Published online Jan 16, 2014. doi: 10.12998/wjcc.v2.i1.9
Revised: December 24, 2013
Accepted: January 7, 2014
Published online: January 16, 2014
Processing time: 57 Days and 15.4 Hours
Gastrointestinal stroma tumours (GIST) are the most common mesenchymal tumour in the digestive tract and commonly found in the stomach. The patient described in this report presented with collapse and a palpable abdominal mass. He was found to have a large gastric GIST that penetrated through the mesocolon. Resection of the GIST was technically challenging but facilitated by a new generation ultrasonic scalpel device. In resection of gastric cancer the use of ultrasonic scalpels has been shown to reduce operating time, blood loss and length of stay. We feel that in technically challenging cases of gastric GIST the use of an ultrasonic scalpel device may be justified as well.
Core tip: This case report about a giant gastric gastrointestinal stroma tumours focuses on surgical technique. Because of its bulk the giant tumour was penetrating through the transverse mesocolon. Dissecting the tumour of the mesocolon and avoiding a concomitant colectomy was facilitated by using a new generation ultrasonic scalpel device.
- Citation: Schneider C, Hewin DF. Resection of giant gastric GIST with a new generation ultrasonic scalpel device. World J Clin Cases 2014; 2(1): 9-11
- URL: https://www.wjgnet.com/2307-8960/full/v2/i1/9.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v2.i1.9
Gastrointestinal stromal tumours (GISTs) are the most common mesenchymal tumour of the digestive tract. Most GISTs are found in the stomach and although bleeding is a frequent complication, they usually present with non-specific symptoms[1]. We present a case of a giant gastric GIST in a patient presenting with collapse and a palpable abdominal mass. Intra-operatively the tumour was found to penetrate the transverse mesocolon. Resection of the GIST without requiring a colectomy was facilitated using a new generation ultrasonic scalpel device (HARMONIC ACE®+).
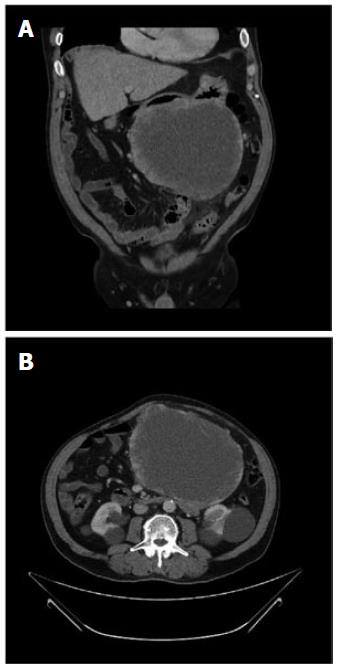
This 71-year-old man with a past medical history of hypertension and peptic ulcer disease was admitted to the local Emergency Department with a sudden onset of abdominal pain followed by collapse. Clinical examination revealed a large epigastric abdominal mass. The patient was haemodynamically stable and initial full blood count and biochemistry tests were unremarkable. The patient was discharged home and booked in for an ultrasound scan (USS), which revealed a large heterogeneous soft tissue mass extending from the epigastrium into the pelvis. CT scan of the abdomen and pelvis was performed immediately, revealing a large mass inseparable from the greater curve of the stomach and the body of the pancreas. A large proportion of the tumour had low attenuation indicating cystic change or necrosis. The Radiology report concluded that the differential diagnosis should include cystadenocarcinoma of the pancreas, neuroendocrine tumour and GIST (Figure 1). The patient was urgently referred to the oesophago-gastric department. After multi-disciplinary discussion and outpatient review the patient was scheduled for surgery.
The operation was performed via a midline laparotomy. Intraoperative findings were that of a large tumour arising from the greater curve of the stomach. The tumour was firmly attached and penetrating completely through the mid-portion of the transverse mesocolon, without invading it. It was difficult to establish a safe plane of dissection between tumour and colonic vessels. At this stage the HARMONIC ACE®+ proved valuable as it aided in the careful separation of tumour and mesocolon. A novel feature added to the latest generation of the device is the audible “tissue sensing” feedback. As the device is activated a constant tone starts, similar to older versions. The dissecting shears “sense” when tissues have been divided and the quality of tone changes which signals to the surgeon to stop activation of the device. In our view the main benefits of this feature were reduced heat dissipation thereby enabling us to dissect the tumour off the transverse mesocolon without inadvertently damaging the colonic blood supply. There was also a marked increase in speed of dissection as the audible feedback reduced the overall activation time during dissection.
The gastro-colic omentum was divided and the tumour dissected from the mesocolon where possible. Several densely adherent branches of the middle colic vessels were sacrificed and the transverse colon checked for viability. The tumour was carefully dissected from its attachments to the duodenum and pancreas. A standard distal gastrectomy with a retrocolic Roux-en-Y reconstruction was carried out.
The patient made an unremarkable recovery and was discharged on the seventh postoperative day. He was readmitted on the 19th postoperative day with haematemesis. Gastroscopy was performed and showed ulcerations around the staple line of the gastro-jejunal anastomosis but no active bleeding was found. The patient remained haemodynamically stable throughout his second admission and was discharged after two days.
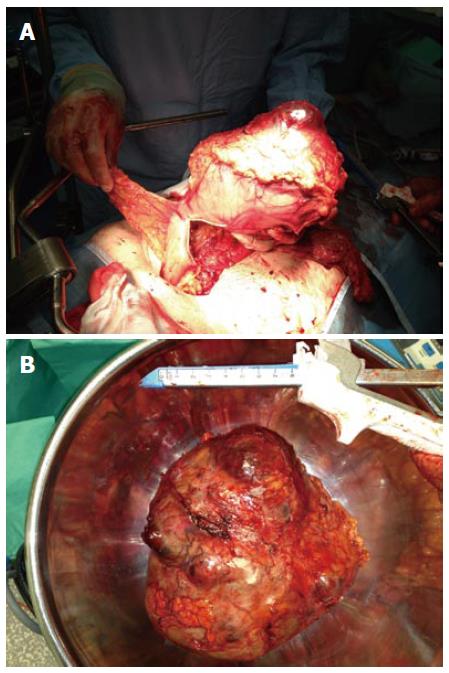
Histopathological macroscopic examination revealed a greyish, pale, soft tumour with cystic haemorrhagic and necrotic areas. Tumour weight was measured at 2.6 kg and dimensions were 19 cm × 18 cm × 16 cm (Figure 2). A massive central area of haemorrhage was noted. On immunostaining the tumour stained positive for KIT (CD 117) and CD 34. Mitotic rate was seven out of ten and immunostaining for Ki-67 showed an increased proliferation index of seven percent. Microscopic examination and immunostaining were compatible with a GIST of the spindle cell type. Resected lymph nodes did not show any metastatic spread. All of the above histopathological findings were congruent with a completely excised GIST with high risk for malignant potential. Following further multidisciplinary team discussion the patient was referred to oncology services for adjuvant chemotherapy.
This case highlights an unusual clinical presentation of a Gastrointestinal Stromal Tumour and a successful approach to the intraoperative challenges.
The patient presented with acute collapse and an abdominal mass. Only a small number of GIST presenting as a palpable abdominal mass have been reported in the world literature[2]. The patients collapse was probably a result of an acute bleed into the tumour; however no clinical or haematological signs of haemodynamic compromise were evident on presentation to emergency services.
The challenges of the operation described above were the large size of the tumour and the penetration of its bulk through the transverse mesocolon. The tissue sensing properties of the HARMONIC ACE®+ enabled us to preserve most of the middle colic vessels, thereby avoiding the added trauma of a concomitant colectomy.
To our knowledge, use of an ultrasonic scalpel has not been reported in open surgery for gastric GIST, however its benefits have been reported in the open resection of gastric cancer. One group found the device to decrease operating time, blood loss and operator stress during lymphadenectomy[3]. These findings were recently confirmed in a trial that, in addition to the above, showed a shorter length of hospital stay and a higher number of lymph nodes harvested in the group undergoing gastrectomy with an ultrasonic scalpel[4]. Overall hospitalisation costs were found to be equal between the traditional and ultrasonic scalpel surgery groups.
This technically challenging case demonstrates that utilisation of the new generation ultrasonic scalpel in the open resection of giant GIST of the stomach is feasible. The device’s tissue sensing technology may help in preserving vital structures and therefore may lessen the extent of resection, reducing morbidity.
A technically challenging case of a giant gastric gastrointestinal stromal tumours (GIST) resection facilitated by the HARMONIC ACE®+ ultrasonic scalpel.
A giant gastric GIST presenting with collapse and a palpable abdominal mass.
The main differential diagnosis in a patients presenting with collapse and an abdominal mass is an abdominal aortic aneurysm rupture.
Routine blood tests performed on admission included a full blood count, liver function tests, urea and electrolytes and C-reactive protein; all of which were unremarkable.
The abdominal ultrasound scan showed a large abdominal mass and computer tomography revealed a large tumour inseparable from the greater curve of the stomach with a central necrotic area.
Histopathological macroscopic examination revealed a greyish, pale, soft tumour which on microscopic examination and immunostaining was compatible with a GIST.
Resection of the GIST was performed via a midline laparotomy and following multidisciplinary team discussion adjuvant treatment with Imatinib was commenced.
GIST. Ultrasonic scalpel - a surgical device that cuts and coagulates tissues by generating friction.
Dissection in proximity to vulnerable structures may be facilitated by the HARMONIC ACE®+ ultrasonic scalpel.
Authors describe a case of a giant gastric GIST respected by HARMONIC ACE+ (as stated in the title). The manuscript is well written. Gastric GISTs are very well known entity.
P- Reviewers: Beegun I, Brcic I, Desai DJ S- Editor: Qi Y L- Editor: A E- Editor: Wang CH
| 1. | Rossi CR, Mocellin S, Mencarelli R, Foletto M, Pilati P, Nitti D, Lise M. Gastrointestinal stromal tumors: from a surgical to a molecular approach. Int J Cancer. 2003;107:171-176. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 101] [Cited by in RCA: 113] [Article Influence: 5.1] [Reference Citation Analysis (0)] |
| 2. | Patil S, Jain S, Kaza RC, Chamberlain RS. Giant gastrointestinal stromal tumor presenting as a palpable abdominal mass: an unusual presentation. ISRN Surg. 2011;2011:894829. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Cited by in RCA: 8] [Article Influence: 0.6] [Reference Citation Analysis (0)] |
| 3. | Inoue K, Nakane Y, Michiura T, Yamada M, Mukaide H, Fukui J, Miki H, Ueyama Y, Nakatake R, Tokuhara K. Ultrasonic scalpel for gastric cancer surgery: a prospective randomized study. J Gastrointest Surg. 2012;16:1840-1846. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 25] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 4. | Huang Y, Mu GC, Qin XG, Lin JL, Liu C, Chen ZB, Zeng YJ. The application of ultrasonic harmonic scalpel in the radical surgery of gastric cancer. Clin Transl Oncol. 2013;15:932-937. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.3] [Reference Citation Analysis (0)] |