Published online Jul 6, 2025. doi: 10.12998/wjcc.v13.i19.101889
Revised: February 17, 2025
Accepted: February 27, 2025
Published online: July 6, 2025
Processing time: 170 Days and 12 Hours
The surgical management of corneal lesions resulting from eyelid pathologies requires a comprehensive approach to ensure optimal patient outcomes. Eyelid lesions, ranging from benign to malignant, can lead to corneal damage through mechanisms such as mechanical abrasion, secondary infection, or inflammatory responses.
To assess the surgical methodologies utilized in the treatment of corneal lesions resulting from eyelid disorders and evaluate their effects on patient outcomes, recurrence rates, and postoperative complications. The incorporation of advanced imaging techniques, including optical coherence tomography and ultrasound biomicroscopy, in conjunction with histopathological analysis, is addressed to improve surgical accuracy and patient outcomes.
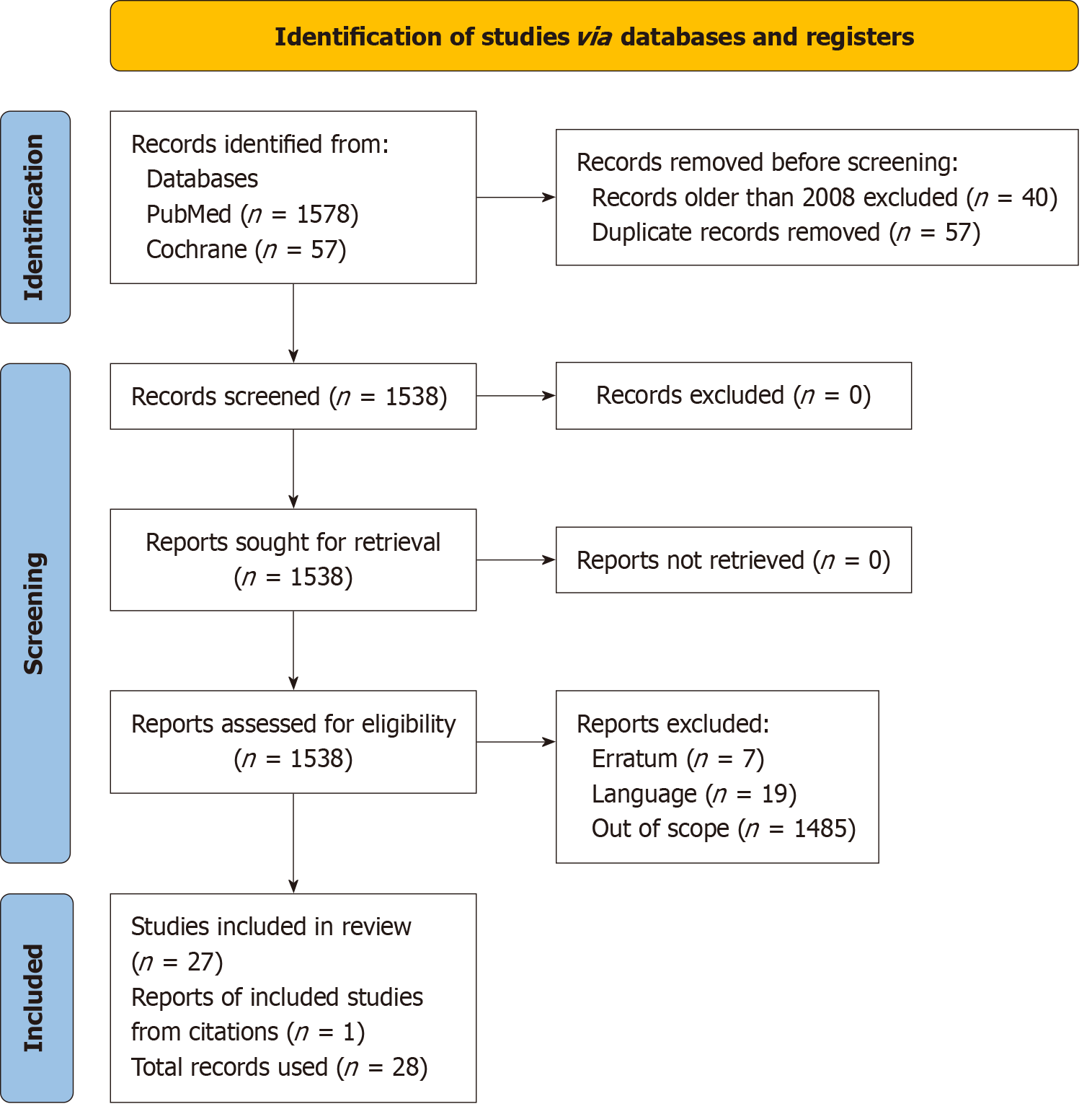
The authors searched online databases (PubMed and Cochrane) for publications on the surgical management of lid lesions. Records received from the two databases were checked for duplicates and relevance. Only records with full texts and in English language were included.
A total of 28 records were obtained following the screening for relevancy and duplication. The review underscores essential surgical approaches employed in the treatment of corneal lesions resulting from common eyelid diseases, focusing on operative efficacy, complication rates, and long-term results.
This systematic review emphasizes the significance of choosing suitable surgical techniques tailored to individual patient characteristics and stresses the need for interdisciplinary collaboration in ophthalmic care. The results indicate that sophisticated imaging techniques and careful preoperative preparation markedly improve surgical accuracy and long-term results.
Core Tip: Eyelid disorders can lead to significant corneal damage, necessitating precise surgical intervention. This systematic review evaluates surgical approaches for correcting entropion, ectropion, and other conditions affecting the ocular surface. The findings highlight the critical role of interdisciplinary collaboration, advanced preoperative imaging, and individualized surgical strategies in optimizing outcomes and minimizing recurrence.
- Citation: Miotti G, Quaglia D, De Marco L, Parodi PC, D’Esposito F, Musa M, Tognetto D, Gagliano C, Zeppieri M. Surgical management of patients with corneal lesions due to lid pathologies. World J Clin Cases 2025; 13(19): 101889
- URL: https://www.wjgnet.com/2307-8960/full/v13/i19/101889.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v13.i19.101889
Corneal injuries are a prevalent reason for emergency room visits, constituting roughly 3 out of 100 cases, with corneal abrasions and foreign bodies as the most common manifestations. These injuries, varying in severity from minor to vision-threatening, can be classified as traumatic or exposure-related. Corneal abnormalities, including abrasion, laceration, or perforation, can occur through multiple processes. Mechanical damage, including contact lens edges, scratches from fingernails, or foreign objects in the eyelid or fornices, or in diseases such as distichiasis or trichiasis, are prevalent causes. Factors connected to exposure also play a part, mainly in neurotrophic disorders that hinder complete eyelid closure, such as seventh cranial nerve palsy or Bell's palsy. Additional factors encompass restricted eyelid disor
Individuals with corneal injuries frequently have sensations of foreign bodies and agony, which may manifest several hours after the injury occurs. In instances of chemical burns, symptoms such as pain, tearing, and sight impairment manifest immediately. Identifying the source of the trauma is crucial, particularly when high-velocity instruments or caustic agents are implicated, to inform diagnostic and therapeutic approaches. The physical examination, enhanced by magnification and fluorescein staining, facilitates the visualization of corneal abnormalities and foreign substances. Perforating injuries present with altered iris morphology, a positive Seidel’s test, and reduced anterior chambers that could be indicative of aqueous leaking[1].
This study seeks to thoroughly analyze the surgical procedures utilized in the management of corneal ulcers caused by eyelid traumatic and functional diseases (trichiasis, lagophthalmos, distichias, epiblepharon, entropion, lagophthamos and ectropion). Through the examination of published literature, we aim to assess procedure effectiveness, indications, complications, and long-term results, eventually offering a thorough resource for doctors managing these disorders.
Using the PubMed database (https://pubmed.ncbi.nlm.nih.gov) and Cochrane databases (https://www.cochranelibra
In accordance with the methodology outlined by Tham et al[2], we performed a systematic review utilizing the PubMed and Cochrane databases. Search phrases were amalgamated using Boolean operators, and results were evaluated according to inclusion and exclusion criteria. Two separate evaluators (Quaglia D and Miotti G) appraised the relevance of the work, and any disagreements were reconciled by a third evaluator (De Marco L). Four hundred and eighty-five papers were discarded for not directly addressing the surgical therapy of corneal lesions resulting from eyelid diseases. These encompassed general ophthalmic evaluations, case reports, and studies devoid of surgical outcome data. Articles were eliminated by a systematic screening procedure involving title, abstract, and full-text assessment.
A total of 28 studies were incorporated into this evaluation following the application of eligibility criteria (Table 1). These studies assessed surgical procedures for corneal lesions associated with the eyelids, emphasizing operative effectiveness, complication rates, and long-term results. Research demonstrates that surgical methods using horizontal lid tightness have reduced recurrence rates. Preoperative imaging, including optical coherence tomography (OCT), has become an essential instrument in enhancing surgical planning. Moreover, interdisciplinary teamwork has demonstrated an improvement in overall patient outcomes. The review emphasizes the necessity of personalized surgical strategies adapted to the severity and cause of eyelid disorders. The research are categorized into three types: (1) Comparative assessments of surgical procedures; (2) Clinical outcomes and complication rates; and (3) Supplementary measures for enhanced prognosis.
| Ref. | Year | Type of study | Results | Conclusions |
| Gu et al[3] | 2009 | Prospective cohort study with 14 patients | Acellular dermis was effective in reducing the palpebral aperture (P = 0.002), lagophthalmos (P = 0.016), and lengthening the upper eyelid height by reducing the upper margin-reflex distance (P = 0.008). There were 2 cases of recurrence because of the shrinkage of graft (70%) and 3 cases of conjunctival granulomas postoperatively | Acellular dermis grafting with insertion of therapeutic contact lenses is an effective and simple measure for rectifying severe cicatricial entropion both structurally and functionally |
| Swamy et al[4] | 2008 | Prospective with 147 eyelid operations | Ninety-four per cent of patients noted symptomatic improvement. The postoperative complications included excess keratin (29%), recurrence of cicatricial entropion (4.1%), punctuate epithelial erosion (2.7%), graft shrinkage (0.7%) and donor site bleeding (2.0%) | Cicatricial Entropion with hard palate mucous membrane grafting for both upper and lower eyelid surgery offers high symptomatic and anatomical cure rates |
| Hintschich[5] | 2008 | Review | ||
| Marcet et al[6] | 2015 | Review | Understanding the demographics and factors linked to involutional entropion allows clinicians to better identify the condition and those most at risk. However, there is insufficient evidence to conclude that a short axial length is an independent risk factor for entropion. Recent advances in surgical techniques have fueled interest in minimally invasive procedures. It is crucial to address each patient’s unique anatomical abnormalities with precision | |
| Han et al[11] | 2019 | Retrospective interventional case series of 46 eyelids in 31 patients with involutional entropion and significant ocular irritation | During the mean follow-up period of 22.1 months (range, 12-34 months), 43 of the eyelids (93.5%) were successfully corrected. Two patients (3 eyelids) experienced recurrence: 1 had involutional entropion combined with a cicatricial component, and the other had blepharospasm and apraxia of eyelid opening related to Parkinsonism. No postoperative complications such as overcorrection, suture-knot exposure, or ocular irritation were observed | Mini-incisional entropion repair based on reinforcement of the lower eyelid retractors using transconjunctival buried sutures is quick, simple, and predictive for involutional entropion repair, and has a high success rate |
| Qurban and Kamil[12] | 2022 | Quasi-experiment study recruiting 50 patients with twenty-five patients in each group | Recurrence of the condition was observed in eight (32%) out of twenty-five patients in group A, who underwent the standard Weis surgical procedure, whereas only one (4%) out of the twenty- five patients of group B who underwent the modified surgical technique with external tamponade experienced recurrence | The modified surgical technique for entropion repair using an external tamponade has a favorable outcome with minimal recurrence and symptomatic relief |
| Cheung et al[14] | 2018 | Retrospective review of 52 eyelids of 46 patients who underwent pentagonal resection + inferior retractor plication for treatment of involutional entropion | A total of 52 eyelids of 46 patients received pentagonal resection + inferior retractor plication. None had recurrence of entropion, 1 (2.1%) had residual entropion, 2 eyelids (4.4%) had lower eyelid notching, 1 eyelid (2.2%) had infection and 1 eyelid (2.2%) had overcorrection. The overall success rate was 90.4% | Combined pentagonal resection + inferior retractor plication is an effective surgical procedure for primary involutional entropion with low recurrence rate; the authors report eye-lid notching as a complication |
| Koreen et al[17] | 2009 | Retrospective interventional case series (35 eyelids, 26 patients) | The success rate of primary repair was 77% (27 of 35 eyelids) with a mean follow-up time of 2.5 +/- 1.9 years. Four eyelids (11%) underwent repeat grafting for recurrent entropion secondary to graft shrinkage (3 eyelids) and graft dislocation (1 eyelid) for a cumulative success rate of 89%. The remaining 4 eyelids (11%) had recurrent entropion that was managed surgically with a technique other than repeat grafting | Anterior lamellar recession with buccal mucous membrane grafting is an effective surgical approach for the treatment of moderate to severe cicatricial entropion |
| Malhotra et al[18] | 2012 | Retrospective, 5-year, single-center, consecutive case series of patients with lower eyelid cicatricial margin entropion (21 eyelids, 19 patients) | The study included 21 eyelids from 19 patients (mean age 577 years) with cicatricial entropion: 38% of eyelids required a second procedure within a year, with 10% and 5% needing a third and fourth within three years. Common revisions were anterior lamellar repositioning, mucous membrane grafts, and everting sutures. Three patients had significant inferior fornix loss, and 90% of eyelids showed improvement after repeated surgeries, with mucosal grafts used in some cases. Lower eyelid elevation was 1 mm in 32% of patients, and lateral retraction improved in 47% | Lower eyelid gray-line split, inferior retractor recession, lateral-horn lysis, and anterior lamella repositioning is of value as a lash-preserving procedure in moderate-to-severe cicatricial lower eyelid entropion, particularly where tarsoconjuctival contraction or eyelid margin distortion exists |
| Kadyan et al[19] | 2010 | Prospective interventional case series; 7 patients, 9 procedures | Residual lashes were noted in three patients. In two cases, the lashes were isolated and managed successfully by a single electrolysis treatment. One patient needed further anterior lamellar excision for residual remnant of trichiatic cilia at the lateral edge of the lid. All patients were satisfied with their post-operative appearance. None of the patients showed exacerbation of disease or needed additional immunosuppression as a consequence of the lid surgery | Anterior lamellar excision with spontaneous granulation is a straightforward and effective method for managing aberrant eyelashes. This technique minimized the risk of disease exacerbation, particularly in cases of ocular cicatricial pemphigoid, by limiting conjunctival manipulation. Additionally, it reduced post-operative lash-globe contact, enhancing patient outcomes |
| Wu et al[20] | 2010 | Retrospective consecutive case series of 26 eyelids with severe, recurrent, or segmental cicatricial entropion | The functional success rate was 90.5%, and the cosmetic success rate was 100% | The eyelash resection procedure is a safe, effective, and cosmetically acceptable procedure for treatment of severe, recurrent, or segmental cicatricial entropion |
| Chi et al[22] | 2016 | Consecutive series of 27 eyelids (15 upper and 12 lower eyelids) of 18 patients (9 men and 9 women) | The success rate was 81.8% (22 of 27 eyelids). Complications included eyelid margin notching (n = 1) and blepharoptosis secondary to avascular necrosis of the distal marginal fragment (n= 1), both were corrected by minor surgical intervention | Modified tarsotomy is effective for the correction of severe cicatricial entropion |
| Singh et al[25] | 2021 | Case series (Six eyelids of five patients) | Entropion resolved in all patients with restoration of eyelid margin and reduction in ocular discomfort. Trichiasis was present in all six eyelids (100%) preoperatively and resolved completely in all but one case (83% success rate) with three residual focal trichiatic lashes in the temporal area, which was successfully managed with radiofrequency ablation. There were no recurrences of trichiatic or distichiatic lashes at a median follow-up duration of 16 months (range, 12-18 months) | Labial mucosa can be effectively used to resolve recurrent cicatricial entropion by spacing the anterior lamella and reconstructing the lid margin and posterior lamella, leading to a low recurrence rate |
| Takahashi et al[26] | 2014 | Retrospective case series (3 patients with congenital entropion); authors also measured the diameters of the pre tarsal Orbicularis Oculi Muscle fibers in these patients and compared them with those measured in the previously reported 67 eyelids of 41 Japanese patients with congenital epiblepharon | Successful correction was achieved in all three patients without recurrence during 12-months of follow-up. No patient exhibited lower eyelid ectropion or lower eyelid retraction. The mean diameter of the pretarsal Orbicularis Oculi Muscle fibers was 21.9 μm (range, 20.5-23.7 μm), which was not significantly different from that of the congenital epiblepharon (25.3 μm; range, 18.1-34.7 μm; P = 0.272, Mann-Whitney U test) | Posterior layer advancement of the lower eyelid retractor is a useful surgical option for treatment of congenital entropion. No histological evidence of pretarsal Orbicularis Oculi Muscle hypertrophy was shown in congenital entropion, which demonstrated that debulking of the pretarsal Orbicularis Oculi Muscle may not be significant for correction of this entity |
| Huang et al[27] | 2023 | Comparison prospective study; ninety-six participants (180 eyes) with congenital lower eyelid entropion diagnosed between January 2019 and April 2021 were included in this study. The patients were divided into Group A (cutaneous orbicularis oculi excision treatment) and Group B (inferior eyelid margin fixation treatment) | No significant difference in age, sex, and eyes distribution in both groups. And higher efficiency rate was found in Group B (P < 0.05). And Group A had a higher recurrence rate in the follow-up after surgical treatment (P < 0.05) | The authors modified inferior eyelid margin fixation of the orbicularis eyelid muscle treatment is an ideal procedure with a high degree of efficacy and low recurrence rate in patients with congenital lower eyelid entropion |
| Khuu et al[28] | 2023 | Retrospective chart review. Twelve patients (19 eyelids). The mean patient age was 7.1 ± 6.1 years (range, 0.2-22 years) | The described entropion repair technique was successful and without recurrence in 17 eyelids (89%). There were no cases of ectropion, lid retraction, or other complications. There were two eyelids (11%) that had entropion recurrence after first procedure. Repeated repair resulted in success with no recurrence at last follow-up | Subciliary rotating sutures combined with a modified Hotz procedure effectively correct congenital lower eyelid entropion. Since this technique avoids manipulating the posterior layer of the lower eyelid retractors, it is beneficial when retractor reinsertion provides insufficient improvement. It also helps minimize the risk of eyelid retraction and overcorrection in specific cases |
| Burton et al[29] | 2015 | Review | No trials specifically evaluated whether interventions for trichiasis prevent blindness, but some showed modest vision improvement. Full-thickness incision of the tarsal plate with lash-bearing lid margin rotation was the most effective technique, preferably performed in the community. Both ophthalmologists and trained ophthalmic assistants can perform the surgery, and results were comparable using silk or absorbable sutures. Post-operative azithromycin improved outcomes, with low recurrence rates overall | |
| Singh[30] | 2022 | Review | Treatment options for congenital and acquired distichiasis are similar, with no specific algorithms available. Managing acquired distichiasis in cicatrizing ocular surface diseases is challenging, with current treatments yielding success rates of 50%-60%. Procedures like electroepilation or direct cryotherapy are less effective compared to surgical excision of distichiatic lashes, which involves splitting the anterior and posterior lamella under direct visualization. Marginal tarsectomy, with or without a free tarsoconjunctival graft, has shown favorable results in both congenital and acquired cases. However, the exact differences in normal vs distichiatic lashes, including depth and growth patterns, remain unclear. Research into the depth of distichiatic eyelashes could improve the outcomes of procedures like cryotherapy or radiofrequency-assisted epilation, which are currently done without precise visualization | |
| Woo and Kim[31] | 2016 | Review | While epiblepharon may improve as the face grows, surgical correction is necessary when significant corneal damage occurs due to lash contact. Surgical treatment should prioritize techniques that are both effective and low-risk, while avoiding the formation of a lower eyelid crease | |
| Ma et al[33] | 2020 | Comparative study | In the surgical and nonsurgical groups, the baseline astigmatism magnitude was similar (2.22 ± 1.39 and 2.26 ± 1.46 D, P = 0.87). Complete resolution of keratopathy at 6 months was 71.4% and 11.5%. The astigmatism magnitude in the surgical group differed among baseline and 3 months (2.25 ± 1.23 D) and 6 months postoperatively (1.97 ± 1.28 D) (P = 0.001) | The surgical group exhibited greater improvement in keratopathy compared to the nonsurgical group, despite having more severe baseline pathology. A reduction in with-the-rule astigmatism was observed six months postoperatively, particularly in patients with higher initial astigmatism. However, the extent of this change was minimal, and the overall outcomes did not significantly differ from those of nonsurgical treatment |
| Sung and Lew[34] | 2019 | Retrospective was series study including 72 eyelids of 36 children with epiblepharon and epicanthal folds | Eyelid contour was normalized and the cilia touch was resolved after the epicanthal tension-releasing procedure | The epicanthal tension-releasing procedure combined with orbicularis oculi ring myotomy resulted in positive surgical outcomes. Clinical findings aligned with pathology and the success of the procedure suggest that medial epicanthal fibrosis is the primary cause of epiblepharon and epicanthal folds |
| Yan et al[35] | 2016 | Retrospective case control (67 patients-mean age, 5.7 ± 2.6 years- and 178 controls. All patients presented with epicanthus | All patients showed successful surgical outcomes according to improvement of symptoms and lack of cilia-cornea contact. There were no cases of recurrence or other complications | Obesity can exacerbate lower eyelid epiblepharon, which can be effectively treated using the rotating suture procedure and the L-plasty procedure. The L-plasty procedure is particularly recommended for patients who also have significant epicanthus |
| Lailaksiri et al[38] | 2024 | Retrospective cohort study; 30 patients (76% females; average age 608 ± 12 years) with facial palsy who underwent implantation of either the traditional pretarsal gold weight or a new supratarsal model | The new model group had significantly better eyelid contour, less weight prominence, less weight migration and less eyelid ptosis than the traditional model group. Improvement of lagophthalmos was not statistically significant between the two groups. The 24-month reoperative rate was 53.3% in the standard group vs 13.3% in the new model group | The author’s newly designed supratarsal gold weight showed superior postoperative outcomes than the standard traditional model |
| Chung et al[39] | 2020 | Case report | Severe lagophthalmos successfully released with pentagonal wedge resection, fat redistribution, and full-thickness skin graft | |
| Medina et al[40] | 2022 | Case report | Multiple contributing factors for severe ectropion of left lower eyelid treated with lateral tarsal strip procedure and full-thickness skin graft | |
| Ghafouri et al[43] | 2014 | Retrospective review of case series (forty-one lower eyelids of 31 patients with involutional ectropion underwent surgical repair) | Surgical success with anatomical correction of involutional ectropion was achieved in 39 of 41 eyelids (95.1%). There were no perioperative or postoperative complications. Two of 41 (4.9%) eyelids had recurrence of ectropion 7 and 18 months after the procedure | The combination of a lateral tarsal strip and internal retractor reattachment using full-thickness eyelid sutures effectively resolves horizontal eyelid laxity and tarsal instability, making it a successful technique for correcting involutional ectropion of the lower eyelid |
| Vahdani et al[44] | 2021 | Retrospective case-note review; twenty-four eyelids of 21 treated patients (17 males; 81%) with lower eyelid cicatricial ectropion | Comparing the outcomes of modified Bick’s procedure + full-thickness skin grafting vs modified Bick’s procedure + monopedicle myocutaneous flap there was no statically significant difference in terms of anatomical (P = 0.48) and functional (P = 1.0) success rates. No cases of failure or recurrence were noted during the follow-up period | Anterior lamellar deficit ectropion arises without visible scarring. It is essential to thoroughly address both the horizontal laxity and the anterior lamellar deficit linked to this condition to reduce the chances of early failure and recurrence. The combination of medialized buccal pad (modified Bick’s procedure) with full-thickness skin graft or myocutaneous flap is a safe and effective treatment for this type of "cicatricial ectropion" and demonstrates a low rate of early recurrence |
| Korteweg et al[45] | 2014 | Cross-sectional outcome (30 cases of paralytic ectropion) | Lateral periosteal flap canthoplasty assessed through Ectropion Severity Score proved to be reliable and sensitive to the presence of ectropion. Significant improvement of the ectropion sequelae was measured after a mean follow-up period of 2 years. In 3 cases (13%), a revision procedure was necessary because of relapse of lower eyelid sagging after a mean time of 1.9 years | The periosteal flap canthoplasty is an effective technique that provides lasting results for patients with paralytic ectropion. This same periosteal flap can also be utilized in revision procedures |
The initial category encompasses research that evaluates the effectiveness of several surgical techniques, including lateral tarsal strip surgery, Quickert-Rathbun sutures, and full-thickness wedge resection, in treating entropion and ectropion. Research indicates that whereas all techniques enhance eyelid alignment, strategies that include horizontal lid tightness have reduced recurrence rates. The second category includes clinical trials that evaluate post-surgical success rates, complication profiles, and patient-reported outcomes after various procedures. Interventions using preoperative imaging, such as OCT, have demonstrated enhanced precision in surgical planning, hence decreasing postoperative problems. Finally, research in the third category underscores the significance of histological analysis and multidisciplinary cooperation in enhancing patient outcomes. These studies demonstrate that the integration of surgical procedures with conservative treatments, like lubricating eye drops and botulinum toxin injections, can improve both functional and cosmetic outcomes. These studies collectively offer a thorough overview of the changing landscape of surgical procedures for corneal diseases, emphasizing the necessity for customized methods based on unique patient presentations.
In this section we summarize evidence collected concerning the common conditions associated with corneal damage requiring surgical approach (trichiasis, lagophthalmos, distichias, epiblepharon, entropion, lagophthamos, ectropion). From a diagnostic and an outcome measurement perspective, advanced imaging modalities, including OCT and Ultrasound Biomicroscopy, have been beneficial in evaluating the anterior segment of the eye assessing corneal lesions resulting from eyelid diseases: OCT enables high-resolution cross-sectional imaging, allowing for precise preoperative evaluation of corneal integrity and stromal involvement. Ultrasound Biomicroscopy provides deeper tissue penetration, assisting in the assessment of posterior segment involvement and structural changes. These techniques assist in identifying surgical strategies and post-operative surveillance, enhancing patient outcomes.
Collaboration among ophthalmologists, plastic surgeons, and dermatologists is crucial for enhancing the surgical treatment of corneal lesions resulting from eyelid disorders. Ophthalmologists provide specialized knowledge in corneal health and the care of ocular surface diseases, whilst plastic surgeons provide sophisticated reconstructive methods to enhance eyelid functionality. Finally, dermatologists are essential in diagnosing systemic disorders that lead to cicatricial alterations potentially affecting the cornea. A multidisciplinary approach guarantees thorough care, minimizing complications, recurrence risk and improving patient safety.
Entropion, characterized by the inward rotation of the eyelid, may impact both or one eye, with a greater prevalence in the lower lid. It is categorized in 4 primary types: Cicatricial, acute spastic, congenital, and age-related (involutional). The symptoms of this disorder include ocular redness and soreness, photophobia, sensitivity to wind, periorbital skin laxity, excessive lacrimation, and diminished vision, particularly in cases of corneal injury[3-6]. A retrospective investigation of the Australian population revealed that, involutional entropion exhibits modest corneal abnormalities, with 95.1% of cases showing either normal corneal epithelium or superficial punctate keratopathy. Vision loss is an uncommon consequence, occurring in 1% of participants in this study, all of whom had previous corneal disease[7].
Various surgical techniques have been delineated for the treatment of entropion[3-6]. The selected treatment must be suitable for the type of entropion being treated. The following are the most prevalent procedures employed in management[6].
Spastic eyelid closure enables the orbicularis oculi muscle to dominate the opposing function of the lower eyelid retractors, causing the lid margin to invert and exacerbating ocular surface irritation due to the mispositioned eyelashes. Spasm of the muscle of Riolan, resulting from irritation, and insufficient support of the eyelid by the globe are the primary pathophysiological changes. The treatment strategy initially necessitates the elimination of the source of discomfort. Minimal botulinum toxin treatments (about 5 U of BOTOX®) are highly successful to treat spastic entropion by attenuating the oculi muscles (mainly the pretarsal orbicularis).
Quickert-Rathbun sutures can be considered for numerous instances of spastic entropion and certain occurrences of involutional entropion when the patient declines or is medically unfit for more decisive interventions. Full-thickness lid sutures, typically composed of gut, are employed anteriorly from the inferior fornix towards the lashes in order to rotate the eyelid edge away from the globe. The tissue response to the intestinal suture facilitates the formation of a scar in the eyelid that preserves the eyelid in an everted posture. Skin and muscle excision procedures, along with Wheeler’s operation, are alternative options when initial treatments fail to induce disease regression; Wheeler orbicularis trans
Anatomical causes responsible for entropion due to aging encompass laxity of the lids horizontally, overriding of the oculi muscle (mainly orbicularis) and wrong insertion of the lower eyelid retractors. The alterations, mainly induced by aging, lead to the inward rotation of eyelid margins, causing the eyelashes to contact the external eyeball including the cornea. This continual irritation results in harm to the ocular surface structures. Orbicularis oculi muscles, tarsus, lower lid retractors, and canthal tendons ensure the horizontal stability of the lower lid. Any deterioration or flexibility in these components may result in the inward turning of the lid. The lower eyelid retractors similarly confer stability vertically, in which laxity may lead to rotation inwardly. The pinch test is commonly employed to evaluate the horizontal laxity severity. Diverse non-surgical and surgical interventions have been utilized to address senile entropion, contingent upon anatomical deficiencies, and to alleviate irritation resulting from misaligned eyelashes induced by the inward-turned eyelid. Conservative methods encompass the administration of lubricating eye drops, the application of contact lenses, and the injection of Botulinum toxin. Nevertheless, conclusive treatment generally necessitates surgical intervention.
Patients typically exhibit gyration of the posterior eyelid retractors, resulting in eyelid inversion akin to spastic entropion. The involution of the orbital soft tissues, especially the orbital fat, may result in involutional enophthalmos, subsequently causing an abberant eyelid posture with entropion.
Various surgical techniques are utilized to rectify involutional entropion. One of the most straightforward and accessible methods entails the application of full-thickness lid-everting sutures, referred to as Quickert sutures. This approach produces anterior rotational torque, modifying the orientation of eyelashes and inhibiting the preseptal orbicularis oculi muscle from dominating. The principal disadvantage is its elevated recurrence rate. A commonly employed technique is the transconjunctival or transcutaneous reinsertion of the lower eyelid retractors, referred to as Jones retractor plication. The method entails the reattachment of the separated lower eyelid retractors to the tarsal plate anterior margin. Although it has the advantage of direct visibility of the afflicted structures and facilitates the excision of the surplus skin and of the pretarsal orbicularis muscle, it is frequently criticized for its intricacy, time demands, and risk in causing eyelid retraction or secondary ectropion.
Surgical alternatives vary from transient, office-based interventions, such as the Quickert suture technique, to more enduring remedies, including the Weis operation, lateral canthal tendon tightening, and lateral tarsal strip method. The latter encompasses all 3 senile entropion etiological elements. These include lower eyelid retractor disinsertion, horizontal eyelid laxity, and overriding orbicularis oculi muscles[6,7].
Early attempts by Bick resulted in development the term "orbital tarsal disparity," associating eyelid flexibility and age-related orbital volume reduction with ectropion and entropion. He demonstrated that lower eyelid entropion may be temporarily rectified by injecting saline into the muscle cone; nonetheless, lid shortening has been considered as a better and more effective treatment. The surgery entails a complete tissue triangular excision at the lateral canthus, followed by the reattachment of the tarsal plate to the lateral canthal tendon, contingent upon eyelid flexibility[8]. In 1977, Tenzel et al[9] introduced a lateral canthal tendon sling for the treatment of involutional ectropion, which was subsequently refined by Anderson into the "tarsal strip" method. Both the tarsal strip and the Bick's treatments laterally shorten the eyelid; however, Bick's technique circumvents the lateral canthal tendon and does not conceal the tarsal plate[10].
Han et al[11], reported a non-incisional blepharoptosis correction method utilizing buried transconjunctival sutures (which plicate the Müller and superior levator palpebral muscles and may be used in advancing the levator aponeurosis to ameliorate blepharoptosis), posited that, given the anatomical similarity between the upper and lower eyelids—where the Müller and levator palpebral muscles in the upper lid correspond to the lower eyelid retractor in the lower eyelid—a non-incisional correction technique for upper lid blepharoptosis can be adapted to address lower eyelid involutional entropion by reinforcing the attenuated or dehisced lower eyelid retractor. The author employed a buried-suture method on the lower lid to fortify the weakened or disinserted lower eyelid retractors, utilizing three knots for precise defect correction. To avert overriding of the preseptal orbicularis oculi muscle, the technique involved excising an orbicularis oculi muscle strip through a minimal subciliary incision thereby integrating the underlying orbicularis oculi muscle into the sutures for optimal closure of the skin.
Qurban et al[12] conducted a quasi-experimental study proposing a modified surgical approach for entropion repair with an external tamponade, resulting in good outcomes, little recurrence, and symptomatic alleviation.
The management of senile entropion may necessitate the correction of horizontal laxity through medial and/or lateral canthal tightening, plication of lower eyelid retractors (according to Jones), transmarginal rotation (according to Weis that involves a full-thickness horizontal eyelid incision), and tucking of palpebral ligaments; a minor resection of the pretarsal orbicularis oculi may be performed simultaneously to avert further tarsal overriding.
The Weis method integrates a transverse full-thickness blepharotomy with everted sutures. Everything sutures the appropriate vertical eyelid laxity by traversing the retractor layer and constricting the lower eyelid retractors. Blepharotomy forms a scar that links the conjunctiva, skin, and the pretarsal and preseptal orbicularis oculi muscles. Collectively, these approaches inhibit the preseptal orbicularis from dominating the pretarsal segment. The Weis method fails to treat horizontal lid laxity, which arises from the looseness of the canthal tendons and tarsal plate. Horizontal laxity may be rectified with eyelid-shortening techniques, including full-thickness wedge resection or lateral tarsal strip techniques. It is generally acknowledged that rates of recurrence tend to increase when horizontal laxity is unaddressed. In cases devoid of horizontal laxity, a straightforward reattachment of the retracted lower lid retractors may be adequate. Addressing horizontal laxity is essential to reduce the likelihood of recurrence, especially when the snapback test yields a positive result. A comprehensive preoperative assessment is crucial to exclude horizontal laxity and guarantee excellent results from the Weis operation, hence minimizing the likelihood of early recurrence[13].
Cheung et al[14] advanced procedure according to Hill-a technique that entails a shortening of the lateral lower lid through full-thickness excision, then fixation of an orbicular muscle strip to the lower tarsal plate border, and curettage of the anterior tarsal plate to avert orbicularis muscle overriding—by integrating pentagonal resection (PR) and inferior retractor plication (IRP) for the primary treatment of lower eyelid laxity with involutional entropion in a Chinese cohort. The combination of PR and IRP constitutes an effective surgical technique for addressing primary involutional entropion, with a minimal risk of recurrence. However, there exists a potential danger of eyelid notching following the procedure.
Cicatricial entropion can be defined as tarsoconjunctival scarring resulting from conditions that include ocular cicatricial pemphigoid, chronic blepharitis, trachoma, Stevens-Johnson syndrome, prolonged use of topical glaucoma medications, and prior surgical interventions. Additional indicators comprise trichiasis, forniceal shortening, and the development of symblepharon[15].
Cicatricial entropion presents a challenging treatment dilemma, as various surgical methodologies exhibit varying degrees of efficacy. It is essential that the inflammation process is not in an acute phase in individuals with Ocular Ciucatricila pemphigoid–a persistent autoimmune condition marked by advancing conjunctival fibrosis, resulting in cicatricial entropion and symblepharon development- prior to any conjunctival surgery. Manipulating the conjunctiva in these patients may provoke a return of inflammation, potentially resulting in the failure of the surgery. The choice of surgical technique is contingent upon parameters like the extent and degree of eyelid retraction, entropion, fornix and tarsus involvement, keratinization, distortion of the eyelid edge, and the advancement of the underlying pathology. Surgical techniques can be categorized into four types: (1) Posterior lamella lengthening; (2) Grayline splitting of the posterior and anterior lamellae; (3) Lid margin eversion or rotation; and (4) A combination of the 3 methods. Grayline splitting of the posterior and anterior lamellae encompasses lamellar splitting with anterior lamella excision or recession, advancement of the posterior lamella, and recession of the anterior lamella accompanied by advancement of posterior lamella; however, in the presence of metaplastic lashes in the posterior lamella, the latter technique is inapplicable. Lengthening of the posterior lamella requires the application of middle and posterior lamella grafts to achieve a flat surface for proper eye contact, hence extending the duration of the surgical procedure[16-21].
Kersten et al[15] characterized transverse tarsotomy and lid margin rotation as straightforward and dependable interventions for mild to moderate cicatricial entropion, achieving a success rate of 94%, but the success rate diminishes for severe cicatricial entropion.
Chi et al[22] refined the transverse tarsotomy technique for severe cicatricial entropion by incorporating a straightforward modification that entails 'two back cuts' at each end of the transverse tarsotomy. These back cuts facilitate greater mobility of the distal tarsal fragment, potentially enhancing the success rate in patients with severe cicatricial entropion. Kadyan et al[19] stated that spontaneous granulation with anterior lamellar excision in seven patients with ocular cicatricial pemphigoid was a straightforward and successful surgery; nonetheless, three individuals had residual lashes.
Wu et al[20] found that the functional success rate of the lamellar splitting with eyelash removal method exceeded 90% for severe, recurring, segmental cicatricial entropion. The limitation of this approach is its inapplicability in cases of metaplastic eyelashes within the posterior lamella.
Studies by Goldberg et al[23] reported an 80% success rate for a shared mucosal graft in their case series including severe cicatricial entropion, based on posterior lamellar lengthening. In the case series by Gu et al[3], posterior lamellar lid reconstruction and terminal tarsal rotation utilizing dermis allograft (acellular) for patients with severe cicatricial entropion was effective in 14 of 16 cases. Seiff et al[24] documented a functional success rate of 100% for the rotation of the upper eyelid tarsal margin and the extensive advancement of the posterior lamellae, integrating eyelid margin rotation with the lamellar division of the anterior and posterior lamellae.
Employing labial mucosa to separate the anterior lamella and repair both the posterior lamella and the eyelid border is an efficacious method for addressing recurrent cicatricial entropion with a minimal recurrence rate[25].
Congenital entropion is an uncommon disorder that predominantly impacts the lower eyelid. It is linked to multiple developmental defects, including hypertrophy of the pretarsal orbicularis oculi muscle, deficits in the tarsal plate, facial nerve paralysis, and dysgenesis of the lower eyelid retractors. It may also manifest concurrently with microphthalmos. In contrast to infantile entropion, which results from fat accumulation in well-nourished children and typically resolves spontaneously, congenital entropion necessitates meticulous distinction owing to its unique underlying causes[4-6].
The advancement of the posterior layer located in the lower lid retractors is an effective surgical method in addressing congenital entropion. Takahashi et al[26] showed in their case series that histological investigation revealed no signs of pretarsal orbicularis oculi muscle hypertrophy in cases with congenital entropion, indicating that diminishing this muscle mass may not be necessary to rectify the problem.
A revised surgical technique involving fixation of the orbicularis oculi muscle at the inferior eyelid edge was assessed for the treatment of congenital entropion of the lower lid. A study including 180 eyes of 96 patients categorized participants in 2 groups: The first group had excision of the cutaneous orbicularis oculi, while the second group underwent the modified surgical method. The second group exhibited a better success rate and a diminished rate of recurrence compared to the first group (P < 0.05). The results indicate that this improved technique can be an efficacious and dependable method for addressing congenital lower eyelid entropion with reduced recurrence rates[27].
The application of subciliary rotating sutures alongside a modified Hotz procedure constitutes an efficient method for rectifying congenital lower eyelid entropion. This procedure is advantageous in situations where retractor reinsertion does not yield adequate enhancement, as it circumvents manipulation of the lower lid retractor posterior layer. Fur
Trachomatous trichiasis—the main cause of trichiasis—represents a critical ophthalmic public health issue, particularly in sub-Saharan Africa. Trichiasis is characterized by abnormally positioned lashes, which grow back toward the ocular surface, touching the conjunctiva or cornea.
Surgical intervention remains the mainstay of treatment, with several techniques described in the literature[29]. One of the more effective procedures involves bilamellar rotation of the tarsal that incises the tarsal plate full thickness and rotates the lash-bearing tarsus to evert the eyelid margin. Another option consists of posterior lamellar tarsal rotation (Trabut procedure), where sutures are placed above the lashes. The literature found no definitive advantage of one method over the other.
While both posterior lamellar and bilamellar tarsal rotation procedures are widely used in regions endemic of trachoma, there is no supporting evidence to suggest the superiority of one technique. Though bilamellar surgery can result in a higher rate of eyelid exposure and overcorrection, these risks remain insignificant. The procedures are both considered to be safe, in which post-operative trichiasis tends to be the most common complication reported in studies.
Non-surgical interventions, such as cryotherapy and electrolysis, used to treat minor trichiasis by targeting lash destruction, have shown lower success rates in preventing recurrence compared to bilamellar tarsal rotation surgery. Given these techniques' high costs and maintenance difficulties, they are not recommended for routine use.
While various surgical methods for trichiasis due to trachomatous exist, posterior lamellar and bilamellar tarsal rotations are commonly employed, with no definitive evidence favoring one over the other. Both are effective and safe, but post-operative trichiasis remains challenging, and non-surgical approaches offer limited efficacy[29].
Distichiasis is an eyelash abnormality in which lashes originate from meibomian gland orifices, differing from normal eyelashes that arise from the skin. It is distinct from trichiasis and other disorders like tetrastichiasis and tris trichiasis. Distichiatic lashes may cause signs and symptoms due to contact to the ocular surface and may vary in appearance. There are two types: Congenital and acquired.
Surgical management of distichiatic eyelashes involves various techniques to address the aberrant cilia. These include excision, cryotherapy, and electrocautery, often performed under high magnification to ensure precision. Historical approaches date back to 1880, where posterior and anterior lamellas were split, and the tarsoconjunctival ciliary-bearing strip was removed, giving rise to a bare eyelid margine. Later modifications included grafting of the mucous membrane, proposed in 1913 by Begle, to reduce complications such as ectropion and entropion. Subsequent methods proposed in 1960s, like Fox’s technique of conjunctival flap removal and anterior lamella reattachment, showed positive outcomes but lacked data on long-term outcomes.
The transconjunctival trapdoor method was proposed to circumvent marginal complications and entropion. It allows the direct cilia root removal without the need for tarsal excision or grafting. However, its effectiveness remains undetermined due to incomplete recurrence data. In elderly patients with dermatochalasis, redundant skin excision offers an additional aesthetic benefit.
Eyelash trephination, using a Sisler ophthalmic micro trephine, is another method. It has shown a 38% rate of recurrence in patients with acquired distichiasis and trichiasis, likely due to the uncertain depth of abnormal lash roots. Direct excision along the lash's vertical axis has been successful in congenital distichiasis, achieving an 80% success rate, but it is time-consuming, requiring up to 1.5 hours per eyelid.
For acquired distichiasis with cicatricial entropion, anterior lamellar recession combined with mucosal grafting is used to reconstruct the excised area. Recurrences, trichiasis, and eyelid malposition, such as entropion, remain common complications. The unknown depth of distichiatic eyelashes poses a significant challenge, particularly in acquired cases. Advances in imaging technology, like high-frequency ultrasound, can enhance the precision of treatment options by enabling the complete removal of the cilia including the roots[30].
Epiblepharon—in—rolling of lashes and the lid margin over the superior tarsal edge—is commonly observed in East-Asian children, and as the population grows, so does the demand for surgical intervention. In managing this condition, surgeons must understand the aesthetic preferences and specific needs of Asian patients[31]. Recent findings indicate a high prevalence of astigmatism in these patients, which can lead to amblyopia; thus, early surgery and visual rehabilitation are crucial[32]. The pathophysiology of epiblepharon involves various etiological factors, and while Western surgical methods are commonly aimed at creating a lower lid crease, this can be undesirable in Asian patients. Careful selection of surgical techniques is essential to minimize muscle and skin resection, reducing the risk of eyelid retraction and ectropion. Although epiblepharon may resolve naturally over time, surgical treatment correction is necessary in patients with severe damage to the cornea due to eyelash contact. Efficient surgical techniques should prioritize reduced rates of complications and limit the formation of new lid creases[31].
According to a comparative study by Ma et al[33] the improvement in keratopathy observed in the surgical cohort surpassed that of the nonsurgical group, despite the greater baseline severity in the former. A reduction in with-the-rule astigmatism was noted at six months postoperatively, particularly in patients with higher baseline astigmatism. However, the magnitude of this change remained minimal, and the overall outcomes did not differ significantly from those achieved with nonsurgical management. Consequently, surgical intervention should primarily be indicated based on the severity of symptoms and the extent of keratopathy.
Among different techniques methods, Sung et al[34] reported successful surgical outcomes with orbicularis oculi ring myotomy and epicanthal tension-releasing procedures. The clinical correlations with altered findings and satisfactory outcomes of the method suggested that fibrosis of the medial epicanthal is the main clinical factor that causes epicanthal folds and epiblepharon. Obesity may exacerbate lower lid epiblepharon that may be effectively addressed with the L-plasty procedure and the rotating suture method. The L-plasty procedure tends to be used in cases that also show significant epicanthus[35].
Lagophthalmos refers to the incomplete or impaired closure of the eyelids, a condition that disrupts normal eyelid function. Complete eyelid closure, along with an intact blink reflex, is critical for maintaining a stable tear film and preserving ocular surface health. Patients with an inability to blink effectively or fully close their eyelids are predisposed to tear film evaporation, corneal exposure, and the subsequent development of keratopathy due to exposure. If left untreated, this may progress to ulceration of the cornea and, ultimate perforation in severe cases. Early recognition of the clinical symptoms and signs of lagophthalmos, followed by early diagnosis of the underlying causes, is essential to initiate appropriate treatment and management.
Diagnosing lagophthalmos requires assessing clinical history for surgeries, trauma, infections, or systemic conditions, with sudden facial motor loss often indicating nerve paralysis. Evaluation includes examining cranial nerve function, incomplete blinking, exophthalmos and lid malposition. Slit lamp evolution of the tear film stability and of the corneal surface using tear breakup time assessment and fluorescein staining are fundamental.
The primary etiology of lagophthalmos tend to be facial nerve paralysis, resulting in paralytic lagophthalmos; facial nerve paralysis could be caused by many underlying etiologies: Infection, trauma, tumor, metabolic disorder, toxic agents, iatrogenic (for example as a consequence of eyelid surgery), neurological, congenital, idiopathic, cicatricial, nocturnal[36].
Eyelid retraction is frequently associated with thyroid eye disease, in which the Müller muscles are stimulated by hyperthyroidism, leading to a typical bilateral asymmetric stare. The infiltration of mast cells and lymphocytes, followed by fibroblastic proliferation in the levator and Müller muscles, give rise to superior temporal lid retraction, often with lateral flaring[37]. In contrast, facial nerve (seventh cranial nerve) paralysis leads to lagophthalmos, typically without eyelid retraction. This paralysis, seen in conditions such as Bell’s palsy, sarcoidosis, ischemic events, or post-surgical outcomes, causes orbicularis oculi dysfunction, resulting in unopposed levator muscle action, lower lid ectropion, and epiphora due to increased reflex tear secretion and deficient lacrimal pump function from ocular surface exposure.
The surgical treatment of lagophthalmos is based on the severity and duration of the condition. In cases of corneal exposure with anticipated recovery within weeks, a temporary tarsorrhaphy may be an effective choice. In most instances, the cornea can be sufficiently safeguarded by closing the lateral one-third of the eyelids. A minimal aperture should be maintained to facilitate ongoing evaluation of the cornea and the administration of necessary topical medicines.
In instances of paralytic lagophthalmos where full eyelid closure is impaired, the insertion of a gold or platinum weight into the upper eyelid may be warranted. This method utilizes gravity to improve eyelid closure. The ideal implant weight must enable complete eyelid closure and opening, without causing ptosis in the primary gaze. Traditionally, gold weights are placed anterior to the tarsus (pretarsal area), specifically tailored for the trapezoidal tarsal shape observed in Caucasian eyes. However, in patients with a sickle-shaped tarsus, such as those of Asian descent, visible implant edges often result in suboptimal cosmetic outcomes and higher incidences of implant exposure, infection, and the need for reoperation. Recent advancements favor supratarsal placement, as this approach has demonstrated reduced visibility, lower exposure risk, and improved postoperative outcomes compared to the conventional technique[38].
In lagophthalmos resulting from upper eyelid retraction, as seen in thyroid eye illness, recession of the levator palpebrae superioris and Müller’s muscles constitutes an effective surgical intervention. Options for postsurgical eyelid shortening comprise full-thickness skin grafts or advancement flaps. Moreover, scar band release and tarsal-sharing techniques are suitable for the management of cicatricial lagophthalmos. Laxity of the lower eyelid is noted in disorders such as facial nerve paralysis and floppy eyelid syndrome. Surgical therapies, including lateral tarsal strip procedures, improve the alignment of the lower eyelid with the globe, thereby decreasing scleral exposure and alleviating symptoms of epiphora[39,40].
When secondary to facial nerve paralysis lagophthalmos may require midface elevation or other facial reanimation procedures[41].
Ectropion denotes the outward turning of the lid margin, leading to inadequate lubrication and ocular exposure and. Patients can have signs and symptoms due to corneal dryness and inflammation. Although ultimate therapy is surgical, medicinal management offers temporary alleviation and symptomatic enhancement during the interval before surgery.
Involutional or age-related ectropion, the predominant variant, is linked to tarsoligamentous sling laxity, widespread elastin depletion, and orbicular atrophy. Surgery encompass blepharotomy with canthopexy, rotational sutures, lateral tarsal strip, and horizontal lid shortening or tightening, either medially, laterally, or both. A comprehensive under
Cicatricial ectropion occurs when anterior lamellar shortening from scar tissue induces traction, elongating the lid border and retracting it from the globe, akin to mechanical ectropion. Contributing variables encompass mechanical, thermal, and chemical injuries, dermatological conditions, eyelid surgery, or cosmetic interventions, frequently aggravated by actinic damage or mid-face decline resulting from habitual eye rubbing or aging.
The surgical management of cicatricial ectropion involves three essential steps: Relieving the radial strain of the lid margin, reducing the elongated lid margin to restore its appropriate alignment with the globe, and correcting the anterior lamellar insufficiency. Various eyelid shortening methods, such as pentagon excision, lateral tarsal strip, and lateral canthopexy, have been proposed to address horizontal eyelid laxity. However, recurrence or chronic ectropion rates may reach 43%, potentially due to insufficient repair of the anterior lamellar insufficiency or the choice of lid margin tightening techniques. Some surgical procedures produce more lasting results than others; nonetheless, accurate diagnosis and correction of both the lamellar deficit and the lid margin are crucial for durable success. The anterior lamellar restoration procedure seems to have a negligible impact on overall outcomes; nevertheless, studies demonstrate a significantly lower recurrence rate of ectropion in eyelids that underwent concurrent horizontal tightening and skin grafting. The Modified Bick’s Procedure has proven to be safe and effective in correcting horizontal eyelid laxity, particularly when augmented with a full-thickness skin graft or a mucous membrane conjunctival flap for the anterior lamella[44].
Congenital ectropion is an exceedingly rare condition sometimes linked with other defects, such as euryblepharon and blepharophimosis, characterized by inadequate anterior lamella, diminished tarsal rigidity, and suboptimal development of canthal tendons. The repair involves methods previously mentioned for other forms of ectropion, such as horizontal lid tightening/shortening and anterior lamella grafting[42].
The lower lid positionis determined by the interaction of the bony orbit and the globe e, gravitational forces, tissue elasticity, the lateral and medial canthal ligaments, in addition to the active activity of the orbicularis oculi muscle, with the deep lateral canthal tendon being essential. As tissue elasticity declines with age, the orbicularis oculi muscle increasingly assumes responsibility for sustaining lower eyelid stability. The abrupt loss of innervation, as shown in facial palsy, leads to paralytic ectropion, which is marked by lagophthalmos, and an elevated risk of exposure keratitis. Over time, paralysis may result in anterior lamella retraction, hence worsening the disease.
Reconstructive surgery for paralytic ectropion is used to realign the lower lid to enhance closure, enhance tear drainage, maintain ocular surface lubrication, diminish vertical aperture, while also improving aesthetic results. Due to the usual tissue laxity and elongation of lateral support systems, canthoplasty with horizontal eyelid shortening is frequently advised. The lateral tarsal strip method and its modifications are frequently employed. Nevertheless, conventional methods, such as suturing to the periosteum or perforating the orbital wall, have hazards including suboptimal outcomes or injury to the globe.
Employing a periosteal flap as a substitute for the deep lateral canthal ligament presents a more secure option. It offers robust, self-sustaining support without requiring suturing or drilling within the orbit, facilitating anatomical adjustment of the lid while reducing problems. This technique can be readily integrated with other treatments and is executable under local anesthesia[45].
The main aspect emerging from this brief review of related literature is the importance of addressing the innermost pathophysiological alteration proper of that specific corneal damaging eye-lid pathology: The peculiar anatomical structure concerned by the disorder has to be identified and any surgical procedure has to be tailored upon that. Furthermore, due to the complexity of illness presentation, multidisciplinary work between ophthalmologists and plastic surgeons is crucial to achieve stable long-term results. A comparative analysis of various surgical interventions for corneal lesions secondary to eyelid pathologies reveals substantial differences in efficacy, complication rates, and long-term outcomes. Techniques such as lateral tarsal strip surgery, Quickert-Rathbun sutures, and full-thickness wedge resection exhibit variable success depending on the underlying pathology. Lateral tarsal strip surgery demonstrates exceptional efficacy in correcting horizontal eyelid laxity, boasting high success rates and low recurrence; however, potential complications include overcorrection and lid malposition. Quickert-Rathbun sutures, commonly employed for spastic and involutional entropion, provide a minimally invasive approach with rapid symptomatic relief but are associated with a higher recurrence rate compared to more definitive surgical techniques. Full-thickness wedge resection, frequently indicated for severe eyelid malposition, offers durable correction but carries risks of scarring and post
| 1. | Willmann D, Fu L, Melanson SW. Corneal Injury. 2023 Jul 17. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing, 2025. [PubMed] |
| 2. | Tham YC, Li X, Wong TY, Quigley HA, Aung T, Cheng CY. Global prevalence of glaucoma and projections of glaucoma burden through 2040: a systematic review and meta-analysis. Ophthalmology. 2014;121:2081-2090. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5390] [Cited by in RCA: 4470] [Article Influence: 406.4] [Reference Citation Analysis (4)] |
| 3. | Gu J, Wang Z, Sun M, Yuan J, Chen J. Posterior lamellar eyelid reconstruction with acellular dermis allograft in severe cicatricial entropion. Ann Plast Surg. 2009;62:268-274. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 19] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 4. | Swamy BN, Benger R, Taylor S. Cicatricial entropion repair with hard palate mucous membrane graft: surgical technique and outcomes. Clin Exp Ophthalmol. 2008;36:348-352. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 18] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 5. | Hintschich C. Correction of entropion and ectropion. Dev Ophthalmol. 2008;41:85-102. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 22] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 6. | Marcet MM, Phelps PO, Lai JS. Involutional entropion: risk factors and surgical remedies. Curr Opin Ophthalmol. 2015;26:416-421. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 21] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 7. | Parsons SR, O'Rourke MA, Satchi K, McNab AA. Corneal Complications Secondary to Involutional Entropion at Presentation. Ophthalmic Plast Reconstr Surg. 2022;38:593-595. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 8. | Bick MW. Surgical management of orbital tarsal disparity. Arch Ophthalmol. 1966;75:386-389. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 94] [Cited by in RCA: 78] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 9. | Tenzel RR, Buffam FV, Miller GR. The use of the "lateral canthal sling" in ectropion repair. Can J Ophthalmol. 1977;12:199-202. [PubMed] |
| 10. | Anderson RL, Gordy DD. The tarsal strip procedure. Arch Ophthalmol. 1979;97:2192-2196. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 370] [Cited by in RCA: 308] [Article Influence: 6.7] [Reference Citation Analysis (0)] |
| 11. | Han J, Lee SH, Shin HJ. Mini-incisional entropion repair for correcting involutional entropion: Full description and surgical outcome. Medicine (Baltimore). 2019;98:e16731. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 9] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 12. | Qurban Q, Kamil Z. Treatment Of Senile Entropion: A Comparison Of Standard And Modified Surgical Technique. J Ayub Med Coll Abbottabad. 2022;34 Suppl 1:S678-S681. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 13. | Shahid E, Fasih U, Shaikh A. Wies procedure for correcting involutional entropion of the lower lid in geriatrics. Malaysia J Ophthalmol. 2021;3:21-29. [DOI] [Full Text] |
| 14. | Cheung JJC, Wong CKH, Cheung LTY. Combined pentagonal resection and inferior retractor plication in involutional entropion. BMC Ophthalmol. 2018;18:329. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 6] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 15. | Kersten RC, Kleiner FP, Kulwin DR. Tarsotomy for the treatment of cicatricial entropion with trichiasis. Arch Ophthalmol. 1992;110:714-717. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 41] [Cited by in RCA: 31] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 16. | McCord CD Jr, Chen WP. Tarsal polishing and mucous membrane grafting for cicatricial entropion, trichiasis and epidermalization. Ophthalmic Surg. 1983;14:1021-1025. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.0] [Reference Citation Analysis (0)] |
| 17. | Koreen IV, Taich A, Elner VM. Anterior lamellar recession with buccal mucous membrane grafting for cicatricial entropion. Ophthalmic Plast Reconstr Surg. 2009;25:180-184. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 25] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 18. | Malhotra R, Yau C, Norris JH. Outcomes of lower eyelid cicatricial entropion with grey-line split, retractor recession, lateral-horn lysis, and anterior lamella repositioning. Ophthalmic Plast Reconstr Surg. 2012;28:134-139. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 10] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 19. | Kadyan A, Barry R, Murray A. Anterior lamellar excision and laissez-faire healing for aberrant lashes in ocular cicatricial pemphigoid. Eye (Lond). 2010;24:990-993. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 7] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 20. | Wu AY, Thakker MM, Wladis EJ, Weinberg DA. Eyelash resection procedure for severe, recurrent, or segmental cicatricial entropion. Ophthalmic Plast Reconstr Surg. 2010;26:112-116. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 15] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 21. | Baylis HI, Silkiss RZ. A structurally oriented approach to the repair of cicatricial entropion. Ophthalmic Plast Reconstr Surg. 1987;3:17-20. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 15] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 22. | Chi M, Kim HJ, Vagefi R, Kersten RC. Modified tarsotomy for the treatment of severe cicatricial entropion. Eye (Lond). 2016;30:992-997. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 6] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 23. | Goldberg RA, Joshi AR, McCann JD, Shorr N. Management of severe cicatricial entropion using shared mucosal grafts. Arch Ophthalmol. 1999;117:1255-1259. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 43] [Cited by in RCA: 37] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 24. | Seiff SR, Carter SR, Tovilla y Canales JL, Choo PH. Tarsal margin rotation with posterior lamella superadvancement for the management of cicatricial entropion of the upper eyelid. Am J Ophthalmol. 1999;127:67-71. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 28] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 25. | Singh S, Narang P, Mittal V. Labial mucosa grafting for lid margin, anterior lamellar, and posterior lamellar correction in recurrent cicatricial entropion. Orbit. 2021;40:301-305. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 17] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 26. | Takahashi Y, Ikeda H, Ichinose A, Kakizaki H. Congenital entropion: outcome of posterior layer advancement of lower eyelid retractors and histological study of orbicularis oculi muscle hypertrophy. Orbit. 2014;33:444-448. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 5] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 27. | Huang Q, Fang Y, Wang Y, Liao H. Comparison of the cutaneous orbicularis oculi excision treatment with the inferior eyelid margin fixation treatment for congenital lower eyelid entropion. Int Ophthalmol. 2023;43:2153-2159. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 28. | Khuu TH, Czyz CN, Michels KS. Subciliary Rotating Sutures Combined With Modified Hotz Procedure for Correction of Congenital Lower Eyelid Entropion. Ann Plast Surg. 2023;90:415-418. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 29. | Burton M, Habtamu E, Ho D, Gower EW. Interventions for trachoma trichiasis. Cochrane Database Syst Rev. 2015;2015:CD004008. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 30] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 30. | Singh S. Distichiasis: An update on etiology, treatment and outcomes. Indian J Ophthalmol. 2022;70:1100-1106. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 9] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 31. | Woo KI, Kim YD. Management of epiblepharon: state of the art. Curr Opin Ophthalmol. 2016;27:433-438. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 21] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 32. | Zhuo D, Chen S, Ren X, Wang B, Liu L, Xiao L. The prevalence of lower eyelid epiblepharon and its association with refractive errors in Chinese preschool children: a cross-sectional study. BMC Ophthalmol. 2021;21:3. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 7] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 33. | Ma ST, Liu YL, Hsieh CJ, Chen YS, Tsai TH. Surgical Treatment of Epiblepharon Effectively Alleviates Keratopathy but Not Astigmatism: A Case-Control Study Utilizing Vector Analysis in East Asian Children. J Ophthalmol. 2020;2020:5073895. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 34. | Sung Y, Lew H. Epiblepharon correction in Korean children based on the epicanthal pathology. Graefes Arch Clin Exp Ophthalmol. 2019;257:821-826. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 7] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 35. | Yan Y, Chen T, Wei W, Li D. Epiblepharon in Chinese children: relationships with body mass index and surgical treatment. J AAPOS. 2016;20:148-152. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 17] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 36. | George E, Richie MB, Glastonbury CM. Facial Nerve Palsy: Clinical Practice and Cognitive Errors. Am J Med. 2020;133:1039-1044. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 17] [Cited by in RCA: 27] [Article Influence: 5.4] [Reference Citation Analysis (0)] |
| 37. | Hodgson NM, Rajaii F. Current Understanding of the Progression and Management of Thyroid Associated Orbitopathy: A Systematic Review. Ophthalmol Ther. 2020;9:21-33. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 21] [Cited by in RCA: 48] [Article Influence: 8.0] [Reference Citation Analysis (0)] |
| 38. | Lailaksiri N, Wanichsetakul P, Saonanon P. Implantation of a Newly Designed Supratarsal Gold Weight versus the Traditional Pretarsal Model for the Correction of Long-standing Paralytic Lagophthalmos: A Retrospective Cohort Study. Arch Plast Surg. 2024;51:163-168. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 39. | Chung CM, Tak SW, Lim H, Cho SH, Lee JW. Early cicatricial lagophthalmos release with pentagonal wedge resection of the scar, fat redistribution, and full-thickness skin grafting. Arch Craniofac Surg. 2020;21:49-52. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1] [Cited by in RCA: 4] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 40. | Medina A. Management of Severe Multifactorial Eyelid Ectropion With Lateral Tarsal Strip Procedure and Full-Thickness Skin Graft. Cureus. 2022;14:e23462. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 41. | Heckmann JG, Urban PP, Pitz S, Guntinas-Lichius O, Gágyor I. The Diagnosis and Treatment of Idiopathic Facial Paresis (Bell's Palsy). Dtsch Arztebl Int. 2019;116:692-702. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 60] [Article Influence: 10.0] [Reference Citation Analysis (0)] |
| 42. | AlHarthi AS. Involutional ectropion: etiological factors and therapeutic management. Int Ophthalmol. 2023;43:1013-1026. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 5] [Reference Citation Analysis (0)] |
| 43. | Ghafouri RH, Allard FD, Migliori ME, Freitag SK. Lower eyelid involutional ectropion repair with lateral tarsal strip and internal retractor reattachment with full-thickness eyelid sutures. Ophthalmic Plast Reconstr Surg. 2014;30:424-426. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 19] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 44. | Vahdani K, Thaller VT. Anterior lamellar deficit ectropion management. Eye (Lond). 2021;35:929-935. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 45. | Korteweg SF, Stenekes MW, van Zyl FE, Werker PM. Paralytic ectropion treatment with lateral periosteal flap canthoplasty and introduction of the ectropion severity score. Plast Reconstr Surg Glob Open. 2014;2:e151. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 9] [Article Influence: 0.8] [Reference Citation Analysis (0)] |