Published online Jun 26, 2025. doi: 10.12998/wjcc.v13.i18.103777
Revised: December 29, 2024
Accepted: February 6, 2025
Published online: June 26, 2025
Processing time: 89 Days and 1.3 Hours
Clavicle fractures are a common type of fracture that often occurs after high-energy trauma. The treatment methods for clavicle fractures remain controversial. Both locking compression and hook plates are recommended.
A 44-year-old male suffered an injury during skiing. Radiography revealed a right-sided distal clavicular fracture. The fracture was treated using a hook plate due to its small size. During the surgical procedure, Kirschner wires were used to drill holes in the acromion. The end of the hook plate was inserted into the hole rather than below the edge of the acromion.
One year later, imaging revealed complete healing of the fracture, and the hook plate was removed. The patient was satisfied with the course and treatment results. Additionally, a new classification system was proposed based on the degree of injury to the distal clavicle joint surface. The incidence of postoperative complications associated with the use of hook plates for clavicular fracture treatment is relatively high. Complications can be reduced by changing the hook plate placement.
Core Tip: Based on the original Operation Method, the new operation method drilled the acromion to reduce the complications of hook plate. We present a classification of distal clavicular fractures based on the distal clavicular articular surface.
- Citation: Hu WT, Zhang ZY, Qu J, Piao CD. New surgical approach for distal clavicle fractures: A case report. World J Clin Cases 2025; 13(18): 103777
- URL: https://www.wjgnet.com/2307-8960/full/v13/i18/103777.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v13.i18.103777
Clavicle fracture is a common type of fracture, accounting for 2.6%–4% of fractures in adults[1]. Robert William Smith studied this injury as early as 1847; however, it was considered trivial at that time[2]. It was not until the 1960s that they gradually gained attention. In 1963, Neer proposed the Neer classification of clavicle fractures, further systematizing their treatment. This classification has been used since then[3]. Neer type I and III fractures are more stable, and nonsurgical treatment can produce ideal results. Neer type II distal clavicle fractures occur when the distal fracture fragment moves downwards under muscle traction due to injury of the conoid ligament with a large distance between the fracture ends. The rate of delayed healing after conservative treatment can reach up to 45%, and the incidence of non-union can reach 20%–30%[4]. Therefore, surgical treatment is usually required for Neer type II distal clavicular fractures. Common fixation methods include clavicular hook plates, distal locking plates, Kirschner wires, suture anchors, and band plates. To date, there is no consensus on the best treatment method for distal clavicle fractures, and their treatment remains challenging[5]. Herein, we report the case of a patient with Neer type II clavicle fracture who underwent surgical treatment. The patient achieved a good prognosis by changing the placement of the hook plate.
A 44-year-old man presented with right-sided shoulder pain and a deformity secondary to skiing.
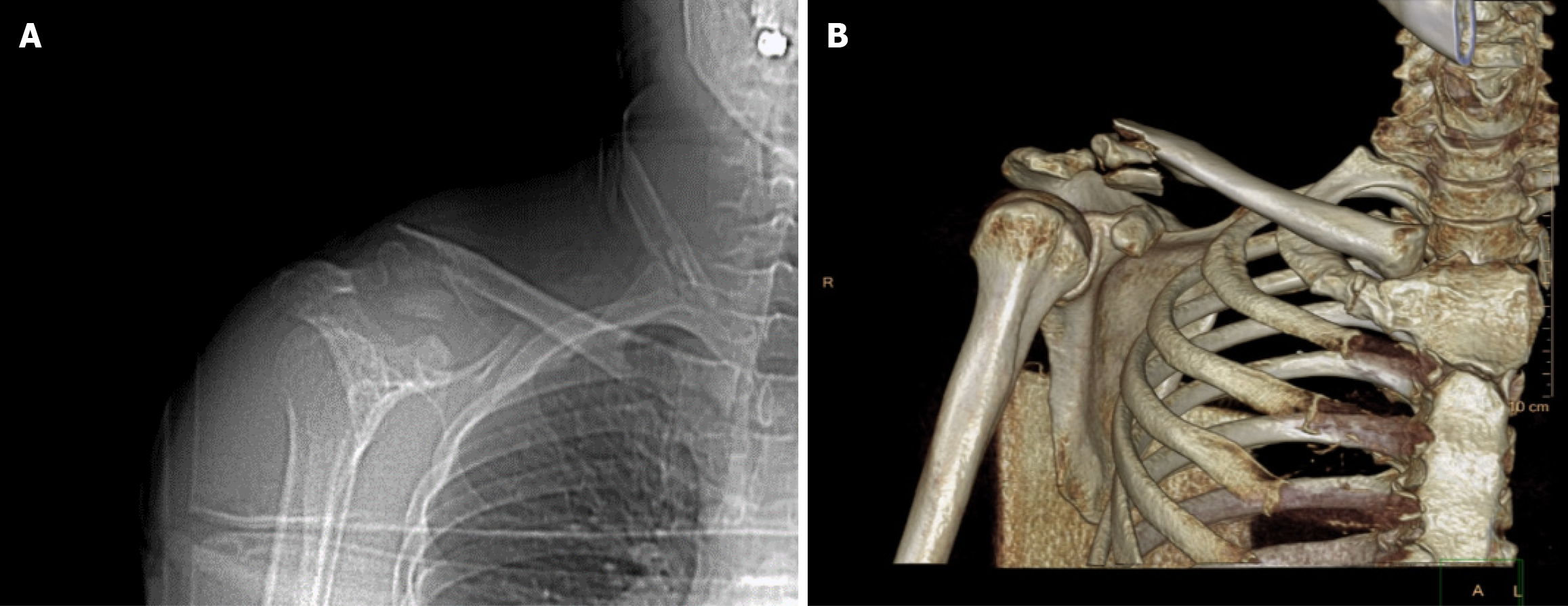
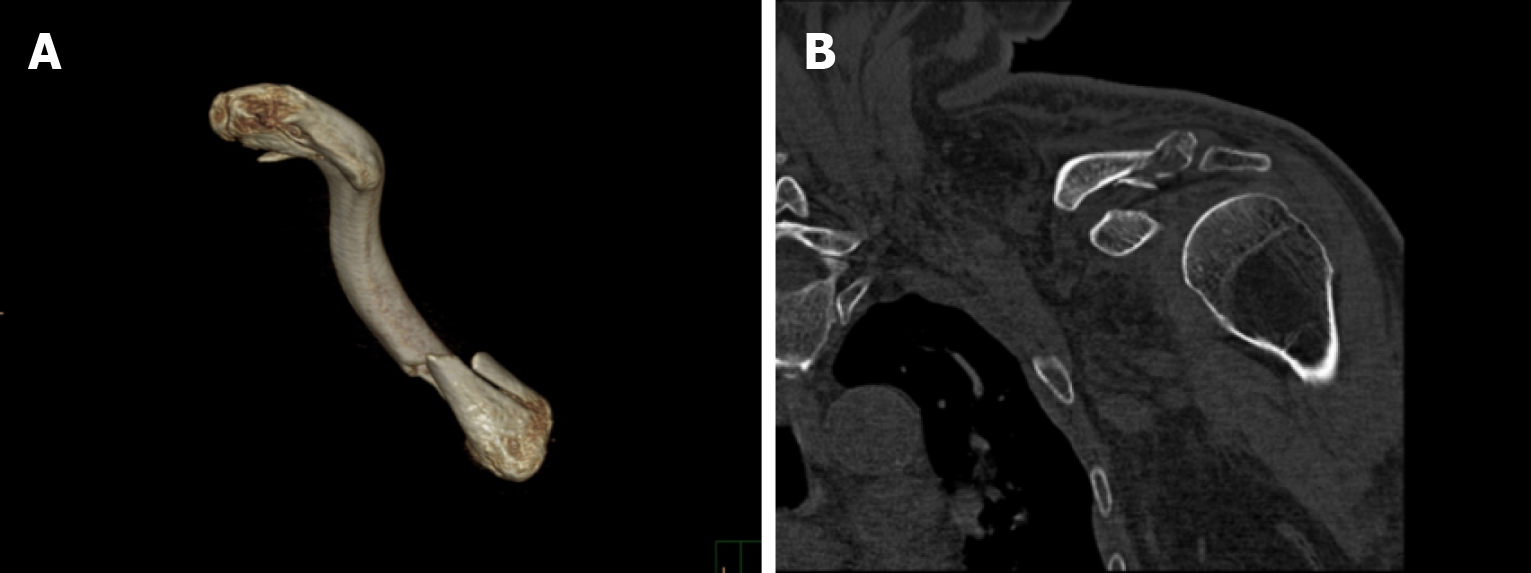
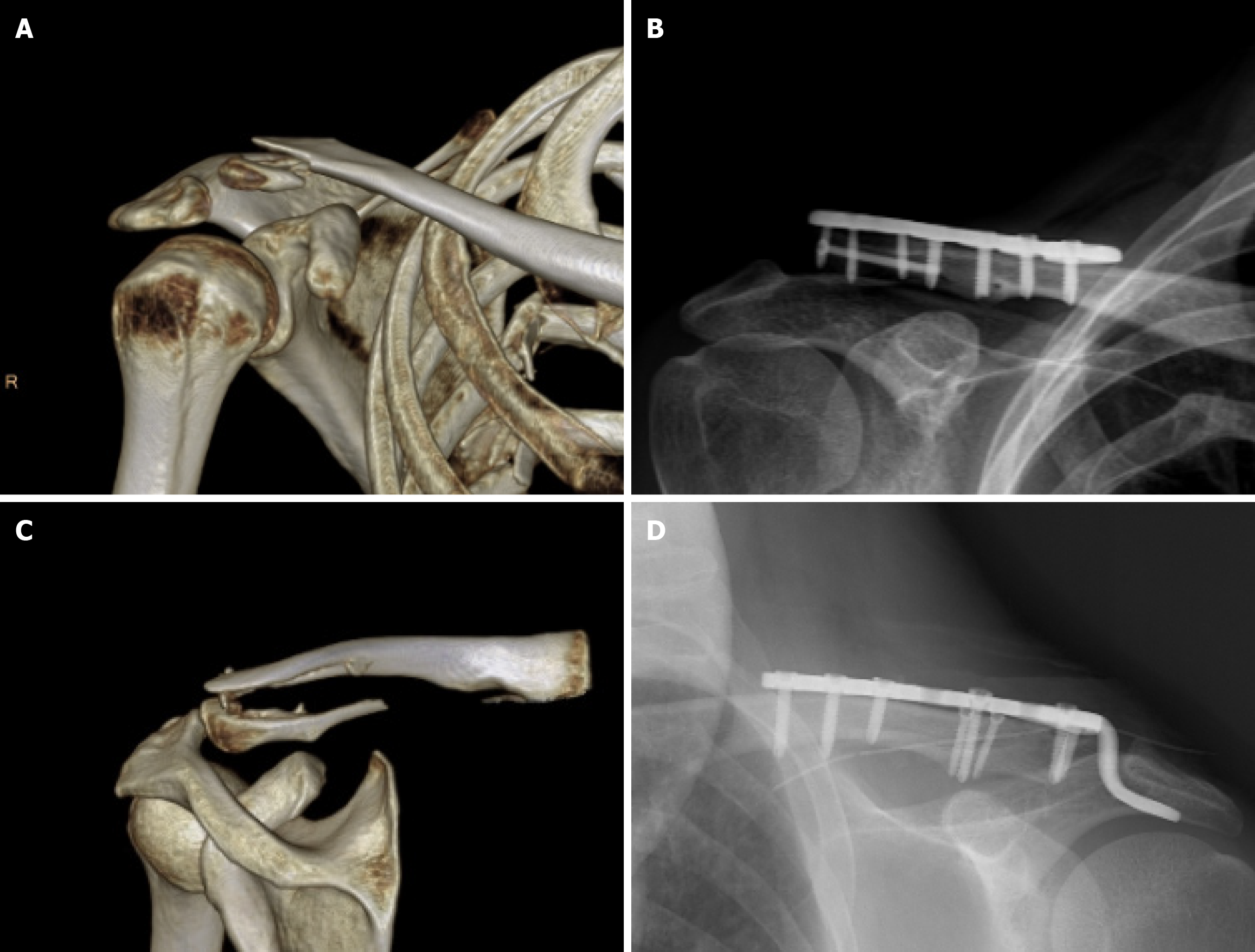
Case report and new operation: Shoulder joint movement was difficult, and no signs of vascular or nerve injury were observed. Plain radiographs and computed tomography (CT) scans revealed a distal clavicle fracture on the right side (Figure 1). The clavicle was split into three fragments, and the fracture was classified as Neer Type II.
No past medical history.
Smoking history; no family history.
Shoulder joint movement was difficult, and no signs of vascular or nerve injury were observed.
There was no obvious abnormality in laboratory examination.
Plain radiographs and CT scans revealed a distal clavicle fracture on the right side (Figure 1). The clavicle was split into three fragments, and the fracture was classified as Neer Type II.
Distal clavicle fracture.
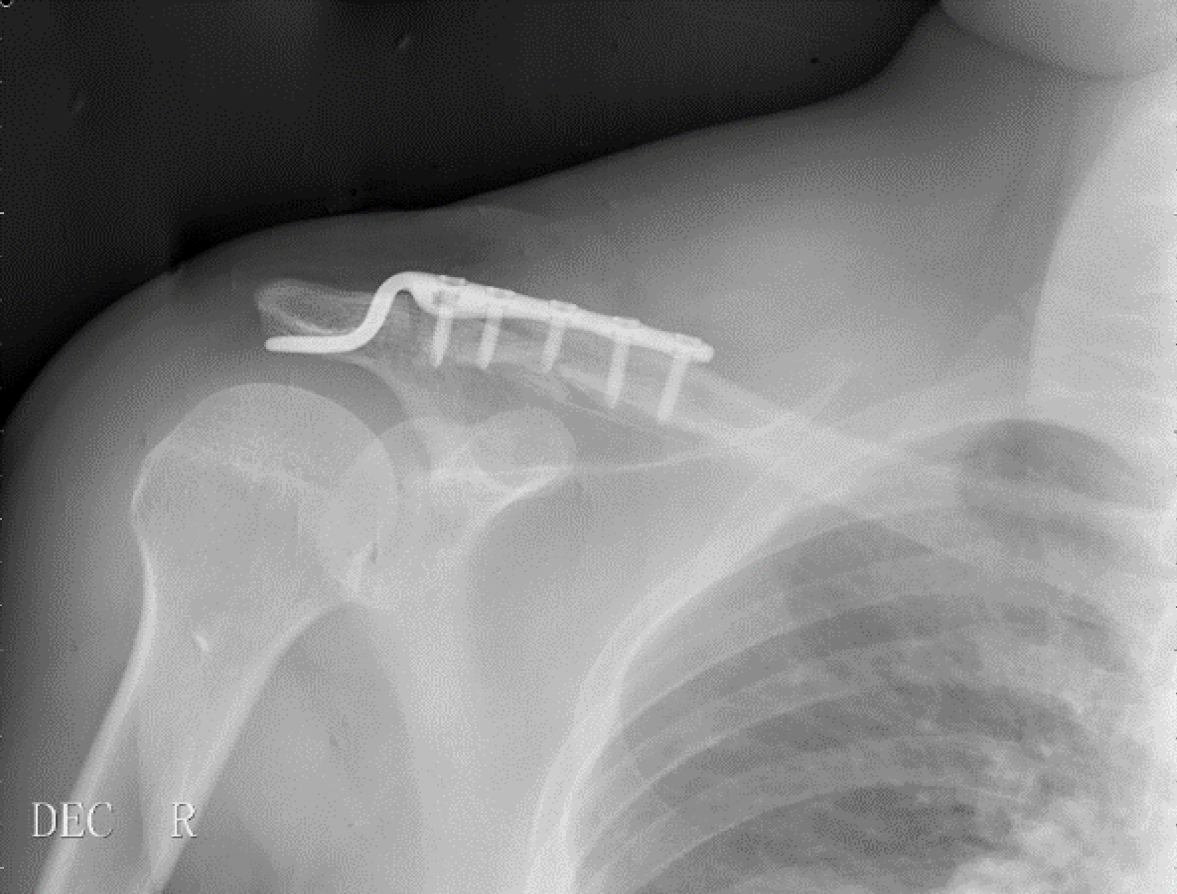
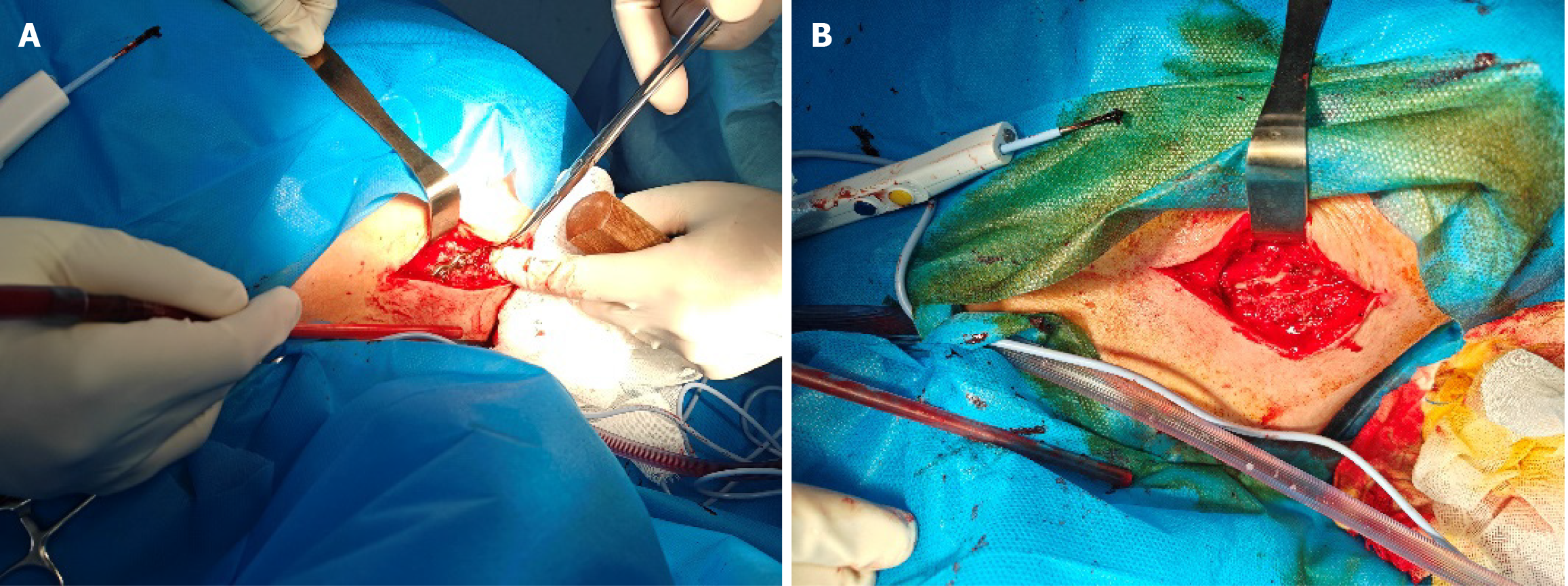
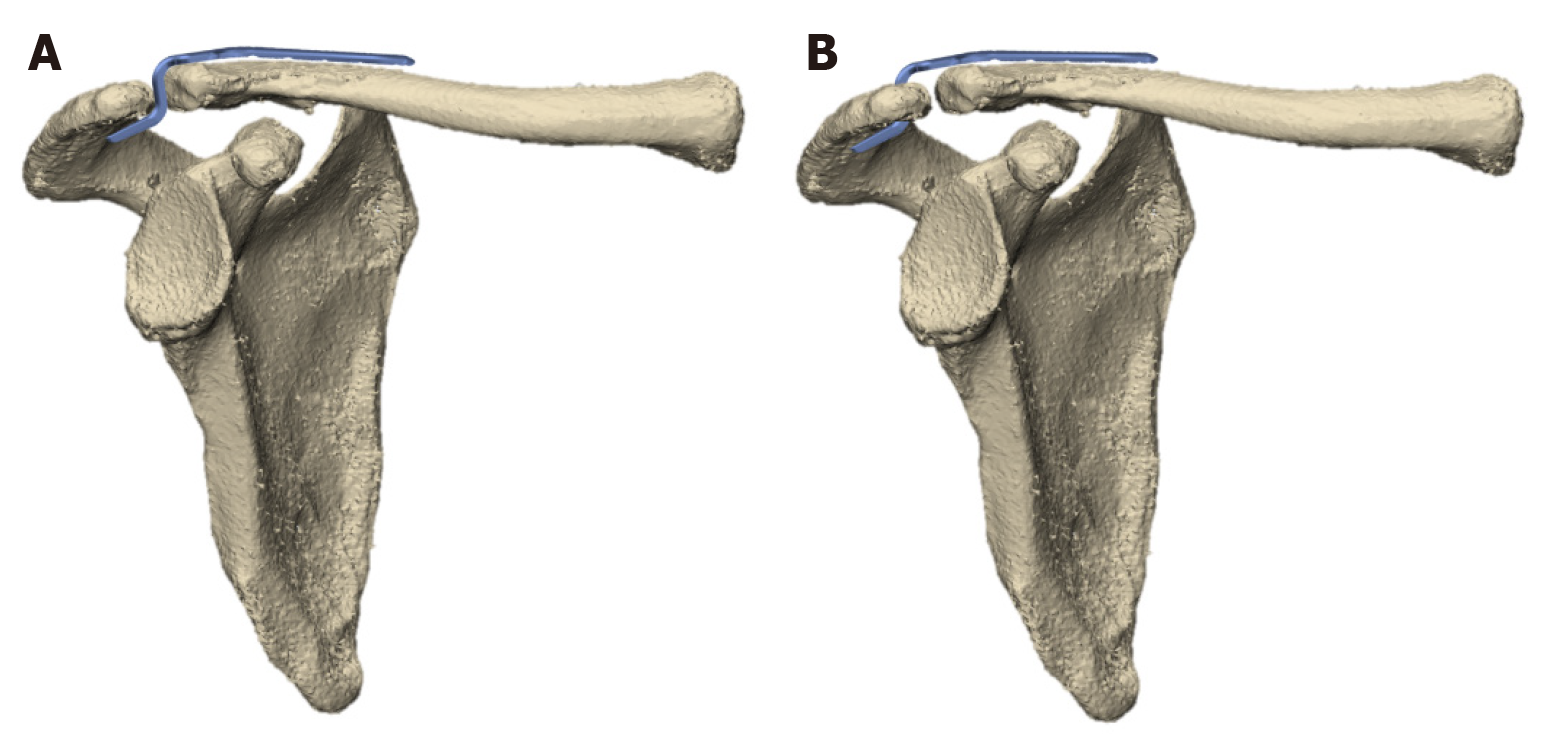
After a detailed explanation of the surgical plan, the patient agreed to undergo surgery and actively cooperated. Surgery was performed under general anesthesia, with the patient in the supine position. The right shoulder was elevated, and an anterolateral clavicular approach was used to make an incision from the clavicle to the acromion, stripping the periosteum to expose the lateral aspect of the clavicle and acromion. The acromioclavicular ligament was intact, and the subacromial soft tissue was gently stripped. A 2.5 mm Kirschner wire was predrilled vertically into the acromion. After reducing the fracture, the surgeon attempted to insert a hook plate suitable for the three fragments into the acromion. Distal pull and proximal compression of the hook plates were tested, and the most suitable plate was selected. The hook end of the plate was inserted through the hole into the acromial bone rather than below the acromion, and the proximal end was attached to the upper clavicle (Figure 2). The incision was sutured after fixation. The patient awoke without discomfort except for pain.
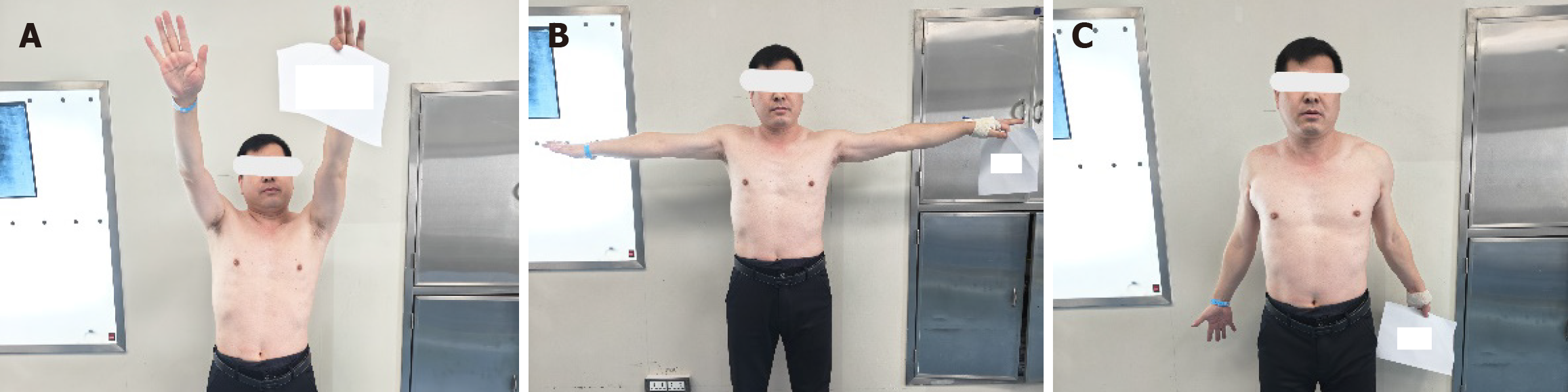
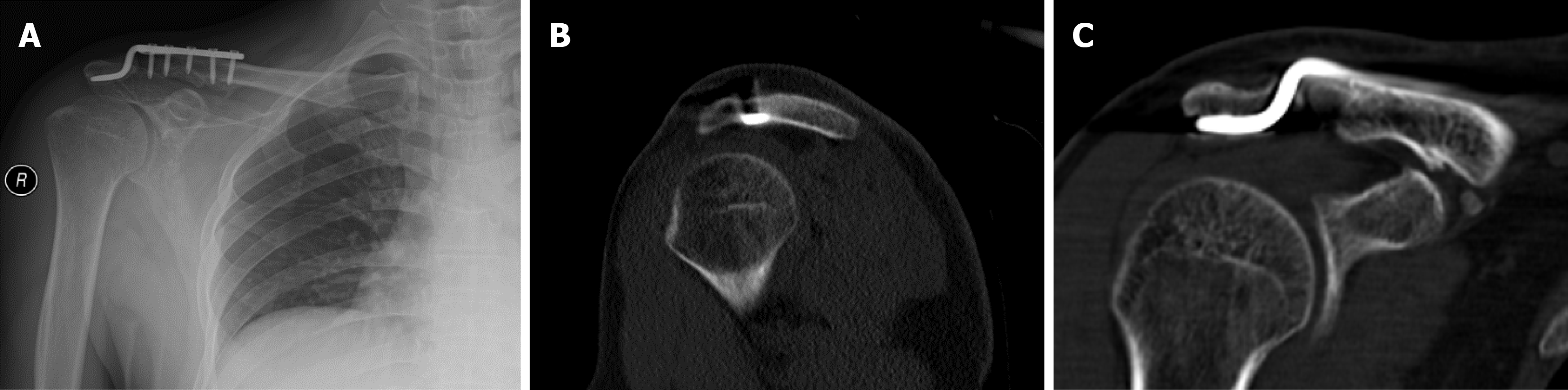
The patient began active and passive range-of-motion training on the third postoperative day. The patient returned to the hospital after 14 months. The patient received no treatment at any other hospital during this period, and the only discomfort experienced was limited movement of the shoulder joint. At this time, the range of motion of the shoulder joint was as follows: Elevation 120° forward (Figure 3A), horizontal abduction 90° (Figure 3B), and elevation 30° posteriorly (Figure 3C). The patient was not a manual laborer or athlete, and the DASH score was approximately 8.4. Plain radiographs and CT scans revealed complete healing of the fracture, without any hyperdense shadows and the plate hook ends having not penetrated the acromion, as well as no osteolysis (Figure 4). The plate was then removed (Figure 5), thereby increasing the range of motion of the shoulder joint.
The injury simultaneously involves the joint surface of the distal clavicle. No studies have investigated the relationship between the degree of injury to the distal clavicle joint surface and the long-term prognosis. Veeger and van der Helm demonstrated that the clavicle bears horizontal forces to support the thorax[6], and Flatow et al[7]. discovered that there is a 5°–8° rotational micromotion between the clavicle and acromion. Consequently, we believe that the patient may experience discomfort due to the irregularity of the distal clavicular joint surface and the long-term effects of these forces. The stability and flatness of fractures involving the clavicular joint surface must be restored.
Currently, Neer, Rockwood, and Robinson classifications are widely used and include inclusive classifications. However, there are few detailed descriptions of joint surface injuries, and treatment approaches vary among physicians, each with its own rationale.
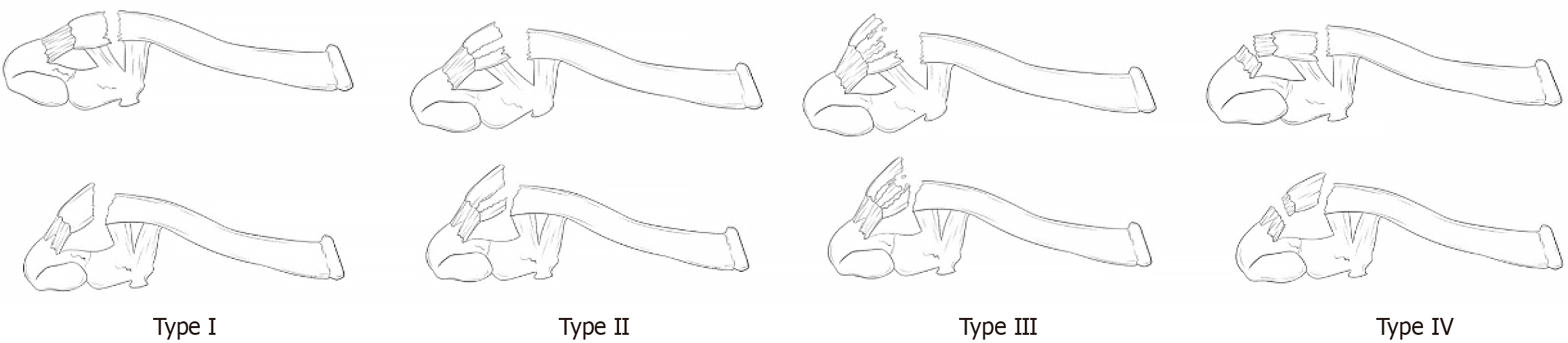
Therefore, we searched for patients with clavicular fractures who were treated surgically at our hospital between July 2022 and July 2024. Based on the inclusion criteria, 29 patients were included in this study. Demographic data of the included patients are listed in Table 1. A new classification was proposed based on the statistical analysis of the fracture morphology of these patients (Figure 6).
| Characteristics | Patient (n = 29) |
| Sex ratio (Male/Female) | 15/14 |
| (1: 0.93) | |
| Age (year) | 46.6 ± 13.3 |
| Age (male/female) | 44.0 ± 13.6/49.3 ± 12.9 |
| Shoulder | 15 (51.7) |
| Left | 15 (51.7) |
| Right | 14 (48.3) |
Due to the small sample size, this article only tentatively presents this classification and provides data for scholars who intend to continue in-depth studies. More importantly, the purpose of this classification is to communicate that it should be refined rather than generalized. Besides, the operator's dependence on surgical experience should be reduced.
The inclusion criteria were as follows: (1) Surgery was performed during hospitalization; (2) Age > 18 years; (3) At least one end of the fracture line was located at or beyond the middle third of the clavicle; and (4) Postoperative imaging revealed a good reduction, flat joint surfaces, and no significant displacement.
Four observers, two experts, and two attending physicians were included in this study. The two experts had an average experience of 20 (± 3) years, and the two attending physicians had an average experience of 11 (± 1) years.
We identified 168 patients with clavicular fractures at our institution between July 2022 and July 2024. A total of 29 patients met the inclusion criteria, of which 15 (51.7%) were male and 14 (48.3%) were female. Left-sided fractures were present in 15 patients (51.7%), while right-sided fractures were present in 14 patients (48.3%). The imaging data, age, and gender of each participant were recorded. The physicians were asked to classify the fractures according to the new classification system and propose the best surgical approach. Four weeks later, four observers were invited to reevaluate the patients.
According to the proposed new classification scheme, Type I fractures are pure distal clavicle fractures that do not involve the joint surface, regardless of the number of fracture lines. Type II fractures have only one fracture line involving the joint surface. Type III fractures have at least two fracture lines involving the joint surface. Type IV fractures with at least one fracture line involving the joint surface and an acromioclavicular joint separation (Figure 6).
Evaluation of the reliability of the new classification and treatment plan: Consistency among evaluators was assessed using Fleiss’ kappa. The reliability of the evaluators was assessed by comparing the results of the two evaluations.
Statistical analysis was performed using Statistical Package for the Social Sciences software (version 27.0; IBM, Armonk). Both classifications by observers with different years of experience resulted in perfect agreement (κ = 0.912, κ = 1.000). Treatment plans demonstrated significant agreement (κ = 0.701) and perfect agreement (κ = 0.826) (Table 2)[8].
| Fleiss Kappa | Standard error | Z value | P value | 95%CI | |
| First Round | 0.912 | 0.070 | 13.056 | 0.000 | 0.907-0.917 |
| Second Round | 1.000 | 0.068 | 14.720 | 0.000 | 0.995-1.005 |
| First treat | 0.701 | 0.076 | 9.251 | 0.000 | 0.696-0.706 |
| Second treat | 0.826 | 0.076 | 10.890 | 0.000 | 0.820-0.831 |
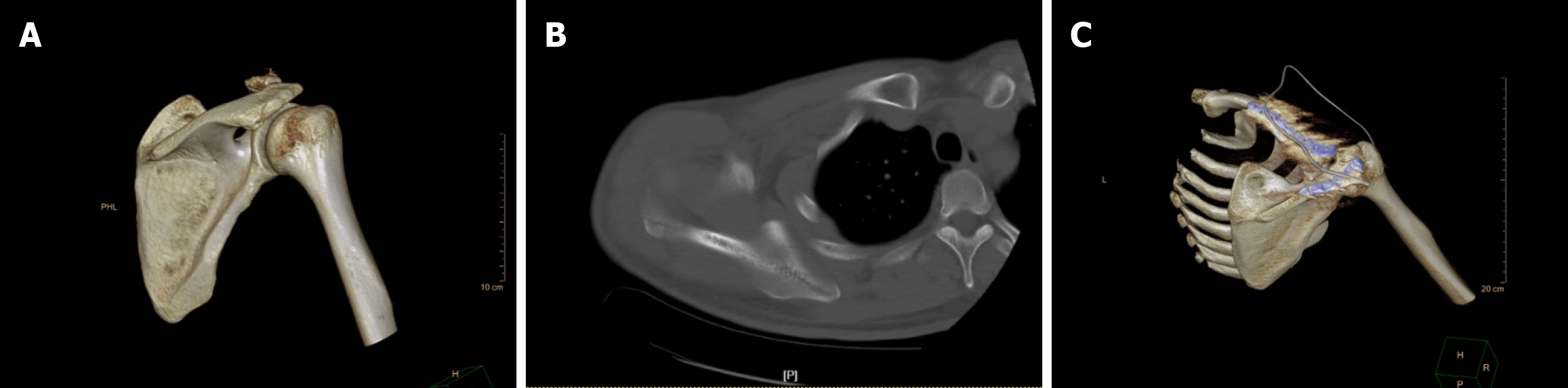
Some controversial cases, such as patients 1 and 2, were also observed. Two attending physicians classified patient 1 as Type II, while two experts classified it as Type I. Compared to the experts, the two attending physicians were more inclined to use 3D CT reconstruction to diagnose the fracture rather than the original images. The 3D CT reconstruction image could blur some details of the fracture, leading to misdiagnosis of the disease. In the second round of testing, the two attending physicians classified patient 1 as Type I after reviewing the original images (Figure 7).
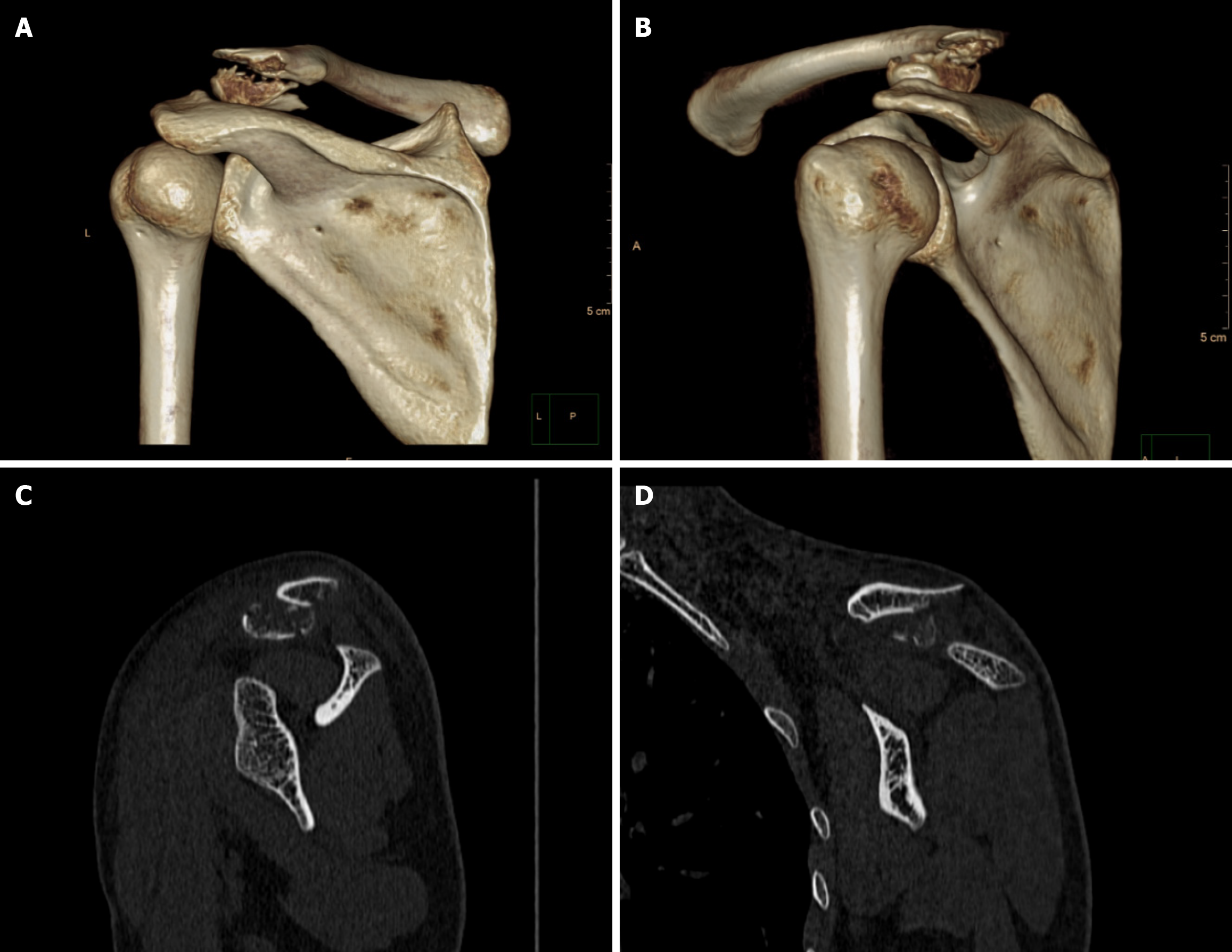
Another controversial case was that of patient 2. In the first round of testing, one expert believed that a locking plate should be used, whereas the other three assessors believed that a hook plate should be used. Ultimately, the patient 2 was treated with a locking plate because of an associated acromial fracture (Figure 8), which precluded the use of a hook plate.
These two cases demonstrate that this classification has some limitations. These include the difficulty in defining the extent of the distal clavicular articular surface and the single factor of extensive focus on it. Besides, although we wanted to reduce the influence of inexperience on fracture treatment by classifying fractures, the classification of fractures depends on experience.
Surgical treatment is often necessary for distal-clavicular fractures. When the distal fragment is too small, the hook plate is considered superior to the locking plate[9]. However, complications associated with the hook plates are difficult to resolve[10,11]. ElMaraghy et al[12] demonstrated through cadaver studies that excessive elevation or rotation of the clavicle could cause micro-motion at the tip of the hook, causing bone erosion or resorption at the point of contact. Li et al[13] developed and used a shoulder height measurement device to control the length of the hook plate hook, thereby reducing complications, including shoulder osteolysis and impingement.
Our approach involved externally rotating the hook plate and inserting the hook tip into the shoulder acromion rather than beneath it (Figure 9). This technique inhibits clavicle rotation and micromotion, thereby reducing friction between the hook tip and acromion, which reduces the occurrence of bone resorption. However, this also temporarily reduced the range of motion of the shoulder joint until the plate was removed. Most scholars believe that the hook plates should be removed. Consequently, we consider the reduction in the shoulder joint range of motion to be temporary and acceptable.
As the hook tip is inserted within the acromion, the length of the hook tip is determined by the thickness of the acromion. If the hook tip is too long, the plate can easily be lifted; if it is too short, the plate cannot adhere to the clavicle. As a consequence, the surgeon can select the optimal hook tip length without requiring any measuring tool, thereby significantly reducing the occurrence of shoulder impingement. However, this implies that the surgical procedure requires a higher level of expertise.
Drilling the acromion can destroy its structure, increasing the risk of acromial fractures. As a result, it is unsuitable for the treatment of patients with osteoporosis.
Herein, we report the case of a patient who underwent this procedure. At the 14-month follow-up, the patient made a satisfactory recovery. Consequently, we believe that surgery is feasible. However, more cases are required to confirm its efficacy.
In this study, the novel classification scheme for distal clavicular fractures achieved significant or perfect agreement with physicians with different years of experience regarding classification and choice of treatment.
Neer classification has been used since the 1960s, but its inclusiveness and practicality are uncontested. The Neer classification systematically categorizes fractures according to their location and the relationship between the ligaments. However, it can only be used for injuries involving the acromioclavicular joint in Neer Type III and does not provide further subclassification. When surgeons develop surgical plans, they provide limited information. In our clinical practice, we discovered that fracture morphology is the most influential factor in the treatment of clavicular fractures. Cases of associated ligament injury are relatively rare. An ideal fracture classification should be comprehensive, simple, and operational while also achieving a high degree of consistency among physicians with different years of experience. However, it was difficult for all three qualities to coexist in the actual classification. Typically, only two of these conditions are satisfied.
The Neer classification is highly inclusive. However, it fails to resolve the controversies surrounding the treatment of distal-clavicular fractures. Therefore, we believe that a classification scheme with a guiding meaning should be developed in a more refined direction, and this classification system has been proposed.
In the new classification system, the use of hook plates for Type I fractures is almost non-controversial. However, Type II fractures are significantly more difficult to treat than Type I fractures, and this classification requires a certain level of surgical experience to begin surgery.
Type II fractures typically require the use of hook plates in combination with additional free-locking screws (Figure 10). These screws have the following functions: 1. The distal fracture fragment was temporarily fixed before the plate was installed to ensure that the joint surface was flat. 2. When the fracture surface was too vertical, screws were applied horizontally to compensate for the functional shortcomings of vertical screws on the plate.
Type III fractures often contain small fragments, for example, patient 3 (Figure 11). Most of these small fragments are unmanageable and must be discarded. However, the absence of small fragments can lead to instability following fracture reduction. As a result, ligation with sutures is recommended before installing the plate in Type III fractures, and free screws and screws on the plate should be used cautiously, as the fragments are small, and too many screws may exacerbate the comminution of the fracture.
Type IV fractures are relatively rare, and no Type IV fractures were found in 29 patients in this study. Consequently, a treatment plan for this type of fracture was not proposed.
This new classification system can serve as a reference for surgeons, facilitating the formulation of surgical plans. However, the treatment plan for fractures is influenced by various factors, and the classification system and treatment plan proposed in this study remain controversial, such as patient 2. Research on classification has verified the reliability of the new system and proven its credibility among different doctors. Due to the limitations of the research conditions, we anticipate enlarging the sample size, particularly by including those with shoulder ligament injuries.
The optimal treatment for distal clavicular fractures remains controversial and challenging. In this study, a patient with a Neer type II clavicle fracture was treated by inserting a hook plate into the acromion, thereby achieving satisfactory prognostic effects. It is possible to move the hook plate outward after drilling holes in the clavicle for insertion into the acromion, thereby reducing complications. Bone resorption and acromion impingement can be reduced by sacrificing mobility in exchange for more stable fixation and shorter hook length. This serves as a reference for treating distal-clavicular fractures. Only one case was included in this study, and the new classification system for distal clavicle fractures requires more samples to determine its reliability. We have listed various situations of distal clavicle fractures and proposed corresponding treatment plans. This study can act as a reference for doctors, especially for those with fewer years of experience.
| 1. | Kihlström C, Möller M, Lönn K, Wolf O. Clavicle fractures: epidemiology, classification and treatment of 2 422 fractures in the Swedish Fracture Register; an observational study. BMC Musculoskelet Disord. 2017;18:82. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 84] [Cited by in RCA: 132] [Article Influence: 16.5] [Reference Citation Analysis (0)] |
| 2. | A Treatise on Fractures in the Vicinity of Joints, and on Certain Forms of Accidental and Congenital Dislocations. Med Chir Rev. 1847;6:137-152. [PubMed] |
| 3. | Neer CS. 5 Fractures of the Distal Third of the Clavicle. Clin Orthop Relat Res. 1968;58:43-50. [RCA] [DOI] [Full Text] [Cited by in Crossref: 209] [Cited by in RCA: 192] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 4. | Choi S, Kim SR, Kang H, Kim D, Park YG. Modified tension band fixation and coracoclavicular stabilisation for unstable distal clavicle fracture. Injury. 2015;46:259-264. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 21] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 5. | Kim DW, Kim DH, Kim BS, Cho CH. Current Concepts for Classification and Treatment of Distal Clavicle Fractures. Clin Orthop Surg. 2020;12:135-144. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 22] [Cited by in RCA: 55] [Article Influence: 11.0] [Reference Citation Analysis (0)] |
| 6. | Veeger HE, van der Helm FC. Shoulder function: the perfect compromise between mobility and stability. J Biomech. 2007;40:2119-2129. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 245] [Cited by in RCA: 242] [Article Influence: 13.4] [Reference Citation Analysis (0)] |
| 7. | Flatow EL. The biomechanics of the acromioclavicular, sternoclavicular, and scapulothoracic joints. Instr Course Lect. 1993;42:237-245. [PubMed] |
| 8. | Landis JR, Koch GG. The Measurement of Observer Agreement for Categorical Data. Biometrics. 1977;33:159-174. [RCA] [DOI] [Full Text] [Cited by in Crossref: 43944] [Cited by in RCA: 41937] [Article Influence: 873.7] [Reference Citation Analysis (0)] |
| 9. | Sim E, Schwarz N, Höcker K, Berzlanovich A. Repair of complete acromioclavicular separations using the acromioclavicular-hook plate. Clin Orthop Relat Res. 1995;134-142. [PubMed] [DOI] [Full Text] |
| 10. | Erdle B, Izadpanah K, Jaeger M, Jensen P, Konstantinidis L, Zwingmann J, Südkamp NP, Maier D. Comparative analysis of locking plate versus hook plate osteosynthesis of Neer type IIB lateral clavicle fractures. Arch Orthop Trauma Surg. 2017;137:651-662. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 47] [Article Influence: 5.9] [Reference Citation Analysis (0)] |
| 11. | Kirsch JM, Blum L, Hake ME. Distal Clavicle Fractures: Open Reduction and Internal Fixation With a Hook Plate. J Orthop Trauma. 2018;32 Suppl 1:S2-S3. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 15] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 12. | ElMaraghy AW, Devereaux MW, Ravichandiran K, Agur AM. Subacromial morphometric assessment of the clavicle hook plate. Injury. 2010;41:613-619. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 63] [Cited by in RCA: 56] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 13. | Li D, Qiao R, Yang N, Zhang K, Zhu Y, Song Z. Clinical analysis of the acromial height-measuring device combined with new-type clavicular hook plate and standard clavicular hook plate in the treatment of Neer type II distal clavicle fractures. J Orthop Surg Res. 2022;17:448. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |