Published online Sep 26, 2023. doi: 10.12998/wjcc.v11.i27.6491
Peer-review started: April 13, 2023
First decision: May 31, 2023
Revised: July 30, 2023
Accepted: August 25, 2023
Article in press: August 25, 2023
Published online: September 26, 2023
Processing time: 159 Days and 18.6 Hours
Blunt abdominal trauma has rarely been reported as a cause of acute appendicitis in the literature. However, the coexistence of the two conditions can cause issues for the patient. We present here a systematic review of cases of traumatic appen
A 12-year-old male was admitted 3 d after abdominal trauma, experiencing peritoneal syndrome. A pelvic formation was discovered during abdominal ultrasound, and surgical exploration revealed a perforated appendix. A literature review was conducted applying the keywords “appendicitis,” “abdominal,” and “trauma” to the PubMed, Embase, and Medline databases. Our initial search included 529 papers published between 1991 and 2022, of which 33 papers were finally included. They revealed 51 reported cases. The trauma mechanisms included road traffic accidents, falls, assaults, ball accidents, a horse kick, and a colonoscopy. Eight patients underwent surgical exploration with no prior radio
Acute traumatic appendicitis represents a diagnostic quandary that can be mis
Core Tip: Appendicitis and abdominal trauma represent the two most common surgical emergencies in both adults and children. However, their coexistence may pose a diagnostic dilemma depending on whether the finding is incidental. Appendicitis should be considered in the differential diagnosis of right lower quadrant pain after abdominal or perineal trauma.
- Citation: Habachi G, Aziza B, Ben-Ammar S, Maherzi O, Houas Y, Kerkeni Y, Sahli S, Jouini R. Acute peritonitis secondary to post-traumatic appendicitis: A case report and literature review. World J Clin Cases 2023; 11(27): 6491-6497
- URL: https://www.wjgnet.com/2307-8960/full/v11/i27/6491.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v11.i27.6491
Appendicitis and abdominal trauma represent the two most common surgical emergencies in both adults and children. However, their coexistence may pose a diagnostic dilemma depending on whether the finding is incidental. Traumatic appendicitis has been a rarely reported but was first recognized in the case of Harry Houdini[1]. In this case, the Hungarian escapologist allowed his student to punch him repeatedly in the right side of his abdomen, and he subsequently died from appendicular peritonitis.
Herein, we reported the case of a 12-year-old male patient who was admitted with acute appendicitis following a blunt abdominal trauma. In addition, we reviewed the literature regarding this uncommon condition.
A 12-year-old male was admitted to the emergency department 3 d after sustaining a fall injury.
The trauma was minor as the patient had fallen from his own height, landing on a concrete floor on his right side and injuring his right hand.
The patient had no surgical history and appeared to be in good health prior to the accident.
The patient had no relevant personal or family history.
Initially, the patient had attended a consult at a local clinic where a physical examination provided normal findings apart from a fifth metacarpal fracture. There were no bruises or tenderness on the abdomen. No further investigation was performed, and the patient was discharged with a plaster cast.
Later that day, he experienced abdominal pain and emesis. By the 3rd day, he developed bilious vomiting and diarrhea prompting his evaluation in the emergency department. Upon examination, his blood pressure, heart rate, and respiratory rate were all normal. His temperature was 37.7 °C. He developed hypogastric tenderness with no rebound or guarding.
Laboratory results revealed an elevated white blood count of 14.5 × 109/L (normal range: 4.5-11.0 × 109/L) and C-reactive protein level of 243 mg/L (normal range: 0.3-1.0 mg/L). Serum electrolytes, lipase, and urinalysis results were all normal.
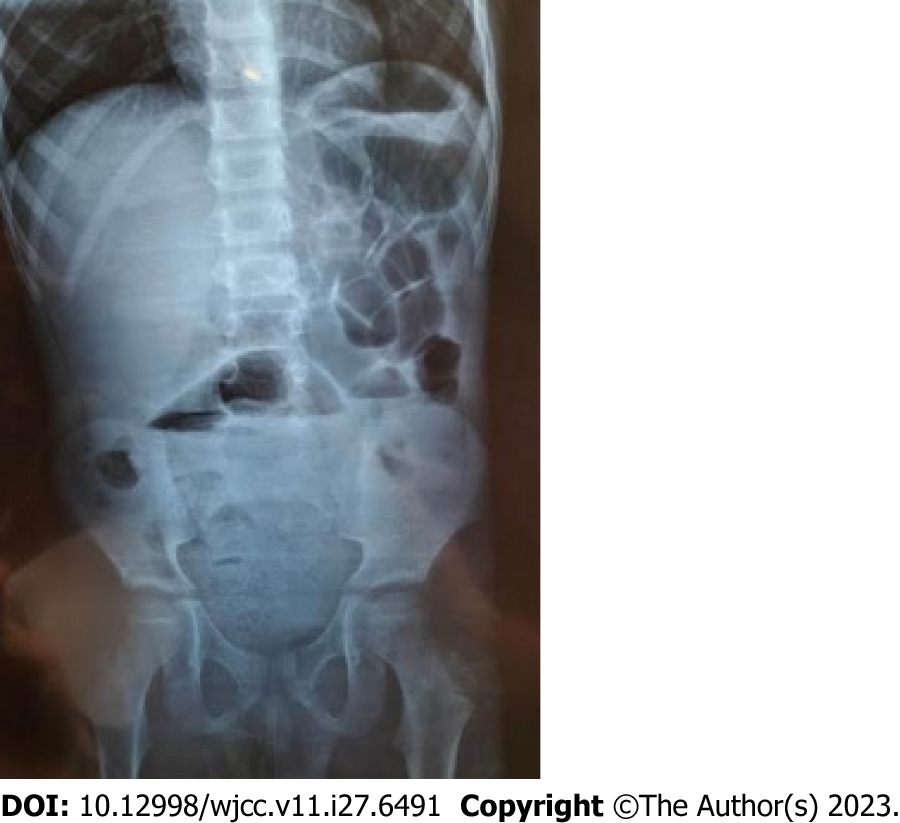
A plain abdominal X-ray revealed multiple gas-fluid levels with no free peritoneal gas (Figure 1). Abdominal ultrasound revealed intestinal dilation as well as a well-limited hypoechoic pelvic formation associated with infiltration of the adjacent intestinal loops.
Acute traumatic appendicitis.
An urgent exploratory laparotomy was performed. Abdominal exploration revealed an intra-abdominal pelvic abscess surrounded by a perforated mesocolic appendix. There were no associated lesions. Appendectomy was performed, and the stump was managed by double ligation.
The postoperative course was uneventful with no postoperative complications. The patient received intravenous triple antibiotic therapy that consisted of cefotaxime, metronidazole, and gentamicin for 10 d. He was then discharged home with no associated treatment. The histopathological examination confirmed the diagnosis of acute appendicitis.
Blunt abdominal trauma is a rare cause of acute appendicitis. However, the direct association is difficult to establish. Ciftci et al[2] discovered a higher incidence of appendicitis after blunt abdominal trauma in pediatric patients. Fowler[3] developed four essential criteria for defining traumatic appendicitis: (1) No history of previous abdominal attacks; (2) Direct abdominal trauma or severe indirect abdominal wall trauma; (3) Symptom onset soon after the trauma; and (4) Progressive symptoms requiring treatment and diagnosis of appendicitis. In this review, all patients met the inclusion criteria, and the diagnosis was confirmed by a histopathological study.
Limited data are available regarding the pathogenesis of traumatic appendicitis. Direct trauma may cause edema and inflammation of the appendicular lymphoid tissue, resulting in obstruction and acute appendicitis. In cases of indirect trauma, an increase in intra-abdominal pressure may cause an increase of intra-cecal pressure resulting in rapid appendiceal distension and appendicitis. Direct trauma of the mesoappendix has also been reported[4]. One patient developed traumatic appendicitis following a perineal trauma[5]. These mechanisms could be isolated or combined, but they are still speculative. Wangensteen et al[6] demonstrated the development of acute appendicitis following direct trauma with no luminal obstruction in a rabbit model. However, this study represents the only experimental theory.
We identified a high incidence of traumatic appendicitis in pediatric patients (52.9%). This can be explained by the smaller abdominal cavity and quality of the muscular anterior abdominal wall in pediatric cases. As a result, clinicians should be suspicious of traumatic appendicitis after blunt abdominal trauma particularly in children. In addition, children are at higher risk of trauma from gaming accidents, such as from balls and bicycles, and animal-related injuries (being kicked by a horse[7]).
Initially, the clinical and radiological signs of traumatic appendicitis may be nonspecific and/or misleading. Routine hematological and biochemical investigations are ineffective as well. Only a strong suspicion of this pathology may lead to a diagnosis. The difficulty of diagnosis may come from the unfamiliarity of traumatic appendicitis and the numerous differential diagnoses of the causes of abdominal pain after an abdominal trauma. However, ultrasound has proven to be beneficial in several cases[4] (Table 1).
| Ref. | Year | Cases, n | Age in yr | Mechanism of injury | Time of presentation | WBC as / | Investigations | Surgery | Findings |
| Hennington et al[13] | 1991 | 2 | 46; 12 | RTA; fall | 48 h; 12 h | 16900; 13000 | CT (free fluid); none | Laparotomy; laparotomy | Isolated; isolated |
| Bangs[14] | 1991 | 1 | 20 | RTA | A few hours | 3250 | CT | Laparotomy | Isolated |
| Musemeche and Baker[15] | 1995 | 1 | 4 | RTA | A few hours | 22900 | CT | Laparotomy | Isolated |
| Stephenson and Shandall[16] | 1995 | 1 | 32 | Seat belt | 120 h | NA | NA | Laparotomy | Wedge fracture of T10 |
| Serour et al[17] | 1996 | 3 | 11; 8; 7 | Assault; fall; assault | 1 h; 3 h; 7 d | 4500; 20100; NA | CT; none; CT | Laparotomy; laparotomy; laparotomy | Isolated; isolated; isolated |
| Ciftci et al[2] | 1996 | 5 | 8; 5; 13; 14; 7 | RTA; fall; ball; RTA; assault | 2 h; 6 h; 12 h; 4 h; 12 h | 9800-18000 | NA; NA; NA; US; US | Laparotomy; laparotomy; laparotomy; laparotomy; laparotomy | Head injury; rib fracture; isolated; head injury; head injury |
| Edwards et al[11] | 1999 | 1 | 41 | RTA | Hours | NA | CT | Laparotomy | Ileocecal lesion and ileocecal resection |
| Osterhoudt[8] | 2000 | 1 | 9 | RTA | Hours | NA | CT (NL) | Laparotomy | Isolated |
| Takagi et al[18] | 2000 | 1 | 45 | Seat belt | 24 h | NA | NA | Laparotomy | Isolated |
| Ramsook[19] | 2001 | 1 | 12 | Assault | 7 h | 15400 | CT | Laparotomy | Isolated |
| Houry et al[20] | 2001 | 1 | 5 | Fall | 1 h | NA | CT | Laparotomy | Isolated |
| Hagger et al[21] | 2002 | 1 | 60 | Fall | 72 h | NA | CT | Laparotomy | Incarcerated direct hernia |
| Ramesh et al[22] | 2002 | 1 | 11 | Bicycle | 48 h | NL | US | Laparotomy | Isolated |
| Karavokyros et al[23] | 2004 | 1 | 21 | Assault | Hours | NA | US | Laparotomy | Isolated |
| Etensel et al[10] | 2005 | 5 | 5; 8; 14; 9; 13 | RTA; RTA; RTA; fall; RTA | 4 h; 1 h; 1 h; 1 h; 15 min | 18700; 19500; 12200; 17700; 19400 | US; US; US; US, CT; CT | Laparotomy; laparotomy; laparotomy; laparotomy; laparotomy | Multiple hepatic lacerations; right diaphragmatic rupture, liver laceration, and retroperitoneal hematoma; retroperitoneal hematoma; isolated; left diaphragmatic rupture, splenic laceration, and left ureteropelvic junction rupture |
| Volchok and Cohn[24] | 2006 | 1 | 60 | Colonoscopy | 60 h | 13700 | CT | Laparoscopy | Isolated |
| Derr and Goldner[25] | 2009 | 1 | 41 | Fall | 24 h | NA | US, CT | Laparoscopy | Isolated |
| Amir et al[5] | 2009 | 1 | 10 | Fall | 2 h | NL | US, CT | Laparotomy | Isolated |
| Toumi et al[26] | 2010 | 1 | 11 | Assault | 3 d | NA | CT | Laparotomy | Isolated |
| O'Kelly et al[27] | 2012 | 1 | 29 | Ball | 24 h | 17470 | CT | Laparotomy | Isolated |
| Paschos et al[28] | 2012 | 1 | 17 | Bicycle | 12 h | 12700 | US | Laparotomy | Isolated |
| Wani[29] | 2013 | 8 | 9-63 | 3 falls; 4 assaults; 1 bicycle | 24 h-4 d | NA | US, CT | Laparotomy | Isolated |
| Bouassria et al[4] | 2013 | 1 | 24 | Stab | 24 h | 14000 | US (2nd) | Laparotomy | Retroperitoneal hematoma |
| Moslemi et al[30] | 2013 | 1 | 13 | Bicycle | 6 h | 14700 | US, CT | Laparotomy | Rupture of the small bowel mesentery |
| Go et al[31] | 2016 | 1 | 23 | Seat belt | 0.5 | NA | US, CT | Laparotomy | Tearing of the distal ileum mesentery |
| Khilji et al[32] | 2017 | 1 | 43 | RTA | 2 h | 11000 | US, CT | Laparoscopy | Isolated |
| Cobb[33] | 2017 | 1 | 17 | RTA | 24 h | 10800 | CT | Laparoscopy, laparotomy | Isolated |
| Aljaberi et al[34] | 2018 | 1 | 24 | Seat belt | 24 h | NA | CT | Laparotomy | Transection of the omentum |
| Çağlar et al[35] | 2018 | 1 | 12 | Fall | 24 h | 21020 | CT | Laparotomy | Isolated |
| Siddiqui et al[36] | 2018 | 1 | 22 | Fall | 3 h | 7500 | CT | Laparoscopy | Isolated |
| Zvizdic et al[7] | 2019 | 1 | 7 | Horse kick | 10 h | 11500 | US, CT | Laparotomy | Isolated |
| Salinas-Castro et al[37] | 2023 | 1 | 14 | Soccer ball | 6 h | NA | US, CT | Laparoscopy | Isolated |
| Goldman et al[38] | 2022 | 1 | 11 | Assault | 24 h | 22000 | MRI | Laparoscopy | Isolated |
| Our study | 2023 | 1 | 12 | Fall | 3 d | 14500 | US | Laparotomy | Isolated |
In our case, ultrasound did not aid in the diagnosis of appendicitis but did rule out other clinical entities. An X-ray revealed a mechanical obstruction, which led us to perform surgery. Computed tomography scans and magnetic resonance imaging scans are more sensitive for diagnosis. However, a computed tomography scan was normal in 1 patient with traumatic appendicitis[8]. These imaging modalities also may not be accessible in all circumstances.
Contrary to other visceral injuries, traumatic appendicitis may have few early indirect signs of its presence[9], which causes a significant delay in diagnosis and increases the risk of an abscess, peritonitis, and mortality. Moreover, the underdevelopment of the omentum in children may result in the diffusion of the infection. Thus, we emphasize the importance of repeated examinations.
In all cases, surgical treatment is required. Due to the trauma and the risk of associated hemorrhagic lesions that may necessitate additional treatment, laparotomy is commonly performed[10]. Laparoscopy may be indicated in stable cases with a positive preoperative diagnosis. In cases of isolated appendicular lesions, an appendectomy with ligation or plicature of the appendicular stump may be curative, and resection of the injured bowel along with the appendectomy may be performed[11,12].
Traumatic appendicitis is rarely reported due to the difficulty of associating the trauma as a direct cause. The causative relationship is proposed based on the basis of circumstantial evidence. It should, however, be considered in the differential diagnosis of right lower quadrant pain after abdominal or perineal trauma. There are also legal implications of traumatic appendicitis because the trauma can occur from aggression or road traffic accidents.
Provenance and peer review: Unsolicited article; Externally peer reviewed.
Peer-review model: Single blind
Specialty type: Medicine, research and experimental
Country/Territory of origin: Tunisia
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): B, B
Grade C (Good): C
Grade D (Fair): D, D
Grade E (Poor): 0
P-Reviewer: Gu GL, China; Hori T, Japan; Shelat VG, Singapore S-Editor: Li L L-Editor: Filipodia P-Editor: Yuan YY
| 1. | Abdelrahman H, Al-Thani S, Sebastian M, Maull K. Traumatic Appendicitis. Panam J Trauma Crit Care Emerg Surg. 2012;1:48-49. [DOI] [Full Text] |
| 2. | Ciftci AO, Tanyel FC, Büyükpamukçu N, Hiçsönmez A. Appendicitis after blunt abdominal trauma: cause or coincidence? Eur J Pediatr Surg. 1996;6:350-353. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 23] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 3. | Fowler RH. The rare incidence of acute appendicitis resulting from external trauma. Ann Surg. 1938;107:529-539. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 13] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 4. | Bouassria A, Ibn Majdoub K, Yazough I, Ousadden A, Mazaz K, Taleb KA. Traumatic appendicitis: a case report and literature review. World J Emerg Surg. 2013;8:31. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 5] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 5. | Amir A, Amir L, Waisman Y. Acute appendicitis after a blunt perineal trauma: an illustrative case. Pediatr Emerg Care. 2009;25:184-185. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 6] [Article Influence: 0.4] [Reference Citation Analysis (1)] |
| 6. | Wangensteen OH, Buirge RE, Dennis C, Ritchie WP. Studies in the etiology of acute appendicitis: the significance of the structure and function of the vermiform appendix in the genesis of appendicitis a preliminary report. Ann Surg. 1937;106:910-942. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 29] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 7. | Zvizdic Z, Pasic-Sefic I, Vranic S. Acute perforated appendicitis after blunt abdominal trauma: A report from a 7-year-old. Am J Emerg Med. 2020;38:408.e1-408.e2. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 8. | Osterhoudt KC. Hocus-pocus: a case of abdominal pain after blunt abdominal trauma. Pediatr Ann. 2000;29:93-96. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 9. | The Committee on Trauma; the American College of Surgeons. Early Care of Acute Soft Tissue Injuries. Br J Surg. 1955;43:107. [RCA] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 10. | Etensel B, Yazici M, Gürsoy H, Ozkisacik S, Erkus M. The effect of blunt abdominal trauma on appendix vermiformis. Emerg Med J. 2005;22:874-877. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 19] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 11. | Edwards RA, Paul DB, Anderson GL, McCarthy MC. Transection of the appendix: a seat belt injury. Arch Surg. 1999;134:90-91. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 12. | Uludag M, Citgez B, Ozkurt H. Delayed small bowel perforation due to blunt abdominal trauma and periappendicitis in a patient with situs inversus totalis: a report of a case. Acta Chir Belg. 2009;109:234-237. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 5] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 13. | Hennington MH, Tinsley EA Jr, Proctor HJ, Baker CC. Acute appendicitis following blunt abdominal trauma. Incidence or coincidence? Ann Surg. 1991;214:61-63. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 24] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 14. | Bangs RG. Acute appendicitis following blunt abdominal trauma. Ann Surg. 1992;216:100. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 3] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 15. | Musemeche CA, Baker JL. Acute appendicitis: a cause of recurrent abdominal pain in pediatric trauma. Pediatr Emerg Care. 1995;11:30-31. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 5] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 16. | Stephenson BM, Shandall AA. Seat-belt compression appendicitis. Br J Surg. 1995;82:325. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 8] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 17. | Serour F, Efrati Y, Klin B, Shikar S, Weinberg M, Vinograd I. Acute appendicitis following abdominal trauma. Arch Surg. 1996;131:785-786. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 24] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 18. | Takagi Y, Yasuda K, Abe T. Seat belt compression appendicitis. J Clin Gastroenterol. 2000;31:184. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 19. | Ramsook C. Traumatic appendicitis: fact or fiction? Pediatr Emerg Care. 2001;17:264-266. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 17] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 20. | Houry D, Colwell C, Ott C. Abdominal pain in a child after blunt abdominal trauma: an unusual injury. J Emerg Med. 2001;21:239-241. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 6] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 21. | Hagger R, Constantinou J, Shrotria S. Acute appendicitis after a fall from a ladder: a traumatic aetiology? Emerg Med J. 2002;19:366-367. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.1] [Reference Citation Analysis (0)] |
| 22. | Ramesh G, Ho PW, Ng KL, Jegan T. Appendicitis following blunt abdominal trauma. Med J Malaysia. 2002;57:123-124. [PubMed] |
| 23. | Karavokyros I, Pikoulis E, Karamanakos P. A case of blunt abdominal trauma and posttraumatic acute appendicitis. Ulus Travma Acil Cerrahi Derg. 2004;10:60-62. [PubMed] |
| 24. | Volchok J, Cohn M. Rare complications following colonoscopy: case reports of splenic rupture and appendicitis. JSLS. 2006;10:114-116. [PubMed] |
| 25. | Derr C, Goldner DE. Posttraumatic appendicitis: further extending the extended Focused Assessment with Sonography in Trauma examination. Am J Emerg Med. 2009;27:632.e5-632.e7. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 3] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 26. | Toumi Z, Chan A, Hadfield MB, Hulton NR. Systematic review of blunt abdominal trauma as a cause of acute appendicitis. Ann R Coll Surg Engl. 2010;92:477-482. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 30] [Cited by in RCA: 21] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 27. | O'Kelly F, Lim KT, Hayes B, Shields W, Ravi N, Reynolds JV. The Houdini effect--an unusual case of blunt abdominal trauma resulting in perforative appendicitis. Ir Med J. 2012;105:86-87. [PubMed] |
| 28. | Paschos KA, Boulas K, Liapis A, Georgiou E, Vrakas X. Traumatic appendicitis in minor blunt abdominal injury. Emerg Med Australas. 2012;24:343-346. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 6] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 29. | Wani I. Post-traumatic retrocaecal appendicitis. OA Case Reports. 2013;2:31. [DOI] [Full Text] |
| 30. | Moslemi S, Forootan HR, Tahamtan M. Co-incidence of acute appendicitis and appendiceal transection after blunt abdominal trauma: a case report. Iran J Med Sci. 2013;38:343-346. [PubMed] |
| 31. | Go SJ, Sul YH, Ye JB, Kim JS. Appendiceal transection associated with seat belt restraint. Ann Surg Treat Res. 2016;91:93-95. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 32. | Khilji MF, Zia Ullah Q. Seat Belt Compression Appendicitis following Motor Vehicle Collision. Case Rep Emerg Med. 2017;2017:8245046. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Reference Citation Analysis (0)] |
| 33. | Cobb T. Appendicitis following blunt abdominal trauma. Am J Emerg Med. 2017;35:1386.e5-1386.e6. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 34. | AlJaberi LM, Salameh AEK, Almarzooqi RM, Emar MF, Salhab R. Transection of the appendix and omentum following a seat belt injury; case report and literature review. Ann Med Surg (Lond). 2018;34:11-13. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 35. | Çağlar A, Er A, Atacan Ö, Gülcü P, Genç S, Çağlar İ, Çelik T, Apa H. A child with acute appendicitis secondary to blunt abdominal trauma: A case report and review of the literature. Pediatr Emerg Care. 2018;5:140-143. [DOI] [Full Text] |
| 36. | Siddiqui J, Oliphant R, Yeh Z, Suen M. Appendicitis A Traumatic Etiology. Journal of Case Reports. 2018;8:176-178. [DOI] [Full Text] |
| 37. | Salinas-Castro KJ, Mejía-Quiñones V, Zúñiga-Londoño NY. Acute appendicitis after closed abdominal trauma: A case report. Radiol Case Rep. 2023;18:631-634. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 38. | Goldman S, Canastra N, Genisca A. Appendicitis Following Blunt Abdominal Trauma: An Illustrative Case. R I Med J (2013). 2022;105:37-38. [PubMed] |