Copyright
©The Author(s) 2016.
World J Hepatol. Nov 28, 2016; 8(33): 1419-1441
Published online Nov 28, 2016. doi: 10.4254/wjh.v8.i33.1419
Published online Nov 28, 2016. doi: 10.4254/wjh.v8.i33.1419
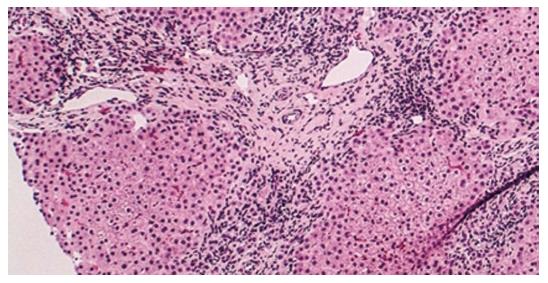
Figure 1 Histology of primary biliary cholangitis (hematoxylin and eosin staining; × 200 liver biopsy).
An absence/paucity of bile ducts is seen with focal chronic inflammation in a portal area consistent with late-stage primary biliary cholangitis[9].
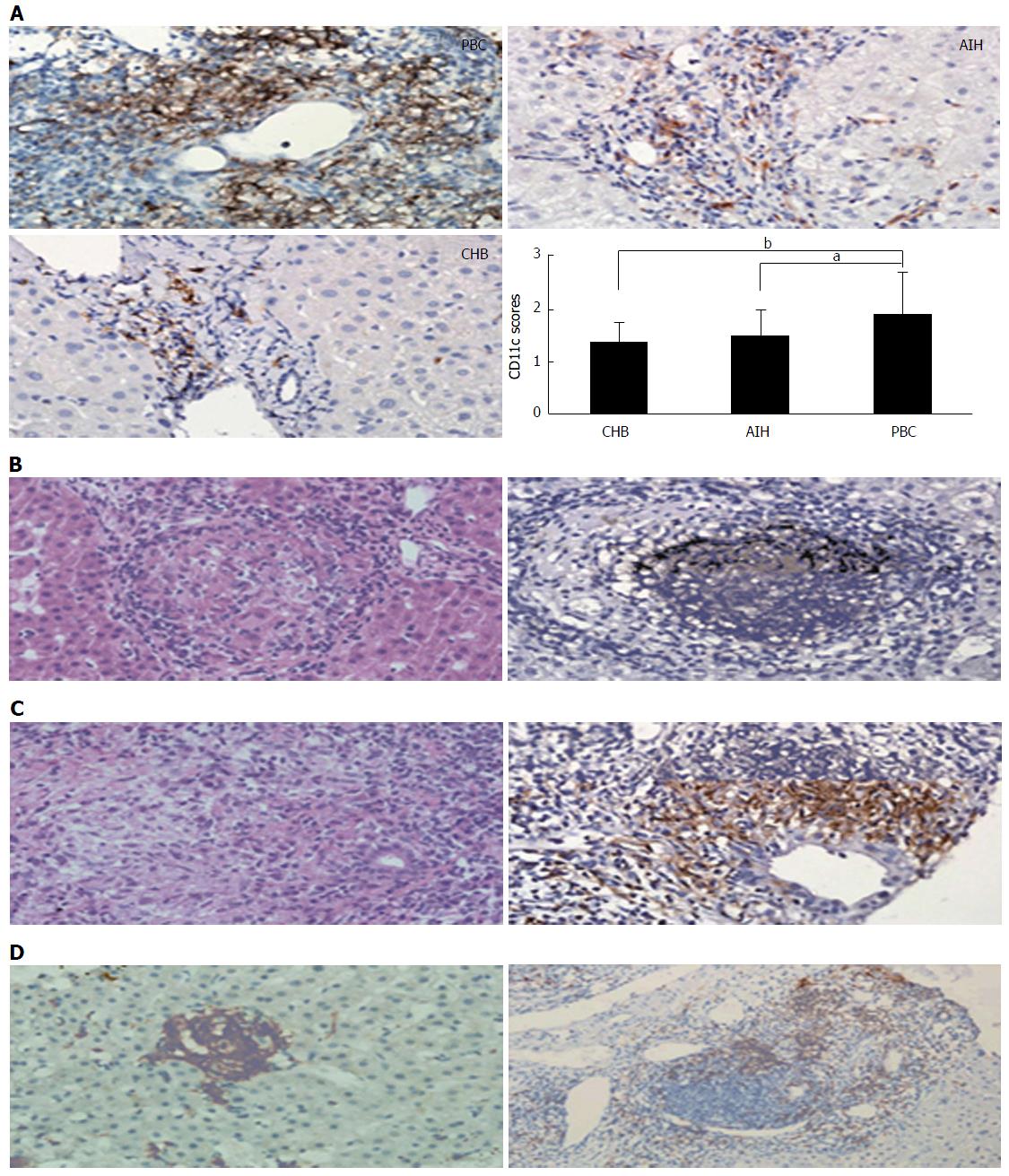
Figure 2 Histology (hematoxylin and eosin staining) and immunochemical staining of primary biliary cholangitis.
A: Magnification × 400; B: Magnification × 400; C, D: Magnification × 400 (left); Magnification × 200 (right). PBC livers demonstrated observably stronger portal area immunostain for CD11c, the position of CD11c sedimentation scored on a 0-4 scale to be compared among PBC, AIH and CHB patients (aP < 0.05, bP < 0.01) (A); PBC hepatic granulomatous lesions were classically situated within portal areas, generally near or around the impaired bile duct (B); Hepatic granulomatous lesions were also occasionally detected in the liver lobule or close to the germinal center (C)[137]. PBC: Primary biliary cholangitis; AIH: Autoimmune hepatitides; CHB: Chronic hepatitis B.
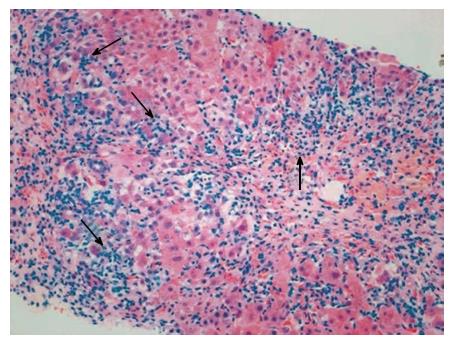
Figure 3 Histology characteristic of autoimmune hepatitis (hematoxylin and eosin staining).
The inflammatory cell infiltration feature of autoimmune hepatitides is composed of leukomonocytes, monocytes/macrophagocytes, and plasmocytes (interface hepatitis, arrows) in the portal and periportal areas[145].
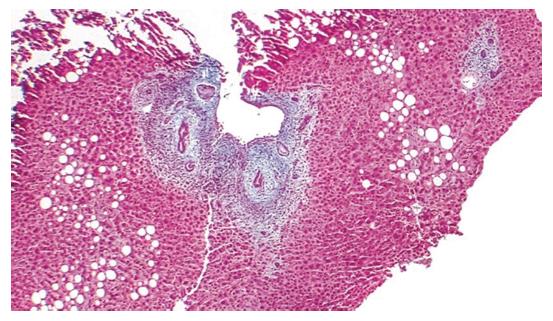
Figure 4 Histology of primary sclerosing cholangitis.
Trichrome × 40, liver biopsy. Low power view demonstrating a focal lesion typical for primary sclerosing cholangitis. Periductular layered fibrosis (featuring “onion skin” pattern) is found with edema and inflammation around the interlobular bile ducts in the center of the field[9].
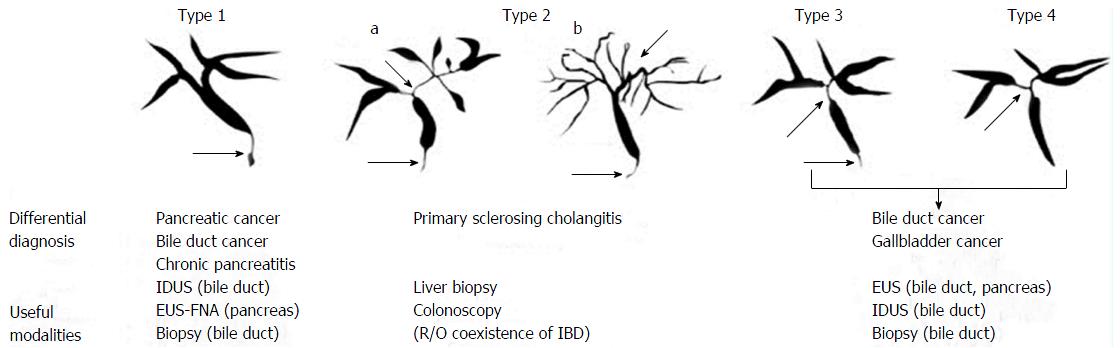
Figure 5 Endoscopic retrograde cholangiography classification of IgG4-SC and anti-diastole.
Stricture is distributed only in the distal choledoch in type 1; stricture is widely spread throughout in the intrahepatic and extrahepatic biliary ducts in type 2. Type 2 is once more divided into two. Expanded stenosis of the intrahepatic biliary ducts in the presence of pre-stenotic expansion is diffusely spread all over in type 2a. Stenosis of the intrahepatic biliary ducts in the absence of pre-stenotic expansion and decreased biliary tree are diffusely spread throughout in type 2b; stricture is found in both porta hepatis damage and the distal choledoch in type 3; stenosis of the biliary ducts are found only in the porta hepatis damage in type 4. IDUS: Intraductal ultra-sonography; EUS-FNA: Endoscopic ultrasonography-guided fine-needle aspiration[152]; IBD: Inflammatory bowel disease.
- Citation: Huang YQ. Recent advances in the diagnosis and treatment of primary biliary cholangitis. World J Hepatol 2016; 8(33): 1419-1441
- URL: https://www.wjgnet.com/1948-5182/full/v8/i33/1419.htm
- DOI: https://dx.doi.org/10.4254/wjh.v8.i33.1419