Published online Jul 16, 2022. doi: 10.12998/wjcc.v10.i20.7054
Peer-review started: December 20, 2021
First decision: January 25, 2022
Revised: February 2, 2022
Accepted: May 22, 2022
Article in press: May 22, 2022
Published online: July 16, 2022
Processing time: 196 Days and 9.2 Hours
Insertion of a catheter into the bladder is a rare complication of peritoneal dialysis (PD), and is mainly related to surgical injury. This paper reports a case of bladder perforation that was caused by percutaneous PD catheterization.
A 64-year-old man underwent percutaneous PD catheterization for end-stage renal disease. On the second day after the operation, urgent urination and gross hematuria occurred. Urinalysis showed the presence of red and white blood cells. Empirical anti-infective treatment was given. On the third day after the operation, urgent urination occurred during PD perfusion. Ultrasound showed that the PD catheter was located in the bladder, and subsequent computed tomography (CT) showed that the PD catheter moved through the anterior wall into the bladder. The PD catheter was withdrawn from the bladder and catheterization was retained. Repeat CT on the fourth day after the operation showed that the PD catheter was removed from the bladder, but there was poor catheter function. The PD catheter was removed and the patient was changed to hemodialysis. CT cystography showed that the bladder healed well and the patient was discharged 14 d after the operation.
Bladder perforation injury should be considered and treated timeously in case of bladder irritation during and after percutaneous PD catheterization. The use of Doppler ultrasound and other related technologies may reduce the incidence of such complications.
Core Tip: For percutaneous peritoneal dialysis catheterization, it is necessary to understand the bladder filling in time during the perioperative period. For patients with intraoperative and postoperative bladder irritation, bladder perforation injury should be considered, which can be treated by indwelling catheterization and cystography to determine the degree of bladder healing.
- Citation: Shi CX, Li ZX, Sun HT, Sun WQ, Ji Y, Jia SJ. Bladder perforation injury after percutaneous peritoneal dialysis catheterization: A case report. World J Clin Cases 2022; 10(20): 7054-7059
- URL: https://www.wjgnet.com/2307-8960/full/v10/i20/7054.htm
- DOI: https://dx.doi.org/10.12998/wjcc.v10.i20.7054
Bladder perforation is commonly seen in trauma or iatrogenic injury[1]. Bladder perforation during peritoneal dialysis (PD) catheterization is a rare complication and mostly occurs during percutaneous catheterization. Here, we describe a patient with bladder perforation due to percutaneous PD catheterization.
A 64-year-old man was hospitalized for end-stage renal disease. He chose PD treatment.
Eighteen months ago, the patient was diagnosed with IgA nephropathy by renal biopsy and was diagnosed as having stage 5 chronic kidney disease 1 wk ago.
The patient had a history of hypertension, hyperuricemia, and gout, a history of sleep apnea syndrome and pharyngopalatoplasty for treatment of sleep apnea syndrome, as well as history of laparoscopic cholecystectomy.
Born in Beijing, the patient has lived here for a long time, has not been to epidemic areas and pastoral areas, and has no bad habits such as smoking and drinking. His parents suffered from hypertension and denied a history of other familial genetic diseases.
The patient’s temperature was 36.2 °C, heart rate 70 bpm, respiratory rate 20 breaths/min, blood pressure 180/90 mmHg, and oxygen saturation in room air 99%. His body height was 167 cm, body weight 91 kg, and body mass index 32.6 kg/m2. Physical examination showed that the breath sound of both lungs was thick, and both lungs had scattered wet rales. He had abdominal swelling and slight bilateral symmetrical finger depression edema of lower limbs, with no tenderness or rebound pain and no percussion pain in the renal area. No other positive signs were found in the physical examination.
Routine blood analysis showed that his hemoglobin was 77 g/L, platelet count 69 × 109/L, serum creatinine 1065 mmol/L, and glomerular filtration rate 4 mL/min. Urinalysis showed urinary occult blood (+) and urine protein (++). The level of B-type natriuretic peptide was 1182.90 pg/mL. Liver function and coagulation tests were normal.
Abdominal computed tomography (CT) showed no clear display of gallbladder, and both kidneys had slight atrophy. Cardiac ultrasound revealed whole heart enlargement.
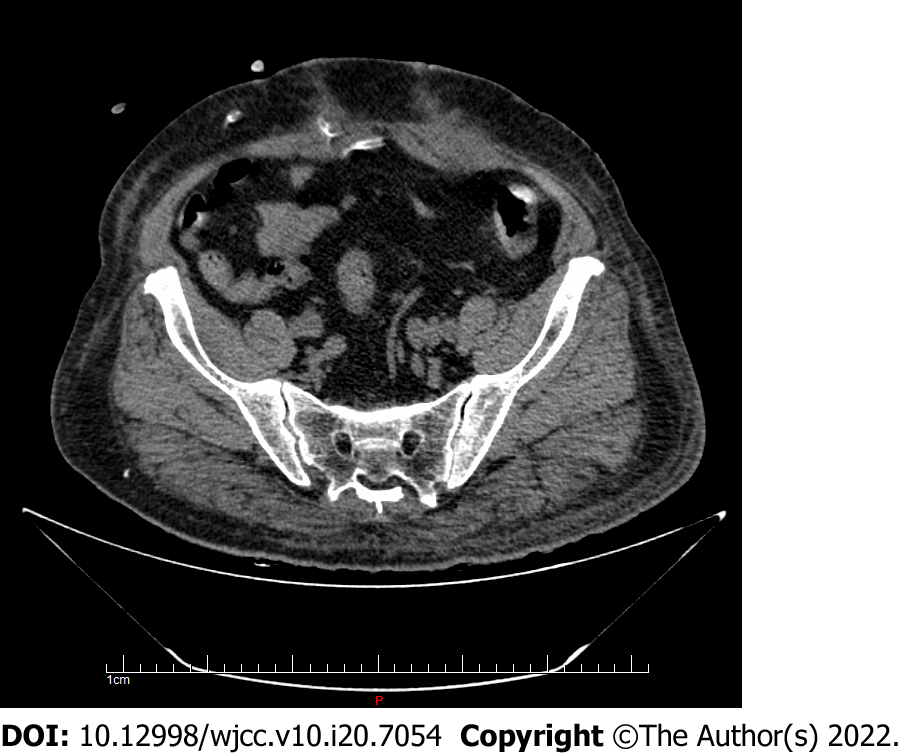
The patient was diagnosed with stage 5 chronic kidney disease and chose PD as long-term renal replacement therapy, and he underwent percutaneous PD catheterization. A Tenckhoff double sleeve straight tube was placed through the subumbilical approach. The patient was instructed to empty the bladder before the operation. PD drainage was unobstructed during the operation, and the flushing tube was unobstructed after operation. On the second day after insertion of the PD catheter, without PD treatment, the patient had urgent urination and macroscopic hematuria. Urinalysis showed the presence of red and white blood cells, with no urine sugar. Considering urinary tract infection, empirical anti-infective treatment was given. On the third day after PD catheter insertion, urgent urination occurred during fluid infusion. Urinalysis, bedside bladder ultrasonography, and total abdominal CT examination were performed immediately. Urinalysis showed the presence of red and white blood cells, and urine sugar (++++). Bedside ultrasound showed that the PD catheter was located in the bladder, and subsequent CT (Figure 1) showed that the catheter moved through the anterior wall into the bladder.
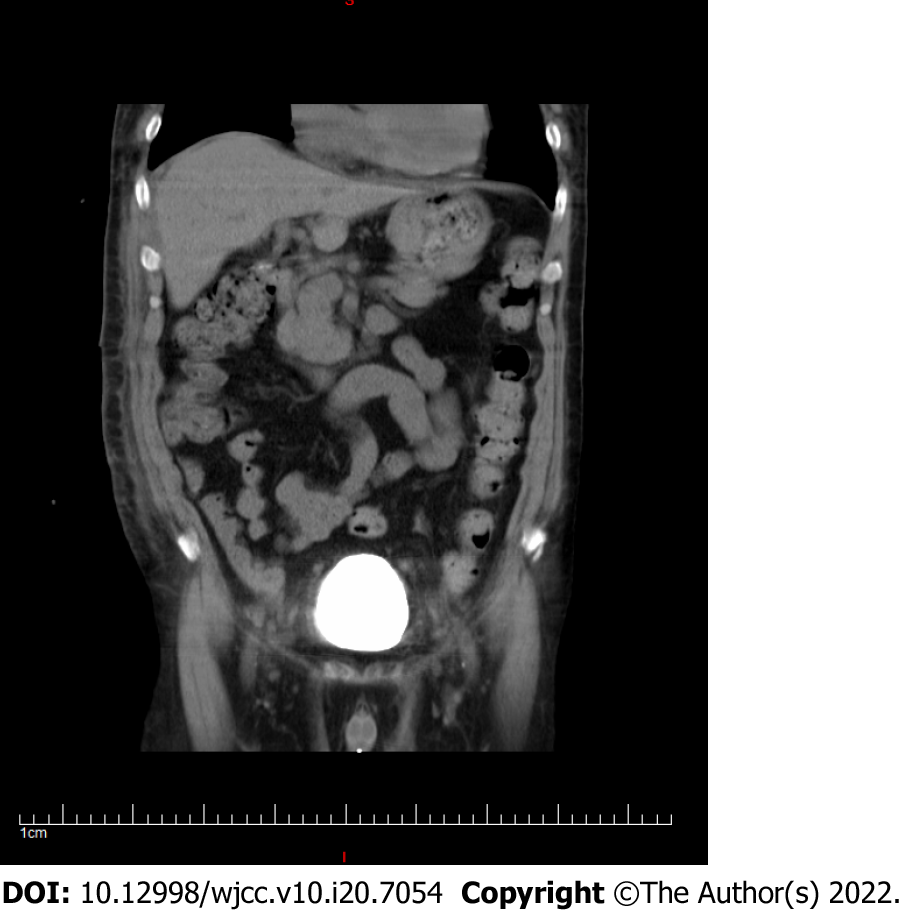
After considering bladder perforation, the catheter was initially inserted and catheterization was continued to repair the bladder. At the same time, the PD catheter was reset under ultrasound guidance. The PD catheter was located in the abdominal cavity by bedside ultrasound after the operation. Re-examination by whole abdominal CT showed that the end of the catheter curled in the rectus abdominis muscle and a small part entered the abdominal cavity (Figure 2). The PD catheter was removed because it showed poor function.
After extubation of the PD catheter, the patient changed to hemodialysis. Repeat bladder CT showed that the bladder healed well (Figure 3). The patient was discharged.
PD as the main treatment for end-stage renal disease is gradually being adopted by more and more patients[2]. By the end of 2018, Mainland China had 86264 registered PD patients[3]. The first step in successful implementation of PD depends on appropriate catheter placement and complete catheter function. PD catheterization methods are generally divided into surgical incision, laparoscopy, and percutaneous puncture[4-6]. At present, the most commonly used method in Mainland China is surgical incision[7]. Percutaneous PD catheterization is a technique that applies Seldinger technology, and uses puncture and guide wire to guide the dialysis tube into the abdominal cavity. PD has several advantages: The operation time is significantly shorter than that of surgery; convenient abdominal dialysis is achieved rapidly after catheterization; the procedure is simple, with no purse suturing; the procedure can be performed under local anesthesia, and results in a small wound; hospital stay is short; and the procedure is low cost[8]. According to the questionnaire survey of the North American Alliance of the International Peritoneal Dialysis Association, 71% of the 42 dialysis centers can carry out laparoscopic catheterization, 62% can use surgical open catheterization, 10% can use trocar blind catheterization, and 29% can use Seldinger method blind catheterization[8]. In recent years, there are more and more reports on percutaneous catheter placement in China.
Catheter-related complications of PD may lead to catheter and technical failure. Mechanical complications associated with PD mainly include pericatheter leakage, infection, visceral injury, and bleeding[9]. Bleeding is one of the most common complications. A case of corpus luteum rupture bleeding caused by open surgery has been reported[10]. Bladder perforation is a rare complication of PD catheterization. The incidence of surgery-related perforation during PD catheter implantation is 0.7%-2.6%[11]. Iatrogenic injuries can occur during laparoscopy, pelvic and endoscopic surgery, and catheter placement. It has been reported that bladder perforation is caused by long-term indwelling of urinary catheters[12]. About 60% of bladder injuries are extraperitoneal, 30% are intraperitoneal, and the remaining 10% are mixed[13].
If the bladder is not fully emptied before PD catheterization, it may be due to neurogenic bladder or chronic bladder outlet obstruction. Our patient had emptied his bladder before PD catheterization, but there was a possibility of refilling the bladder during the procedure due to the patient’s large urine volume. Iatrogenic bladder injury may include postoperative hematuria, urine in the abdominal drainage tube, abdominal distension, intestinal obstruction, or elevated serum creatinine[13]. Bladder perforation caused by PD catheterization first appeared as bladder irritation, which was more obvious when dialysis fluid was injected. Our patient first showed symptoms of urgency and gross hematuria, and urine outflow occurred when PD fluid was injected.
Bladder perforation can be diagnosed by many methods, preferably by CT or X-ray fluoroscopy cystography. The PD fluid is mainly glucose, so urinalysis shows that glucose is strongly positive. Our patient was strongly positive for urinary glucose after administration of PD fluid. Bladder ultrasound and abdominal CT are helpful in the diagnosis of bladder perforation. Cystography shows the contrast of bladder, which has good value for diagnosis and healing of bladder perforation.
For extraperitoneal bladder injury, the initial treatment is usually urethral catheterization[13]. The standard treatment method is indwelling catheterization for 2-3 wk. Intraperitoneal or mixed bladder injury requires early catheterization and then open repair. Although the bladder injury during percutaneous PD catheterization is intraperitoneal, because the catheter material is soft, it can still be treated by indwelling catheterization. After indwelling catheterization, the bladder of our patient healed well. Therefore, whether to carry out emergency open repair will depend on the patient’s clinical condition, postoperative duration, and location of the bladder injury. International guidelines recommend that all patients with bladder injury should undergo cystography before removing the catheter to determine the degree of bladder healing[13-15].
The introduction of Doppler ultrasound in peritoneal dialysis makes the original blind puncture visible, which not only improves the surgical accuracy and catheter survival rate, but also reduces the postoperative complications, without complications such as catheter related bleeding and abdominal organ injury[16]. When we performed the second operation, we could see that ultrasound showed the abdominal wall and interior better.
The emergence of percutaneous catheter placement has made a new breakthrough in peritoneal dialysis catheter placement technology, but there are still a certain proportion of mechanical and infectious complications, especially the risk of blind puncture brought by the puncture technology itself. Here we describe a rare and serious complication of bladder perforation caused by percutaneous catheter placement. Therefore, it is hoped that in the future work, during the operation of percutaneous peritoneal dialysis catheterization, the filling of bladder be evaluated in time, especially for obese patients with more urine volume. It is recommended that preoperative catheterization reduce the complications related to the operation. If such complications occur, the degree of bladder healing can be determined by timely pulling out the catheter, indwelling catheterization, and cystography. Through the use of related technologies such as Doppler ultrasound, we hope to reduce the occurrence of such mechanical complications.
Provenance and peer review: Unsolicited article; Externally peer reviewed.
Peer-review model: Single blind
Specialty type: Urology and nephrology
Country/Territory of origin: China
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): 0
Grade C (Good): C, C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Cabezuelo AS, Spain; Cabezuelo AS, Spain; Stepanova N, Ukraine A-Editor: Wang JL, China S-Editor: Chang KL L-Editor: Wang TQ P-Editor: Chang KL
| 1. | Matlock KA, Tyroch AH, Kronfol ZN, McLean SF, Pirela-Cruz MA. Blunt traumatic bladder rupture: a 10-year perspective. Am Surg. 2013;79:589-593. [RCA] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 43] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 2. | Mehrotra R, Devuyst O, Davies SJ, Johnson DW. The Current State of Peritoneal Dialysis. J Am Soc Nephrol. 2016;27:3238-3252. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 354] [Cited by in RCA: 365] [Article Influence: 40.6] [Reference Citation Analysis (0)] |
| 3. | Ni Zhao-hui, Jin Hai-jiao. The developmental history of peritoneal dialysis in China in the 70 years. Chin J Blood Purif. 18:661-663. [DOI] [Full Text] |
| 4. | Crabtree JH, Chow KM. Peritoneal Dialysis Catheter Insertion. Semin Nephrol. 2017;37:17-29. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 55] [Cited by in RCA: 62] [Article Influence: 8.9] [Reference Citation Analysis (0)] |
| 5. | Carpenter JL, Fallon SC, Swartz SJ, Minifee PK, Cass DL, Nuchtern JG, Pimpalwar AP, Brandt ML. Outcomes after peritoneal dialysis catheter placement. J Pediatr Surg. 2016;51:730-733. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 15] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 6. | Jalandhara N, Balamuthusamy S, Shah B, Souraty P. Percutaneous Peritoneal Dialysis Catheter Placement in Patients with Complex Abdomen. Semin Dial. 2015;28:680-686. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 5] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 7. | China peritoneal dialysis catheterization expert group. China peritoneal dialysis catheterization guidelines. Chin J Nephrol. 2016;32:867-871. [DOI] [Full Text] |
| 8. | Wallace EL, Fissell RB, Golper TA, Blake PG, Lewin AM, Oliver MJ, Quinn RR. Catheter Insertion and Perioperative Practices Within the ISPD North American Research Consortium. Perit Dial Int. 2016;36:382-386. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 22] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 9. | Crabtree JH, Shrestha BM, Chow KM, Figueiredo AE, Povlsen JV, Wilkie M, Abdel-Aal A, Cullis B, Goh BL, Briggs VR, Brown EA, Dor FJMF. Creating and Maintaining Optimal Peritoneal Dialysis Access in the Adult Patient: 2019 Update. Perit Dial Int. 2019;39:414-436. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 254] [Cited by in RCA: 201] [Article Influence: 33.5] [Reference Citation Analysis (0)] |
| 10. | Gan LW, Li QC, Yu ZL, Zhang LL, Liu Q, Li Y, Ou ST. Abdominal hemorrhage after peritoneal dialysis catheter insertion: A rare cause of luteal rupture: A case report. World J Clin Cases. 2021;9:6510-6514. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 1] [Cited by in RCA: 2] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 11. | Abreo K, Sequeira A. Bowel Perforation During Peritoneal Dialysis Catheter Placement. Am J Kidney Dis. 2016;68:312-315. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 13] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 12. | Wu B, Wang J, Chen XJ, Zhou ZC, Zhu MY, Shen YY, Zhong ZX. Bladder perforation caused by long-term catheterization misdiagnosed as digestive tract perforation: A case report. World J Clin Cases. 2020;8:4993-4998. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 6] [Cited by in RCA: 6] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 13. | Sahai A, Ali A, Barratt R, Belal M, Biers S, Hamid R, Harding C, Parkinson R, Reid S, Thiruchelvam N; Section of Female, Neurological, Urodynamic Urology, British Association of Urological Surgeons. British Association of Urological Surgeons (BAUS) consensus document: management of bladder and ureteric injury. BJU Int. 2021;128:539-547. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 14] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 14. | Morey AF, Broghammer JA, Hollowell CMP, McKibben MJ, Souter L. Urotrauma Guideline 2020: AUA Guideline. J Urol. 2021;205:30-35. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 22] [Cited by in RCA: 26] [Article Influence: 6.5] [Reference Citation Analysis (0)] |
| 15. | Kitrey ND, Djakovic N, Hallscheidt P, Kuehhas FE, Lumen N, Serafetinidis E, Sharma DM. EAU Guidelines on Urological Trauma. European Association of Urology. 2020;. |
| 16. | Li Z, Ding H, Liu X, Zhang J. Ultrasound-guided percutaneous peritoneal dialysis catheter insertion using multifunctional bladder paracentesis trocar: A modified percutaneous PD catheter placement technique. Semin Dial. 2020;33:133-139. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 10] [Cited by in RCA: 14] [Article Influence: 2.8] [Reference Citation Analysis (0)] |