Published online Apr 27, 2025. doi: 10.4240/wjgs.v17.i4.103136
Revised: January 17, 2025
Accepted: February 10, 2025
Published online: April 27, 2025
Processing time: 139 Days and 20.7 Hours
Gastrointestinal duplication is a rare congenital anomaly of the digestive tract, with colonic manifestations being particularly uncommon. Malignant trans
A 49-year-old woman was found to have an elevated cancer antigen 19-9 level during a routine checkup. Imaging revealed a well-defined abdominal cavity cystic mass, which was initially suspected to be an ovarian teratoma. Laparoscopic surgery revealed a duplication cyst, and pathological examination con
Colonic duplications, though rare, remain a differential diagnosis of unexplained abdominal masses, with complete resection being their primary treatment approach.
Core Tip: In cases of gastrointestinal duplication involving cystic masses, maintaining a high suspicion for potential malignancy is crucial, even in asymptomatic patients. Due to the rarity of these conditions, a multidisciplinary approach is essential for accurate diagnosis and treatment. Comprehensive imaging studies, like contrast computed tomography, should evaluate the cyst’s characteristics and its relation to adjacent structures. Surgical intervention, preferably through en bloc resection, is recommended to ensure complete removal of any neoplastic tissue. Regular follow-up and monitoring of tumor markers are vital for early detection of recurrence or progression.
- Citation: Lee J, Suh JW. Adenocarcinoma originating from a colonic duplication cyst: A case report. World J Gastrointest Surg 2025; 17(4): 103136
- URL: https://www.wjgnet.com/1948-9366/full/v17/i4/103136.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v17.i4.103136
Gastrointestinal duplication is an uncommon congenital anomaly, with gastrointestinal cystic or tubular abnormalities observed in any part of the gastrointestinal tract. The prevalence of congenital disease ranges from 1 in 4500 to 1 in 10000, with 80% of the cases diagnosed either before birth or within the first two years of life[1-4]. However, this condition may remain undetected until later in life.
The occurrence of gastrointestinal duplication has been reported in the ileum, ileocecal valve, and jejunum at rates of 30%, 30%, and 8%, respectively. However, its occurrence is rare in the colon and rectum, with incidences of 6%-7% and 5%, respectively[4-6]. If no related abnormalities are present, symptoms may not be observed until complications occur[5,7]. Clinical symptom development depends on factors such as location, size, abnormal mucosa presence within the duplication site, adjacent bowel connection, and inflammation.
The main symptoms are abdominal pain and intestinal obstruction, while the other symptoms include the presence of an abdominal mass, chronic pain, constipation, and, less frequently, acute abdominal symptoms, including intestinal volvulus[8], intussusception, perforation, or active bleeding[9].
Herein, we present a case of adenocarcinoma arising from an asymptomatic duplication cyst in the colon of a 49-year-old female patient.
Detection of abnormal cancer markers.
A 49-year-old woman with no previous medical history presented to the gynecology outpatient clinic of a tertiary hospital with abnormal cancer markers detected during an examination at a local clinic.
There was no specific medical history such as diabetes, hypertension, or surgery.
There was no specific personal and family history.
There were no abnormal findings in the physical examination upon admission.
Elevated levels of cancer antigen (CA)-19-9: 61.6 U/mL, normal range: < 37 U/mL; CA-125: 47.3 U/mL, normal range: < 55 U/mL and normal levels of carcinoembryonic antigen: 1.1 U/mL, normal range: < 5 U/mL.
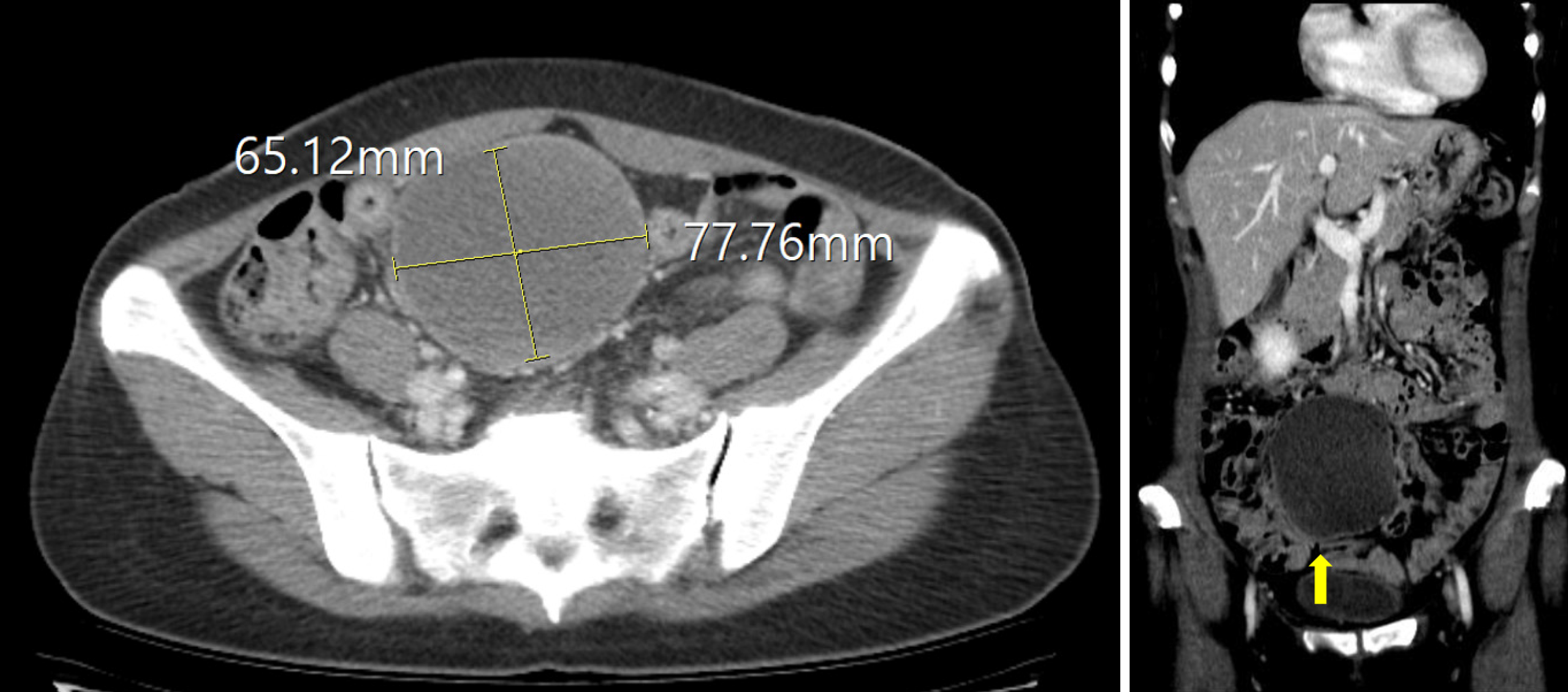
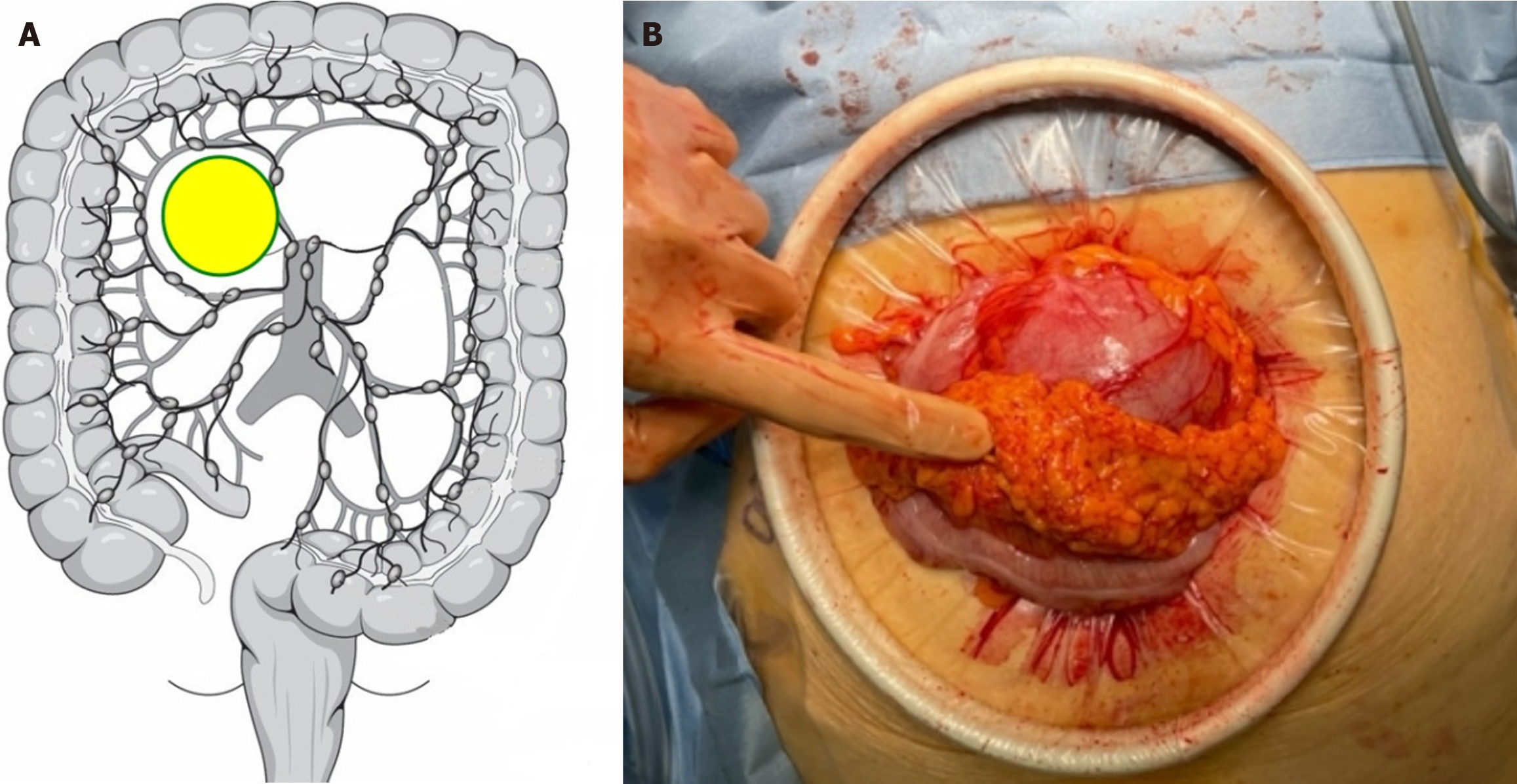
Abdominal-pelvic computed tomography (CT) revealed a well-defined 6.5 cm × 7.8 cm × 8.5 cm cystic mass with internal fatty attenuation and fluid-fluid level in the right adnexa without enhancement (Figure 1). The gynecology department at our hospital uses diagnostic laparoscopy to differentiate extragonadal teratomas, ovarian teratomas, and myxoid liposarcomas. During laparoscopy, the cyst had no communication with the ovaries; however, it was in the transverse mesocolon (Figure 2A).
As this case was rare, we discussed the treatment plan for the patient at a multidisciplinary treatment, consisting of a colorectal surgeon, oncologist, pathologist, radiologist, and gastroenterologist, conference and concluded that no further chemotherapy was needed due to the complete surgical resection. Regular checkups were recommended.
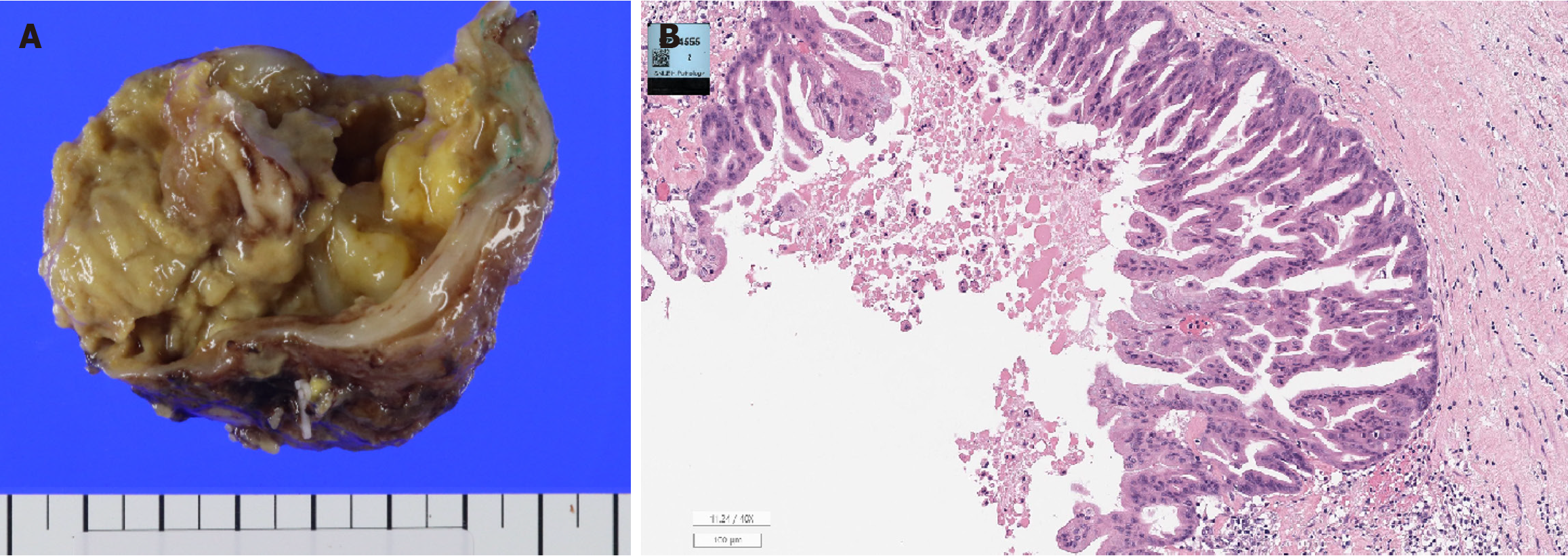
The cyst was diagnosed as adenocarcinoma originating from a colonic duplication cyst with muscularis propria invasion (Figure 3).
As the tumor was hard and did not adhere to the floor and was capable of movement, a mini-laparotomy procedure was performed (Figure 2B). The cyst was then separated from the colon, mobilized, and excised by a colorectal surgeon. The well-defined cystic mass did not communicate with the colon, and no damage to the colon was observed after the resection. The patient was discharged without any postoperative complications.
Immunohistochemical analysis revealed that the tumor cells were positive for cytokeratin (CK) 7, CK 20, and caudal-type homeobox transcription factor 2 (Table 1).
| Variables | Results |
| Preoperative treatment | Not done |
| Gross type | Other (cystic) |
| Tumor location | Transverse colon, mesentery |
| Histologic variant (World Health Organization 5th ed.) | Not otherwise specified |
| Histology grade | Moderately differentiated |
| Tumor size | 9.2 cm × 8.0 cm × 7.8 cm |
| Invasion margins | Muscularis propria |
| Resection margins | Safety margin: Radial 02 cm |
| Lymph node | Not submitted |
| Lymphatic invasion | Not identified |
| Venous invasion | Not identified |
| Perineural invasion | Not identified |
| Tumor deposits | Not identified |
| Tumor budding | Negative (× 1/200) |
| Tumor border | Infiltrative |
| Stromal reaction | Absent |
| Preexisting adenoma | Not identified |
| Associated findings | None |
| Caudal-type homeobox transcription factor 2 | Positive |
| Cytokeratin 20 | Positive |
| Cytokeratin | Positive |
| Estrogen receptor | Negative |
| Paired box gene 8 | Negative |
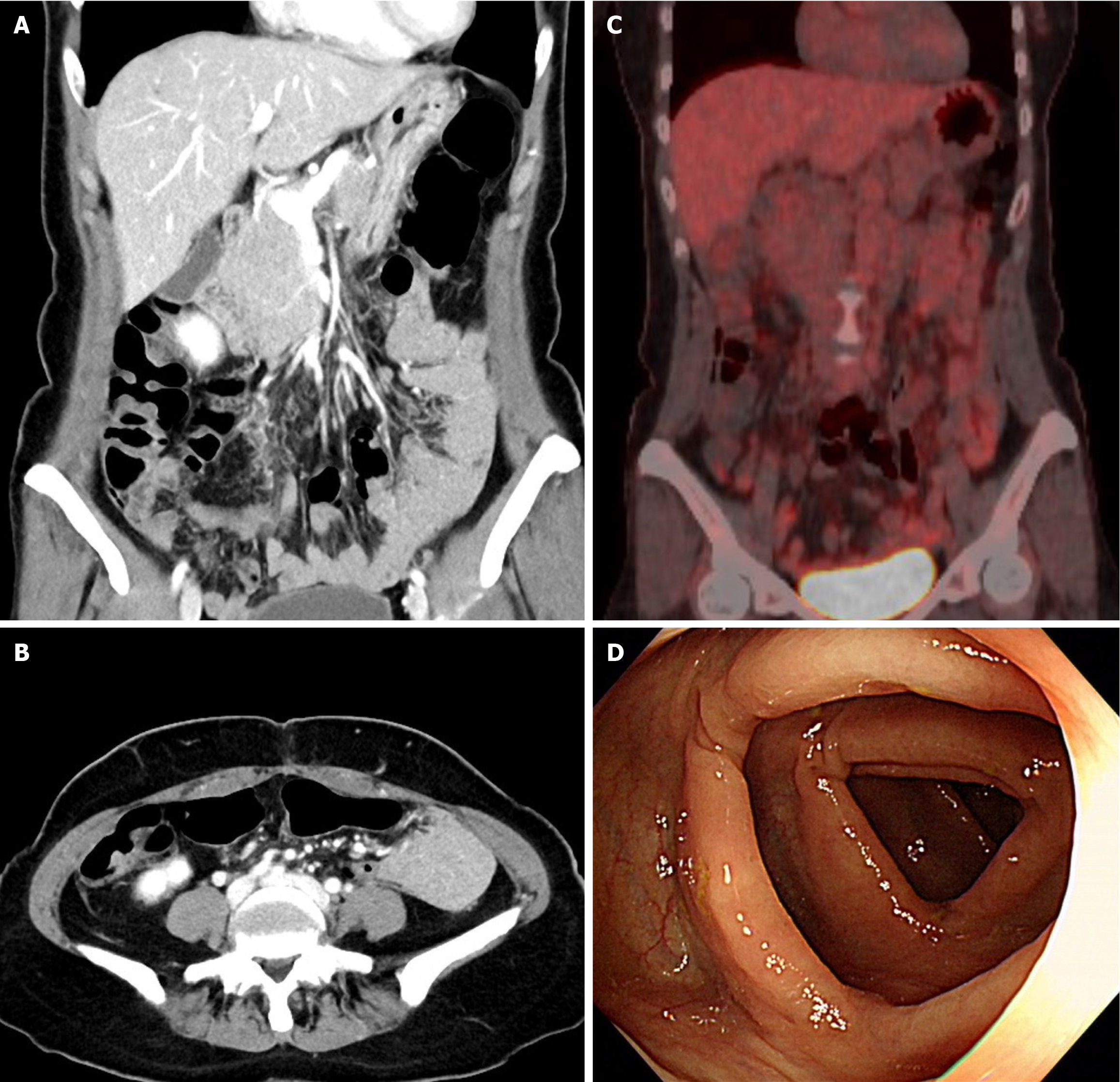
Postoperatively, endoscopy revealed no abnormal lesions. Moreover, whole-body positron emission tomography revealed no abnormal hypermetabolic lesions suggesting malignancy (Figure 4). CA 19-9 levels measured 1 month post-surgery were 9.3 U/mL, which was within the normal range (< 37 U/mL); no other specific findings were observed. No evidence of recurrence has been observed two years post-surgery.
Gastrointestinal duplications are uncommon congenital abnormalities diagnosed during the prenatal period or within the first two years of life in approximately 80% of cases[2,3]. Colonic duplications account for only 13% of all duplications and arise in the cecum[3,10]. Although malignant transformation in a duplication is rare, cases of adenocarcinoma, squamous cell carcinoma, carcinoid tumors, gastrointestinal stromal tumors, and leiomyosarcoma have been reported. In these rare cases, adenocarcinoma is the predominant histological malignancy type[11-14]. The duplication diagnosis is based on well-established morphological criteria, including: (1) Direct attachment to the alimentary tract; (2) Presence of a smooth muscle layer; and (3) A lining epithelium similar to that of the alimentary tract[11]. Our case met criteria 2 and 3, leading to a diagnosis of adenocarcinoma arising from a colonic duplication cyst.
The diagnosis of colonic duplications may be challenging. In children before the age of 2 years, it is often diagnosed by intrauterine ultrasonography; however, in adults, it is often revealed during surgery[3,15-17]. Contrast CT is the most effective method for establishing a diagnosis and determining the cyst composition and its interaction with adjacent structures[18]. The cysts usually have attenuation levels comparable to that of water with a discernible calcification rim in some cases[11]. The differential diagnoses include colonic duplication cyst, primary colonic malignancy, atypical gastrointestinal stromal tumor, intestinal lymphoma, myxoid liposarcoma, or loculated perforation. In women, ovarian teratoma and extragonadal teratoma should also be considered. However, a definitive diagnosis is often challenging to establish preoperatively, and surgical resection is frequently required to confirm the final pathological diagnosis[19]. In this case, a well-defined cystic mass with internal fatty attenuation and fluid-fluid level was observed; however, ovarian teratoma was more likely than colon duplication. Furthermore, nuclear medicine scans can reveal duplications in the stomach mucosa, whereas contrast enema or colonoscopy may be useful in cases in which there is a link to the colonic lumen.
Previous studies have reported colonic duplication causing intussusception, rectal hemorrhage, and pancreatitis, with abdominal pain and a palpable mass being the most common symptoms in adenocarcinoma cases[11]. In this case, the condition was detected during a regular checkup without specific symptoms.
Colonic duplication is primarily managed through en bloc resection of the adjacent large intestine[2,10]. In selected cases without damage to the bowel wall or vascular supply, enucleation of duplication cysts may be performed alternatively[2]. Furthermore, advances in laparoscopic procedures and instrumentation have enabled laparoscopic resection[10]. In this case, a gynecologist attempted to approach the tumor laparoscopically and confirmed that it was distant from the uterus and ovaries and adjacent to the transverse colon. A colorectal surgeon then completed the duplication cyst resection, separating the colon and duplication cyst via mini-laparotomy, without damaging the colonic wall or blood vessels. Lymph node dissection was not performed because no malignancy was suspected.
The potential for colonic duplication cysts and malignancy warrants consideration of the extent of resection via a multidisciplinary approach; however, this team was not assembled before surgery. Following the postoperative adenocarcinoma confirmation, a multidisciplinary group was organized to assess the pathological findings and postoperative evaluations. Although lymph node dissection was not performed, further assessment revealed no increase in lymph node uptake or enlargement, and no high-risk characteristics were revealed by pathology. Therefore, complete surgical resection was considered appropriate, adjuvant chemotherapy was not administered, and routine surveillance was performed.
Colonic duplication is an uncommon congenital anomaly, and malignant transformation is extremely rare. When assessing a cystic mass adjacent to or enclosed by the gastrointestinal tract, duplication should be considered in the differential diagnosis. The potential for malignancy arising from a duplication cyst should be considered, and thorough en bloc resection of the tumor is imperative.
| 1. | Schalamon J, Schleef J, Höllwarth ME. Experience with gastro-intestinal duplications in childhood. Langenbecks Arch Surg. 2000;385:402-405. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 64] [Cited by in RCA: 57] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 2. | Ricciardolo AA, Iaquinta T, Tarantini A, Sforza N, Mosca D, Serra F, Cabry F, Gelmini R. A rare case of acute abdomen in the adult: The intestinal duplication cyst. case report and review of the literature. Ann Med Surg (Lond). 2019;40:18-21. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 12] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 3. | Rodríguez García P, Sánchez Pérez A, Romera Barba E, Calero García P, González-Costea Martínez R. Colonic duplication cyst in adult. Gastroenterol Hepatol. 2020;43:360-361. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 4. | Kekez T, Augustin G, Hrstic I, Smud D, Majerovic M, Jelincic Z, Kinda E. Colonic duplication in an adult who presented with chronic constipation attributed to hypothyroidism. World J Gastroenterol. 2008;14:644-646. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 25] [Cited by in RCA: 20] [Article Influence: 1.2] [Reference Citation Analysis (1)] |
| 5. | Banchini F, Delfanti R, Begnini E, Tripodi MC, Capelli P. Duplication of the transverse colon in an adult: case report and review. World J Gastroenterol. 2013;19:586-589. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 20] [Cited by in RCA: 17] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 6. | Puligandla PS, Nguyen LT, St-Vil D, Flageole H, Bensoussan AL, Nguyen VH, Laberge JM. Gastrointestinal duplications. J Pediatr Surg. 2003;38:740-744. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 158] [Cited by in RCA: 150] [Article Influence: 6.8] [Reference Citation Analysis (0)] |
| 7. | Correia-Pinto J, Romero R, Carvalho JL, Silva G, Guimarães H, Estevão-Costa J. Neonatal perforation of a Y-shaped sigmoid duplication. J Pediatr Surg. 2001;36:1422-1424. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 17] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 8. | Salvador II, Modelli ME, Pereira CR. [Tubular duplication of the colon: a case report and review of the literature]. J Pediatr (Rio J). 1996;72:254-257. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 6] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 9. | Fotiadis C, Genetzakis M, Papandreou I, Misiakos EP, Agapitos E, Zografos GC. Colonic duplication in adults: report of two cases presenting with rectal bleeding. World J Gastroenterol. 2005;11:5072-5074. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 37] [Cited by in RCA: 45] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 10. | Nolan HR, Wengler C, Hartin CW, Glenn JB. Laparoscopic excision of an ascending colon duplication cyst in an adolescent. J Pediatr Surg Case Rep. 2016;4:32-34. [RCA] [DOI] [Full Text] [Cited by in Crossref: 2] [Reference Citation Analysis (0)] |
| 11. | Kang M, An J, Chung DH, Cho HY. Adenocarcinoma arising in a colonic duplication cyst: a case report and review of the literature. Korean J Pathol. 2014;48:62-65. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 6] [Cited by in RCA: 8] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 12. | Heiberg ML, Marshall KG, Himal HS. Carcinoma arising in a duplicated colon. Case report and review of literature. Br J Surg. 1973;60:981-982. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 25] [Cited by in RCA: 26] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 13. | Jung KH, Jang SM, Joo YW, Oh YH, Park YW, Paik HG, Choi JH. Adenocarcinoma arising in a duplication of the cecum. Korean J Intern Med. 2012;27:103-106. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 8] [Cited by in RCA: 10] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 14. | Lee J, Jeon YH, Lee S. Papillary adenocarcinoma arising in a duplication of the cecum. Abdom Imaging. 2008;33:601-603. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 16] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 15. | Shanmugalingam A, Duxbury H, Choi JDW, Kwik C, P'Ng CH, Kim L, Pathma-Nathan N. An unusual case of colonic duplication cyst in an adult with dysplasia. J Surg Case Rep. 2023;2023:rjad039. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 16. | Radhakrishnan L, George J, Abraham LK. Right-Sided Colonic Duplication Cyst with a Malignant Twist in a Young Adult - a Case Report. J Gastrointest Cancer. 2022;53:805-808. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 17. | Hsu H, Gueng MK, Tseng YH, Wu CC, Liu PH, Chen CC. Adenocarcinoma arising from colonic duplication cyst with metastasis to omentum: A case report. J Clin Ultrasound. 2011;39:41-43. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 14] [Cited by in RCA: 14] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 18. | Carachi R, Azmy A. Foregut duplications. Pediatr Surg Int. 2002;18:371-374. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 55] [Cited by in RCA: 41] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 19. | Yan J, Yan J, Ding C, Guo J, Peng Y, Chen Y. Clinical features of colorectal duplication in children: A study of 25 cases. J Pediatr Surg. 2022;57:97-101. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 5] [Article Influence: 1.7] [Reference Citation Analysis (0)] |