Published online Apr 16, 2017. doi: 10.12998/wjcc.v5.i4.148
Peer-review started: January 25, 2016
First decision: February 29, 2016
Revised: November 11, 2016
Accepted: January 2, 2017
Article in press: January 3, 2017
Published online: April 16, 2017
Processing time: 444 Days and 10.8 Hours
Inferior vena cava filters have gained increasing popularity in recent decades and knowledge on rare complications becomes vital to practicing physicians. A 30-year-old African American male with diabetes mellitus, hypertension, end-stage renal disease, history of deep venous thrombosis and placement of venacaval filter who was seen in the cardiology clinic for cardiac risks stratification prior to renal transplant. Patient denied any cardiac symptoms. A transthoracic echocardiogram was performed and showed two linear echoes bright densities in the right atrium and right ventricle embedded which was later found to be fractured filter struts by computed tomography. We discuss the various outcomes associated with non-retrieval of retrievable inferior vena cava filters.
Core tip: Retrievable vena cava filters as indicated by the name, is temporary and should be retrieved timely. However noncompliance to follow-up and retrieval has been associated with numerous complications which could also be life threatening in extreme cases. We are writing this case with the intent to enlighten physicians on various types of available filters, complications associated with it and the challenges associated with delayed retrieval of filters. This case report also emphasizes the challenges associated with delayed retrieval of the filters and the management of the complications associated with inferior vena cava filters.
- Citation: Sivasambu B, Kabirdas D, Movahed A. Incidental echocardiographic finding: Fractured inferior vena cava filter. World J Clin Cases 2017; 5(4): 148-152
- URL: https://www.wjgnet.com/2307-8960/full/v5/i4/148.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v5.i4.148
Intracardiac foreign bodies have been described in the literature with the first case described in 1954. Various post traumatic and iatrogenic cardiac foreign bodies have been implicated with catheters fragments, needles, pacemaker electrodes, and stents being the commonest. We describe an asymptomatic patient who was found to have an intra cardiac foreign body on a transthoracic echocardiogram done for preoperative evaluation for renal transplant. On further evaluation it was confirmed as inferior vena cava (IVC) filter fragments.
Vena cava filters have gained increasing popularity in recent decades with the simplicity of the procedure, and the expansion of the indications including prophylactic insertion especially in patients following trauma with high risk for venous thromboembolism. Thus knowledge about the possible complications associated with IVC filters becomes vital for practicing physicians. Fracture of IVC filters and intra cardiac embolization can lead to potentially life threatening complications.
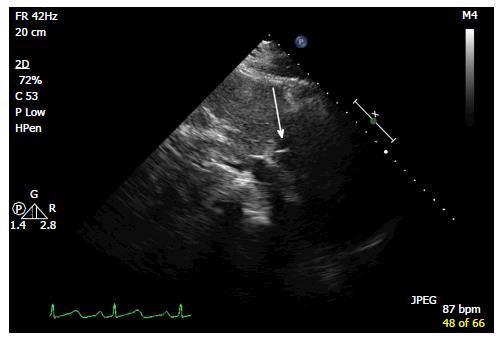
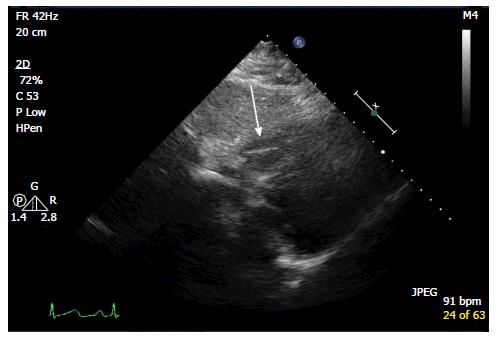
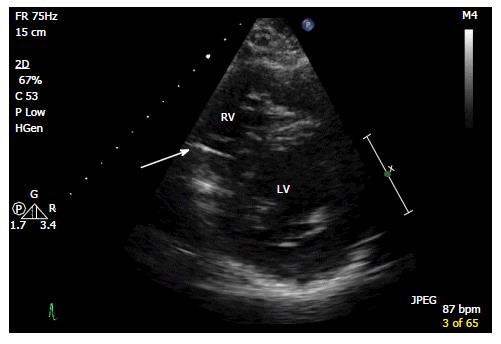
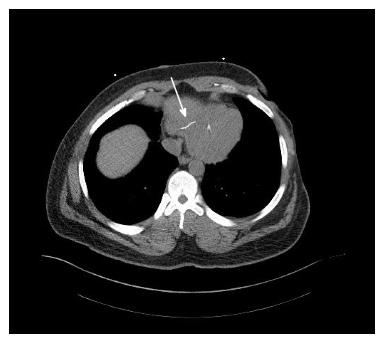
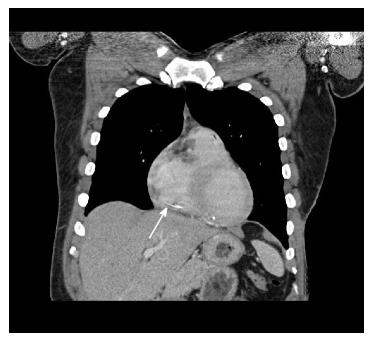
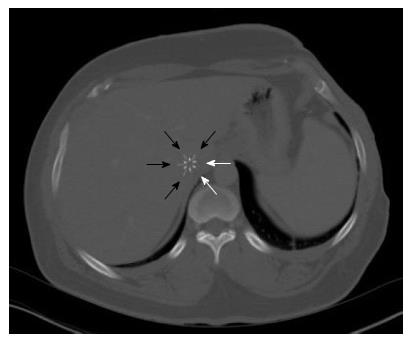
A 30-year-old African American male with diabetes mellitus, hypertension and end-stage renal disease was seen in the cardiology clinic for cardiac risk stratification prior to renal transplant. Patient denied any cardiac symptoms and stated to have good functional status. One year prior he had sustained a motor vehicle accident with extensive burn injuries and fracture of the left tibia and fibula for which he had an external fixation performed. His hospital course was complicated by deep venous thrombosis (DVT) for which he underwent placement of an IVC filter. On examination pulse rate was 78, arterial pressure was 140/88 mmHg and respiratory rate was 14. Physical examination was remarkable for scars in chest and extremities from prior burns treated with skin graft. Cardiovascular examination revealed normal heart sounds with no gallops or murmurs and no volume over load. Electrocardiogram showed normal sinus rhythm. The transthoracic echocardiogram showed two linear echo bright densities in the right atrium (Figure 1) and ventricle embedded in the wall (Figures 2 and 3) otherwise unremarkable. Non-contrast computed tomography of the chest confirmed the presence of the foreign bodies which was identified to be the fractured limbs of the IVC filter (Figures 4 and 5). IVC filter was in place with the missing limbs evident on imaging (Figure 6). As patient was asymptomatic and the objects were found to be embedded in the myocardium vena cava filter retrieval was not advocated. Though the indication for IVC filter placement was transient patient had lost to follow-up and now presented with an incidental intra cardiac foreign body.
The Mobin-Uddin umbrella filter[1] was the initial filter of historical value followed by the Greenfield filter which was introduced in 1973 by Greenfield et al[2] and still remains the standard to which other filters are compared. Vena cava filter is utilized as a treatment option of venous thromboembolism in specific situations. Venous thrombo embolism (VTE) comprises of deep venous thrombosis and pulmonary embolism (PE). VTE is known to be associated with increased morbidity and mortality. The gold standard treatment for DVT and PE is anticoagulation. However in the presence of contraindication for anticoagulation or if significant risk of bleeding persists vena cava filters are the safest treatment modality[3,4]. Vena cava filters can also be placed for treatment failure of anticoagulation and recurrent thrombosis despite therapeutic levels of anticoagulation and development of new contraindications after initiation of anticoagulation. In the latter however the decision of placement depends on the required duration of anticoagulation and the risk of thrombosis on cessation of anticoagulation.
Vena cava filters (IVC filters) are commonly placed in the IVC below the level of renal veins owing to the high prevalence of lower extremity thrombosis and subsequent pulmonary embolism. Even in the absence of demonstrable Lower extremity thrombosis in pulmonary embolism, IVC filters are placed if anticoagulation is contraindicated as thrombus in the pelvis or calf veins may be undetected or can form later. Nevertheless in the context of upper extremity thrombosis IVC filters are not beneficial and superior vena cava filters should be placed.
Utilization of IVC filters for DVT varies widely and has been recently evaluated in a study in 263 hospitals. Approximately 15% of the patients with venous thromboembolism received filter placement with a wide range between 0% to 39%. The characteristics associated with the wide variability in filter placement were acute bleeding at the time of admission, major operation after admission, presence of metastatic cancer, more severe illness, small hospital, and rural location.
Various types of IVC filters are available for use currently and can be classified as permanent and retrievable filters. The Society of Interventional Radiology guidelines recommends that the decision to select between the permanent and retrievable filter should be based on required duration of treatment for venous thromboembolism and the risks associated with anticoagulation therapy[5]. Complications are associated with both type of filters but the prevalence of complications varies with each specific type of IVC filter. Complications could be directly associated with the insertion of the filter such as bleeding or infection at the puncture site, allergic reactions to contrast or other medications used during placement, misplacement of the filter and entrapment of the guidewire within the filter. Late complications include fracture, migration, limb embolization, tilt, IVC penetration, VTE and IVC thrombus[6,7].
A review of data from the United States Food and Drug Administration Manufacturer and User Facility Device Experience (MAUDE) from January 2009-December 2012 reveled 1606 reported AEs involving 1057 IVC filters were identified. Of reported AEs, 1394 (86.8%) involved retrievable IVC filters, and 212 (13.2%) involved permanent IVC filters (P < 0.0001). Reported AEs included fracture, migration, limb embolization, tilt, IVC penetration, venous thromboembolism and pulmonary embolism, IVC thrombus, and malfunctions during placement.
IVC filters mechanically provide protection from lower extremity DVT migration to the lungs however does not protect against thrombosis at or below the filter. Knowledge on management of IVC filter thrombosis is limited to experience with small group of patients. Various techniques have been utilized with endovascular treatment being more successful. Other techniques such as catheter-directed thrombolysis, power pulse spray, various mechanical devices, judicious use of tPA or stent placement have also been used in case by case basis.
Though the most reported complication with retrievable filter was fracture according to the MAUDE database[8] other studies revealed significantly varying fracture risk according to the brand of filter with the Celect filters having a very low fracture rate and the Bard Recovery filters having the highest as high as 25%[9].
Fracture of a filter strut and intracardiac embolization[10] has been reported in literature to be a devastating complication in some patients. An intracardiac strut can be asymptomatic as in our patient or present with a clinical picture similar to PE with shortness of breath pleuritic chest pain, non-sustained ventricular tachycardia and life threatening cardiac tamponade. The use of IVC filter is trending up and the availability of various types with different risk profile mandates physicians to have knowledge regarding types of filters and clinical implications associated with each type to recognize the complications and institute timely appropriate management. The choice of filter should take into consideration individual risks of the filter, clinical indication for the filter and the required duration of treatment to avoid unnecessary complications.
Timely retrieval of retrievable filter can prevent the sequelae of fracture and embolization and the subsequent complications. In systematic review by Angel et al[11] the retrieval rate was as low as 34%. As a consequence of reported low retrieval rates the Food and Drug Administration in the United States has recommended that “the implanting physicians and clinicians responsible for the ongoing care of patients with retrievable IVC filters consider removing the filter as soon as protection is no longer needed”[12].
Optimum management of intracardiac foreign bodies depends on the size and shape of the foreign body and the symptoms. Asymptomatic patients with a foreign body that is smoothly shaped and less than 5-10 mm can be managed conservatively. Our patient did not demonstrate any high risk features and thus was managed conservatively.
In conclusion, IVC filters are increasingly utilized in the clinical practice albeit with low retrieval rates of temporary filters which could result in potentially life threatening preventable complications. Timely retrieval of IVC filter is vital to prevent the unwanted sequelae associated with filter strut fracture and embolization. This case was written to highlight the importance of timely retrieval of filters and to enlighten physicians on rare complications associated with non-retrieval.
A 30-year-old African American male presented to the cardiology clinic for cardiac risks stratification prior to renal transplant.
Physical examination was remarkable for scars in chest and extremities from prior burns treated with skin graft otherwise unremarkable.
Foreign body in right atrium suspected either a fractured inferior vena cava (IVC) filter or a metal travelling intravascularly to heart following car accident.
Unremarkable other than elevated creatinine due to end stage renal failure.
The transthoracic echocardiogram showed two linear echo bright densities in the right atrium and ventricle embedded in the wall. Non-contrast computed tomography of the chest confirmed the presence IVC filter was in place with the missing limbs evident on imaging.
As patient was asymptomatic and the objects were found to be embedded in the myocardium vena cava filter retrieval was not advocated.
Fracture of a filter strut and intracardiac embolization has been reported in very few case reports to be a devastating complication in some patients. However rates of IVC filter removal remains low.
IVC filters are used in patients with deep venous thrombosis of lower extremities with contraindications for anticoagulation’s.
Timely retrieval of IVC filter is vital to prevent the unwanted sequelae associated with filter strut fracture and embolization.
The authors describe an interesting and well documented complication of cava filter and give a nice review of literature.
Manuscript source: Invited manuscript
Specialty type: Medicine, research and experimental
Country of origin: United States
Peer-review report classification
Grade A (Excellent): A
Grade B (Very good): 0
Grade C (Good): C
Grade D (Fair): D
Grade E (Poor): 0
P- Reviewer: Najafi M, Rauch B, Skobel E S- Editor: Gong XM L- Editor: A E- Editor: Li D
| 1. | Mobin-Uddin K, Smith PE, Martinez LO. A vena caval filter for the prevention of pulmonary embolus. Surg Forum. 1967;18:209-211. |
| 2. | Greenfield LJ, McCurdy JR, Brown PP, Elkins RC. A new intracaval filter permitting continued flow and resolution of emboli. Surgery. 1973;73:599-606. [PubMed] |
| 3. | Prevention of venous thrombosis and pulmonary embolism. Natl Inst Health Consens Dev Conf Consens Statement. 1986;6:1-8. [PubMed] |
| 4. | Dalen JE, Alpert JS. Natural history of pulmonary embolism. Prog Cardiovasc Dis. 1975;17:259-270. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 777] [Cited by in RCA: 657] [Article Influence: 13.1] [Reference Citation Analysis (0)] |
| 5. | Caplin DM, Nikolic B, Kalva SP, Ganguli S, Saad WE, Zuckerman DA. Quality improvement guidelines for the performance of inferior vena cava filter placement for the prevention of pulmonary embolism. J Vasc Interv Radiol. 2011;22:1499-1506. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 6. | Ferris EJ, McCowan TC, Carver DK, McFarland DR. Percutaneous inferior vena caval filters: follow-up of seven designs in 320 patients. Radiology. 1993;188:851-856. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 253] [Cited by in RCA: 226] [Article Influence: 7.1] [Reference Citation Analysis (0)] |
| 7. | Ray CE, Kaufman JA. Complications of inferior vena cava filters. Abdom Imaging. 1996;21:368-374. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 85] [Cited by in RCA: 72] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 8. | Andreoli JM, Lewandowski RJ, Vogelzang RL, Ryu RK. Comparison of complication rates associated with permanent and retrievable inferior vena cava filters: a review of the MAUDE database. J Vasc Interv Radiol. 2014;25:1181-1185. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 113] [Cited by in RCA: 128] [Article Influence: 11.6] [Reference Citation Analysis (0)] |
| 9. | Nicholson W, Nicholson WJ, Tolerico P, Taylor B, Solomon S, Schryver T, McCullum K, Goldberg H, Mills J, Schuler B. Prevalence of fracture and fragment embolization of Bard retrievable vena cava filters and clinical implications including cardiac perforation and tamponade. Arch Intern Med. 2010;170:1827-1831. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 147] [Cited by in RCA: 160] [Article Influence: 10.7] [Reference Citation Analysis (0)] |
| 10. | Poudel DR, Pathak R, Karmacharya P, Ghimire S, Khanal R, Badal M. Stuck in the Heart: Embolized Strut Fracture of IVC Filter. Vasc Endovascular Surg. 2015;49:93-94. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 6] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 11. | Angel LF, Tapson V, Galgon RE, Restrepo MI, Kaufman J. Systematic review of the use of retrievable inferior vena cava filters. J Vasc Interv Radiol. 2011;22:1522-1530.e3. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 396] [Cited by in RCA: 351] [Article Influence: 25.1] [Reference Citation Analysis (0)] |
| 12. | United States Department of Health and Human Service. Removing Retrievable Inferior Vena Cava Filters: FDA Safety Communication. Available from: http://www.fda.gov/MedicalDevices/Safety/AlertsandNotices/ucm396377.htm. |