Published online May 26, 2020. doi: 10.12998/wjcc.v8.i10.1958
Peer-review started: December 2, 2019
First decision: April 1, 2020
Revised: April 9, 2020
Accepted: April 27, 2020
Article in press: April 27, 2020
Published online: May 26, 2020
Processing time: 174 Days and 21.9 Hours
In recent years, the mechanical concept of intervertebral disc regeneration has become more and more popular due to the increasing awareness of the importance of preservation of spine movement. Interestingly, there is increasing evidence, however, that dynamic stabilization systems may compensate non-physiological loads, limit pathological movement, normalize disc height and intradiscal pressure, and provide an adaptive environment for disc regeneration.
The patient was a 54-year-old man, who presented with a 10-year history of mechanical back pain, which had become progressively serious and radiated into the left lower limb with numbness 3 mo prior. He had decreased muscle strength (class IV) of the left dorsal extensor and plantar flexor. Magnetic resonance imaging scans showed L3-S1 disc degeneration and L4-L5 disc herniation. Because the patient did not respond to various conservative treatments, he underwent a posterior L4-5 discectomy with fixation of the BioFlex dynamic stabilization system (Bio-Spine, Seoul, Korea). Preoperative symptoms were relieved and lumbar function was markedly improved after the operation. L4-L5 disc rehydration of instrumented segment was noted on magnetic resonance imaging at the 2-year follow-up.
Rehydration of the degenerated disc in our patient indicates that the BioFlex dynamic stabilization system may promote disc regeneration. Further research is needed to provide more evidence to support lumbar disc rehydration in the bridged segment using this system.
Core tip: The mechanical concept of intervertebral disc regeneration has become more and more popular due to the increasing awareness of the importance of preservation of spine movement. Interestingly, there is increasing evidence that dynamic stabilization systems may provide an adaptive environment for disc regeneration. In this study, we showed supporting evidence of rehydration of a degenerated disc after implantation of the BioFlex dynamic stabilization system, and reviewed the relevant medical literature.
- Citation: Li YC, Feng XF, Pang XD, Tan J, Peng BG. Lumbar disc rehydration in the bridged segment using the BioFlex dynamic stabilization system: A case report and literature review. World J Clin Cases 2020; 8(10): 1958-1965
- URL: https://www.wjgnet.com/2307-8960/full/v8/i10/1958.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v8.i10.1958
Degeneration of intervertebral disc is commonly accompanied by alterations of disc height, intradiscal pressure, load distribution, and motion patterns[1]. Since these alterations are subsequent results following disc degeneration, it is unlikely that regeneration will occur without first restoring the physiological status of the affected spinal segment[1]. Dynamic stabilization systems (DSS) are currently designed to restore physiological motion patterns and disc height and to normalize intradiscal pressure. Theoretically, they may have the potential to provide an adaptive environment for disc regeneration. Recently, both animal and clinical studies have indicated that disc distraction[2] or application of lumbar DSS[3-16] can enhance hydration in the degenerated disc and, therefore, regeneration.
This article describes a case whose lumbar disc showed rehydration in the implanted segment using the BioFlex DSS, and reviews the existing literature.
A 54-year-old man presented with a 10-year history of mechanical back pain, which became worse with activities and was reduced after bed rest. In the last 3 mo, his back pain had progressively increased and radiated into the left lower limb with numbness.
He had no relevant traumatic history.
Physical examination revealed a stiff lumbar spine with limited range of flexion, extension, and lateral bending. There were tenderness and percussion pain over the L4-L5 lumbar spine. Bilateral lower limb dermatomal sensation was normal, but he had decreased muscle strength (class IV) of the left hallux dorsal extensor. Lower extremity muscle tension, bilateral straight leg raising test, and strengthening test were all normal.
Laboratory data showed no infectious or inflammatory findings.
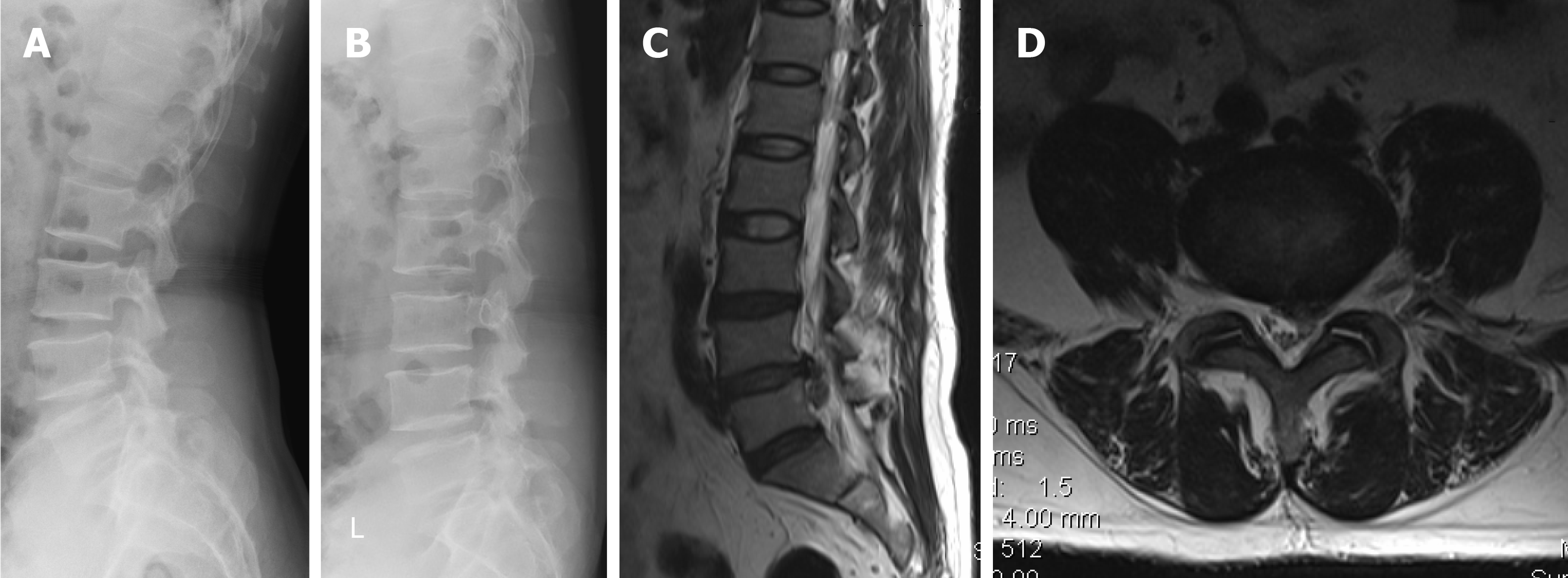
The initial plain radiographs revealed a decrease in height of the L4-L5 disc space. No instability was noted on the dynamic radiographs of flexion and extension of the lumbar spine (Figure 1A and 1B). Magnetic resonance imaging (MRI) scans showed L3-S1 disc degeneration with associated low signal intensity and L4-L5 disc herniation (Figure 1C and 1D).
The final diagnosis was lumbar disc herniation (L4-L5).
Before admission to our hospital, the patient had accepted various forms of conservative treatments such as physiotherapy, exercise, and drug therapy in a local clinic for 3 mo, but these therapies did not relieve his symptoms. Therefore, a posterior L4-L5 discectomy with fixation of a dynamic stabilization system (BioFlex system, Bio-Spine, Seoul, Korea) was recommended for this patient. During surgical decompression, left L4-5 laminotomy was performed with resection of the superior half of the L5 lamina and the inferior half of the L4 lamina along with preservation of left L4/5 facet joint.
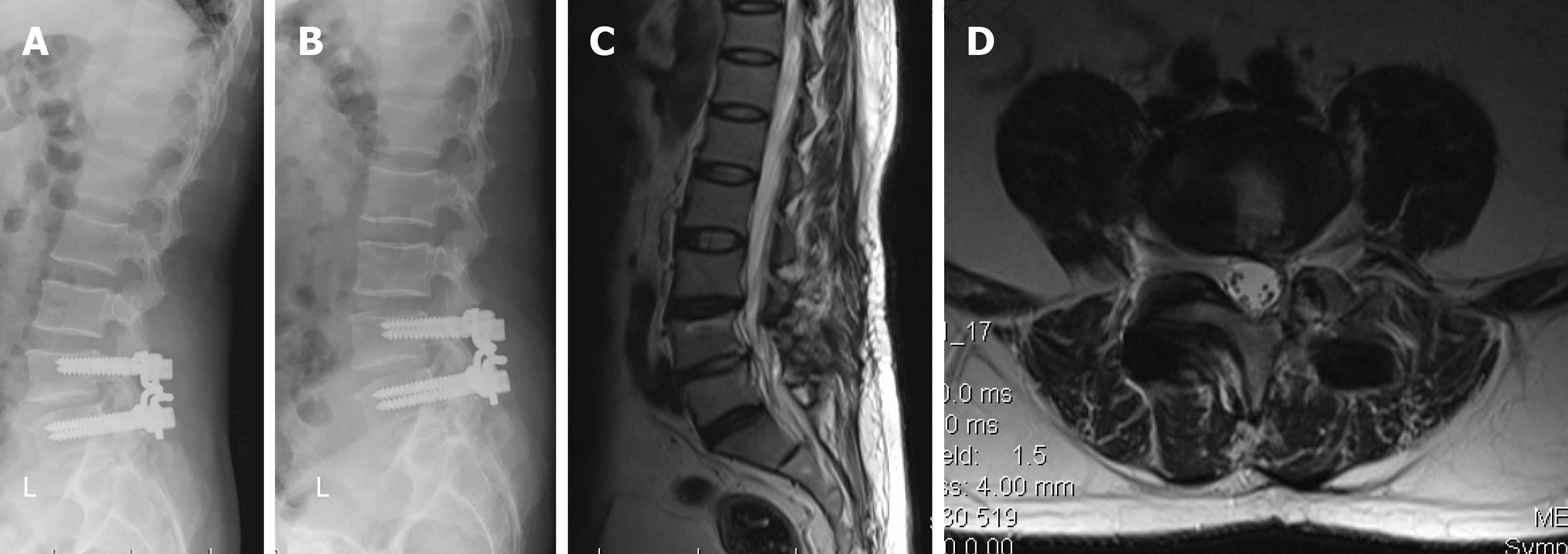
Surgery was successful and his symptoms were clearly relieved and lumbar function was markedly improved. The visual analogue scale score of back pain, left leg pain and Oswestry disability index decreased from 6, 8, and 58 preoperatively to 1, 0, and 0 at 24 mo, respectively, after the procedure. Partial motion of the implanted level was noted on postoperative flexion-extension plain radiographs (Figure 2A and 2B). An increasing signal intensity in the L4-L5 disc was noted on T2-weighted MRI (Figure 2C and 2D) after 2 years of follow-up after the operation.
A degenerate intervertebral disc is associated with significant structural failure such as nucleus pulposus dehydration, endplate sclerosis, annular protrusion, internal disc disruption, and disc space narrowing[1,17]. As the disc starts to degenerate, the water content of the nucleus pulposus is reduced, which is well tracked through MRI evaluation. A well-hydrated disc has bright signal intensity on T2-weighted MRI, whereas a degenerated disc appears gray to dark according to the severity of degeneration[17].
Regenerative strategies, such as transplantation of stem cells into nucleus pulposus, have been attempted to reverse disc degeneration experimentally and clinically[18]. However, the lack of an appropriate microenvironment and impaired capacity of diffusion of nutrients across a calcified endplate in the degenerated disc have hampered the survival of the transplanted stem cells[17]. The biomechanical concept for disc regeneration has grown popular in recent years with the improved understanding of the importance of spinal movement preservation. There is increasing evidence, however, that lumbar DSS may compensate non-physiological loads, limit pathological movement, normalize intradiscal height and pressure, and provide an adaptive microenvironment for disc regeneration[1,3,5,7,13,19]. However, controversial results still exist[20,21].
Currently, two kinds of available DSS are applied clinically including pedicle screw-based DSS and interspinous process spacers. The former includes Graf ligamentoplasty (Neoligaments, Leeds, United Kingdom), and the Dynesys system (Zimmer, Inc., Warsaw, IN, United States), FASS system (AO International, Davos, Switzerland), cosmic system (Ulrich GmbH and Co. KG, Ulm, Germany), TOPS system (Premia Spine USA, Philadelphia, PA, United States), FPSS system (Spine Vision, Paris, France), Accuflex system (Globus Medical, Inc., Audubon, PA, United States), Safinaz (Medikon AS, Medikon, Turkey), and BioFlex system (Bio-Spine) among others. The latter includes Wallis (Abbott Spine, Bordeaux, France), DIAM (Medtronic, Memphis, TN, United States), X-Stop (St. Francis Medical Technologies, Concord, CA, United States), and Coflex (Paradigm Spine LLC, New York, NY, United States).
In this study, we showed evidence of rehydration of a degenerated disc after implantation of the BioFlex system and reviewed the relevant medical literature. PubMed, the Cochrane Library, Medline, and EMBASE were searched using the following keywords, "disc rehydration" and "dynamic stabilization system, "which identified all possible studies published up to July 2019. References from these articles were also reviewed. We found 14 original studies on this topic. The detailed clinical information and device choices of all 15 studies are shown and summarized with the current case in Table 1. A study performed by Fay et al[7] found that Dynesys may stop or reverse disc degeneration in young patients but not in older patients. Instead, Vaga et al[14] discovered that the Dynesys was able to stop and partially reverse the disc degeneration, especially in a seriously degenerated disc. However, most studies on this topic are case reports[13] or case series[3-5,7-12,15,16] with low-quality and small samples. Degenerated disc rehydration has often been found serendipitously[4-6,10-12,15].
| Ref. | Types of implants | Age in yr | Number of patients | Follow-up in mo | Proportion of disc rehydration | Assessment method | Main findings | Comments |
| Bordes-Monmeneu et al[15], 2005 | Dynesys | 46.4 (26-68) | 20 | 9 | 9/20 (45%) | MRI, signal intensity | Disc rehydration occurred in some patients | Retrospective study, case series |
| Vaga et al[14], 2009 | Dynesys | 43.5 ± 9 | 10 | 6 | 3/10 (30%) | Molecular MRI, Pfirrmann grading | The Dynesys was able to stop and partially reverse the disc degeneration, especially in seriously degenerated disc and Pfirrmann grading was not sensitive enough to detect the disc change | Prospective study |
| Cho et al[13], 2010 | BioFlex | 22 | 1 | 12 | 1/1 (100%) | MRI, signal intensity | Increased disc height and disc rehydration occurred after BioFlex system | Case report |
| Reyes-Sánchez et al[12], 2010 | Accuflex | 44.05 (24-60) | 20 | 24 | 3/18 (16.67%) 2 cases lost follow | MRI, Pfirrmann grading | Three patients showed disc rehydration with one grade higher on the Pfirrmann classification and the Accuflex system stopped the degenerative process in 83% the patients | Prospective study, consecutive case series |
| Sandu et al[11], 2011 | Wallis | 67 (39-79) | 15 | 12 | NA | MRI, Modic grading | Wallis implantation could lead to disc rehydration | Retrospective study, case series |
| Heo et al[9], 2012 | BioFlex | 59.0 ± 8.4 | 25 | > 24 | 2/13 (15.4%) Exclude discectomy cases | MRI, modified Pfirrmann grading | BioFlex system might not prevent adjacent level degeneration completely. However, disc rehydration of the implantation segment occurred in 2 patients | Prospective study, case series |
| Xu et al[10], 2012 | Wallis | 41.5 (21-68) | 96 | 28 ± 14 | NA | MRI, signal intensity | Disc rehydration of the implantation segment occurred in some patients | Retrospective study, case series |
| Zagra et al[8], 2012 | FPSS system | 51.65 (25-65) | 32 | 12 | 8/32 (25%) | MRI, Pfirrmann grading | FPSS system was able to provide a potential disc rehydration | Prospective study, case series |
| Fay et al[7], 2013 | Dynesys | 53.0 ± 9.0 | 37 | > 48 | NA | MRI, CDS | Intervertebral disc rehydration was seen in younger patients and the Dynesys might stop or reverse the disc degeneration in the young age patients but not for the elderly patients | Retrospective study, case series |
| Gao et al[6], 2014 | ISOBAR TTL | 58.3 ± 13.5 | 24 | 28.7 ± 5.3 | 14/24 (58.33%) | MRI, Pfirrmann grading, ADC | ISOBAR TTL system could prevent or delay the degeneration of intervertebral discs | Retrospective study, comparative study |
| Canbay et al[5], 2015 | cosmicMIA | 38.7 ± 8.39 | 27 | 49.3 ± 18.35 | 4/27 (14.8%) | MRI, Pfirrmann grading, HIZ | Observations such as Pfirrmann grade improvements and disappearance of HIZs are concordant with improvements in VAS and ODI scores demonstrated that cosmicMIA systems might provide an environment for regeneration | Retrospective study, case series |
| Jiang et al[4], 2015 | Wallis | 47.6 (43-56) | 26 | 66.8 (60-70) | NA | MRI, Pfirrmann grading | Rehydration of the nucleus was observed, however, there were no statistically significant changes in the Pfirrmann grade at the instrumented level | Retrospective study, case series |
| Yilmaz et al[3], 2017 | Cosmic, Safinaz | 46.5 (27-67) | 59 | 86.8 (12-132) | 20/59 (34%) | MRI, Pfirrmann grading | DSS might decelerate the degeneration process and appears to facilitate regeneration | Retrospective study, case series |
| Luo et al[16], 2018 | Dynesys | 40.6 (21-55) | 23 | 39 (26-59) | 6/13 (46.2%) | MRI, Woodend classification | Dynamic stabilization promoted disc regeneration to some extent | Retrospective study, case series |
| Li et al1 | BioFlex | 54 | 1 | 24 | 1/1 (100%) | MRI, signal intensity | Decreased disc height and disc rehydration occurred after BioFlex system | Case report |
Physiologic motion, load distribution, and intradiscal pressure are mandatory for disc viability. Because a degenerate disc cannot regenerate itself, external devices may provide preconditions for biological attempts of regeneration[1]. Guehring et al[2] demonstrated that disc distraction can enhance disc rehydration of the degenerated disc and may also improve disc nutrient diffusion via the endplates. Furthermore, the authors thought that disc rehydration after distraction was probably related to the upregulated expression of the matrix genes collagen 1, collagen 2, decorin, and biglycan and the decline of apoptosis[2]. Wilke and colleagues found that changing positions are crucial to promoting fluid flow (nutrition) to the disc[22]. In addition, disc loading pattern with high load, low volume, and low frequency might impart healing or regeneration of the intervertebral discs[23]. DSS can not only result in disc distraction but also limit disc extension reasonably. Physiological spine motion and optimal intradiscal pressure after implantation of DSS may be maintained, which may provide optimal preconditions for disc rehydration and even further regeneration. Biological attempts of disc regeneration including stem cell, gene, and protein therapies combined with mechanical DSS may be optimal options. However, challenges still exist regarding the long-term tolerance of dynamic implants especially on the screw bone interface, and the fatigability of the composite materials[12]. In addition, there may be risk of bias by industry influence in our study. At the same time, our study is a case report and more evidence is needed to support lumbar disc rehydration in the bridged segment using the BioFlex system in the future.
Rehydration of a degenerated disc occurred after implantation of the BioFlex System in an adult patient after 2 years of follow-up.
Manuscript source: Unsolicited manuscript
Specialty type: Medicine, research and experimental
Country/Territory of origin: China
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): 0
Grade C (Good): C
Grade D (Fair): D
Grade E (Poor): 0
P-Reviewer: Emara KM, Jain SK S-Editor: Yan JP L-Editor: Filipodia E-Editor: Liu MY
| 1. | Schnake KJ, Putzier M, Haas NP, Kandziora F. Mechanical concepts for disc regeneration. Eur Spine J. 2006;15 Suppl 3:S354-S360. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 42] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 2. | Guehring T, Omlor GW, Lorenz H, Engelleiter K, Richter W, Carstens C, Kroeber M. Disc distraction shows evidence of regenerative potential in degenerated intervertebral discs as evaluated by protein expression, magnetic resonance imaging, and messenger ribonucleic acid expression analysis. Spine (Phila Pa 1976). 2006;31:1658-1665. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 48] [Cited by in RCA: 51] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 3. | Yilmaz A, Senturk S, Sasani M, Oktenoglu T, Yaman O, Yildirim H, Suzer T, Ozer AF. Disc Rehydration after Dynamic Stabilization: A Report of 59 Cases. Asian Spine J. 2017;11:348-355. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 17] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 4. | Jiang YQ, Che W, Wang HR, Li RY, Li XL, Dong J. Minimum 5 year follow-up of multi-segmental lumbar degenerative disease treated with discectomy and the Wallis interspinous device. J Clin Neurosci. 2015;22:1144-1149. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 11] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 5. | Canbay S, Ataker Y, Canbulat N, Kabaoglu ZU, Oktenoglu T, Sasani M, Ozer AF. Effect of Posterior Dynamic Instrumentation on High-Intensity Zone in Lumbar Degenerative Disc Disease. Turk Neurosurg. 2015;25:578-585. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 2] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 6. | Gao J, Zhao W, Zhang X, Nong L, Zhou D, Lv Z, Sheng Y, Wu X. MRI analysis of the ISOBAR TTL internal fixation system for the dynamic fixation of intervertebral discs: a comparison with rigid internal fixation. J Orthop Surg Res. 2014;9:43. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9] [Cited by in RCA: 11] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 7. | Fay LY, Wu JC, Tsai TY, Tu TH, Wu CL, Huang WC, Cheng H. Intervertebral disc rehydration after lumbar dynamic stabilization: magnetic resonance image evaluation with a mean followup of four years. Adv Orthop. 2013;2013:437570. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 16] [Cited by in RCA: 20] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 8. | Zagra A, Minoia L, Archetti M, Corriero AS, Ricci K, Teli M, Giudici F. Prospective study of a new dynamic stabilisation system in the treatment of degenerative discopathy and instability of the lumbar spine. Eur Spine J. 2012;21 Suppl 1:S83-S89. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 8] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 9. | Heo DH, Cho YJ, Cho SM, Choi HC, Kang SH. Adjacent segment degeneration after lumbar dynamic stabilization using pedicle screws and a nitinol spring rod system with 2-year minimum follow-up. J Spinal Disord Tech. 2012;25:409-414. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 20] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 10. | Xu L, Yu X, Bi LY, Liu GZ, Li PY, Qu Y, Jiao Y. [Intermediate and long-term follow-up evaluation of posterior dynamic lumbar stabilization in lumbar degenerative disease]. Zhonghua Wai Ke Za Zhi. 2012;50:792-796. [PubMed] |
| 11. | Sandu N, Schaller B, Arasho B, Orabi M. Wallis interspinous implantation to treat degenerative spinal disease: description of the method and case series. Expert Rev Neurother. 2011;11:799-807. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 11] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 12. | Reyes-Sánchez A, Zárate-Kalfópulos B, Ramírez-Mora I, Rosales-Olivarez LM, Alpizar-Aguirre A, Sánchez-Bringas G. Posterior dynamic stabilization of the lumbar spine with the Accuflex rod system as a stand-alone device: experience in 20 patients with 2-year follow-up. Eur Spine J. 2010;19:2164-2170. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 27] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 13. | Cho BY, Murovic J, Park KW, Park J. Lumbar disc rehydration postimplantation of a posterior dynamic stabilization system. J Neurosurg Spine. 2010;13:576-580. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 15] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 14. | Vaga S, Brayda-Bruno M, Perona F, Fornari M, Raimondi MT, Petruzzi M, Grava G, Costa F, Caiani EG, Lamartina C. Molecular MR imaging for the evaluation of the effect of dynamic stabilization on lumbar intervertebral discs. Eur Spine J. 2009;18 Suppl 1:40-48. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 39] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 15. | Bordes-Monmeneu M, Bordes-Garcia V, Rodrigo-Baeza F, Saez D. [System of dynamic neutralization in the lumbar spine: experience on 94 cases]. Neurocirugia (Astur). 2005;16:499-506. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 16. | Luo L, Zhang C, Zhou Q, Zhao C, Wang L, Liang L, Tu B, Ouyang B, Gan Y. Effectiveness of Transpedicular Dynamic Stabilization in Treating Discogenic Low Back Pain. World Neurosurg. 2018;111:e192-e198. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 17. | Kanna RM. Expert's comment concerning Grand Rounds case entitled "Rehydration of a degenerated disc on MRI synchronized with transition of Modic changes following stand-alone XLIF" by K. Kita, T. Sakai, M. Abe, Y. Takata and K. Sairyo (Eur Spine J; 2017: doi:10.1007/s00586-017-4945-6). Eur Spine J. 2017;26:632-634. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 18. | Peng B. Issues concerning the biological repair of intervertebral disc degeneration. Nat Clin Pract Rheumatol. 2008;4:226-227. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 10] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 19. | Putzier M, Schneider SV, Funk JF, Tohtz SW, Perka C. The surgical treatment of the lumbar disc prolapse: nucleotomy with additional transpedicular dynamic stabilization versus nucleotomy alone. Spine (Phila Pa 1976). 2005;30:E109-E114. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 116] [Cited by in RCA: 102] [Article Influence: 5.1] [Reference Citation Analysis (0)] |
| 20. | Grob D, Benini A, Junge A, Mannion AF. Clinical experience with the Dynesys semirigid fixation system for the lumbar spine: surgical and patient-oriented outcome in 50 cases after an average of 2 years. Spine (Phila Pa 1976). 2005;30:324-331. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 242] [Cited by in RCA: 189] [Article Influence: 9.5] [Reference Citation Analysis (0)] |
| 21. | Kumar A, Beastall J, Hughes J, Karadimas EJ, Nicol M, Smith F, Wardlaw D. Disc changes in the bridged and adjacent segments after Dynesys dynamic stabilization system after two years. Spine (Phila Pa 1976). 2008;33:2909-2914. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 68] [Cited by in RCA: 66] [Article Influence: 3.9] [Reference Citation Analysis (0)] |
| 22. | Wilke HJ, Neef P, Caimi M, Hoogland T, Claes LE. New in vivo measurements of pressures in the intervertebral disc in daily life. Spine (Phila Pa 1976). 1999;24:755-762. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1013] [Cited by in RCA: 889] [Article Influence: 34.2] [Reference Citation Analysis (0)] |
| 23. | Steele J, Bruce-Low S, Smith D, Osborne N, Thorkeldsen A. Can specific loading through exercise impart healing or regeneration of the intervertebral disc? Spine J. 2015;15:2117-2121. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 28] [Article Influence: 2.8] [Reference Citation Analysis (0)] |