphlebitis could both play a major role in our case.
Acute MVT can happen at any age, though it is more common among elderly patients. Nonspecific gastrointestinal symptoms such as abdominal pain and nausea are often the only manifestation, and peritonitis or shock usually suggest advanced illness[7]. Although classic “pain out of proportion to examination” symptoms are typical, MVT does not have specific manifestations. Difficulties in diagnosis at the early stage will lead to delayed treatment and cause severe sequelae, especially in cases of MVT complicated with other acute abdominal diseases. Laboratory tests are usually not helpful for a definitive diagnosis, as the usual finding is an increased white blood cell count, which is not specific. Some patients can exhibit acidosis and increased blood lactic acid, which generally suggests a late stage[7-9]. In recent decades, contrast-enhanced CT has gradually become the preferred test in the diagnosis of ischemic bowel disease. Ischemic bowel disease has been increasingly recognized with the widespread use of CT technology[2,10]. Other examination tools, such as angiography and magnetic resonance venous imaging, are often too time-consuming or invasive and are rarely used clinically[11]. The specific manifestation of MVT on CT imaging consists of venous filling defects, while nonspecific changes include abnormal or decreased intestinal-wall enhancement, intestinal-wall thickening or gas accumulation, etc, which are difficult to identify. However, some studies have shown that if clinicians suspect ischemic bowel disease, imaging can help identify this condition, which may reduce the rate of surgery[12].
Treatment of MVT mainly depends on the disease progression. For early-stage patients (especially those with acute thromboembolism), systemic anticoagulation, including LMWH and oral anticoagulants, is the most basic therapy. If treated promptly, the thrombus can disappear completely. However, interventional therapy and surgery are inescapable options for advanced patients or those with a poor response to conservative treatment[1,2,9,13]. There are no guidelines for the application of antibiotics in ischemic bowel disease. Ischemic bowel diseases such as MVT destroy the integrity of the intestinal mucosal barrier and cause translocation of intestinal flora at an early stage[14]. Therefore, broad-spectrum antibiotics (such as third-generation cephalosporins combined with antianaerobic drugs) are recommended to be administered as soon as possible. For patients with infectious complications such as appendicitis, antibiotics are definitely necessary.
MVT is an uncommon but possible complication of acute appendicitis and can lead to severe sequelae. Enhanced-contrast CT scans are essential for avoiding misdiagnosis of suspected MVT patients. Therefore, clinicians must have an awareness of and concern about MVT. Although they have more limitations than plain CT scans, enhanced-contrast CT scans are critical and sometimes inevitable in emergency departments.
Provenance and peer review: Unsolicited article; Externally peer reviewed.
Peer-review model: Single blind
Specialty type: Medicine, research and experimental
Country/Territory of origin: China
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): B
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Surani S, Yoshizawa T S-Editor: Wang JJ L-Editor: Wang TQ P-Editor: Wang JJ
| 1. | Singal AK, Kamath PS, Tefferi A. Mesenteric venous thrombosis. Mayo Clin Proc. 2013;88:285-294. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 136] [Cited by in RCA: 120] [Article Influence: 10.0] [Reference Citation Analysis (0)] |
| 2. | Clair DG, Beach JM. Mesenteric Ischemia. N Engl J Med. 2016;374:959-968. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 312] [Cited by in RCA: 327] [Article Influence: 36.3] [Reference Citation Analysis (1)] |
| 3. | Copin P, Zins M, Nuzzo A, Purcell Y, Beranger-Gibert S, Maggiori L, Corcos O, Vilgrain V, Ronot M. Acute mesenteric ischemia: A critical role for the radiologist. Diagn Interv Imaging. 2018;99:123-134. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 21] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 4. | Beckermann J, Walker A, Grewe B, Appel A, Manz J. Mesenteric venous thrombosis complicating acute appendicitis: A case series. Int J Surg Case Rep. 2020;73:100-104. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 2] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 5. | Takehara K, Miyano S, Machida M, Kitabatake T, Fujisawa M, Kojima K. Superior mesenteric vein thrombosis as a complication of acute appendicitis : report of a case. Clin J Gastroenterol. 2013;6:269-273. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9] [Cited by in RCA: 8] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 6. | Chang YS, Min SY, Joo SH, Lee SH. Septic thrombophlebitis of the porto-mesenteric veins as a complication of acute appendicitis. World J Gastroenterol. 2008;14:4580-4582. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 40] [Cited by in RCA: 34] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 7. | Tilsed JV, Casamassima A, Kurihara H, Mariani D, Martinez I, Pereira J, Ponchietti L, Shamiyeh A, Al-Ayoubi F, Barco LA, Ceolin M, D'Almeida AJ, Hilario S, Olavarria AL, Ozmen MM, Pinheiro LF, Poeze M, Triantos G, Fuentes FT, Sierra SU, Soreide K, Yanar H. ESTES guidelines: acute mesenteric ischaemia. Eur J Trauma Emerg Surg. 2016;42:253-270. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 202] [Cited by in RCA: 201] [Article Influence: 22.3] [Reference Citation Analysis (0)] |
| 8. | Dewitte A, Biais M, Coquin J, Fleureau C, Cassinotto C, Ouattara A, Janvier G. [Diagnosis and management of acute mesenteric ischemia]. Ann Fr Anesth Reanim. 2011;30:410-420. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 15] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 9. | Bala M, Kashuk J, Moore EE, Kluger Y, Biffl W, Gomes CA, Ben-Ishay O, Rubinstein C, Balogh ZJ, Civil I, Coccolini F, Leppaniemi A, Peitzman A, Ansaloni L, Sugrue M, Sartelli M, Di Saverio S, Fraga GP, Catena F. Acute mesenteric ischemia: guidelines of the World Society of Emergency Surgery. World J Emerg Surg. 2017;12:38. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 242] [Cited by in RCA: 299] [Article Influence: 37.4] [Reference Citation Analysis (0)] |
| 10. | Kärkkäinen JM, Acosta S. Acute mesenteric ischemia (part I) - Incidence, etiologies, and how to improve early diagnosis. Best Pract Res Clin Gastroenterol. 2017;31:15-25. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 84] [Cited by in RCA: 86] [Article Influence: 10.8] [Reference Citation Analysis (0)] |
| 11. | Russell CE, Wadhera RK, Piazza G. Mesenteric venous thrombosis. Circulation. 2015;131:1599-1603. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 39] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 12. | Lehtimäki TT, Kärkkäinen JM, Saari P, Manninen H, Paajanen H, Vanninen R. Detecting acute mesenteric ischemia in CT of the acute abdomen is dependent on clinical suspicion: Review of 95 consecutive patients. Eur J Radiol. 2015;84:2444-2453. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 53] [Cited by in RCA: 71] [Article Influence: 7.1] [Reference Citation Analysis (0)] |
| 13. | Kärkkäinen JM, Acosta S. Acute mesenteric ischemia (Part II) - Vascular and endovascular surgical approaches. Best Pract Res Clin Gastroenterol. 2017;31:27-38. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 27] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 14. | Wong PF, Gilliam AD, Kumar S, Shenfine J, O'Dair GN, Leaper DJ. Antibiotic regimens for secondary peritonitis of gastrointestinal origin in adults. Cochrane Database Syst Rev. 2005;CD004539. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 55] [Article Influence: 2.8] [Reference Citation Analysis (0)] |