Published online Apr 27, 2025. doi: 10.4240/wjgs.v17.i4.102681
Revised: January 17, 2025
Accepted: February 26, 2025
Published online: April 27, 2025
Processing time: 113 Days and 21.7 Hours
Appendicitis is a common acute abdominal pain disorder. Laparoscopic appen
To explore the effects of rapid rehabilitation and surgical nursing care on gas
A total of 120 patients who underwent laparoscopic appendectomy at our hospital between January 2019 and March 2024 and for whom complete clinical data were available were selected. Patients were randomly assigned to two groups (n = 60 each) using the random number table method. The control group received routine nursing care, while the experimental group received rapid rehabilitation surgical nursing care; all patients continued to receive nursing care until discharge. The recovery of gastrointestinal function, length of hospital stay, complications, Pittsburgh sleep quality index, and nursing satisfaction were compared between groups.
Following the implementation of effective nursing measures, the times to bowel sound recovery, first exhaust, first defecation, and first feeding were notably shorter in the study vs control group (P < 0.05). Additionally, the duration of the first postoperative activity and the length of hospital stay were significantly shorter in the study vs control group (P < 0.05). Furthermore, the study group exhibited better sleep quality than the control group (P < 0.05). The postoperative complication rate was significantly lower and the nursing satisfaction rate significantly higher in the study vs control group (P < 0.05).
Rapid rehabilitation surgical nursing interventions provided to patients after laparoscopic appendectomy can accelerate their postoperative recovery, reduce the occurrence of complications, and improve their sleep quality and nursing satisfaction.
Core Tip: To explore the effects of rapid rehabilitation surgical nursing on gastrointestinal function recovery and sleep quality in patients undergoing laparoscopic appendectomy. Rapid rehabilitation surgical nursing interventions provided to patients after laparoscopic appendectomy can accelerate their postoperative recovery, reduce the occurrence of complications, and improve their sleep quality and nursing satisfaction.
- Citation: Chen SS, Gao YM, Yao XF, Zhang QQ, Yang KL, Xia Q, Ding J. Effect of rapid rehabilitation surgical nursing on patients' gastrointestinal function recovery and sleep quality after laparoscopic appendectomy. World J Gastrointest Surg 2025; 17(4): 102681
- URL: https://www.wjgnet.com/1948-9366/full/v17/i4/102681.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v17.i4.102681
Appendicitis, a common surgical emergency, involves inflammation of the appendix that can be classified into early, acute, gangrenous, and chronic stages based on its progression[1]. It mainly manifests as abdominal pain in individuals aged 5-45 years, carries a risk of occurrence of 8.6% in men vs 6.7% in women[2], and is usually treated by surgical excision[3]. Laparoscopic appendectomy is currently the conventional approach[4]; it is typically performed after hours, features less trauma, and leads to faster recovery than traditional open appendectomy[5]. This minimally invasive technique reduces incision time and minimizes postoperative pain and complications, leading to a quicker return to normal activities[6]. However, postoperative recovery remains an important issue affecting rehabilitation quality and surgical results[7].
Conventional postoperative nursing methods usually involve bed rest and lack systematic rehabilitation intervention measures, resulting in a slow recovery period and high incidence of complications[8]. Rapid rehabilitation surgical nursing is a comprehensive nursing measure that follows evidence-based medicine standards and optimizes routine nursing interventions[9] and includes early activity, pain management, nutritional support, psychological support, and other measures aiming to promote postoperative rehabilitation, reduce the incidence of complications, and improve patient quality of life[10,11]. Rapid rehabilitation is widely administered in various clinical settings. Anal preservation surgery for rectal cancer accelerates the recovery process and reduces length of hospital stay and medical costs[11].
Rapid rehabilitation surgery is increasingly used in clinical nursing to alleviate stress, reduce postoperative pain and complications, and enhance patient quality of life while accelerating the rehabilitation process. According to previous clinical studies, patients undergoing laparoscopic appendectomy with an enhanced recovery surgery protocol have significantly shorter exhaust times, lengths of hospital stay, hospitalization costs, and pain scores than those receiving conventional therapy[5,12]. Implementing rapid rehabilitation in surgical nursing care can effectively reduce patients' postoperative stress and complications, allowing for their quicker recovery[13,14]. This finding suggests that enhanced surgical recovery regimens can significantly accelerate the recovery process, shorten the length of hospital stay, and reduce the hospitalization costs of patients with appendicitis. In addition, evidence-based nursing interventions for patients with heart failure and tumors demonstrated significant clinical effects that improved patient postoperative status and quality of life[15]. Comprehensive nursing interventions are important in post–lumbar surgery rehabilitation because they can effectively relieve pain, reduce inflammation, and improve overall recovery quality[8]. Therefore, it is important that we explore the effects of rapid rehabilitation surgical nursing on gastrointestinal function recovery and sleep quality in patients undergoing laparoscopic appendectomy.
This study aimed to explore the effects of a rapid rehabilitation surgical nursing intervention on gastrointestinal function recovery and sleep quality in patients undergoing laparoscopic appendectomy; evaluate its ability to promote postoperative rehabilitation, improve sleep quality, and reduce complication rates; and provide a basis for improving the surgical treatment effect and optimizing clinical nursing to promote the development of surgical nursing.
We retrospectively selected 120 patients who underwent laparoscopic appendectomy at our hospital between January 2019 and March 2024. The participants were randomly assigned using a random number table to the control group, consisting of 60 patients who received standard nursing care, and the study group, consisting of 60 patients who received rapid rehabilitation surgical nursing care.
The inclusion criteria were as follows[16]: (1) Diagnosis of appendicitis based on clinical manifestations, ultrasonography, and laboratory examination results (excluding cases of appendiceal perforation and periappendiceal abscess); (2) No contraindications for general anesthesia or laparoscopic surgery; (3) No history of mental illness but normal cognitive function; and (4) Availability of complete clinical data.
The exclusion criteria were as follows: (1) Currently pregnant or lactating; (2) Serious mental illness or psychological disorder; and (3) Severe hypertensive heart disease.
This study was approved by our institution's research ethics committee and performed in accordance with the Decla
Control group: Patients in the control group received routine nursing care as follows: (1) Monitoring of vital signs (body temperature, pulse, respiration, and blood pressure); (2) timely administration of analgesics to ensure pain control; (3) Regular dressing changes to keep the wound clean and dry and avoid infection with monitoring for redness, swelling, seepage, or other abnormalities; (4) Monitoring of fluid volume and output to ensure water balance and prevent dehydration or water poisoning; (5) Gradual restoration of diet according to patient's postoperative recovery progress to avoid overeating-induced indigestion; (6) Gradual resumption of normal activities according to the doctor's advice including avoiding strenuous exercise, lifting heavy objects, and preventing wounds from splitting; and (7) Regular postoperative follow-ups including observations of wound healing, assessments of patient rehabilitation progress, and timely detection and treatment of complications.
Study group[17]: Patients in the study group received rapid rehabilitation surgical nursing interventions as follows: (1) Preoperatively, a comprehensive assessment of the patient's physical condition, chronic disease, drug use, etc. to ensure the creation of a more individualized care plan; (2) Formation of a team of surgeons, nurses, rehabilitation doctors, etc. to ensure seamless surgical and postoperative care; (3) Use of appropriate analgesic methods, such as local anesthesia or an analgesic pump, to reduce postoperative pain and promote movement and deep breathing; (4) Encouragement of early postoperative patient activity, including early awakening, walking, and simple rehabilitation activities, to help prevent complications such as deep vein thrombosis; (5) Provision of digestible nutrient-rich food to meet any special needs and monitoring of fluid intake to ensure adequate hydration; (6) Development of a personalized rehabilitation plan, including physical therapy and rehabilitation exercises, to help patients gradually regain their ability to move; (7) Implementation of appropriate infection control measures, including hand hygiene, wound care, and antibiotic use, to reduce the risk of infection; (8) Provision of psychological support to patients to meet their emotional and mental health needs; (9) Provision of regular postoperative follow-ups to monitor the patient's recovery process and identify and timely solve potential problems; and (10) Provision of relevant health education to ensure that patients and their families understand the postoperative precautions, dietary recommendations, and drug management protocols to promote patient participation in the rehabilitation process.
Postoperative recovery of gastrointestinal function included time to bowel sound recovery, first defecation, first exhaust, and first feeding as well as length of hospital stay.
Sleep quality[18]: The Pittsburgh sleep quality index (PSQI), which was used to evaluate patients' sleep quality, encompasses seven dimensions (total of 19 items): Sleep efficiency, quality, disturbances, duration, and latency; hypnotic medication use; and daytime dysfunction. A four-point scoring system was employed (maximum score, 21 points), with higher scores indicating poorer sleep quality. The scale demonstrated good reliability and validity as evidenced by a Cronbach's α coefficient of 0.710.
Postoperative complications: Postoperative complications included incisional infection, intestinal obstruction, adhesions, and abscesses.
Nursing satisfaction[19]: Satisfaction with the nursing care was assessed using a custom-made questionnaire developed at our hospital. A score of < 60 was considered "unsatisfactory,” indicating that patients believed that the clinical nursing care had no significant effect on their psychological status, comfort level, and pain degree; a score of 60-85 was considered "basically satisfied," indicating that the clinical nursing care somewhat improved their own psychological condition, comfort, and pain degree; and a score of > 85 was considered "very satisfied," indicating that the clinical nursing work significantly improved their psychological condition, comfort, and pain degree. Total satisfaction rate = [(basically satisfied + satisfied) cases/total cases] × 100.
Data analyses were performed using SPSS Statistics for Windows (version 26.0; IBM, Armonk, NY, United States). Continuous variables are presented as mean ± SD and were compared between groups using independent t-tests to identify significant differences. Categorical variables are shown as count and percentage, n (%) and were assessed using the χ2 test for intergroup comparisons. Statistical significance was set at P < 0.05.
The patients' baseline characteristics were comparable between groups (P > 0.05) (Table 1). The study group included 35 men and 25 women with a median age (25th-75th interquartile range) of 39 (33-37) years and a mean disease duration of 4.45 ± 0.64 hours. The control group included 33 men and 27 women with a median age (25th-75th interquartile range) of 38 (32-38) years and a mean disease duration of 4.51 ± 0.70 hours.
| Index | Study group (n = 60) | Control group (n = 60) | P value |
| Median age (25th-75th IQR) (years) | 39 (33-37) | 38 (32-38) | 0.532 |
| Sex | 0.723 | ||
| Male | 35 (58.3) | 33 (55.0) | |
| Female | 25 (41.7) | 27 (45.0) | |
| BMI (kg/m2) | 23.23 ± 3.05 | 23.26 ± 3.24 | 0.512 |
| Mean duration of disease (h) | 4.45 ± 0.64 | 4.51 ± 0.70 | 0.964 |
| Pathological types | 0.737 | ||
| Acute pure appendicitis | 36 (60.0) | 34 (56.7) | |
| Acute purulent appendicitis | 24 (40.0) | 26 (43.3) | |
| Smoking history (n) | 0.182 | ||
| Yes | 16 (26.7) | 18 (30.0) | |
| No | 44 (73.3) | 42 (70.0) | |
| Drinking history (n) | 0.173 | ||
| Yes | 20 (33.3) | 22 (36.7) | |
| No | 40 (66.7) | 38 (63.3) |
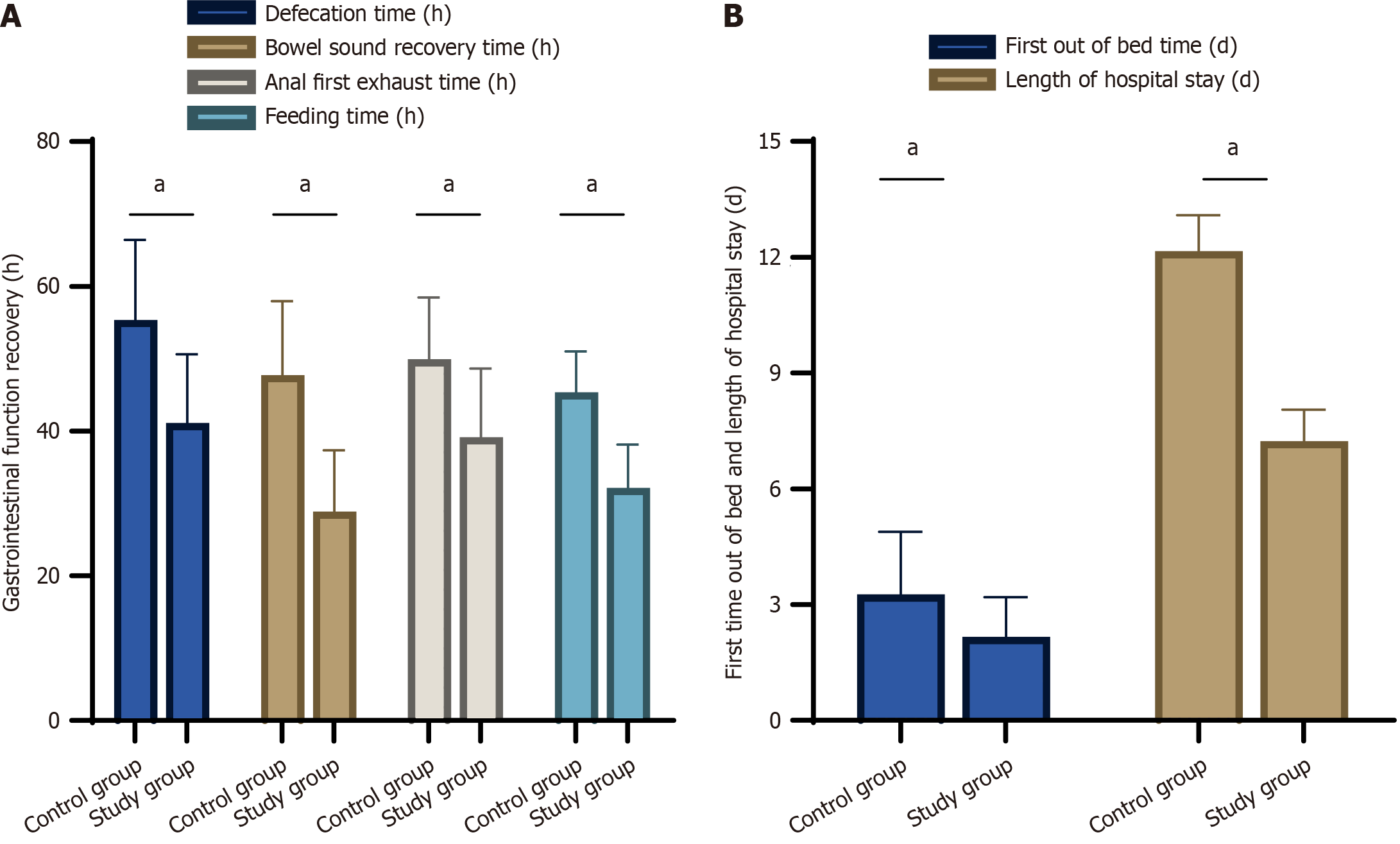
After effective nursing measures were provided, bowel sound recovery, first exhaust, first defecation, and first feeding times were significantly shorter in the intervention vs control group (P < 0.05). The first postoperative activity time and length of hospital stay were also significantly shorter in the intervention vs control group (P < 0.05) (Figure 1).
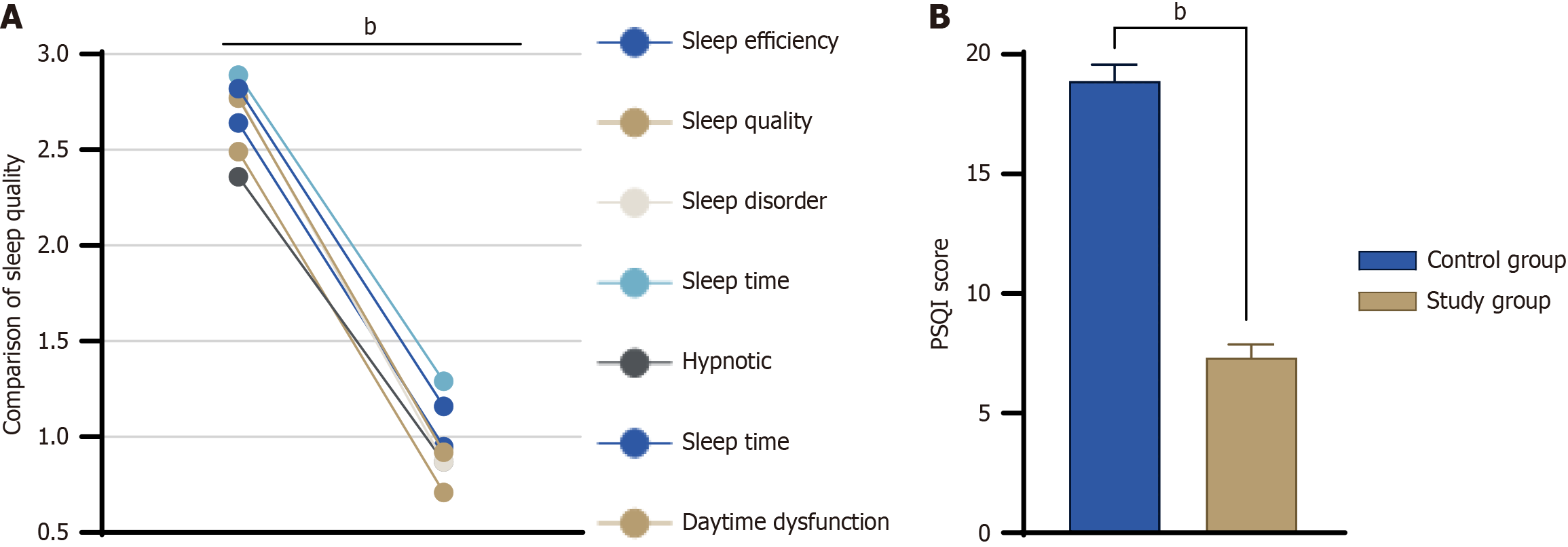
All PSQI and total scores were lower in the study vs control group (P < 0.01) (Figure 2), suggesting that patients in the control group had poorer sleep quality than those in the study group.
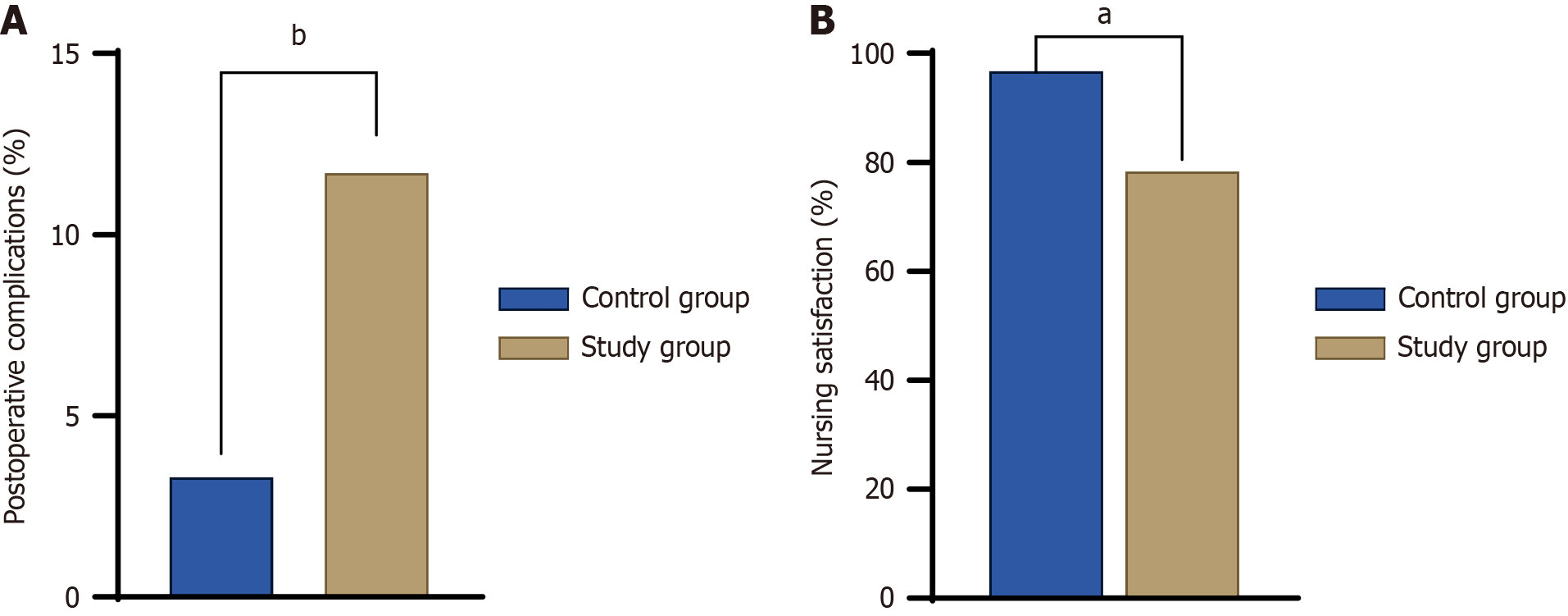
The incidence of postoperative complications was significantly lower in the study [3.3% (2/60)] vs control [11.7% (7/60)] group (P < 0.01) (Figure 3A).
The nursing satisfaction rate was significantly higher in the study [96.7% (58/60)] vs control group [78.3% (47/60)] (P < 0.05) (Figure 3B).
The rapid rehabilitation surgical care model uses an evidence-based medical approach to accelerate postoperative patient recovery and improve clinical outcomes. This model has been widely used with good results in laparoscopic surgery in various clinical departments[20]. Rapid rehabilitation surgical nursing protocols reportedly promote the recovery of gastrointestinal function, accelerate postoperative rehabilitation, and reduce complication rates[21]. Moreover, the use of rapid rehabilitation surgical nursing practices for patients undergoing laparoscopic myomectomy was proven effective at decreasing intraoperative bleeding, shortening the first postoperative exhaust time and length of hospital stay, and decreasing the bladder irritation rate[20]. These findings indicate that the rapid rehabilitation surgical nursing model enhances patient satisfaction and significantly reduces the incidence of postoperative complications. Therefore, it has important clinical application value for improving postoperative recovery and clinical outcomes[22].
These results showed that, after the nursing intervention, bowel sound recovery, first exhaust, first defecation, and first feeding times were significantly shorter in the study vs control group (P < 0.05). These findings suggest that rapid rehabilitation surgical nursing care can effectively promote functional intestinal reconstruction and shorten the recovery time by reducing postoperative intestinal dysfunction. Moreover, the duration of the first postoperative mobilization and length of hospitalization were significantly shorter in the study vs control group (P < 0.05), further supporting the important role of the rapid rehabilitation nursing strategy in reducing the length of hospitalization and accelerating the recovery process, a finding that is consistent with previous research results[23].
Improved sleep is another notable outcome of rapid rehabilitation among surgical nurses. The mean PSQI score was significantly lower in the study vs control group (P < 0.01), indicating that its use improved patients' physical and mental health recovery. The efficacy of this approach was validated in several previous studies. For example, patients who received rapid rehabilitation nursing care after radical gastrectomy showed significantly improved gastrointestinal function and fewer complications[21]. Moreover, rapid rehabilitation nursing care provided to patients undergoing laparoscopic myomectomy results in a lower incidence of postoperative complications and a higher rate of patient satisfaction[23]. These findings suggest that rapid rehabilitation care accelerates the physical recovery of patients and improves their overall quality of life and mental health.
The postoperative complication rate was significantly lower in the study (3.3%) vs control (11.7%) group (P < 0.01). These findings suggest that rapid rehabilitation nursing care can significantly reduce the incidence of postoperative complications. Rapid rehabilitation nursing care helps reduce patient anxiety and stress by using scientific nursing measures and personalized patient-centered programs, thereby reducing the occurrence of postoperative complications.
The mechanisms by which rapid rehabilitation surgical nursing enhance gastrointestinal function and sleep quality require further investigation. Physiologically, improved gastrointestinal function may be linked to earlier mobilization and dietary interventions that stimulate bowel activity. Psychologically, reducing anxiety through effective communi
This single-center retrospective study has certain limitations. First, its relatively small sample size (n = 120) may have affected the generalizability and reliability of the statistical results. Although the results were significant, validation in a larger sample size is necessary to ensure that these findings are applicable across hospitals and populations. Second, the study's single-center design may have led to selection bias, as variations in nursing practices, patient population characteristics, and the availability of medical resources in different hospitals may have affected the nursing outcomes. Therefore, future studies should adopt a multicenter design to increase sample diversity and representativeness, thereby improving the external validity of our findings. Third, its retrospective design influenced the results to some extent because missing or incorrectly recorded patient data may have affected the accuracy of the results. To overcome this problem, future studies should consider using prospective randomized controlled designs to enhance confidence in the results. Finally, although this study focused on postoperative improvements in gastrointestinal function and sleep quality, other potential influencing factors, such as the patient's psychological state, social support system, and follow-up care arrangements, require further exploration in future studies. Therefore, future studies will require larger sample sizes and multicenter design to further verify the efficacy of rapid rehabilitation surgical nursing care and provide a solid foundation for development in this field.
This study demonstrated that rapid rehabilitation surgical nursing care effectively supports patients after laparoscopic appendectomy by enhancing their gastrointestinal recovery, sleep quality, and nursing satisfaction while reducing complications. These findings are crucial to the advancement of modern surgical nursing. Future larger multicenter studies are needed to confirm its effectiveness and feasibility.
| 1. | Zhang G, Wu B. Meta-analysis of the clinical efficacy of laparoscopic appendectomy in the treatment of acute appendicitis. World J Emerg Surg. 2022;17:26. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 2] [Cited by in RCA: 10] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 2. | Turkes GF, Unsal A, Bulus H. Predictive value of immature granulocyte in the diagnosis of acute complicated appendicitis. PLoS One. 2022;17:e0279316. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 11] [Reference Citation Analysis (0)] |
| 3. | Reitz KM, Zuckerbraun BS. Treating the Patient With Appendicitis, Not Just the Appendicitis. JAMA Surg. 2019;154:149. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.2] [Reference Citation Analysis (0)] |
| 4. | Sohn M, Agha A, Bremer S, Lehmann KS, Bormann M, Hochrein A. Surgical management of acute appendicitis in adults: A review of current techniques. Int J Surg. 2017;48:232-239. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 15] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 5. | Li ZL, Ma HC, Yang Y, Chen JJ, Wang ZJ. Clinical study of enhanced recovery after surgery in laparoscopic appendectomy for acute appendicitis. World J Gastrointest Surg. 2024;16:816-822. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |
| 6. | Chen Y, Liu Y, Guo S, Yuan J, Li X. Single-port laparoscopic appendectomy using a needle-type grasping forceps for selective adult patients with acute uncomplicated appendicitis. J Surg Case Rep. 2022;2022:rjab557. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 3] [Cited by in RCA: 4] [Article Influence: 1.3] [Reference Citation Analysis (1)] |
| 7. | Yang L, Zheng R, Li H, Ren Y, Chen H. The burden of appendicitis and surgical site infection of appendectomy worldwide. J Infect Dev Ctries. 2023;17:367-373. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 7] [Reference Citation Analysis (0)] |
| 8. | Liang J, Wang L, Song J, Zhao Y, Zhang K, Zhang X, Hu C, Tian D. The impact of nursing interventions on the rehabilitation outcome of patients after lumbar spine surgery. BMC Musculoskelet Disord. 2024;25:354. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 9. | Zhang Y, Guo L, Zheng G, Tang J, Xue Y, Zhang M, Yang X. Analysis of the Effect of Rapid Rehabilitation Nursing in the Perioperative Period of Brucellar Spondylitis. Altern Ther Health Med. 2024. [PubMed] |
| 10. | Song JY, Cao J, Mao J, Wang JL. Effect of rapid rehabilitation nursing on improving clinical outcomes in postoperative patients with colorectal cancer. World J Gastrointest Surg. 2024;16:2119-2126. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Reference Citation Analysis (12)] |
| 11. | Zhang Q, Lin H, Wang F, Li Q, Song W. Factors Affecting Low Anterior Resection Syndrome following Anus-Preserving Surgery for Rectal Cancer and Assessing the Impact of Nursing Interventions in Rapid Rehabilitation Surgery. Altern Ther Health Med. 2024;. [PubMed] |
| 12. | Shen Q, Jiang T. Implementing Accelerated Rehabilitation Nursing to Facilitate Intestinal Function Recovery Following Cytoreductive Surgery for Gynecological Ovarian Cancer. Altern Ther Health Med. 2024;. [PubMed] |
| 13. | Smith TW Jr, Wang X, Singer MA, Godellas CV, Vaince FT. Enhanced recovery after surgery: A clinical review of implementation across multiple surgical subspecialties. Am J Surg. 2020;219:530-534. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 52] [Cited by in RCA: 144] [Article Influence: 28.8] [Reference Citation Analysis (0)] |
| 14. | Yan W, Xu X, Cui H, Li W. Application of the concept of rapid rehabilitation in the operating room nursing of laparoscopic gastrointestinal surgery. Panminerva Med. 2021;. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1] [Cited by in RCA: 1] [Article Influence: 0.3] [Reference Citation Analysis (0)] |
| 15. | Bao X, Zhang L, Du Y, Yan F, Sun S, Wu H. Evidence-Based Nursing Interventions in Care of Heart-failure Patients With Concurrent Tumors. Altern Ther Health Med. 2024;30:377-383. [PubMed] |
| 16. | Ljubas I, Jurca I, Grgić D. Chronic Appendicitis: Possible Differential Diagnosis in Patients with Chronic Abdominal Pain. Case Rep Surg. 2024;2024:6032042. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 17. | Hong H, Qian K, Ying Y, Xu H. Observation on the Effect of Rapid Rehabilitation Nursing with Integrated Medical Care in Perioperative Period of Laparoscopic Appendicitis in Children. Ann Ital Chir. 2024;95:401-410. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 2] [Reference Citation Analysis (0)] |
| 18. | Xie G, Wu Q, Guo X, Zhang J, Yin D. Psychological resilience buffers the association between cell phone addiction and sleep quality among college students in Jiangsu Province, China. Front Psychiatry. 2023;14:1105840. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 17] [Reference Citation Analysis (0)] |
| 19. | Ye Y, Ge J. Clinical application of comfort nursing in elderly patients with advanced lung cancer. Am J Transl Res. 2021;13:9750-9756. [PubMed] |
| 20. | Ljungqvist O, Scott M, Fearon KC. Enhanced Recovery After Surgery: A Review. JAMA Surg. 2017;152:292-298. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1487] [Cited by in RCA: 2226] [Article Influence: 278.3] [Reference Citation Analysis (0)] |
| 21. | Wang X, Li Y, Yang W. Rapid Rehabilitation Program Can Promote the Recovery of Gastrointestinal Function, Speed Up the Postoperative Rehabilitation Process, and Reduce the Incidence of Complications in Patients Undergoing Radical Gastrectomy. J Oncol. 2022;2022:1386382. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 6] [Reference Citation Analysis (0)] |
| 22. | Robella M, Tonello M, Berchialla P, Sciannameo V, Ilari Civit AM, Sommariva A, Sassaroli C, Di Giorgio A, Gelmini R, Ghirardi V, Roviello F, Carboni F, Lippolis PV, Kusamura S, Vaira M. Enhanced Recovery after Surgery (ERAS) Program for Patients with Peritoneal Surface Malignancies Undergoing Cytoreductive Surgery with or without HIPEC: A Systematic Review and a Meta-Analysis. Cancers (Basel). 2023;15. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 11] [Reference Citation Analysis (0)] |
| 23. | Song R, Chen C, Shang L. Efficacy and Satisfaction Evaluation of Rapid Rehabilitation Nursing Intervention in Patients with Laparoscopic Myomectomy. J Oncol. 2022;2022:9412050. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 1] [Reference Citation Analysis (0)] |