Published online Apr 27, 2025. doi: 10.4240/wjgs.v17.i4.103700
Revised: February 25, 2025
Accepted: March 5, 2025
Published online: April 27, 2025
Processing time: 79 Days and 23.3 Hours
Tumor progression in patients with esophageal precancerous lesions (EPLs) or early esophageal carcinoma (EEC) is typically confined in both extent and lo
To determine the effect of endoscopic submucosal dissection (ESD) on efficacy, serum tumor markers (STMs), and 6-month postoperative recurrence rate in patients with either EPL or EEC.
This study initially enrolled 120 patients with EPL or EEC, who were admitted from April 2021 to April 2024. Participants were divided into the control group (60 cases), which underwent thoracotomy, and the research group (60 cases) which received ESD treatment. The comparative analysis involved information regarding the efficacy (dissection area and resection rate per unit time), complications (delayed bleeding, wound infection, esophageal reflux, and postoperative esophageal stenosis), surgery-related parameters (bleeding volume, operation duration, and hospital length of stay), STMs [carcinoembryonic antigen (CEA), carbohydrate antigen 724 (CA724), and tumor-specific growth factor (TSGF)], and the 6-month postoperative recurrence rate of the two groups.
Data indicated statistically higher dissection area and resection rate per unit of time in the research group than in the control group. Meanwhile, the research group demonstrated a notably lower overall incidence rate of complications, bleeding volume, operation duration, and hospital length of stay. Further, the CEA, CA724, and TSGF were markedly reduced in the research group after treatment, which were statistically lower compared to the baseline and those of the control group. Finally, during the follow-up, a comparable 6-month postoperative recurrence rate was determined in the two groups.
ESD is clinically effective and safe for EPL and EEC and can significantly restore abnormally increased levels of STMs.
Core Tip: Studies on the efficacy of endoscopic submucosal dissection (ESD) in treating esophageal precancerous lesions (EPLs) or early esophageal carcinoma (EEC), as well as its effects on serum tumor markers (STMs) and the 6-month postoperative recurrence rate, remains limited. This study included 120 patients with EPL or EEC and compared the clinical outcomes of ESD with thoracotomy. The results indicate that ESD provides significant clinical advantages for these patients, including larger dissection area, higher resection rate per unit time, reduced risk of complications, less intraoperative bleeding, shorter operative duration, and accelerated recovery. Moreover, ESD effectively suppresses abnormal STM levels, such as carcinoembryonic antigen, carbohydrate antigen 724, and tumor-specific growth factor. These results provide comprehensive and robust clinical evidence to support the use of ESD in EPL and EEC management.
- Citation: Yuan XC, Jia P, Tian T, Zhu J, Zhang XY. Endoscopic submucosal dissection for esophageal precancerous lesions and early esophageal carcinoma: Analysis of efficacy and serum tumor markers. World J Gastrointest Surg 2025; 17(4): 103700
- URL: https://www.wjgnet.com/1948-9366/full/v17/i4/103700.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v17.i4.103700
Esophageal carcinoma (EC), as a prevalent malignant neoplasm in the digestive tract, ranks as the sixth leading cause of cancer-related mortality globally[1]. Its etiological factors potentially involve smoking, alcohol consumption, low fruit and vegetable ingestion, gastroesophageal reflux, and predisposing genes, all of which may augment the risk of EC development[2]. Statistically, the 5-year survival rates of EC in the United States and China are 18.5% and 36.9%, respectively, demonstrating a poor prognosis, which is primarily related to the majority of patients being diagnosed at an advanced stage[3,4]. To improve the 5-year survival rate and the prognosis of patients with EC, early diagnosis and prompt intervention are of paramount significance[5]. The extent and location of tumor progression are circumscribed for patients with esophageal precancerous lesions (EPLs) and early EC (EEC), and effective intervention at this stage confers superior therapeutic efficacy and prognosis[6,7]. Endoscopic submucosal dissection (ESD) represents the treatment of choice for patients with EPL or EEC. Compared with conventional thoracotomy, ESD provides advantages such as less surgical trauma and esophageal physiological structure preservation. It enables en-bloc and complete lesion resection and contributes to reduced risk of distant metastasis[8-10]. Besides, this technique provides an en-bloc specimen; thus, it furnishes more detailed pathological information for risk stratification in esophageal diseases[11]. Ning et al[12] indicated that, when ESD is used to treat patients with EEC, it entails a low recurrence risk while enabling relatively high overall, R0, and radical resection rates. However, this surgical modality has certain disadvantages. Specifically, the risk of postoperative esophageal stenosis is as high as 70%–80% if the resection exceeds 75% of the circumference, and the risk approaches nearly 100% if the entire circumference is resected[13]. The present study primarily focuses on analyzing the effect of ESD on the efficacy of EPL and EEC treatment, serum tumor markers (STMs), and the six-month postoperative recurrence rate. Studies in this domain are scarce, and this research aims to provide more abundant and comprehensive clinical evidence and practical guidance.
This study included 120 patients with EPL or EEC, who visited the Affiliated Taizhou Second People’s Hospital of Yangzhou University from April 2021 to April 2024. Of the participants, 60 underwent thoracotomy (control group) and 60 received ESD treatment (research group). The male-to-female ratios of the control and research groups were 43:17 and 40:20, with a mean age of 70.20 ± 6.09 and 68.20 ± 7.00 years, respectively.
Inclusion criteria: All patients were diagnosed with EPL or EEC based on gastroscopy and pathological diagnosis and conformed to the surgical indications, with an expected survival period of over 3 months and complete clinical data available.
Exclusion criteria: Patients with comorbid cardiocerebrovascular diseases (hypertension, heart diseases, liver disorders, kidney diseases, etc.), autoimmune deficiency, coagulation dysfunction, cognitive impairment, or psychological disorders, such as depression, as well as those with other concurrent malignant tumors.
The control group received a conventional thoracotomy. The specific measures were as follows. After routine disinfection, an incision was created from the posterior–lateral part of the left chest, and the lateral muscle group and intercostal muscles were dissected. Subsequently, the nature, size, and location of the esophageal tumor were identified, and the lesion and enlarged lymph nodes were removed. An effective resection was performed at a position 6–8 cm above the tumor, and a gastric tube and a nutrition tube were placed. Finally, routine sutures and hemostasis were performed.
The research group underwent ESD. Magnifying endoscopy combined with image-enhanced technology was used to assess the microvascular and microsurface structures of the lesions, enabling precise pathological tissue identification. Part of the tissue was extracted through the gastroscope for biopsy, and iodine staining was conducted to assess whether it met the EC or EPL pathological criteria. The iodine staining patterns within the lesion areas were meticulously analyzed to clearly define the lesion boundaries. The distribution range and metastasis status of the lesion were then evaluated using endoscopic ultrasonography. An argon knife electrocoagulation was utilized to mark the area adjacent to the lesion, and a mixture consisting of glycerol fructose (to rapidly elevate the lesion and minimize the bleeding risk) and methylene blue (to enhance lesion visibility and delineate its margins) was injected into the lesion and the surrounding mucosa to make the lesion protrude. The injection volume was tailored based on the lesion’s size and location, ranging from 5 to 10 mL. The mucosa adjacent to the lesion was then cut off with a needle-like knife along the mark, and the mucosal tissue at the lower edge of the lesion was gradually dissected to achieve complete resection. Anti-infection and hemostasis were performed postoperatively to prevent cross-infection.
Efficacy evaluation: The dissection area and the resection rate per unit time (calculated as the dissection area-to-operation duration ratio) of patients in both groups were compared and recorded.
Complication assessment: Cases with adverse events, including delayed bleeding, wound infection, esophageal reflux, and postoperative esophageal stenosis in both groups, were observed and counted, with the incidence rate calculated.
Surgery-related parameter analysis: The bleeding volume, operation duration, and hospital length of stay of both groups were assessed and compared.
STM measurement: Preoperatively and 1 week postoperatively, 5 mL of early-morning venous blood was collected on an empty stomach and sent to the laboratory for assessment after centrifugation. Carcinoembryonic antigen (CEA), carbohydrate antigen 724 (CA724), and tumor-specific growth factor (TSGF) levels were determined using enzyme-linked immunosorbent assay.
Prognosis evaluation: All patients underwent a 6-month follow-up after discharge using telephone, QQ, WeChat, and email to record and statistically analyze their recurrence rates.
In this research, the Statistical Package for the Social Sciences version 21.0 statistical software was used for data analysis. Statistical description was conducted using mean ± SE of the mean for quantitative data. The comparison of quantitative data between the two groups was conducted using the t-test, and the paired t-test was utilized for the comparison between pre- and posttreatment data within the group. Frequency (percentage) was used for statistical description and the intergroup comparison was conducted using the χ2 test for qualitative data. A P value of < 0.05 was considered statistically significant.
No significant differences were observed in the baseline data, such as gender, age, disease course, lesion site, and family medical history, between the control and research groups (P > 0.05, Table 1).
| Indicators | Control group (n = 60) | Research group (n = 60) | t value | P value |
| Gender, n (%) | 0.352 | 0.553 | ||
| Male | 43 (71.67) | 40 (66.67) | ||
| Female | 17 (28.33) | 20 (33.33) | ||
| Age (years) | 70.20 ± 6.09 | 68.20 ± 7.00 | 1.670 | 0.098 |
| Disease course (years) | 2.70 ± 0.67 | 2.58 ± 0.67 | 0.981 | 0.329 |
| Lesion site, n (%) | 0.357 | 0.836 | ||
| Upper esophageal segment | 20 (33.33) | 23 (38.33) | ||
| Middle esophageal segment | 23 (38.33) | 22 (36.67) | ||
| Lower esophageal segment | 17 (28.33) | 15 (25.00) | ||
| Family medical history, n (%) | 0.745 | 0.388 | ||
| Without | 48 (80.00) | 44 (73.33) | ||
| With | 12 (20.00) | 16 (26.67) |
The dissection area in the research group was statistically greater than in the control group (P < 0.001), as was the resection rate per unit time (P < 0.001, Table 2).
| Indicators | Control group (n = 60) | Research group (n = 60) | t value | P value |
| Dissection area (cm2) | 6.76 ± 5.95 | 10.17 ± 4.64 | 3.501 | < 0.001 |
| Resection rate per unit time (mm2/min) | 3.03 ± 3.20 | 9.65 ± 6.54 | 7.043 | < 0.001 |
Delayed bleeding, wound infection, esophageal reflux, and postoperative esophageal stenosis were observed in 3, 9, 19, and 9 cases in the control group and 2, 0, 4, and 4 cases in the research group, respectively. Incidences of wound infection, esophageal reflux, and total complications were markedly lower in the research group than in the control group (P < 0.05, Table 3).
| Indicators | Control group (n = 60) | Research group (n = 60) | χ2 value | P value |
| Delayed bleeding | 3 (5.00) | 2 (3.33) | 0.209 | 0.648 |
| Wound infection | 9 (15.00) | 0 (0.00) | 9.730 | 0.002 |
| Esophageal reflux | 19 (31.67) | 4 (6.67) | 12.102 | < 0.001 |
| Postoperative esophageal stenosis | 9 (15.00) | 4 (6.67) | 2.157 | 0.142 |
| Total | 40 (66.67) | 10 (16.67) | 30.857 | < 0.001 |
Statistical analysis of the bleeding volume, operation duration, and hospital length of stay of the two groups revealed that each indicator in the research group was significantly lower than that in the control group (P < 0.001, Table 4).
| Indicators | Control group (n = 60) | Research group (n = 60) | t value | P value |
| Bleeding volume (mL) | 151.83 ± 126.35 | 31.75 ± 23.68 | 7.236 | < 0.001 |
| Operation duration (hours) | 4.05 ± 1.14 | 2.15 ± 1.02 | 9.621 | < 0.001 |
| Hospital length of stay (days) | 21.70 ± 6.52 | 9.63 ± 2.31 | 13.516 | < 0.001 |
Analysis of STMs, including CEA, CA724, and TSGF, pre- and postoperatively revealed no significant between-group differences in all markers preoperatively (P > 0.05). Further, all markers in both groups exhibited a significant downward trend postoperatively (P < 0.01), with more notable decreases in the research group than in the control group (P < 0.05, Table 5).
| Indicators | Control group (n = 60) | Research group (n = 60) | t value | P value |
| CEA (ng/mL) | ||||
| Before surgery | 12.65 ± 3.33 | 12.86 ± 3.66 | 0.329 | 0.743 |
| After surgery | 3.19 ± 2.15a | 2.35 ± 1.60a | 2.428 | 0.017 |
| CA724 (U/mL) | ||||
| Before surgery | 27.53 ± 5.35 | 28.27 ± 5.40 | 0.754 | 0.452 |
| After surgery | 4.06 ± 3.70a | 2.77 ± 1.93a | 2.394 | 0.018 |
| TSGF (U/mL) | ||||
| Before surgery | 96.50 ± 20.80 | 97.37 ± 22.00 | 0.223 | 0.824 |
| After surgery | 49.83 ± 13.26a | 39.22 ± 14.18a | 4.233 | < 0.001 |
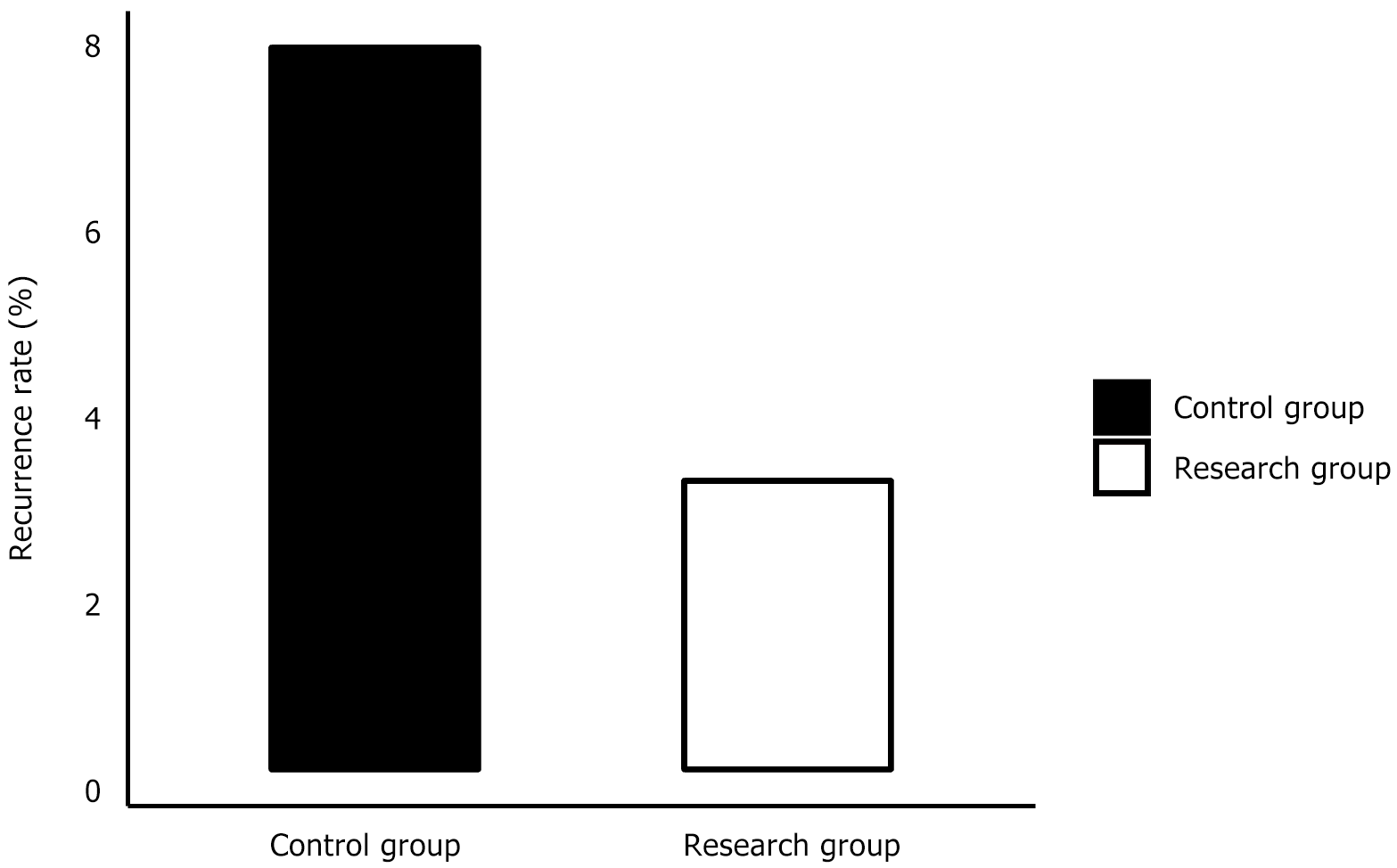
The control and research groups involved five and 2 recurrence cases, respectively, 6 months postoperatively. The two groups were not statistically different in the recurrence rate (χ2 = 1.365, P = 0.243, Figure 1).
This study revealed that both the dissection area and the resection rate per unit time were statistically higher in the research group than in the control group, indicating that ESD demonstrates superior efficacy compared to thoracotomy in treating patients with EPL or EEC. During the ESD procedure, surgeons introduce an endoscope into the esophagus and conduct precise manipulations to obtain high-quality tissue samples, thereby facilitating the acquisition of more accurate pathological assessment information. This, in turn, enables more appropriate treatment regimen formulation based on lesion severity[14]. The most prevalent complications in the control group include esophageal reflux, wound infection, postoperative esophageal stenosis, and delayed bleeding, whereas esophageal reflux, postoperative esophageal stenosis, and delayed bleeding were observed in the research group. The research group demonstrated a lower overall complication rate than the control group, indicating that ESD is associated with a higher safety profile in treating patients with EPL or EEC. Yu et al[15] revealed the operation duration as an independent predictor of postoperative esophageal stenosis in patients with EEC or EPL. In the current study, the shorter operation duration of ESD helps, to a certain extent, decrease the risk of postoperative esophageal stenosis. Furthermore, the research group demonstrated significant reductions in bleeding volume, operation duration, and hospital length of stay. This indicates that ESD for patients with EPL or EEC is beneficial for reducing intraoperative bleeding, shortening the surgical procedure, and facilitating recovery. The underlying mechanism may involve the introduction of normal saline or other injections into the esophageal submucosa via an endoscope during ESD surgery for the mucosal layer bulges to form a protrusion, enhancing surgical field clarity and lesion boundary demarcation, and consequently reducing bleeding and tissue damage[16]. Moreover, ESD only requires tissue sampling from the local lesion rather than complete esophageal resection, which obviates the requirement for total esophageal reconstruction surgery and promotes rapid patient recovery[17]. Li et al[18] revealed that preincision traction using an internal clip-with-spring device in colorectal ESD treatment, compared with conventional on-demand traction, further shortened the operation duration and postoperative hospital length of stay while being advantageous in reducing the amount of submucosal injection, the intraoperative bleeding rate, and the muscle injury rate . The application of this technique in esophageal ESD treatment may yield similar improvement effects, which needs comparative analysis in future research. CEA is intimately associated with EC occurrence, and both CEA and CA724 exert a strong connection with bone metastases in EC. Further, TSGF is significantly correlated with pathological progression, such as the tumor location, lymph node involvement, and TNM staging of EC, as well as prognosis[19-21]. Hence, this study analyzed the effect of ESD on the indices in patients with EPL or EEC. Our data revealed an evident decline in CEA, CA724, and TSGF levels in the research group postoperatively, which were lower compared with the baseline and those of the control group. This indicates that ESD significantly downregulates the abnormally increased serum STM levels in patients with EPL or EEC.
Considering the occult symptoms of EEC, patients are more likely to be diagnosed in the middle and late stages, causing not only a high risk of posttreatment recurrence but also a relatively low 5-year survival rate[22]. Therefore, this study also analyzed the effect of ESD on the recurrence rate of patients. A 6-month follow-up indicated a comparable recurrence rate in the research group (3.33%) compared to the control group, indicating that ESD will not increase the recurrence risk in patients with EPL or EEC. Wu et al[23] applied ESD to patients with EPL or EEC and achieved a surgical success rate of 96.6%. This indicates a certain safety and reliability level of the ESD procedure, along with low recurrence and complication rates. Ling et al[24], which enrolled 89 cases of EPL and EEC treated with ESD, reported one recurrence case. Additionally, Xu et al[25] demonstrated that ESD has a low incidence of residual lesions and recurrence in elderly patients with early gastric cancer and precancerous lesions and is beneficial for promoting gastric cell and glandular function recovery, which supports our research results. Besides the above-mentioned treatment modalities, several investigators have conducted relevant studies on the treatment approaches for EPL and EEC. For instance, Zheng et al[26] have demonstrated that both multi-band mucosectomy (MBM) and ESD can be effectively utilized in treating patients with EPL or EEC. MBM presents the advantages of shorter hospitalization duration, faster recovery, and lower cost, whereas ESD offers benefits such as a high complete resection rate of the lesions, the ability to avoid positive resection margins, and the reduction of the risks associated with secondary treatments and additional surgeries. Furthermore, Xie et al[27] demonstrated that clip traction helps in esophageal ESD treatment by increasing the operative field exposure, which is conducive to reducing the risk of injury to the muscularis propria and shortening the dissection time. Further, evidence revealed that cryotherapy can be used to treat patients with EPL, which induces refrigerants (liquid nitrogen or carbon dioxide) to destroy tumor tissues through rapid cooling and thawing cycles, thereby playing a therapeutic role[28].
This study has several limitations to be improved. First, long-term follow-up could be incorporated to analyze the extended effect of ESD treatment on patients’ quality of life, which would provide deeper information into the potential clinical value of ESD. Second, expanding the analysis to include factors that affect treatment efficacy, complications, and prognosis in patients with EPL or EEC post-ESD would help determine crucial determinants, thereby facilitating the development of more targeted clinical optimization strategies. Third, coordinating multicenter efforts to obtain large-sample data for prospective studies would further improve the accuracy and generalizability of the research findings. Future research will focus on these directions to maximize the study's clinical applicability and practical significance.
In conclusion, ESD application in patients with EPL or EEC significantly improved the dissection area and the resection rate per unit time while reducing the risk of complications, including delayed bleeding, wound infection, esophageal reflux, and postoperative esophageal stenosis. Moreover, it reduced intraoperative bleeding, shortened operation duration and hospital stays, facilitated recovery, and suppressed the abnormal levels of serum CEA, CA724, and TSGF.
| 1. | Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, Bray F. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J Clin. 2021;71:209-249. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 75126] [Cited by in RCA: 64683] [Article Influence: 16170.8] [Reference Citation Analysis (177)] |
| 2. | Yang CS, Chen X, Tu S. Etiology and Prevention of Esophageal Cancer. Gastrointest Tumors. 2016;3:3-16. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 66] [Article Influence: 7.3] [Reference Citation Analysis (0)] |
| 3. | An L, Zheng R, Zeng H, Zhang S, Chen R, Wang S, Sun K, Li L, Wei W, He J. The survival of esophageal cancer by subtype in China with comparison to the United States. Int J Cancer. 2023;152:151-161. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 30] [Reference Citation Analysis (0)] |
| 4. | Abnet CC, Arnold M, Wei WQ. Epidemiology of Esophageal Squamous Cell Carcinoma. Gastroenterology. 2018;154:360-373. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 935] [Cited by in RCA: 1155] [Article Influence: 165.0] [Reference Citation Analysis (1)] |
| 5. | Liu J, Dai L, Wang Q, Li C, Liu Z, Gong T, Xu H, Jia Z, Sun W, Wang X, Lu M, Shang T, Zhao N, Cai J, Li Z, Chen H, Su J, Liu Z. Multimodal analysis of cfDNA methylomes for early detecting esophageal squamous cell carcinoma and precancerous lesions. Nat Commun. 2024;15:3700. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 10] [Reference Citation Analysis (0)] |
| 6. | Ciocirlan M, Lapalus MG, Hervieu V, Souquet JC, Napoléon B, Scoazec JY, Lefort C, Saurin JC, Ponchon T. Endoscopic mucosal resection for squamous premalignant and early malignant lesions of the esophagus. Endoscopy. 2007;39:24-29. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 92] [Cited by in RCA: 84] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 7. | Dan X, Lv XH, San ZJ, Geng S, Wang YQ, Li SH, Xie HH. Efficacy and Safety of Multiband Mucosectomy Versus Cap-assisted Endoscopic Resection For Early Esophageal Cancer and Precancerous Lesions: A Systematic Review and Meta-Analysis. Surg Laparosc Endosc Percutan Tech. 2019;29:313-320. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 4] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 8. | Gan T, Wu JC, Yang JL. [Diagnosis and Minimally Invasive Endoscopic Treatment of Early Esophageal Cancer and Precancerous Lesions]. Sichuan Da Xue Xue Bao Yi Xue Ban. 2018;49:833-839. [PubMed] |
| 9. | Park CH, Kim EH, Kim HY, Roh YH, Lee YC. Clinical outcomes of endoscopic submucosal dissection for early stage esophagogastric junction cancer: a systematic review and meta-analysis. Dig Liver Dis. 2015;47:37-44. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 35] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 10. | Early Diagnosis and Treatment Group of the Chinese Medical Association Oncology Branch. [Chinese expert consensus on early diagnosis and treatment of esophageal cancer]. Zhonghua Zhong Liu Za Zhi. 2022;44:1066-1075. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 4] [Reference Citation Analysis (0)] |
| 11. | Fukami N. Endoscopic Submucosal Dissection in the Esophagus: Indications, Techniques, and Outcomes. Gastrointest Endosc Clin N Am. 2023;33:55-66. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 12. | Ning B, Abdelfatah MM, Othman MO. Endoscopic submucosal dissection and endoscopic mucosal resection for early stage esophageal cancer. Ann Cardiothorac Surg. 2017;6:88-98. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 59] [Cited by in RCA: 58] [Article Influence: 7.3] [Reference Citation Analysis (0)] |
| 13. | Martínek J, Juhas S, Dolezel R, Walterová B, Juhasova J, Klima J, Rabekova Z, Vacková Z. Prevention of esophageal strictures after circumferential endoscopic submucosal dissection. Minerva Chir. 2018;73:394-409. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 10] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 14. | Draganov PV, Wang AY, Othman MO, Fukami N. AGA Institute Clinical Practice Update: Endoscopic Submucosal Dissection in the United States. Clin Gastroenterol Hepatol. 2019;17:16-25.e1. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 214] [Cited by in RCA: 321] [Article Influence: 53.5] [Reference Citation Analysis (0)] |
| 15. | Yu X, Liu Y, Xue L, He S, Zhang Y, Dou L, Liu X, Lu N, Wang G. Risk factors for complications after endoscopic treatment in Chinese patients with early esophageal cancer and precancerous lesions. Surg Endosc. 2021;35:2144-2153. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 11] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 16. | Jun Oh D, Jung Na H, Hyung Nam J, Jeong Lim Y, Hak Kim J. Could immediate second-look endoscopy reduce post-endoscopic submucosal dissection bleeding? Arab J Gastroenterol. 2023;24:245-250. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 17. | Matsuura N, Kato M, Iwata K, Miyazaki K, Masunaga T, Kubosawa Y, Mizutani M, Hayashi Y, Takabayashi K, Takatori Y, Nakayama A, Okabayashi K, Kawakubo H, Kitagawa Y, Yahagi N. Endoscopic ultrasound classification for prediction of endoscopic submucosal dissection resectability: PREDICT classification. Endosc Int Open. 2024;12:E1075-E1084. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Reference Citation Analysis (0)] |
| 18. | Li J, Wei Y, Zhang D, Hou X, Shen M, Chen K, Wu R, Peng K, Liu F. Comparison Between Preincision Traction and On-Demand Traction in Assisting Colorectal Endoscopic Submucosal Dissection. Clin Transl Gastroenterol. 2022;13:e00539. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 19. | Zhang H, Li H, Ma Q, Yang FY, Diao TY. Predicting malignant transformation of esophageal squamous cell lesions by combined biomarkers in an endoscopic screening program. World J Gastroenterol. 2016;22:8770-8778. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 6] [Cited by in RCA: 10] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 20. | Wang X, Gao Y, Wang J, Chen L, Zhang X, Chen M, Lan N, Li W, Wu F, Ren J. Predictive Role of Elevated Neutrophil-Lymphocyte Ratio for Bone Metastasis in Esophageal Cancer. Technol Cancer Res Treat. 2024;23:15330338241272043. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Reference Citation Analysis (0)] |
| 21. | Xu X, Wang W, Tian B, Zhang X, Ji Y, Jing J. The predicting role of serum tumor-specific growth factor for prognosis of esophageal squamous cell carcinoma. BMC Cancer. 2023;23:1067. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 22. | Wang M, Smith JS, Wei WQ. Tissue protein biomarker candidates to predict progression of esophageal squamous cell carcinoma and precancerous lesions. Ann N Y Acad Sci. 2018;1434:59-69. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 28] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 23. | Wu Y, Zhang H, Zhou B, Han S, Zhang Y. Clinical efficacy of endoscopic submucosal dissection in the treatment of early esophageal cancer and precancerous lesions. J Cancer Res Ther. 2018;14:52-56. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 7] [Cited by in RCA: 9] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 24. | Ling A, Zhu F, Wu P, Fang C, Cao F. [Synthetic evaluation of precancerous lesions and early esophageal cancers after endoscopic submucosal dissection]. Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2016;41:71-77. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 25. | Xu WS, Zhang HY, Jin S, Zhang Q, Liu HD, Wang MT, Zhang B. Efficacy and safety of endoscopic submucosal dissection for early gastric cancer and precancerous lesions in elderly patients. World J Gastrointest Surg. 2024;16:511-517. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 26. | Zheng J, Yang J, Zhao Z. Comparison of MBM and ESD in the Treatment of Single Early Esophageal Cancer and Precancerous Lesions. Ann Ital Chir. 2024;95:534-541. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 27. | Xie X, Bai JY, Fan CQ, Yang X, Zhao XY, Dong H, Yang SM, Yu J. Application of clip traction in endoscopic submucosal dissection to the treatment of early esophageal carcinoma and precancerous lesions. Surg Endosc. 2017;31:462-468. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 25] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 28. | Lal P, Thota PN. Cryotherapy in the management of premalignant and malignant conditions of the esophagus. World J Gastroenterol. 2018;24:4862-4869. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 16] [Cited by in RCA: 11] [Article Influence: 1.6] [Reference Citation Analysis (1)] |