Published online Mar 28, 2025. doi: 10.3748/wjg.v31.i12.99846
Revised: February 1, 2025
Accepted: March 3, 2025
Published online: March 28, 2025
Processing time: 237 Days and 2.9 Hours
Most patients who were included in previous studies on achalasia had increased lower esophageal sphincter (LES) pressure. Peroral endoscopic myotomy (POEM) has been confirmed to be effective at relieving the clinical symptoms of achalasia associated with increased LES pressure.
To identify the safety and efficacy of POEM for patients with normal LES integrated relaxation pressure (LES-IRP).
The clinical data of patients who underwent POEM successfully in The First Medical Center of Chinese PLA General Hospital were retrospectively analyzed. A total of 481 patients who underwent preoperative high-resolution manometry (HRM) at our hospital were ultimately included in this research. According to the HRM results, the patients were divided into two groups: 71 patients were included in the normal LES-IRP group (LES-IRP < 15 mmHg) and 410 patients were included in the increased LES-IRP group (LES-IRP ≥ 15 mmHg). Clinical characteristics, procedure-related parameters, adverse events, and outcomes were compared between the two groups to evaluate the safety and efficacy of POEM for patients with normal LES-IRP.
Among the 481 patients included in our study, 209 were males and 272 were females, with a mean age of 44.2 years. All patients underwent POEM without severe adverse events. The median pre-treatment Eckardt scores of the normal LES-IRP and increased LES-IRP groups were 7.0 and 7.0 (P = 0.132), respectively, decreasing to 1.0 and 1.0 post-treatment (P = 0.572). The clinical success rate of the normal LES-IRP group was 87.3% (62/71), and that of the increased LES-IRP group was 91.2% (374/410) (P = 0.298). Reflux symptoms were measured by the GerdQ questionnaire, and the percentages of patients with GerdQ scores ≥ 9 in the normal LES-IRP and increased LES-IRP groups were 8.5% and 10.7%, respectively (P = 0.711). After matching, the rates of clinical success and the rates of GerdQ score ≥ 9 were not significantly different between the two groups.
Our results suggest that POEM is safe and effective for achalasia and patients with normal LES-IRP. In addition, in patients with normal LES-IRP, compared with those with increased LES-IRP, POEM was not associated with a greater incidence of reflux symptoms.
Core Tip: Peroral endoscopic myotomy (POEM) has been confirmed to be effective at relieving the clinical symptoms of achalasia associated with increased lower esophageal sphincter (LES) pressure. However, there are few studies on safety and efficacy of POEM for patients with normal LES integrated relaxation pressure (LES-IRP). Therefore, we conducted a retrospective and found that POEM is safe and effective for achalasia and patients with normal LES-IRP. And POEM was not associated with a greater incidence of reflux symptoms in patients with normal LES-IRP.
- Citation: Li X, Zhang XB, Shao JK, Zhang B, Li LS, Zhu RQ, Zou JL, Wang JF, Zhao X, Wu QZ, Chai NL, Linghu EQ. Peroral endoscopic myotomy for achalasia and patients with normal lower-esophageal-sphincter integrated relaxation pressure: A propensity-score-matched retrospective study. World J Gastroenterol 2025; 31(12): 99846
- URL: https://www.wjgnet.com/1007-9327/full/v31/i12/99846.htm
- DOI: https://dx.doi.org/10.3748/wjg.v31.i12.99846
Achalasia, characterized by esophageal dilation, is a rare disorder of esophageal motility or function[1]. The incidence and prevalence of achalasia are 1 in 100000 persons annually and 10 in 100000 persons annually, respectively[2]. At present, the underlying etiology of achalasia is still unknown, and the proposed causes are neuronal degeneration of the esophageal myenteric plexus, autoimmune diseases, genetic inheritance and viral infection[2-4]. Patients with achalasia often suffer from regurgitation, heartburn, chest pain, dysphagia and eventually progressive weight loss[5].
There are three main methods used to diagnose achalasia: Esophageal manometry, barium esophagram and endo
The treatment options for achalasia include pharmacologic therapy, peroral esophageal myotomy (POEM), endoscopic balloon dilation, endoscopic botulinum toxin injection, temporary esophageal stenting and surgical myotomy[6,7]. Among these options, POEM has become the first-line treatment due to its minimally invasive nature and high success rate[8,9]. Heller myotomy (HM) is effective in the long term and is suitable for patients who are not tolerant of POEM[9,10]. Pharmacological therapy and botulinum toxin injection can serve as short-term or adjunctive treatments[9].
According to the Chicago classification, achalasia can be classified into three subtypes by HRM, and LES-IRP, the key indicator of achalasia, can help determine the extent of relaxation of the esophagogastric junction (EGJ)[11]. However, the findings of HRM do not preclude the diagnosis of achalasia[12]. Besides, some patients presenting with normal LES-IRP and those who have been treated before, also have clinical manifestations and abnormal endoscopic findings. However, studies on the outcomes of POEM in patients with normal LES-IRP are rare. A few of articles have concluded that POEM is effective for patients with normal LES-IRP, while the number of patients included in these studies was low[13,14]. Therefore, a retrospective study was conducted to compare the safety and efficacy of POEM between achalasia and patients with normal LES-IRP.
We reviewed the data of patients who underwent POEM at Department of Gastroenterology, The First Medical Center of Chinese PLA General Hospital between December 2010 and September 2019. Patients were divided into two groups according to the diagnostic criteria for achalasia: The increased LES-IRP and the normal LES-IRP group. Ultimately, we conducted a retrospective study on 481 patients who received preoperative HRM at our hospital. The study was approved by the Ethics Committee of the Chinese PLA General Hospital (Approval No. S2021-206-01), and consent was obtained from all patients in our study. All patients included in the study were sorted into 2 groups: 71 patients in the normal LES-IRP group (< 15 mmHg) and 410 patients in the increased LES-IRP group (≥ 15 mmHg).
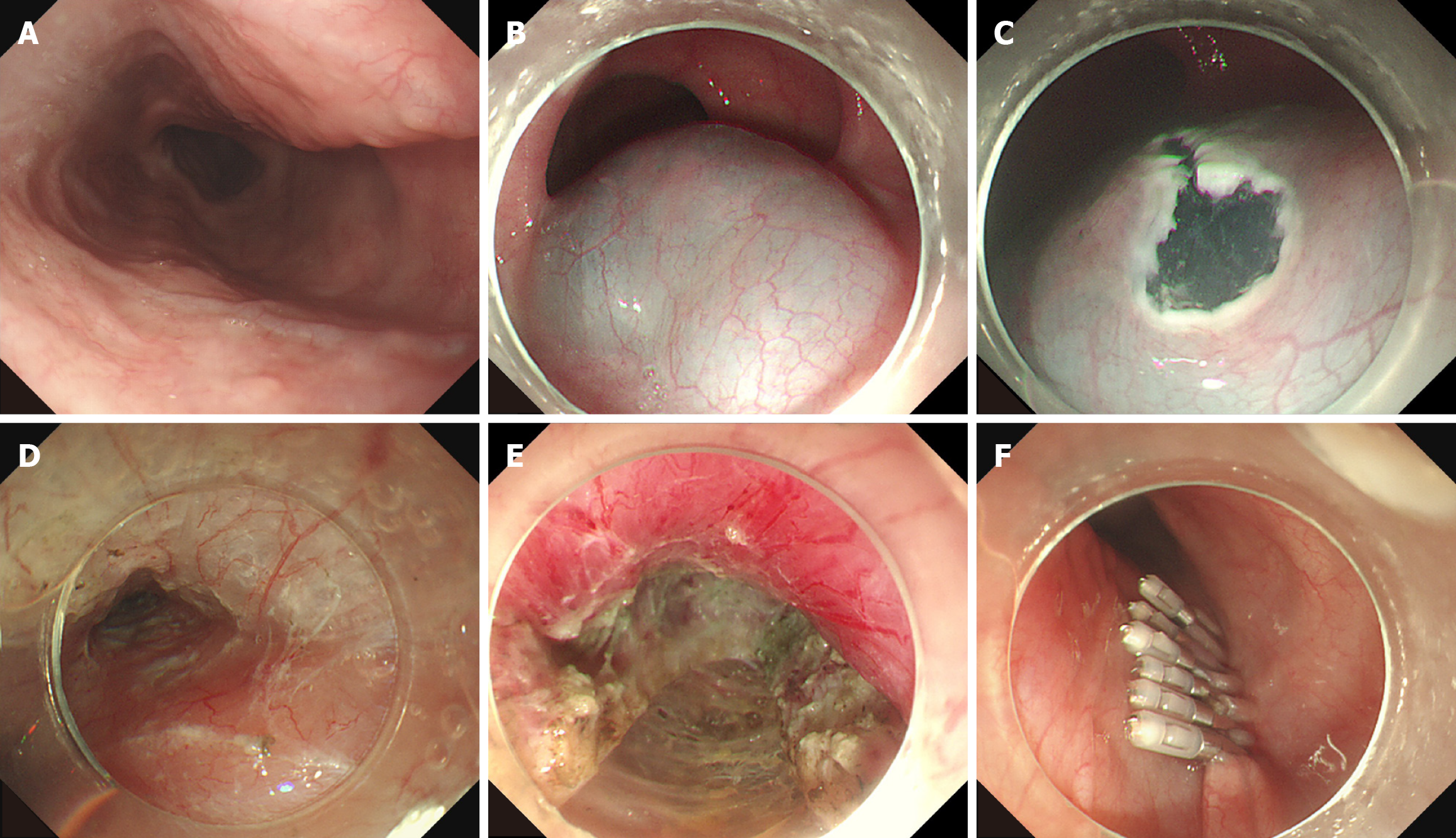
The patients were admitted and fasted for 48 hours before POEM. During the operation, the patients were kept in a supine position with the right shoulder elevated. The procedure of POEM was showed in detail as follows (Figure 1).
The appropriate location of the tunnel was identified. Then, sufficient submucosal injections were conducted to separate the mucosal layer and submucosal layer. The entry incision of the tunnel included a transverse incision, longitudinal incision, and inverse T-shaped incision. An electrosurgical knife was used to dissect between the submucosal layer and muscular layer. Then, the submucosal tunnel was established. The proper myotomy type was selected. Finally, the tunnel opening was closed with metallic clips.
X-ray or computed tomography (CT) was used to evaluate operation-related adverse events, such as pneumothorax, pneumoperitoneum, pneumomediastinum and subcutaneous emphysema. In addition, delayed bleeding, infection-related fever and other complications were also monitored. If these symptoms occurred, active steps were taken in a timely manner. Moreover, as all patients fasted for 3 days after POEM, parenteral nutrition, antibiotics and proton pump inhibitors (PPIs) were used. Then, patients’ diet was gradually transitioned from liquid food to soft meals, and oral PPIs were administered for at least 4 weeks after discharge.
The follow-up visits were scheduled at 3 months, 6 months, 1 year, 2 years, and so on after POEM. All patients were contacted by telephone to assess their complaints, Eckardt scores[15], and GerdQ scores after POEM. Endoscopy, HRM and barium esophagram findings were monitored if possible.
According to the type of data, the median value (interquartile range, Q1-Q3) or numerical value (percentage) is presented. Continuous variables were compared by t test or Mann-Whitney U test. Categorical variables were compared by χ2 test or Fisher exact test. All the statistical analyses, included propensity score matching, were completed with IBS SPSS version 26.0 and GraphPad Prism 8.0. P < 0.05 was considered to indicate a significant difference.
Among the 481 patients included in our study, there were 209 males and 272 females, with a mean age of 44.2 years (range, 19-79 years) and an average body mass index (BMI) of 21.6 kg/m2 (range, 13.9-32.4 kg/m2).
As shown in Table 1, there were 71 patients (14.8%) and 410 patients (85.2%) in the normal LES-IRP group and the increased LES-IRP group, respectively. The median duration of symptoms in the normal LES-IRP group was 72.0 months (Q1-Q3, 24.0-180.0 months), and that in the increased LES-IRP group was 36.0 months (Q1-Q3, 24.0-84.0 months) (P = 0.006). Before the patients underwent POEM, 21 patients (29.5%) in the normal LES-IRP group had undergone previous treatments, whereas 59 patients (14.4%) in the increased LES-IRP group had undergone previous treatments (P = 0.002). Before treatment, the median lower esophageal sphincter (LES) basal pressure and LES-IRP in the normal LES-IRP group were 14.8 mmHg (Q1-Q3, 12.0-20.3 mmHg) and 11.4 mmHg (Q1-Q3, 9.2-12.5 mmHg), respectively, while those in the increased LES-IRP group were 32.3 mmHg (Q1-Q3, 23.7-41.8 mmHg) and 25.7 mmHg (Q1-Q3, 20.3-32.3 mmHg), respectively (P = 0.000). In the normal LES-IRP group, according to the Ling classification[16,17], there were 7 (9.9%) type I cases, 21 (29.6%) type IIa cases, 17 (23.9%) type IIb cases, 22 (31.0%) type IIc cases and 4 (5.6%) type III cases. In the increased LES-IRP group, there were 84 (20.5%) type I cases, 142 (34.6%) type IIa cases, 105 (25.6%) type IIb cases, 66 (16.1%) type IIc cases and 13 (3.2%) type III cases (P = 0.014).
| Normal LES-IRP group (n = 71) | Increased LES-IRP group (n = 410) | P value | |
| Sex, male/female (n) | 37/34 | 172/238 | 0.111 |
| Age, median (Q1-Q3) (years) | 45.0 (35.0-57.0) | 43.0 (33.0-54.0) | 0.134 |
| BMI, median (Q1-Q3) (kg/m2) | 21.5 (19.1-23.8) | 20.9 (19.2-23.7) | 0.543 |
| Duration of symptoms, median (Q1-Q3) (months) | 72.0 (24.0-180.0) | 36.0 (24.0-84.0) | 0.006 |
| Previous treatment | 21 (29.5) | 59 (14.4) | 0.002 |
| Balloon dilation | 10 (14.1) | 30 (7.3) | |
| Botox injection | 2 (2.8) | 16 (3.9) | |
| Temporary stenting | 1 (1.4) | 6 (1.5) | |
| Heller myotomy | 4 (5.6) | 2 (0.5) | |
| POEM | 1 (1.4) | 2 (0.5) | |
| Balloon dilation + botox injection | 1 (1.4) | 2 (0.5) | |
| Balloon dilation + temporary stenting | 2 (2.8) | 1 (0.2) | |
| Pre-treatment HRM | |||
| LES basal pressure, median (Q1-Q3) (mmHg) | 14.8 (12.0-20.3) | 32.3 (23.7-41.8) | 0.000 |
| LES-IRP, median (Q1-Q3) (mmHg) | 11.4 (9.2-12.5) | 25.7 (20.3-32.3) | 0.000 |
| Ling classification | 0.014 | ||
| Type Ling I | 7 (9.9) | 84 (20.5) | |
| Type Ling IIa | 21 (29.6) | 142 (34.6) | |
| Type Ling IIb | 17 (23.9) | 105 (25.6) | |
| Type Ling IIc | 22 (31.0) | 66 (16.1) | |
| Type Ling III | 4 (5.6) | 13 (3.2) |
The procedure-related parameters are shown in Table 2. All patients underwent POEM without severe adverse events.
| Normal LES-IRP group (n = 71) | Increased LES-IRP group (n = 410) | P value | |
| ASA classification | 0.328 | ||
| I | 6 (8.5) | 62 (15.1) | |
| II | 64 (90.1) | 342 (83.4) | |
| III | 1 (1.4) | 6 (1.5) | |
| Operation time, median (Q1-Q3) (minute) | 40.0 (33.0-51.0) | 42.0 (32.0-55.0) | 0.519 |
| Tunnel length, median (Q1-Q3) (cm) | 12.0 (9.0-12.0) | 12.0 (10.0-12.0) | 0.738 |
| Myotomy length, median (Q1-Q3) (cm) | 7.0 (5.0-9.0) | 7.0 (6.0-9.0) | 0.661 |
| Types of myotomy | 0.425 | ||
| Inner circular muscle myotomy | 7 (9.9) | 70 (17.1) | |
| Full-thickness muscle myotomy | 3 (4.2) | 30 (7.3) | |
| Partial-thickness muscle myotomy | 4 (5.6) | 19 (4.6) | |
| Glass-style anti-reflux myotomy | 1 (1.4) | 9 (2.2) | |
| Progressive full-thickness myotomy | 56 (78.9) | 282 (68.8) | |
| Intraoperative adverse events | 5 (7.0) | 58 (14.2) | 0.186 |
| Bleeding | 1 (1.4) | 2 (0.5) | |
| Mucosal injury | 3 (4.2) | 29 (7.1) | |
| Gas-related adverse events | 1 (1.4) | 27 (6.6) | |
| Pneumothorax | 0 (0.0) | 1 (0.2) | |
| Pneumoperitoneum | 1 (1.4) | 13 (3.2) | |
| Pneumomediastinum | 0 (0.0) | 2 (0.5) | |
| Subcutaneous emphysema | 0 (0.0) | 11 (2.7) |
In the normal LES-IRP group, according to the American Society of Anesthesiologists (ASA) classification[18], there were 6 (8.5%) type I cases, 64 (90.1%) type II cases and 1 (1.4%) type III case. The median operation time was 40.0 minutes (Q1-Q3, 33.0-51.0 minutes), and the median tunnel length was 12.0 cm (Q1-Q3, 9.0-12.0 cm), and the median myotomy length was 7.0 cm (5.0-9.0 cm). Regarding the type of myotomy[19], 7 (9.9%) inner circular muscle myotomies, 3 (4.2%) full-thickness muscle myotomies, 4 (5.6%) partial-thickness muscle myotomies, 1 (1.4%) glass-style anti-reflux myotomy and 56 (78.9%) progressive full-thickness myotomies were performed. No severe adverse events occurred during the surgical procedures. Only 5 (7.0%) patients experienced adverse events during the operation, including 1 (1.4%) bleeding event, 3 (4.2%) mucosal injuries and 1 (1.4%) gas-related adverse event (pneumoperitoneum).
In the increased LES-IRP group, regarding the ASA classification, there were 62 (15.1%) type I cases, 342 (83.4%) type II cases and 6 (1.5%) type III cases. The median operation time was 42.0 minutes (Q1-Q3, 32.0-55.0 minutes), and the mean tunnel length was 12.0 cm (Q1-Q3, 10.0-12.0 cm), and the mean myotomy length was 7.0 cm (Q1-Q3, 6.0-9.0 cm). The types of myotomy consisted of 70 (17.1%) inner circular muscle myotomies, 30 (7.3%) full-thickness muscle myotomies, 19 (4.6%) partial-thickness muscle myotomies, 9 (2.2%) glass-style anti-reflux myotomies and 282 (68.8%) progressive full-thickness myotomies. No severe adverse events occurred during the operation. Fifty-eight (14.2%) patients had adverse events during the operation, including 2 (0.5%) bleeding events, 29 (7.1%) mucosal injuries and 27 (6.6%) gas-related adverse events containing 1 (0.2%) case of pneumothorax, 13 (3.2%) cases of pneumoperitoneum, 2 (0.5%) cases of pneumomediastinum, and 11 (2.7%) cases of subcutaneous emphysema.
There was no significant difference in the above procedure-related parameters between the two groups.
As shown in Table 3, the median follow-up period of the normal LES-IRP group was 25.0 months (Q1-Q3, 19.0-57.0 months) and that of the increased LES-IRP group was 41.0 months (Q1-Q3, 23.0-63.0 months) (P = 0.010). An Eckardt score ≤ 3 after POEM was considered clinical success. In the normal LES-IRP group, the median Eckardt score before treatment was 7.0 (Q1-Q3, 5.0-8.0), while the median Eckardt score after treatment was 1.0 (Q1-Q3, 0.0-2.0) and the median pre-post change in the Eckardt score was 5.0 (Q1-Q3, 4.0-7.0). Compared with above, the scores for the increased LES-IRP group were 7.0 (Q1-Q3, 6.0-9.0) (P = 0.132), 1.0 (Q1-Q3, 0.0-2.0) (P = 0.572), and 6.0 (Q1-Q3, 4.0-8.0) (P = 0.068) respectively. There were no significant differences in the Eckardt score between the two groups before or after POEM. In addition, clinical success was recorded for 62 patients (87.3%) and 374 patients (91.2%) in the two groups (P = 0.298).
| Normal LES-IRP group (n = 71) | Increased LES-IRP group (n = 410) | P value | |
| Follow-up period, median (Q1-Q3) (months) | 25.0 (19.0-57.0) | 41.0 (23.0-63.0) | 0.010 |
| Clinical success (Eckardt score ≤ 3) | 62 (87.3) | 374 (91.2) | 0.298 |
| Eckardt score, median (Q1-Q3) | |||
| Pre-treatment | 7.0 (5.0-8.0) | 7.0 (6.0-9.0) | 0.132 |
| Post-treatment | 1.0 (0.0-2.0) | 1.0 (0.0-2.0) | 0.572 |
| Pre-post change | 5.0 (4.0-7.0) | 6.0 (4.0-8.0) | 0.068 |
| GerdQ score, median (Q1-Q3) | 6.0 (6.0-7.0) | 6.0 (6.0-7.0) | 0.200 |
| GerdQ score ≥ 9 | 6 (8.5) | 44 (10.7) | 0.561 |
Reflux was common after POEM[20] and was measured by the GerdQ questionnaire. Jonasson et al[21] concluded that a GerdQ score ≥ 9 reflected the best level of balance regarding sensitivity and specificity for gastroesophageal reflux disease. In our study, the percentages of patients with GerdQ scores ≥ 9 were 8.5% and 10.7% in the normal and increased LES-IRP groups, respectively (P = 0.561). The results showed that the incidence of reflux esophagitis did not increase after POEM in the normal LES-IRP group.
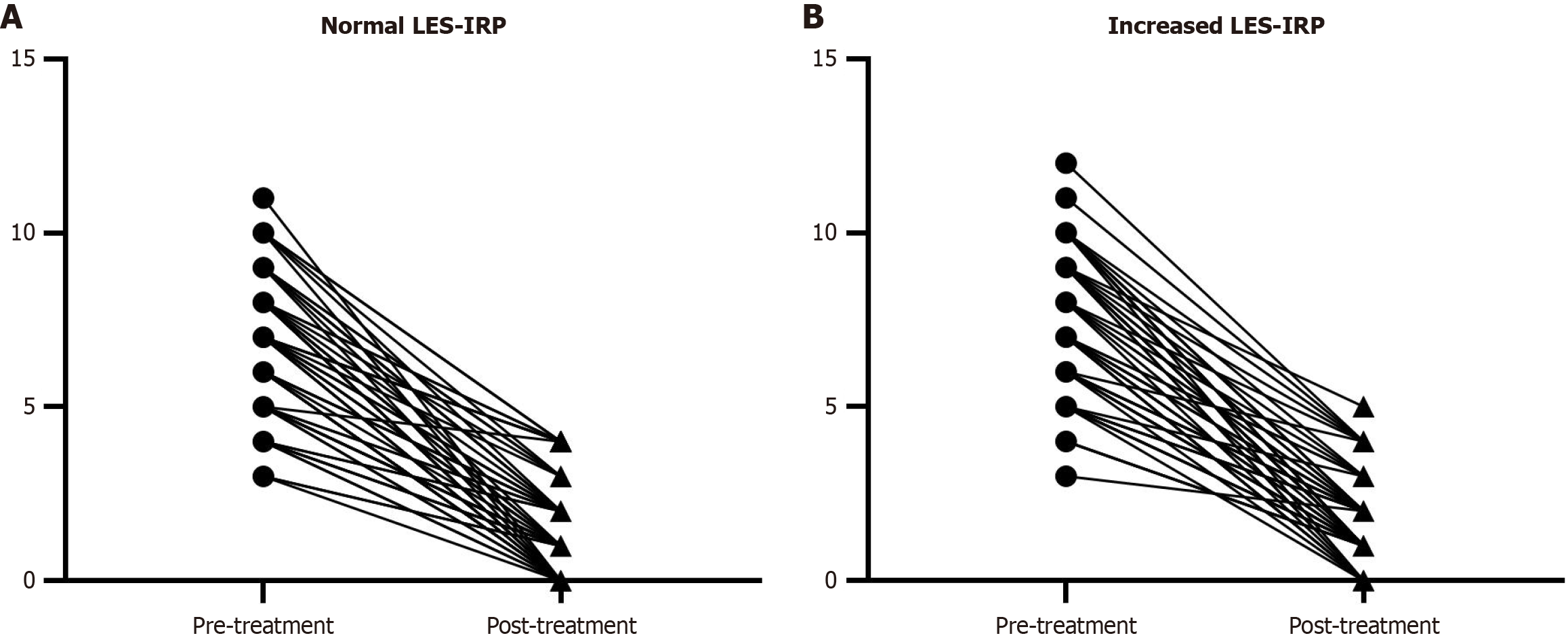
After propensity score matching (sex, age, BMI, duration of symptoms, previous treatment and ASA classification), 69 patients in each group were compared (Table 4). There was no significant difference between the two groups in terms of basal characteristics. The rates of clinical success for patients with normal LES-IRP and increased LES-IRP were 88.4% and 89.9%, respectively (P = 0.784). In addition, the percentage of patients with GerdQ score ≥ 9 in the two groups were 8.7% and 10.1%, respectively (P = 0.771). Figure 2 clearly show the change in the Eckardt score about every patient in the two groups matched by propensity score.
| Normal LES-IRP group (n = 69) | Increased LES-IRP group (n = 69) | P value | |
| Sex, male/female (n) | 35/34 | 41/28 | 0.305 |
| Age, median (Q1-Q3) (years) | 45.0 (34.0-55.0) | 44.0 (35.5-56.0) | 0.797 |
| BMI, median (Q1-Q3) (kg/m2) | 21.5 (19.1-23.7) | 20.9 (19.0-24.1) | 0.764 |
| Duration of symptoms, median (Q1-Q3) (months) | 60.0 (24.0-174.0) | 60.0 (24.0-120.0) | 0.582 |
| Previous treatment | 19 (27.5) | 18 (26.1) | 0.848 |
| ASA classification | 0.573 | ||
| I | 6 | 8 | |
| II | 62 | 59 | |
| III | 1 | 2 | |
| Ling classification | 0.145 | ||
| Type Ling I | 6 (8.7) | 16 (23.2) | |
| Type Ling IIa | 21 (30.4) | 18 (26.1) | |
| Type Ling IIb | 17 (24.7) | 16 (23.2) | |
| Type Ling IIc | 21 (30.4) | 18 (26.1) | |
| Type Ling III | 4 (5.8) | 1 (1.4) | |
| Pre-treatment HRM | |||
| LES basal pressure, median (Q1-Q3) (mmHg) | 14.8 (12.0-20.3) | 31.9 (22.5-40.4) | 0.000 |
| LES-IRP, median (Q1-Q3) (mmHg) | 11.4 (9.3-12.5) | 22.3 (19.0-28.4) | 0.000 |
| Follow-up period, median (Q1-Q3) (month) | 25.0 (18.5-54.5) | 42.0 (28.5-63.5) | 0.002 |
| Clinical success (Eckardt score ≤ 3) | 61 (88.4) | 62 (89.9) | 0.784 |
| Intraoperative adverse events | 5 (7.1) | 8 (11.5) | 1.000 |
| Bleeding | 1 (1.4) | 1 (1.4) | |
| Mucosal injury | 3 (4.3) | 4 (5.8) | |
| Gas-related adverse events | 1 (1.4) | 3 (4.3) | |
| Pneumothorax | 0 (0.0) | 1 (1.4) | |
| Pneumoperitoneum | 1 (1.4) | 2 (2.9) | |
| Eckardt score, median (Q1-Q3) | |||
| Pre-treatment | 7.0 (5.0-8.0) | 7.0 (6.0-9.0) | 0.021 |
| Post-treatment | 1.0 (0.0-2.0) | 1.0 (1.0-2.0) | 0.201 |
| Pre-post change | 5.0 (4.0-7.0) | 6.0 (4.0-8.0) | 0.086 |
| GerdQ score, median (Q1-Q3) | 6.0 (6.0-7.0) | 6.0 (6.0-7.0) | 0.917 |
| GerdQ score ≥ 9 | 6 (8.7) | 7 (10.1) | 0.771 |
Achalasia is considered an esophageal motility or functional disorder[22]. There are several ways to treat patients with achalasia, including medicine, endoscopic operations, and surgery. POEM has been indicated to be a safe and effective method for treating patients since Inoue et al[8] developed it for treating achalasia in 2010. The diagnosis of achalasia relies mainly on HRM, clinical manifestations, patient past medical history, the results of barium esophagram and endoscopy need to be considered as well. Patients with normal LES-IRP and those who have been previously treated also exhibit clinical manifestations and abnormal endoscopic findings. Therefore, we conducted research on the outcomes of POEM in patients with normal LES-IRP and found that POEM is safe and effective for treating achalasia, including in patients with normal LES-IRP.
Most patients with achalasia have increased LES-IRP. However, according to the Chicago Classification Standards for Esophageal Dynamics Disorders v3.0, some patients have normal LES-IRP[23], and their main presentations are the absence of esophageal contractions and increased esophageal lumen pressure. In our study, we found that patients with normal LES pressure, especially those who had been treated previously, had obvious clinical symptoms and disorders of esophageal motility, such as weight loss and dysphagia. In addition, patients with recurrent achalasia after surgery often had normal LES-IRP.
Considering that such patients had a long disease course, high disease severity, and esophageal body motility disorders, esophageal dilation was found in these patients. In terms of patients’ past medical history, the patients in the normal LES-IRP group had a significantly greater possibility of having previously undergone treatment than increased LES-IRP group (P = 0.002). In addition, the duration of symptoms (P = 0.006) and the percentage of patients with specific Ling classifications (P = 0.014) were significantly different between the two groups. These differences indicated that patients with normal LES-IRP tended to have a longer course of achalasia. Although some of these patients with a long disease course had been treated previously, stasis of ingested food in the esophagus made the esophageal lumen more dilated. Li and Linghu[17] proposed Ling classification based on the morphology of the esophageal lumen, and we found that the esophageal lumen of type Ling II and type Ling III was more enlarged and twisted compared with type Ling I. Therefore, the percentages of patients with Ling classification types II and III in the normal LES-IRP group were larger than those in the increased LES-IRP group.
According to our study, POEM is safe and effective for patients with either normal or increased LES-IRP. In the normal LES-IRP group, only 5 (7.0%) patients experienced adverse events during the operation, and in the increased LES-IRP group, 58 (14.2%) patients experienced adverse events. The results confirmed that there was no significant difference in safety between the two groups (P = 0.186). In addition, based on the rate of clinical success, we found that the efficacy of the two groups was equal (P = 0.298). After propensity score matching, 69 patients in each group were compared, and we found that there was no significant difference between the two groups in terms of the rate of clinical success (P = 0.784) and safety (P = 1.000).
In previous studies, the LES pressure was lower after POEM than before[24]. In our study, as patients in the normal LES-IRP group had a normal LES pressure, the LES pressure relief rate was low, but the outflow of food was unob
By analyzing the follow-up data, we found that the patients in the two groups experienced obvious relief of dysphagia. To evaluate the occurrence of reflux symptoms, we used the GerdQ questionnaire for every patient, and the results showed that there were no differences between the groups (P = 0.561). After propensity score matching, there was still no significant difference between two groups in reflux symptoms (P = 0.771). Therefore, we speculate that for patients with normal LES-IRP, POEM is not associated with a greater incidence of reflux symptoms.
For patients with achalasia, pneumatic dilation is one of the most commonly performed treatments. Ponds et al[29] confirmed that compared with pneumatic dilation, POEM had an obviously greater treatment success rate. Compared with HM, POEM is superior in terms of short-term efficacy[30]. As a result, for patients with achalasia, POEM is recommended as the first choice, and for those who have been treated before, POEM is also recommended if there are no contraindications. Besides, for patients with achalasia who also have esophageal diverticulum, such as Zenker’s diverticulum and Killian-Jamieson diverticulum, Zenker-POEM and Killian-Jamieson POEM are safe and effective alternative treatments for their benefits of more precise myotomy and reduced risk of perforation[31-33].
As patients came from different regions, the postoperative follow-up was mainly based on Eckardt score and GerdQ questionnaire. The follow-up period between the two groups remained unbalanced. Besides, our study was retrospective and was conducted at a single center. Therefore, selection bias, the potential for selection bias, information bias, confounding bias and unmeasured confounders may have affected our results, which is a limitation of our study. Multicenter prospective studies are necessary to obtain clearer evidence.
POEM is safe and effective for treating achalasia and patients with normal LES-IRP. The rates of clinical success in the normal LES-IRP and increased LES-IRP groups were 87.3% and 91.2%, respectively. In patients with normal LES-IRP, compared with patients with increased LES-IRP, POEM is not associated with a greater incidence of reflux symptoms.
| 1. | Tuason J, Inoue H. Current status of achalasia management: a review on diagnosis and treatment. J Gastroenterol. 2017;52:401-406. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 42] [Cited by in RCA: 45] [Article Influence: 5.6] [Reference Citation Analysis (0)] |
| 2. | Francis DL, Katzka DA. Achalasia: update on the disease and its treatment. Gastroenterology. 2010;139:369-374. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 146] [Cited by in RCA: 154] [Article Influence: 10.3] [Reference Citation Analysis (0)] |
| 3. | Park W, Vaezi MF. Etiology and pathogenesis of achalasia: the current understanding. Am J Gastroenterol. 2005;100:1404-1414. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 253] [Cited by in RCA: 255] [Article Influence: 12.8] [Reference Citation Analysis (0)] |
| 4. | Felix VN, DeVault K, Penagini R, Elvevi A, Swanstrom L, Wassenaar E, Crespin OM, Pellegrini CA, Wong R. Causes and treatments of achalasia, and primary disorders of the esophageal body. Ann N Y Acad Sci. 2013;1300:236-249. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 8] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 5. | Schlottmann F, Patti MG. Esophageal achalasia: current diagnosis and treatment. Expert Rev Gastroenterol Hepatol. 2018;12:711-721. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 48] [Cited by in RCA: 62] [Article Influence: 8.9] [Reference Citation Analysis (0)] |
| 6. | Vaezi MF, Pandolfino JE, Yadlapati RH, Greer KB, Kavitt RT. ACG Clinical Guidelines: Diagnosis and Management of Achalasia. Am J Gastroenterol. 2020;115:1393-1411. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 106] [Cited by in RCA: 238] [Article Influence: 47.6] [Reference Citation Analysis (0)] |
| 7. | Rolland S, Paterson W, Bechara R. Achalasia: Current therapeutic options. Neurogastroenterol Motil. 2023;35:e14459. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 8. | Inoue H, Minami H, Kobayashi Y, Sato Y, Kaga M, Suzuki M, Satodate H, Odaka N, Itoh H, Kudo S. Peroral endoscopic myotomy (POEM) for esophageal achalasia. Endoscopy. 2010;42:265-271. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1168] [Cited by in RCA: 1234] [Article Influence: 82.3] [Reference Citation Analysis (1)] |
| 9. | Pandolfino JE, Gawron AJ. Achalasia: a systematic review. JAMA. 2015;313:1841-1852. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 278] [Cited by in RCA: 297] [Article Influence: 29.7] [Reference Citation Analysis (0)] |
| 10. | Schlottmann F, Luckett DJ, Fine J, Shaheen NJ, Patti MG. Laparoscopic Heller Myotomy Versus Peroral Endoscopic Myotomy (POEM) for Achalasia: A Systematic Review and Meta-analysis. Ann Surg. 2018;267:451-460. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 211] [Cited by in RCA: 256] [Article Influence: 42.7] [Reference Citation Analysis (0)] |
| 11. | Kahrilas PJ, Bredenoord AJ, Fox M, Gyawali CP, Roman S, Smout AJ, Pandolfino JE; International High Resolution Manometry Working Group. The Chicago Classification of esophageal motility disorders, v3.0. Neurogastroenterol Motil. 2015;27:160-174. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1373] [Cited by in RCA: 1452] [Article Influence: 145.2] [Reference Citation Analysis (0)] |
| 12. | Mearin F, Malagelada JR. Complete lower esophageal sphincter relaxation observed in some achalasia patients is functionally inadequate. Am J Physiol Gastrointest Liver Physiol. 2000;278:G376-G383. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 31] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 13. | Sanaka MR, Parikh MP, Thota PN, Gupta NM, Gabbard S, Lopez R, Murthy S, Raja S. Peroral Endoscopic Myotomy Is Effective for Patients With Achalasia and Normal Lower-Esophageal Sphincter Relaxation Pressures. Clin Gastroenterol Hepatol. 2019;17:2803-2805. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 14. | Ponds FA, Bredenoord AJ, Kessing BF, Smout AJ. Esophagogastric junction distensibility identifies achalasia subgroup with manometrically normal esophagogastric junction relaxation. Neurogastroenterol Motil. 2017;29. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 79] [Cited by in RCA: 100] [Article Influence: 12.5] [Reference Citation Analysis (0)] |
| 15. | Laurino-Neto RM, Herbella F, Schlottmann F, Patti M. Evaluation of esophageal achalasia: from symptoms to the Chicago classification. Arq Bras Cir Dig. 2018;31:e1376. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 13] [Cited by in RCA: 20] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 16. | Chai N, Zhang X, Xiong Y, Ding H, Feng J, Li Y, Yao S, Niu X, Linghu E. Ling classification applied in the preoperative safety and effectiveness assessment of POEM. Surg Endosc. 2017;31:368-373. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 10] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 17. | Li HK, Linghu EQ. New endoscopic classification of achalasia for selection of candidates for peroral endoscopic myotomy. World J Gastroenterol. 2013;19:556-560. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 26] [Cited by in RCA: 22] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 18. | Horvath B, Kloesel B, Todd MM, Cole DJ, Prielipp RC. The Evolution, Current Value, and Future of the American Society of Anesthesiologists Physical Status Classification System. Anesthesiology. 2021;135:904-919. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 172] [Article Influence: 43.0] [Reference Citation Analysis (0)] |
| 19. | Chai NL, Li HK, Linghu EQ, Li ZS, Zhang ST, Bao Y, Chen WG, Chiu PW, Dang T, Gong W, Han ST, Hao JY, He SX, Hu B, Hu B, Huang XJ, Huang YH, Jin ZD, Khashab MA, Lau J, Li P, Li R, Liu DL, Liu HF, Liu J, Liu XG, Liu ZG, Ma YC, Peng GY, Rong L, Sha WH, Sharma P, Sheng JQ, Shi SS, Seo DW, Sun SY, Wang GQ, Wang W, Wu Q, Xu H, Xu MD, Yang AM, Yao F, Yu HG, Zhou PH, Zhang B, Zhang XF, Zhai YQ. Consensus on the digestive endoscopic tunnel technique. World J Gastroenterol. 2019;25:744-776. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 41] [Cited by in RCA: 34] [Article Influence: 5.7] [Reference Citation Analysis (0)] |
| 20. | Arevalo G, Sippey M, Martin-Del-Campo LA, He J, Ali A, Marks J. Post-POEM reflux: who's at risk? Surg Endosc. 2020;34:3163-3168. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 13] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 21. | Jonasson C, Wernersson B, Hoff DA, Hatlebakk JG. Validation of the GerdQ questionnaire for the diagnosis of gastro-oesophageal reflux disease. Aliment Pharmacol Ther. 2013;37:564-572. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 132] [Cited by in RCA: 185] [Article Influence: 15.4] [Reference Citation Analysis (0)] |
| 22. | Boeckxstaens GE, Zaninotto G, Richter JE. Achalasia. Lancet. 2014;383:83-93. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 390] [Cited by in RCA: 428] [Article Influence: 38.9] [Reference Citation Analysis (0)] |
| 23. | Sanagapalli S, Roman S, Hastier A, Leong RW, Patel K, Raeburn A, Banks M, Haidry R, Lovat L, Graham D, Sami SS, Sweis R. Achalasia diagnosed despite normal integrated relaxation pressure responds favorably to therapy. Neurogastroenterol Motil. 2019;31:e13586. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 27] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 24. | Feng J, Ali RW, Hao JY, Kong GX, Yang LH, Huang XJ. Peroral endoscopic myotomy for esophageal motility disorders. Esophagus. 2020;17:11-18. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9] [Cited by in RCA: 9] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 25. | Filicori F, Dunst CM, Sharata A, Abdelmoaty WF, Zihni AM, Reavis KM, Demeester SR, Swanström LL. Long-term outcomes following POEM for non-achalasia motility disorders of the esophagus. Surg Endosc. 2019;33:1632-1639. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 44] [Article Influence: 6.3] [Reference Citation Analysis (0)] |
| 26. | Vosoughi K, Ichkhanian Y, Benias P, Miller L, Aadam AA, Triggs JR, Law R, Hasler W, Bowers N, Chaves D, Ponte-Neto AM, Draganov P, Yang D, El Halabi M, Sanaei O, Brewer Gutierrez OI, Bulat RS, Pandolfino J, Khashab M. Gastric per-oral endoscopic myotomy (G-POEM) for refractory gastroparesis: results from an international prospective trial. Gut. 2022;71:25-33. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 75] [Article Influence: 25.0] [Reference Citation Analysis (0)] |
| 27. | Parsa N, Friedel D, Stavropoulos SN. POEM, GPOEM, and ZPOEM. Dig Dis Sci. 2022;67:1500-1520. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 12] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 28. | Vohra I, Gopakumar H, Adler DG. G-POEM for gastroparesis: past, present and future. Curr Opin Gastroenterol. 2023;39:390-396. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 29. | Ponds FA, Fockens P, Lei A, Neuhaus H, Beyna T, Kandler J, Frieling T, Chiu PWY, Wu JCY, Wong VWY, Costamagna G, Familiari P, Kahrilas PJ, Pandolfino JE, Smout AJPM, Bredenoord AJ. Effect of Peroral Endoscopic Myotomy vs Pneumatic Dilation on Symptom Severity and Treatment Outcomes Among Treatment-Naive Patients With Achalasia: A Randomized Clinical Trial. JAMA. 2019;322:134-144. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 209] [Cited by in RCA: 256] [Article Influence: 42.7] [Reference Citation Analysis (0)] |
| 30. | Park CH, Jung DH, Kim DH, Lim CH, Moon HS, Park JH, Jung HK, Hong SJ, Choi SC, Lee OY; Achalasia Research Group of the Korean Society of Neurogastroenterology and Motility. Comparative efficacy of per-oral endoscopic myotomy and Heller myotomy in patients with achalasia: a meta-analysis. Gastrointest Endosc. 2019;90:546-558.e3. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 29] [Article Influence: 4.8] [Reference Citation Analysis (0)] |
| 31. | Assefa RL, Bejjani M, Mehta A, Shrigiriwar A, Fayyaz F, Shimamura Y, Inoue H, Mandarino FV, Azzolini F, Bowers SP, Li Z, Robles-Medranda C, Arevalo M, Dhir V, Andrisani G, Tantau A, Lajin M, Sampath K, Khashab MA. Peroral endoscopic myotomy as a treatment for Killian-Jamieson diverticulum (KJ-POEM). Endosc Int Open. 2024;12:E1214-E1219. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 32. | Dell'Anna G, Fasulo E, Fanizza J, Barà R, Vespa E, Barchi A, Cecinato P, Fuccio L, Annese V, Malesci A, Azzolini F, Danese S, Mandarino FV. The Endoscopic Management of Zenker's Diverticulum: A Comprehensive Review. Diagnostics (Basel). 2024;14:2155. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 5] [Reference Citation Analysis (0)] |
| 33. | Swei E, Pokala SK, Menard-Katcher P, Wagh MS. Comparison of Zenker's per-oral endoscopic myotomy (Z-POEM) with standard flexible endoscopic septotomy for Zenker's diverticulum: a prospective study with 2-year follow-up. Surg Endosc. 2023;37:6818-6823. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 15] [Article Influence: 7.5] [Reference Citation Analysis (0)] |