Published online Sep 27, 2023. doi: 10.4240/wjgs.v15.i9.2074
Peer-review started: April 24, 2023
First decision: June 12, 2023
Revised: July 9, 2023
Accepted: July 28, 2023
Article in press: July 28, 2023
Published online: September 27, 2023
Processing time: 151 Days and 4.7 Hours
Lupus mesenteric vasculitis (LMV) is a serious condition that may occur as an acute manifestation of gastrointestinal (GI) involvement and is not easily diagnosed by physicians. Delayed diagnosis and treatment of LMV may lead to rapid disease progression and can be life threatening.
A previously healthy 27-year-old woman presented with abdominal pain following a history of fatigue and consumption of cold water. Laboratory investigations, physical examinations, and enhanced abdominal computed tomography (CT) suggested systemic lupus erythematosus complicated by LMV. She received treatments, such as GI decompression, somatostatin, glucocorticoids, and immu
Early diagnosis of LMV is essential for successful treatment; this depends on a combination of clinical manifestations, laboratory investigations, and imaging findings. Enhanced CT is preferred, but ultrasonography can be used for prompt screening and follow-up.
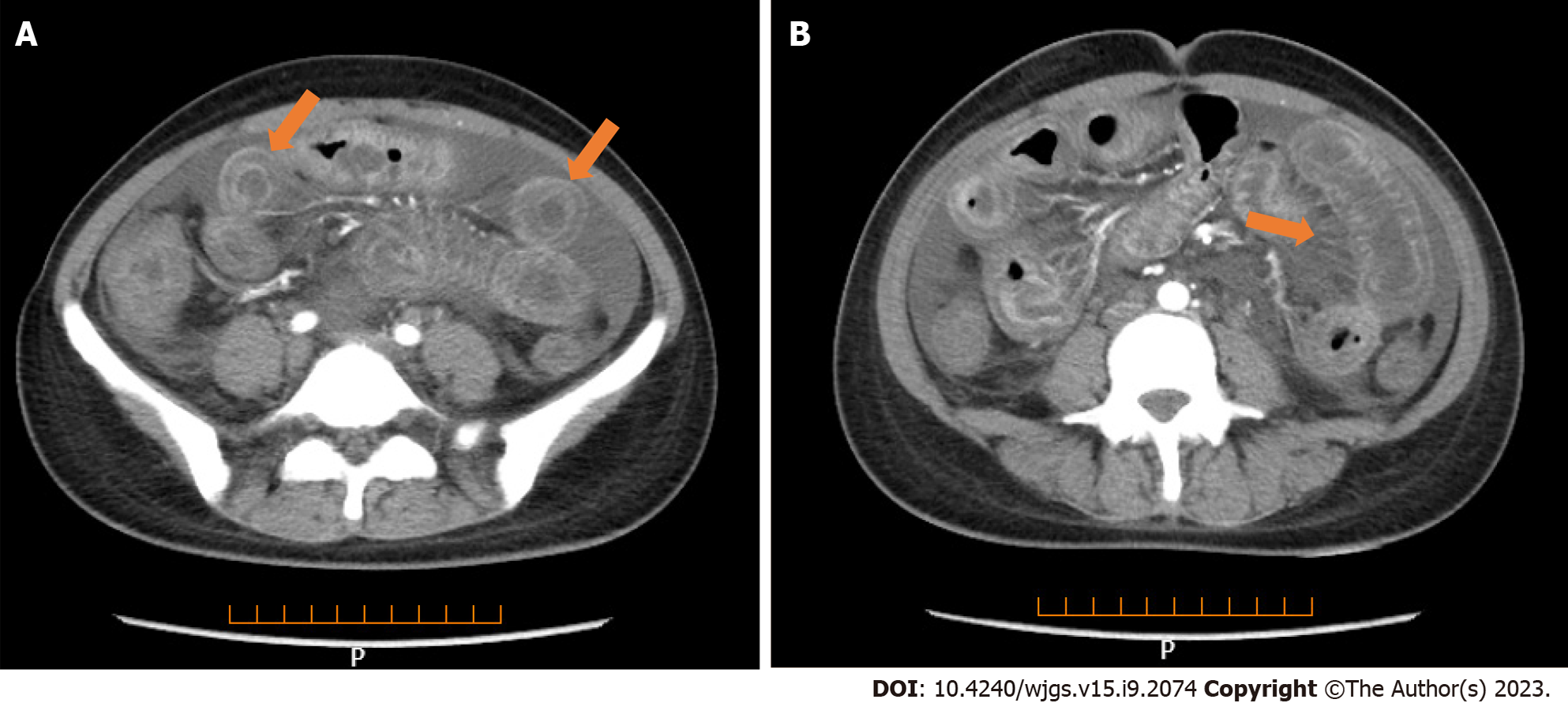
Core Tip: When a systemic lupus erythematosus patient presenting with gastrointestinal symptoms, lupus mesenteric vasculitis (LMV) must be considered despite being rare. Enhanced abdominal computed tomography revealing thicked jejunal wall (target sign) and engorgement of the mesenteric vessels (comb sign) were suggestive of mesenteric vasculitis and provide evidence for accurately treatment. Abdominal ultrasonography can be a reliable tool used for preliminary screening, therapeutic evaluation and follow-up for LMV.
- Citation: Huang H, Li P, Zhang D, Zhang MX, Yu K. Acute flare of systemic lupus erythematosus with extensive gastrointestinal involvement: A case report and review of literature. World J Gastrointest Surg 2023; 15(9): 2074-2082
- URL: https://www.wjgnet.com/1948-9366/full/v15/i9/2074.htm
- DOI: https://dx.doi.org/10.4240/wjgs.v15.i9.2074
Systemic lupus erythematosus (SLE) is a chronic multisystemic autoimmune disease of unknown etiology. Under the influence of genetic predisposition and environmental risk factors, alterations in the immune response include hyperactivation of T and B lymphocytes, loss of self-tolerance and formation of circulating pathogenic immune complexes and subsequent deposition in several organs, thereby causing damage. The incidence of SLE is approximately 30–70 cases per 100000 individuals in China[1]. Females of reproductive age are mostly affected.
Gastrointestinal (GI) symptoms are present in > 50% of SLE patients throughout the course of the disease[2]. Among the wide spectrum of SLE-associated GI complications, including abdominal serositis/peritonitis, protein-losing enteropathy, intestinal pseudo-obstruction, hepatic involvement, and pancreatitis, lupus mesenteric vasculitis (LMV) is rare, but one of the most serious complications of SLE with high mortality[3]. Early diagnosis of LMV is crucial for prompt treatment.
LMV or lupus enteritis (LE), was originally proposed by Hoffman and Katz[4] in 1980. The early clinical presentation of LE comprises abdominal pain, nausea, vomiting, or severe GI bleeding, which is unremarkable and non-specific and is easily mistaken for infectious gastroenteritis and medication-related adverse effects. The rarity of LE in SLE, which makes it unincluded in any SLE classification criteria or weighted in the SLE Disease Activity Index (SLEDAI), makes early clinical suspicion difficult to elicit. In the British Isles Lupus Assessment Group disease activity index, LE is defined as either vasculitis or inflammation of the small or large bowel with supportive imaging and/or biopsy findings[5]. Since histological evidence is difficult to obtain, it is important to find a rapid, reliable, and safe diagnostic tool. This case review aimed to identify possible strategies for early diagnosis of LE among women of reproductive age.
A 27-year-old woman was referred to our department on account of abdominal pain that had persisted for six days.
The patient was initially transferred to our department after an enhanced abdominal computed tomography (CT) examination and GI decompression.
The patient had no photosensitivity, alopecia, oral ulcers, arthritis, or Raynaud’s phenomenon, and was previously healthy.
The patient had no family history of SLE.
Upon examination, the abdomen was distended with no tenderness or rebound pain. No palpable masses or active bowel sounds were detected.
Antinuclear antibody titer was 1:320, and anti-U1 ribonucleoprotein and anti-Sjogren's syndrome A antibodies were positive, whereas anti-double-stranded DNA (anti-dsDNA) antibody and anti-Smith antibody were negative. The levels of C3 and C4 compliments decreased to 0.245 g/L (0.7–1.4 g/L) and 0.024 g/L (0.1–0.4 g/L), respectively. Immunoglobulin G (IgG) level was 10.45 g/L (7–16 g/L), and direct antiglobulin "Coombs" test results were positive. Routine blood tests showed a white blood cell count of 1.40 × 1010/L (3.5× 109–9.5 × 109/L), platelet count of 2.01 × 1011/L (1.25 × 1011–3.50 × 1011/L), and hemoglobin level of 114 g/L (115–150 g/L). Urine microscopy revealed a pathological tube-type 1 per low power field. Liver enzyme levels and renal function were normal. Moreover, serum albumin level was 33.2 g/L (40–55 g/L); erythrocyte sedimentation rate (ESR) was 3 mm/h (0-22 mm/h); C-reactive protein (CRP) level was 1.28 mg/L (< 10 mg/L); procalcitonin level was 0.293 ng/mL (0–0.046 ng/mL); blood potassium level was 2.9 mmol/L (3.5–5.3 mmol/L); cardiac enzyme levels were normal; and 24 h total urine protein level was 0.51 g/d (0.01–0.15 g/d).
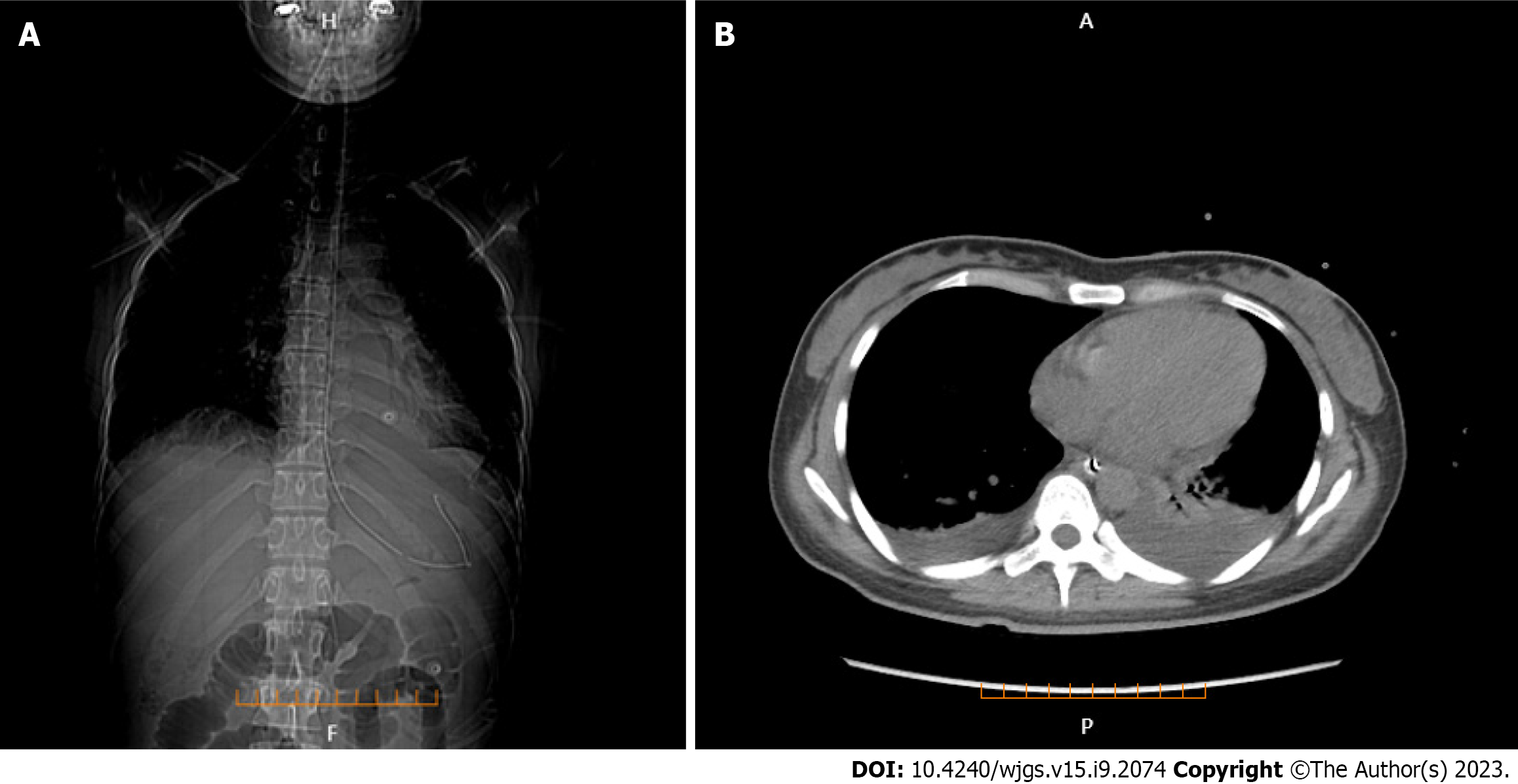
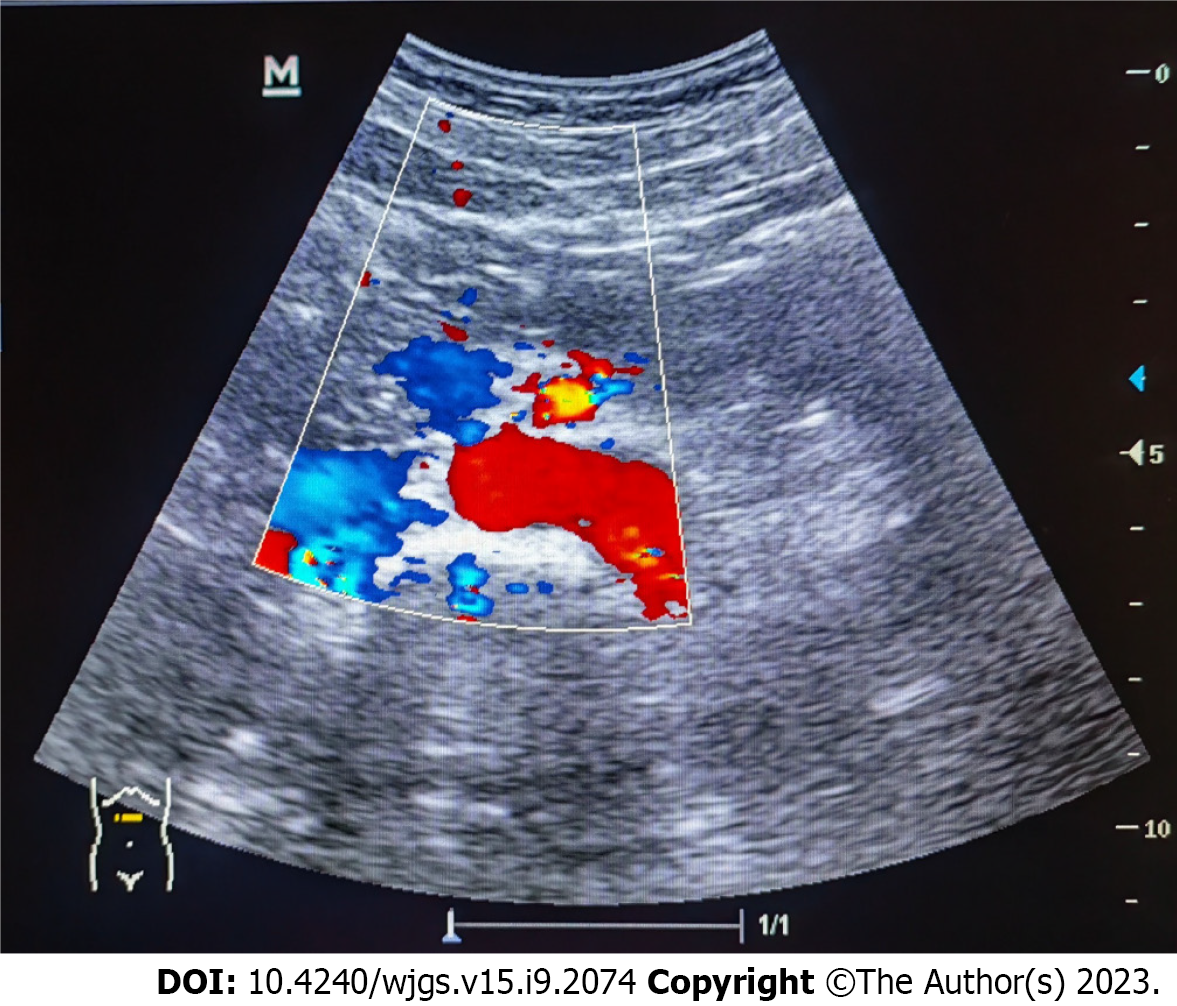
Lung CT showed bilateral pleural effusion (Figure 1). Enhanced abdominal CT showed the typical "target and comb signs" performance (Figure 2). Further investigation revealed LMV and incomplete intestinal obstruction. Some segmental bowel walls of the transverse colon were thickened by approximately 5 mm, and the main color flow of the superior mesenteric artery was well filled without embolism (Figures 3 and 4).
According to the 2019 European League Against Rheumatism/American College of Rheumatology classification criteria for SLE, autoimmune hemolysis (4 points) + pleural or pericardial effusion (5 points) + low C3 and C4 (4 points) + proteinuria (4 points) = 17 points, which was > 10 points, and the patient met the diagnostic criteria; therefore, LMV and lupus nephritis were diagnosed. The SLEDAI-2K score was eight.
After fasting, GI decompression, intravenous nutrition, methylprednisolone 80 mg per day intravenously, and immunoglobulin 20 g per day intravenously for five days, the symptoms were relieved, and the patient was able to tolerate semi-liquid food. Furthermore, the methylprednisolone dose was gradually decreased to 40 mg per day intravenously. Fourteen days later, the methylprednisolone dose was adjusted to 36 mg per day orally, and this dosage was maintained for approximately one month, even after the patient was discharged. Moreover, she was treated with cyclophosphamide 0.2 g qod intravenously twice with a cumulative dose of 0.4 g, which was switched to mycophenolate mofetil (MMF) 0.75 g bid orally. Owing to the GI inflammation, intravenous antibiotics were administered for 15 d. Somatostatin reduced the intestinal inflammation, exudation, and gastric acid secretion. Nadroparin calcium was administered to prevent micro- or small mesenteric thrombosis.
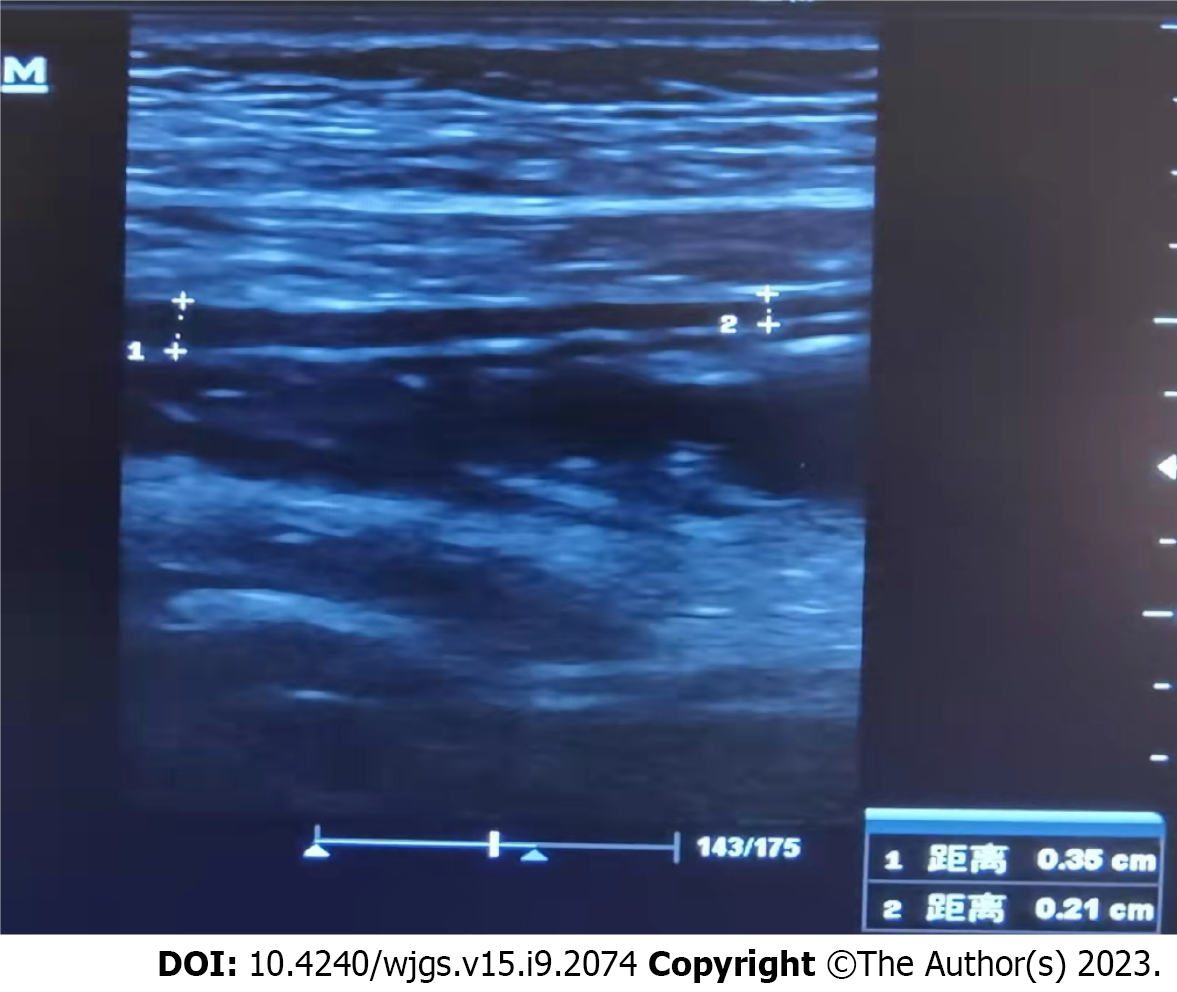
Twenty days after the treatment, the patient was able to eat semi-liquid food without stomach discomfort. Bowel sounds returned to normal. Laboratory investigations showed complement levels had increased. The IgG level was 15.6 g/L (7–16 g/L), and renal function, hepatic enzyme levels, and electrolyte levels were normal. Routine urine and stool test results were normal. Ten days after the treatment, ultrasonography was used to assess the patient’s condition, which demonstrated that the local intestinal wall was approximately 0.35 cm at its thickest part (Figure 5), and that there was no effusion in the pleural, abdominal, or pelvic cavities. Most of the intestinal wall thickness decreased to a normal size. Finally, the intestinal lumen did not expand, and the multiserous cavity effusion disappeared. The abdominal signs and symptoms reduced, and the patient tolerated full feeding and was discharged.
The patient was follow-up at two-weekly intervals for the first three months and monthly thereafter. One year later, the patient was treated with methylprednisolone, which was tapered to 4 mg per day, MMF 0.75 g bid, and hydroxychloroquine 0.2 g bid. The C4 complement level was normalized, but the C3 complement level was 0.663 g/L (0.7–1.4 g/L), still slightly below the normal level. Table 1 shows the timeline from symptom onset to the last follow-up visit.
| Time of admission (March 29, 2022) | Time of discharge (April 4, 2022) | Last follow-up (June 16, 2023) | |
| WBC (3.5 × 109-9.5 × 109/L) | 6.4 | 4.3 | 6.2 |
| Hemoglobin (115–150 g/L) | 98 | 100 | 133 |
| Platelet (1.25 × 1011–3.50 × 1011/L) | 212 | 226 | 224 |
| CRP (0–6 mg/L) | 0.4 | 1.28 | 0.2 |
| ESR (0–20 mm/h) | 3 | 11 | 6 |
| IgG (7–16 g/L) | 10.45 | 15.6 | 11.56 |
| IgA (0.7–4 g/L) | 0.81 | 1.02 | 0.78 |
| IgM (0.4–2.3 g/L) | 0.46 | 0.603 | 0.72 |
| C3 (0.9–1.8 g/L) | 0.245 | 0.449 | 0.663 |
| C4 (0.1–0.4 g/L) | 0.027 | 0.082 | 0.143 |
| Serum albumin (40–55 g/L) | 22.8 | 38.3 | 43.5 |
| Alanine aminotransferase (7–40 U/L) | 9.22 | 14 | 13.31 |
| Aspartate aminotransferase (13–35 U/L) | 20.86 | 9 | 22.37 |
| Serum creatinine (41-73 μmol/L) | 73.2 | 42 | 52.2 |
| Serum urea nitrogen (3.1–8 mmol/L) | 8.24 | 3.84 | 3.74 |
| Lung CT | Bilateral pleural effusion | Normal | Normal |
| Ultrasonography | Bowel walls were thickened by approximately 5 mm | Bowel walls were thickened by approximately 3.5 mm | Normal |
LE, also known LMV[6], is rare and one of the most devastating complications of SLE. The incidence of LMV is estimated to range between 0.2%–9.7% among patients already diagnosed with SLE and between 13.0%–62.5% in patients with isolated LE as the initial presentation of SLE[7].
The pathophysiology of LMV is leukocytoclastic vasculitis secondary to the deposition of immune complexes in vascular walls, and antiphospholipid antibody-associated vasculopathy leading to thrombosis[8]. Ischemia causes the greatest damage to the mucosal mesenteric vessels, followed by the vasculature of the muscularis propria, submucosa, and plasma membrane[6]. Certain triggering factors (bacterial or viral infections, chemicals, etc.) can activate endothelial cells and expose them to cryptic antigens, resulting in the production of anti-endothelial cell antibodies, activation of complement, and deposition of immune complexes on inflamed blood vessel walls, which can lead to vascular damage and thrombosis[6]. The literature reported that vasculitis was histologically confirmed by biopsy samples of the affected intestinal segments[9]. The submucosa, filled with a mild diffuse inflammatory infiltrate of mononuclear cells, becomes edematous, and hemorrhage can be observed mostly in the muscular and subserosal layers; fibrinoid necrosis, leukocytoclasis on the vascular wall, and fibrin thrombus formation can be observed in the subserosal vessels.
The initial presenting signs and symptoms of LE are heterogeneous and commonplace and are usually mistaken for GI infections, peptic ulcers, lithiasis cholecystitis, or side effects of medications. However, the most common symptom in more than 90% of patients is abdominal pain of varying intensity caused by intestinal ischemia secondary to vasculitis[10]. Signs and symptoms of impaired GI motility and peritonitis are also common in patients with SLE. Diarrhea was frequent, with a frequency of 43.5%–64.7% in different studies[11]. Vomiting was found among 39.5%–72.2% of Asian patients[12]. Ascites was also frequently reported in the literature (27.9%–94.1%). This was also observed in our patient. GI bleeding is a rare but serious presentation that may be due to intestinal ischemia and intestinal necrosis. If not recognized in time, it may lead to perforation with a mortality rate of up to 50%[13]. The ileum and jejunum were the most frequently involved intestinal sites (> 80%) reported in the literature[14].
Timely and accurate diagnosis of LMV is a great challenge due to the lack of knowledge about LMV. Therefore, it is necessary to explore the factors associated with LMV.
Several studies have found that patients accompanied by oral ulcers or lupus urinary tract involvement have a greater risk of encountering LMV[15-17]. Therefore, clinicians should suspect LMV when clinical laboratory results suggest lupus involvement of oral ulcers and the urinary system.
Previous studies have shown that there is no significant difference in SLEDAI scores in patients with SLE presenting with abdominal pain, regardless of the presence or absence of LE[14]. In patients with LMV, there was no difference in SLEDAI scores for serious adverse events, such as intestinal hemorrhage, infarction, perforation, or death due to serious complications, suggesting that SLE activity does not correlate with the severity of LMV[9]. Although SLEDAI was higher at baseline in LE patients than in non-LE patients, it did not predict the development of LE[18].
Laboratory tests are of value in the diagnosis of LE. However, CRP is usually normal and complement levels are decreased[7]. In seropositive cases, antibodies were more reliable, with increased titers of antinuclear, anti-dsDNA, and anti-Smith antibodies, which were approximately 92%, 80%, and 20%, respectively[19]. These autoimmune and inflammatory markers, while informative in diagnosis, are not essential. LE can occur without clinically active lupus[7]. Other researchers did not find laboratory parameters, including complement, ESR, CRP, lupus-related antibodies, and antiphospholipid antibodies to be correlated with the risk of LE[8,14].
Multiple methods, including ultrasonography, CT, magnetic resonance imaging, and GI endoscopy, have been used to evaluate LMV. However, CT is fast and non-invasive and can be used to perform image reconstruction and post-processing, to observe the LMV in multiple directions, and to observe lesions of the mesentery and blood vessels. Enhanced abdominal CT is more sensitive in detecting intestinal abnormalities, as it can reveal thickened and swollen bowel walls that contain enhanced mucosal, edematous submucosal, and enhanced serosal layers. Normal bowel wall thickness visualized by CT was < 3 mm; 3–5 mm thick bowel walls were considered mildly thickened, 6–7 mm moderately thickened, and > 8 mm markedly thickened[20]. This categorization is important in judging the occurrence of LE[9,21]. There are three typical abdominal CT findings in patients with LE, and these can appear alone or concurrently: Bowel wall thickening (> 3.0 mm), which leads to separation of the mucosa and muscle layers and “target sign” appearance; mesenteric vasodilation with “comb sign” appearance; and increased attenuation of mesenteric fat[15,19,22-25]. The co-occurrence of “target sign” and “comb sign” is particularly specific to LE, and can be used to establish a diagnosis. Unfortunately, these imaging manifestations are not uncommon in inflammatory bowel disease, intestinal ischemia, and mesenteric vein thrombosis.
Magnetic resonance enterography can also be used to diagnose LE. The main advantages of magnetic resonance enterography are that it allows for a holistic assessment of the bowel, both intestinal and extra-intestinal, as well as a high degree of safety as the examination can be repeated in a short period of time[26]. However, the slightly longer scan time, the radiologist's manipulation, and the patient's tolerance of the contrast agent may limit magnetic resonance enterography.
Ultrasonography is likely to be the most readily available imaging method, and a valuable alternative to CT when the latter is not available or is contraindicated. Being a safe and more accessible technique, ultrasonography was the first imaging examination when our patient presented to the emergency room. The study[27] have described patients with LE who had characteristic intestinal wall edema and ascites based on ultrasonography. Ultrasonography revealed thickening of the intestinal wall, in which the submucosal edema of the Kerckring fold resembled an accordion[28], dilation of intestinal segments, increased reflectivity of mesenteric fat, and mild ascites. CT confirmed these features, suggesting that both methods have similar sensitivities for LE diagnosis. Regarding specificity, ultrasonography has similar limitations with CT. If the patient is a young woman of childbearing age, ultrasonography is likely to be the best screening examination for suspected LMV diagnosis and follow-up[14]. Therefore, ultrasonography is a reliable and accessible tool.
Although the gold standard for diagnosing LE is pathology, the positive rate is low. Therefore, endoscopy is not used as a routine diagnostic tool. Only a few cases present intestinal edema, congestion and ischemia with or without ulceration or necrosis[7].
Due to the lack of prospective randomized controlled clinical trials, there are currently no available guidelines or recommendations for LE treatment.
The prognosis is good when the diagnosis is made early, and high-dose steroids are started in a timely manner; however, patients may occasionally experience recurrence. Glucocorticoids are the primary medications used to treat LE. Cyclophosphamide is one of the most commonly used immunosuppressants used for SLE treatment in China, and its combination with corticosteroids results in a good response[29]. Cyclophosphamide, whether intravenous pulse or not, has been useful in preventing relapses of lupus flares[2]. However, considering its lower reproductive toxicity, we switched to MMF treatment, which is preferred in young men and women due to the high risk of testicular and ovarian failure following cyclophosphamide[30]. Although rituximab, an anti-CD20 antibody, showed promising potential in observational studies, the LUNAR randomized controlled trials did not show that rituximab combined with MMF had additional benefits during remission compared with MMF alone[31].
LMV causes inflammation in the intestinal wall, which enhances its permeability. Dysregulation of the intestinal microbiota can lead to intestinal infection. Antibiotics were administered to control the risk of infection. Octreotide treatment may be effective, owing to its immunomodulatory effects, regulation of intestinal microvasculature blood flow, and amelioration of lymphatic dilatation[32]. Considering the aforementioned effects of somatostatin, we administered it to the patient and good outcomes were achieved.
Despite being rare, LMV must always be considered in any SLE patient presenting with GI symptoms. The diagnosis of LMV requires a combination of history and clinical and immunological indicators. Moreover, enhanced CT examination can reveal the extent and scope of GI lesions involved in SLE and provide evidence for timely clinical diagnosis and treatment. For pregnant women, or physicians in primary hospitals, ultrasonography can be an alternative method for preliminary screening and follow-up.
We are grateful to the patient for permitting us to publish this study.
Provenance and peer review: Unsolicited article; Externally peer reviewed.
Peer-review model: Single blind
Specialty type: Gastroenterology and hepatology
Country/Territory of origin: China
Peer-review report’s scientific quality classification
Grade A (Excellent): 0
Grade B (Very good): 0
Grade C (Good): C, C, C
Grade D (Fair): 0
Grade E (Poor): 0
P-Reviewer: Makovicky P, Slovakia; Yale SH, United States S-Editor: Lin C L-Editor: A P-Editor: Guo X
| 1. | Zeng QY, Chen R, Darmawan J, Xiao ZY, Chen SB, Wigley R, Le Chen S, Zhang NZ. Rheumatic diseases in China. Arthritis Res Ther. 2008;10:R17. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 276] [Cited by in RCA: 280] [Article Influence: 16.5] [Reference Citation Analysis (0)] |
| 2. | Chng HH, Tan BE, Teh CL, Lian TY. Major gastrointestinal manifestations in lupus patients in Asia: lupus enteritis, intestinal pseudo-obstruction, and protein-losing gastroenteropathy. Lupus. 2010;19:1404-1413. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 47] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 3. | Fawzy M, Edrees A, Okasha H, El Ashmaui A, Ragab G. Gastrointestinal manifestations in systemic lupus erythematosus. Lupus. 2016;25:1456-1462. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 33] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 4. | Hoffman BI, Katz WA. The gastrointestinal manifestations of systemic lupus erythematosus: a review of the literature. Semin Arthritis Rheum. 1980;9:237-247. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 110] [Cited by in RCA: 101] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 5. | Isenberg DA, Rahman A, Allen E, Farewell V, Akil M, Bruce IN, D'Cruz D, Griffiths B, Khamashta M, Maddison P, McHugh N, Snaith M, Teh LS, Yee CS, Zoma A, Gordon C. BILAG 2004. Development and initial validation of an updated version of the British Isles Lupus Assessment Group's disease activity index for patients with systemic lupus erythematosus. Rheumatology (Oxford). 2005;44:902-906. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 397] [Cited by in RCA: 454] [Article Influence: 22.7] [Reference Citation Analysis (0)] |
| 6. | Ju JH, Min JK, Jung CK, Oh SN, Kwok SK, Kang KY, Park KS, Ko HJ, Yoon CH, Park SH, Cho CS, Kim HY. Lupus mesenteric vasculitis can cause acute abdominal pain in patients with SLE. Nat Rev Rheumatol. 2009;5:273-281. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 97] [Cited by in RCA: 98] [Article Influence: 6.1] [Reference Citation Analysis (0)] |
| 7. | Janssens P, Arnaud L, Galicier L, Mathian A, Hie M, Sene D, Haroche J, Veyssier-Belot C, Huynh-Charlier I, Grenier PA, Piette JC, Amoura Z. Lupus enteritis: from clinical findings to therapeutic management. Orphanet J Rare Dis. 2013;8:67. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 85] [Cited by in RCA: 101] [Article Influence: 8.4] [Reference Citation Analysis (0)] |
| 8. | Kwok SK, Seo SH, Ju JH, Park KS, Yoon CH, Kim WU, Min JK, Park SH, Cho CS, Kim HY. Lupus enteritis: clinical characteristics, risk factor for relapse and association with anti-endothelial cell antibody. Lupus. 2007;16:803-809. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 56] [Cited by in RCA: 59] [Article Influence: 6.6] [Reference Citation Analysis (0)] |
| 9. | Yuan S, Ye Y, Chen D, Qiu Q, Zhan Z, Lian F, Li H, Liang L, Xu H, Yang X. Lupus mesenteric vasculitis: clinical features and associated factors for the recurrence and prognosis of disease. Semin Arthritis Rheum. 2014;43:759-766. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 50] [Cited by in RCA: 49] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 10. | Zhang W, Huang G, Lin J, Lin Q, Zheng K, Hu S, Zheng S, Du G, Matucci-Cerinic M, Furst DE, Wang Y. Predictive model of risk and severity of enteritis in systemic lupus erythematosus. Lupus. 2022;31:1226-1236. [RCA] [PubMed] [DOI] [Full Text] [Reference Citation Analysis (0)] |
| 11. | Koo BS, Hong S, Kim YJ, Kim YG, Lee CK, Yoo B. Lupus enteritis: clinical characteristics and predictive factors for recurrence. Lupus. 2015;24:628-632. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 32] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 12. | Chen L, He Q, Luo M, Gou Y, Jiang D, Zheng X, Yan G, He F. Clinical features of lupus enteritis: a single-center retrospective study. Orphanet J Rare Dis. 2021;16:396. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in RCA: 16] [Reference Citation Analysis (0)] |
| 13. | Trapani S, Rubino C, Simonini G, Indolfi G. Gastrointestinal and hepatic involvement in paediatric systemic lupus erythematosus. Clin Exp Rheumatol. 2021;39:899-906. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 2] [Cited by in RCA: 2] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 14. | Lee CK, Ahn MS, Lee EY, Shin JH, Cho YS, Ha HK, Yoo B, Moon HB. Acute abdominal pain in systemic lupus erythematosus: focus on lupus enteritis (gastrointestinal vasculitis). Ann Rheum Dis. 2002;61:547-550. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 151] [Cited by in RCA: 130] [Article Influence: 5.7] [Reference Citation Analysis (0)] |
| 15. | Chu YC, Hsu BB, Tseng KC. Lupus mesenteric vasculitis with GI and genitourinary tract involvement. Clin Gastroenterol Hepatol. 2014;12:e69-70; quiz e71. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 6] [Article Influence: 0.5] [Reference Citation Analysis (0)] |
| 16. | Shimizu A, Tamura A, Tago O, Abe M, Nagai Y, Ishikawa O. Lupus cystitis: a case report and review of the literature. Lupus. 2009;18:655-658. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 22] [Article Influence: 1.4] [Reference Citation Analysis (0)] |
| 17. | Tan TC, Wansaicheong GK, Thong BY. Acute onset of systemic lupus erythematosus with extensive gastrointestinal and genitourinary involvement. Lupus. 2012;21:1240-1243. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 12] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 18. | Duarte-García A, Hocaoglu M, Osei-Onomah SA, Dabit JY, Giblon RE, Helmick CG, Crowson CS. Population-based incidence and time to classification of systemic lupus erythematosus by three different classification criteria: a Lupus Midwest Network (LUMEN) study. Rheumatology (Oxford). 2022;61:2424-2431. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 12] [Article Influence: 4.0] [Reference Citation Analysis (0)] |
| 19. | Smith LW, Petri M. Lupus enteritis: an uncommon manifestation of systemic lupus erythematosus. J Clin Rheumatol. 2013;19:84-86. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 21] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 20. | Si-Hoe CK, Thng CH, Chee SG, Teo EK, Chng HH. Abdominal computed tomography in systemic lupus erythematosus. Clin Radiol. 1997;52:284-289. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 31] [Cited by in RCA: 28] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 21. | Kim YG, Ha HK, Nah SS, Lee CK, Moon HB, Yoo B. Acute abdominal pain in systemic lupus erythematosus: factors contributing to recurrence of lupus enteritis. Ann Rheum Dis. 2006;65:1537-1538. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 37] [Cited by in RCA: 30] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 22. | Goh YP, Naidoo P, Ngian GS. Imaging of systemic lupus erythematosus. Part II: gastrointestinal, renal, and musculoskeletal manifestations. Clin Radiol. 2013;68:192-202. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 9] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 23. | Lin HP, Wang YM, Huo AP. Severe, recurrent lupus enteritis as the initial and only presentation of systemic lupus erythematosus in a middle-aged woman. J Microbiol Immunol Infect. 2011;44:152-155. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 10] [Article Influence: 0.7] [Reference Citation Analysis (0)] |
| 24. | Sran S, Sran M, Patel N, Anand P. Lupus enteritis as an initial presentation of systemic lupus erythematosus. Case Rep Gastrointest Med. 2014;2014:962735. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 4] [Cited by in RCA: 11] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 25. | Alves SC, Fasano S, Isenberg DA. Autoimmune gastrointestinal complications in patients with systemic lupus erythematosus: case series and literature review. Lupus. 2016;25:1509-1519. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 29] [Cited by in RCA: 33] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 26. | Cicero G, Blandino A, D'Angelo T, Bottari A, Cavallaro M, Ascenti G, Mazziotti S. Magnetic resonance enterography appraisal of lupus enteritis: A case report. Radiol Case Rep. 2018;13:915-919. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 7] [Cited by in RCA: 7] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 27. | Demiselle J, Sayegh J, Cousin M, Olivier A, Augusto JF. An Unusual Cause of Abdominal Pain: Lupus Enteritis. Am J Med. 2016;129:e11-e12. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 5] [Cited by in RCA: 7] [Article Influence: 0.8] [Reference Citation Analysis (0)] |
| 28. | Shirato M, Hisa N, Fujikura Y, Ohkuma K, Kutsuki S, Hiramatsu K. [Imaging diagnosis of lupus enteritis--especially about sonographic findings]. Nihon Igaku Hoshasen Gakkai Zasshi. 1992;52:1394-1399. [PubMed] |
| 29. | Chen Z, Li MT, Xu D, Yang H, Li J, Zhao JL, Zhang HH, Han SM, Xu T, Zeng XF. Protein-losing enteropathy in systemic lupus erythematosus: 12 years experience from a Chinese academic center. PLoS One. 2014;9:e114684. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 25] [Cited by in RCA: 23] [Article Influence: 2.1] [Reference Citation Analysis (0)] |
| 30. | Soares PM, Borba EF, Bonfa E, Hallak J, Corrêa AL, Silva CA. Gonad evaluation in male systemic lupus erythematosus. Arthritis Rheum. 2007;56:2352-2361. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 79] [Cited by in RCA: 82] [Article Influence: 4.6] [Reference Citation Analysis (0)] |
| 31. | Rovin BH, Furie R, Latinis K, Looney RJ, Fervenza FC, Sanchez-Guerrero J, Maciuca R, Zhang D, Garg JP, Brunetta P, Appel G; LUNAR Investigator Group. Efficacy and safety of rituximab in patients with active proliferative lupus nephritis: the Lupus Nephritis Assessment with Rituximab study. Arthritis Rheum. 2012;64:1215-1226. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 866] [Cited by in RCA: 995] [Article Influence: 76.5] [Reference Citation Analysis (0)] |
| 32. | Kubo M, Uchida K, Nakashima T, Oda S, Nakamura T, Hashimoto S, Watada T, Nakamura H, Araki J, Matsuzaki M, Yano M. [Protein-losing enteropathy with systemic lupus erythematosus effectively treated with octreotide and medium chain triglyceride diet: A case report]. Nihon Rinsho Meneki Gakkai Kaishi. 2015;38:421-425. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 4] [Article Influence: 0.4] [Reference Citation Analysis (0)] |