Published online May 14, 2018. doi: 10.3748/wjg.v24.i18.1925
Peer-review started: March 28, 2018
First decision: April 19, 2018
Revised: April 27, 2018
Accepted: May 6, 2018
Article in press: May 6, 2018
Published online: May 14, 2018
Processing time: 44 Days and 16.9 Hours
Gastrointestinal stromal tumors (GISTs) are the most common mesenchymal tumors located in the alimentary tract. Its usual manifestation is gastrointestinal bleeding. However, small asymptomatic lesions are frequently detected as incidental finding. Characteristically, most GISTs (> 95%) are positive for the KIT protein (CD117) by IHC staining and approximately 80%-90% of GISTs carry a mutation in the c-KIT or PDGFRA genes. Mutational analysis should be performed when planning adjuvant and neoadjuvant therapy, due to its possible resistance to conventional treatment. The arise of tyrosine kinase inhibitor has supposed a revolution in GISTs treatment being useful as adjuvant, neoadjuvant or recurrence disease treatment. That is why a multidisciplinary approach to this disease is required. The correct characterization of the tumor at diagnosis (the diagnosis of recurrences and the evaluation of the response to treatment with tyrosine kinase inhibitors) is fundamental for facing these tumors and requires specialized Endoscopist, Radiologists and Nuclear Medicine Physician. Surgery is the only potentially curative treatment for suspected resectable GIST. In the case of high risk GISTs, surgery plus adjuvant Imatinib-Mesylate for 3 years is the standard treatment. Neoadjuvant imatinib-mesylate should be considered to shrink the tumor in case of locally advanced primary or recurrence disease, unresectable or potentially resectable metastasic tumors, and potentially resectable disease in complex anatomic locations to decrease the related morbidity. In the case of Metastatic GIST under Neoadjuvant treatment, when there are complete response, stable disease or limited disease progression, complete cytoreductive surgery could be a therapeutic option if feasible.
Core tip: The treatment of gastrointestinal stromal tumors with tyrosine kinase inhibitors represents the paradigm of the new era of molecular targeted therapy against cancer. During the last years, there have been improvements in the control of this disease and in the prognosis of these patients, deriving in hopeful perspectives in the management of these tumors partly thanks to the numerous specialists. In this work, we define the role of each specialist in the different clinical scenarios.
- Citation: Sanchez-Hidalgo JM, Duran-Martinez M, Molero-Payan R, Rufian-Peña S, Arjona-Sanchez A, Casado-Adam A, Cosano-Alvarez A, Briceño-Delgado J. Gastrointestinal stromal tumors: A multidisciplinary challenge. World J Gastroenterol 2018; 24(18): 1925-1941
- URL: https://www.wjgnet.com/1007-9327/full/v24/i18/1925.htm
- DOI: https://dx.doi.org/10.3748/wjg.v24.i18.1925
Gastrointestinal stromal tumors (GIST) are the most common mesenchymal tumor located in the gastrointestinal (GI) tract. Most studies have reported the incidence of clinically relevant GIST between 10 and 15 cases per million; however, it is common to detect small asymptomatic lesions as incidental findings during abdominal surgery or in radiological or endoscopic studies, so GIST cases are often misdiagnosed[1,2].
The majority of studies have reported an increase in incidence since 2000; nevertheless, this may be a consequence of improvements in diagnostic criteria rather than a true increase in incidence[3].
GISTs are more often located in the stomach (56%) followed by small bowel (32%), colorectum (6%), and esophagus (< 1%). Sporadically, it may affect the omentum, mesentery, and peritoneum[4]. Liver and peritoneum are the most common locations for distant metastases where they appear up to 47% at the time of diagnosis[5]. Pulmonary metastases, which are highly frequent in soft tissue sarcomas, are uncommon in the case of GISTs.
Interstitial cells of Cajal (ICCs) are recognized as the precursor cells of GISTs being implicated in the regulation of gut peristalsis. They are considered the pacemaker cells of the gastrointestinal tract and are immunostained by antibodies against CD117 (KIT) like GISTs[6,7]. ICCs are located between the layers of the muscularis propria in the interface between the autonomic innervation of the gastrointestinal wall and the smooth muscle, having immunophenotypic and ultrastructural features of smooth muscle and neuronal differentiation[8].
Characteristically, most GISTs (> 95%) are positive for KIT (CD117) protein staining. Approximately 80%-90% of GISTs carry a mutation in the c-KIT gene (80%) or platelet-derived growth factor receptor alpha (PDGFRA) gene, which code for type III receptor tyrosine kinases[9].
Traditionally, GIST tumors have been characterized by their resistance to conventional chemotherapy and radiotherapy treatments. Nevertheless, in 2002, the appearance of the tyrosine kinase inhibitor, Imatinib-Mesylate, was the first to be used to treat metastatic disease and currently has been introduced as an adjuvant or neoadjuvant. This drug was suggested to revolutionize treatment of these tumors that normally requires a multidisciplinary approach, which involves numerous specialists such as physicians, endoscopist, surgeons, radiologists, oncologists, nuclear medicine physicians, or pathologists[10].
A high proportion of GISTs are asymptomatic, and frequently, they are discovered incidentally during an endoscopic study (It is common to notice the presence of a sub epithelial mass) or on radiological images obtained for another purpose. Incidental finding can cause a significant diagnostic delay. Currently, a significant number of patients presents with metastases at the time of diagnosis (up to 50% in some series)[5]. It is essential that physicians include GISTs in differential diagnosis due to the importance of early diagnosis in these cases.
Clinical manifestations depend on the location of the primary tumor. There is no difference between gender and mean age reported is approximately 60-70 years old[1,11].
Usually, these tumors are associated with nonspecific symptoms (early satiety, swelling) unless they ulcerate, bleed or grow enough to cause pain, obstruct, or present other manifestations related to their disproportionate size[12,13]. In the case of esophageal GIST, dysphagia represents the first specific symptom in this location[14].
In general terms, the most frequent manifestation is gastrointestinal bleeding, either evident or hidden, which may be associated with anemia and sometimes melena or hematemesis[15]; bleeding is the most frequent symptom in case of small intestine GISTs and often require urgent surgical intervention[16]. Because their silent growth tumors may be particularly large causing abdominal distention or a palpable mass and sometimes provoking intestinal obstruction (25%-40%); however, intestinal perforation has rarely been described[16,17].
Paraneoplastic syndromes are unusual in case of GISTs; however, some have been reported as consumptive hypothyroidism or hypoglycemia secondary to IGF-II production, so they should be included in the differential diagnosis when endocrine-metabolic symptoms appear[18,19].
Patients with multifocal disease are generally classified as advanced (metastatic) stage, but it should be taken into account, particularly in those cases with hereditary conditions, that multiple primaries may be possible[20].
In adults, GIST tumors have been associated with multiples syndromes as neurofibromatosis type 1 (NF1), Carney Triad syndrome and Carney Stratakis syndrome; GISTs associated with NF1 usually appear in the gastrointestinal tract and are usually multicentric. In these tumors, the KIT mutation is not characteristic, and they are usually positive for the CD117 antigen[21]; on the other hand, Carney’s triad consists of epithelioid GISTs is associated with extra-adrenal paraganglioma and pulmonary chondroma. It lacks the conventional KIT and PDGFRA gene mutations and tends to present an indolent course[22]; the Carney Stratakis syndrome is extremely rare and is similar to Carney’s Triad syndrome but lacks pulmonary chondroma and follows a benign course. Mutations have been identified in KIT or PDGFRA. The tumors are generally small, lack mitotic activity and arise in interstitial cells of Cajal[23].
Pediatric GISTs are assumed to be 1%-2% of all GISTs. Two subgroups exist: (1) with mutations (KIT or PDGFRA) or (2) without mutations (the most frequent). The patients are almost exclusively young women who develop gastric epithelioid GISTs, which are KIT types. Unlike adult GISTs, these tumors can spread to lymph nodes[24,25].
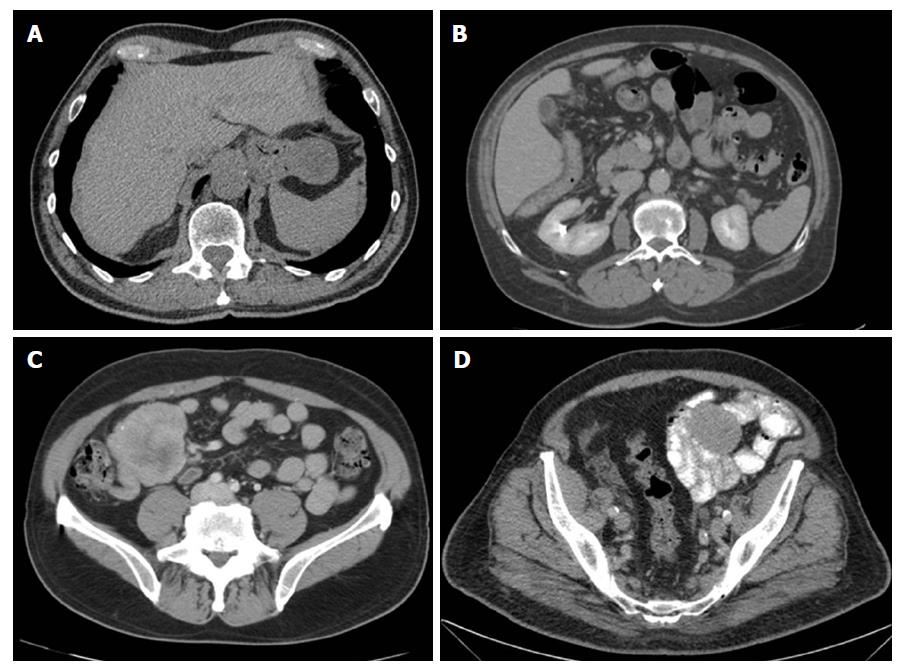
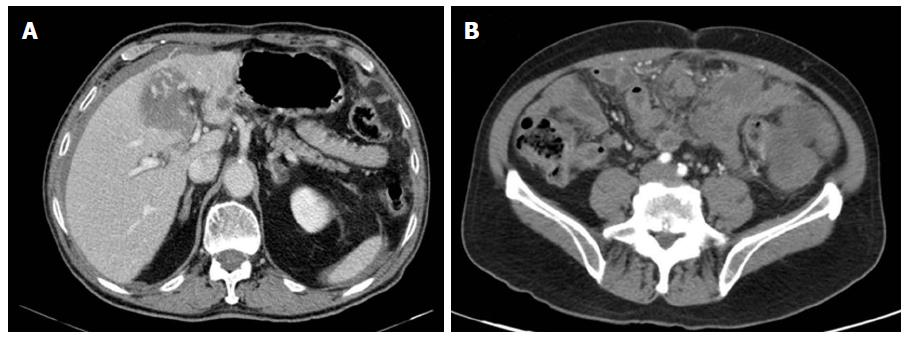
Computed tomography (CT) is the gold standard for imaging that is used to characterize any abdominal mass in addition to assessing its extent and the presence/absence of disease at a distance (GIST metastasize more frequently to the liver, omentum, and peritoneal cavity). Therefore, with suspicion of a tumor in the digestive tract, as in the case in question, an initial CT scan should be done. It should be noted that for the optimal performance of CT, oral and intravenous contrast should be administered in order to define the intestinal margins[26,27] (See Figures 1 and 2).
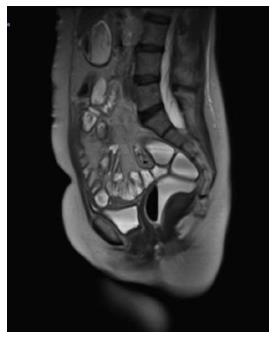
Magnetic resonance imaging (MRI) has a diagnostic performance comparable to CT and the advantage of lacking ionizing radiation; however, CT is the preferred initial imaging study for screening and staging of the disease. There are exceptions to this process; for example, there are patients who cannot receive intravenous contrast for various reasons (allergies, IR). In addition, MRI can sometimes be the choice for GISTs found in specific locations (such as the rectum) and is especially useful for evaluating the anatomical degree of surgery or for evaluating the suspicion of liver metastases[26] (See Figure 3).
The usual characteristic images seen on these images include the presence of a solid mass with a soft contour that is enhanced with intravenous contrast in the case of CT[28]. Very large tumors may appear more complex due to necrosis, haemorrhage, or degenerative components, and it may be difficult to identify the origin of a large mass due to exophytic growth[27].
With regard to the evaluation of response to treatment, patients are routinely subject to CT, and two-dimensional measurements are used to determine response, stability, or progression.
During neoadjuvant and adjuvant treatment, radiologists are mainly involved in the evaluation of the response to treatment with tyrosine kinase inhibitors (TKI). On the one hand, Response Criteria in Solid Tumors (RECIST) is the standard method used to measure the way in which a cancer patient responds to treatment. In order to apply the RECIST criteria, it is necessary to first identify representative and reproducible target lesions during follow-up; it should be taken into account that its great variability (fragmentation, poor definition, imaging technique, appreciation) in addition to the difficulty in measuring them, as occurs in mobile organs, cause intra-observer and inter-observer discrepancies. Assessments of the response will be made with the same technique used in the initial study, stating the duration of the response. The sum of the target lesions in the baseline study can be used to objectively monitor and assess the response. When a target lesion fragments during treatment, its parts will be measured, added up, and considered as a single lesion. The RECIST criteria are a series of published rules to establish the response to treatments and indicate when cancer patients improve (“respond”), stay the same (“stable”), or get worse (“disease progression[29,30].
In the other hand, the Choi Criteria[31] are useful in the evaluation of imatinib treatment of GISTs. In this case, the most characteristic feature is a decrease in the density of lesions associated with myxoid degeneration, hemorrhage, or necrosis. These criteria, based on CT studies, include tumor size, its density, and the appearance of intratumoral hypervascular nodules. They present a high correlation between the results obtained in CT and positron emission tomography (PET). CT should be performed in arterial phases (to see changes in vascularization and uptake) and portal (to measure tumor density)[32].
As described previously, GISTs usually manifest as gastrointestinal bleeding. Transcatheter arterial embolization has proven to be a safe option for controlling gastrointestinal bleeding, thus preventing emergency surgery that would probably allow a more accurate diagnosis to be made and the best possible surgical plan to be executed[33].
Traditionally, preoperative percutaneous biopsy has not been used due to the possibility of tumor rupture or peritoneal spread of disease[8]. There are data supporting the finding that it may not increase the risk for GIST recurrence in those patients who receive adjuvant Imatinib after the biopsy was obtained. Percutaneous biopsy should be considered when it is necessary to plan preoperative treatment with TKI and endoscopic biopsy is not feasible[17,34].
In the case of patients with unresectable liver metastases, some local interventional modalities, such as transarterial embolization or radiofrequency ablation may be used; however, further studies are necessary to evaluate its effectiveness as adjuvant therapy or combined with TKI[35-37].
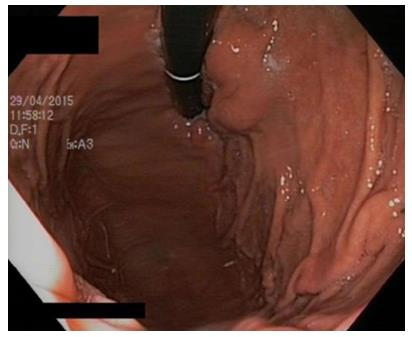
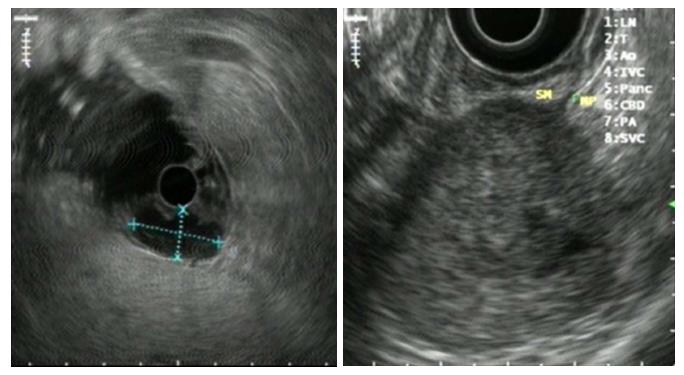
In the presence of a gastric mass, endoscopy is indicated to characterize the lesion. GISTs and leiomyomas may appear as a submucosal mass with smooth margins and a normal overlying mucosa that protrudes in the gastric lumen, but sometimes, a central ulceration may be observed[38] (See Figure 4).
Simple endoscopy lacks the ability to accurately distinguish between intramural and extramural tumors. In this sense, Endoscopic Ultrasonography (EUS) has proved to be a valuable technique, being able to characterize such masses by identifying the layer of origin and allowing for acquisition of tissue by a guided puncture for anatomopathological diagnostic studies, which is suitable for immunohistochemical tests[39,40]. Standard endoscopic biopsies generally do not obtain enough tissue for a definitive diagnosis, and loop biopsies can cause a perforation and should generally be avoided[34].
Most GISTs originate within the muscularis propria although small lesions may originate in the muscularis mucosae. By EUS, GISTs are typically hypoechoic and present as homogeneous lesions with well-defined margins although there are a small number of described tumor cases of tumors that may have irregular margins and ulcerations (See Figure 5). Ultrasound (US)-guided biopsy forceps may also not obtain enough tissue, but its main utility is to exclude other lesions arising from the submucosa[39].
Preoperative biopsy is not generally recommended for a resectable lesion if there is high clinical and radiological suspicion of GIST, and the lesion is completely resectable. However, a preoperative biopsy is preferred to confirm the diagnosis if metastatic disease is suspected, if the neoadjuvant Imatinib is considered, or in cases in which there exists high operative morbidity or the diagnosis is not clear.
If a preoperative biopsy is performed, an US-guided biopsy is preferred to a percutaneous biopsy because of the risk of tumor capsule rupture and consequent peritoneal dissemination[34].
The combined use of cytological analysis and immunohistochemistry for KIT protein detection and expression and polymerase chain reaction (PCR) to detect KIT mutations allow the diagnosis of most of these lesions obtained by EUS - fine- needle aspiration Biopsy (FNAB). In a study of 65 patients undergoing EUS-FNAB for a submucosal lesion of the upper GI tract, among the 28 lesions with a definitive pathological diagnosis, the sensitivity for the diagnosis of GIST was 82% and the specificity 100%[41].
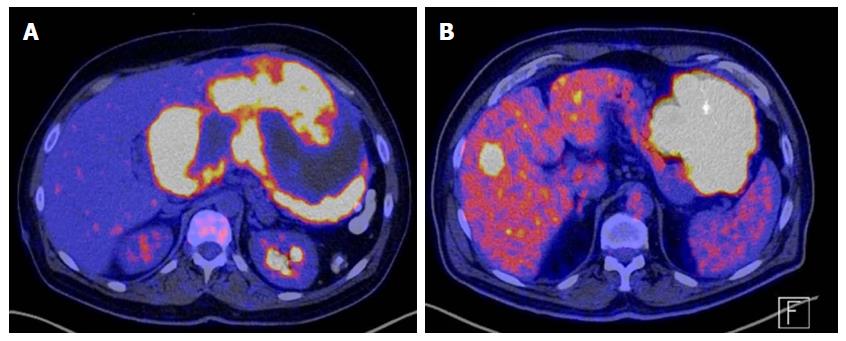
PET with fluorodeoxyglucose (FDG-PET) is highly sensitive detection of very metabolically active tumors resulting from a significant glycolysis (See Figure 6); however, this test is not considered to be specific enough to obtain a preoperative diagnostic, so it has not replaced CT as the initial imaging modality of choice in patients suspected of having a mesenchymal tumor in the GI tract. FDG-PET may be useful for detecting an unknown primary site or resolving ambiguities on the CT (inconclusive CT findings or inconsistent with clinical findings)[42]. The reported sensitivity of PET for GIST (including metastatic lesions) is 86%-100%[43].
The FDG-PET response, which is characterized by a mark in the glycolytic metabolism of tumors, may be seen one month after starting treatment with Imatinib-Mesylate and an early response may be seen in the first 24 h[44]. FDG-PET may detect an early response to a tyrosine kinase inhibitor, which may be important when the treatment is administered and would allow identification of patients with primary resistance to treatment or even identify secondary resistance in the case of patients already treated with Imatinib-Mesylate[45].
Surgery is the only potentially curative treatment for suspected resectable GIST. The primary objective of this process is to ensure that clear resection margins are obtained in a complete resection of the tumor, and it can be extirpated without tumor pseudocapsule rupture; nevertheless wide margins have no benefit in disease control[5]. Conservative surgery must be the procedure of choice due to local GIST infiltrative behavior; lymphadenectomy is not necessary due to lymphatic affectation, which is rare[46]. A thorough exploration of the liver and parietal peritoneum is important in order to objectify possible metastases.
At least 40%-50% of patients who have undergone optimal surgery may experience a tumor recurrence; however, with the appearance of TKI, a new option disease control has been offered[47,48] (See Figure 1).
The management of GISTs < 2 cm is controversial; in spite of the fact that an active follow-up of the lesion could be an option, surgery should be considered because there is no data concerning growth behavior and metastasic potential[49,50].
In the case of gastric GISTs, which is the most common location, wedge resections are preferred to classic gastrectomies[51]. Currently, there are multiple studies comparing laparoscopic wedge resection for gastric GISTs versus open surgery showing multiple benefits that patients could obtain resulting from this less invasive approach as reducing postoperative discomfort or shortening the length of postoperative hospital stay. In this sense, laparoscopy wedge resection is considerate the standard treatment for gastric GIST[52-55]. In a multi-institutional analysis performed by Bischof et al[56], minimally invasive surgery for gastric GIST was shown to reduce length of the hospital stay, blood loss, and morbidity with same R0 and tumor rupture rates. The main limitation to laparoscopy resection is technical difficulty due to tumor size and location; nevertheless, multiple studies have demonstrated that laparoscopy wedge resection for gastric GISTs > 5 cm is feasible[54,57,58].
Incidental GIST finding in bariatric surgery is rare with a reported incidence between 0.3%-1.2% in different series of sleeve gastrectomy and gastric bypass[59-61]. In many cases, the performed procedure may be curative; however, the finding of GISTs in certain locations such as the gastroesophogeal junction or lesser curve could require abandoning the proposed technique in favor of a suitable and complete tumor excision[59].
For patients who have primary localized small bowel GIST, segmental bowel resection remains the first choice of treatment. Emergent resections are more often needed in patients diagnosed with small bowel stromal tumors secondary to hemorrhage, obstruction, or perforation[62]. Laparoscopic segmental resection with intra- or extracorporeal anastamoses, when possible, is the elective approach achieving comparable oncologic results[63-65]. Tabrizian et al[66] reported that in their series, laparoscopic removal of tumors up to 85 mm shows low rates of morbidity (10%), mortality (1.3%), and conversion (19%); the main reason for conversion was the tumor’s proximity to the gastroesophageal junction, local invasion of adjacent organs, association with another malignant lesion, preoperative tumor perforation, extensive adhesions, and large tumor size[66].
In spite of the fact that the colon is an uncommon location for GISTs, patients with tumors in this location present a much poorer prognosis with a higher rate of disease-specific mortality and a higher percentage of patients with distant disease[67,68].
Due to intrinsic characteristics of GIST tumors, a wide resection is not required and segmental colectomy is the standard approach; Moreover, as previously mentioned, GIST does not metastasize through lymphatics thus mesocolic resection is unnecessary[69].
In cases of potentially resectable disease that are located in complex anatomic locations and require extensive organ disruption, neoadjuvant therapy with Imatinib has been proposed to downstage tumors and facilitates complete resection or decrease the morbidity of resection[67].
Esophagus: Esophageal location of a GIST is infrequent[16]. Robb et al[14] proposed that enucleation of the tumor is safe for esophageal GISTs < 65 mm as long as negative margins and intact pseudocapsule can be achieved, while in tumors of > 90 mm with evidence of mucosal ulceration and/or a high mitotic activity, an esophagectomy should be performed. The choice between esophagectomy and enucleation for tumors of between 65 and 90 mm needs further clarification with the decision being influenced by the location, malignant risk, patient comorbidity, and the presence of mucosal affectation[14,70]. Neoadjuvant therapy is indicated with the aim of shrinking the primary tumor[70].
Duodenum: GISTs located in duodenum are rarely observed and often manifest as nonspecific abdominal pain, gastrointestinal hemorrhaging, and intestinal obstruction may infrequently have been observed[71,72].
When possible, limited resection should be the procedure of choice; nonetheless, due to peculiar anatomic location because of proximity of the pancreatic head and papilla of Vater and the difficulties to get an adequate section margin, Pancreaticoduodenectomy is often necessary[73]. In the meta-analysis accomplished by Chok et al[74], it was appreciated an increase of positive margins in case of Limited resection, although there was no significant difference in local recurrence between Limited Resection and Pancreaticoduodenectomy.
Neoadjuvant treatment with TKI has been proposed to downstage GISTs, and possibly increases the chance of preserving normal biliary and pancreatic anatomy which would otherwise require more aggressive surgery[74,75].
Rectum: Outcomes in colonic or rectal locations appear to be worse than those located in the stomach[67]. Rectal GIST may require an abdominoperineal amputation to achieve a surgically complete resection. To avoid an extensive and limiting surgery, neoadjuvant Imatinib-Mesylate should be considered to reduce tumor size and facilitate complete surgical resection by increasing negative margins and less radical sphincter-sparing surgery[76,77]. Laparoscopic sphincter-preserving surgery is safe and feasible after neoadjuvant treatment of Imatynib Mesylate[78]. Mesorectal resection for rectal GISTs is not required due to the absence of lymphatic dissemination. Transanal endoscopic surgery has been employed for local treatment of low rectal GISTs with no evidence of recurrence after an 18-mo follow-up[79].
Most studies define locally advanced primary GIST as the significant involvement of a single organ with large tumor size or extension of the tumor to adjacent organs[80]. Neoadjuvant use of imatinib has been demonstrated to be useful in primary locally advanced GISTs by causing a decrease in tumor volume in the majority of the patients. Tumor response may facilitate complete resection of these advanced tumors and could allow less invasive procedures without tumor rupture[10,16,81].
Metastases may be detected at first presentation or at the time of disease progression. The first line of treatment for patients with metastatic or recurrent GISTs are TKI in the form of neoadjuvant or adjuvant therapy with the choice of treatment being Imatinib-mesylate[82]. The appropriate time for surgical intervention is still unknown. It is proposed to consider surgery if a complete cytoreductive resection is feasible after six to nine months with a tyrosine kinase inhibitor.
After treatment with TKI, there are three possible radiological response of the disease[83]: (1) Complete response: Non metabolic activity in PET; Disappearance of disease in CT; Infrequent clinical situation. (2) Partial response or responding to drug therapy; Decrease of metabolic activity in PET and/or decrease of size in CT. (3) Stable disease: Disease is radiographically (CT, PET) stable. (4) Limited/localized disease progression: Progression in spite of drug therapy is seen at one or a few (but not all) sites of disease. Patients with Partial response, stable disease or limited/localized disease progression could undergo cytoreductive surgery. And (5) Generalized disease progression: In this case, disease is progressing at multiple sites while on drug therapy. Debulking surgery does not seem to prolong survival so cytoreductive surgery is not recommended.
Peritoneal GIST metastases may be detected, especially in cases in which the primary tumor ruptured spontaneously or surgically. When disease progression occurs due to Imatinib resistance and GISTs relapse loco-regionally after surgical resection or disease disseminates to peritoneum, prognosis is poor and standard treatments such as conventional surgery, radiotherapy ,and systemic chemotherapy are generally ineffective[84].
Imatinib-Mesylate and Sunitib-Malate (used in cases in which GIST develops resistance to Imatinib) have been shown to increase disease control and survival rates; nevertheless, although patients experience durable periods of disease stability to Imatinib lasting months to years, the response is not maintained indefinitely[85].
Aggressive surgical procedures to treat loco-regional relapse and peritoneal metastases have been proposed. These cytoreductive strategies involve peritonectomy procedures and multivisceral resection to remove all macroscopic tumor(s)[84]. Cytoreductive surgery has been shown to increase progression-free survival and overall survival rates in patients with metastatic GIST who are receiving Imatinib Mesylate therapy. Patients with stable disease or responsiveness to Imatinib Mesylate had demonstrated an increase in survival rates compared to those with disease progression[81,85-87].
Sugarbaker[84] proposes the complete resection of recurrent sarcomas using peritonectomy and visceral resections to complete cytoreduction of disease and perioperative intraperitoneal chemotherapy. The randomized trial performed by Bonvalot et al[88] in 2005 demonstrate the importance of the positive impact of complete cytoreductive surgery; however, the use of intraperitoneal chemotherapy didn’t increase greatly overall survival of sarcomatosis. Cytoreductive Surgery combined with perioperative intraperitoneal chemotherapy is a promising future approach to sarcomatosis, awaiting new chemotherapy agents.
After the surgical excision of GISTs metastases, it is necessary to continue treatment with TKI[85].
GIST metastases are often located in liver and may appear as primary disease or as a recurrence after surgery. In cases of metastatic GIST in which stable disease or localized disease progression exists, hepatic resection is the mainstay of treatment for liver metastasis[83].
In DeMatteo et al[89] 56 patients with liver metastasis who underwent complete resection of all gross disease had significantly longer survival (1-,3-,5-year disease-specific survival rate was 88%, 50%, and 30%, respectively) than those 275 patients who did not undergo complete resection (1-, 3-, and 5-year disease-specific survival rates of 50%, 13%, and 4%, respectively). Completing surgical treatment with Imatinib Mesylate showed an increase in disease-free and overall survival[37,90].
There exist few references in the literature concerning liver transplantation in patients with metastatic sarcoma showing uninspiring results[91,92].
The use of TKI against GIST introduced a new era in molecular-targeted therapies in clinical oncology. The oncologist plays a major role in GIST treatment for carrying out the indication for the TKI for metastatic tumors after a curative surgery or as a neoadjuvant treatment (See Figure 1).
Almost 85% of GISTs have a mutation in KIT or PDGFRA that induces an KIT activation, which is a tyrosine kinase receptor that stimulates the growth of cancer cells. Mutational analysis is acquiring a growing importance and should be performed when adjuvant and/or neoadjuvant therapy show possible mutations with a tendency toward Imatinib Mesylate-resistance[17]. Tyrosine kinase inhibitor selection based on gene mutations is described in Table 1.
| Gene | Mutation | TKI. Dose |
| KIT | Exon 11 | Imatinib-Mesylate 400 mg/d |
| Exon 13 | ||
| Exon 17 | ||
| Exon 9 | Imatinib-Mesylate 800 mg/d | |
| PDGFRA | Exon 18. D842V mutation | Sunitinib 50 mg/d |
| Regorafenib 160 mg/d | ||
| Exon 12 | Imatinib-Mesylate 400 mg/d | |
| Exon 14 | ||
| Exon 18. Non D842V mutations. | ||
| Wild-type | Sunitinib 50 mg/d | |
| Regorafenib 160 mg/d |
KIT gene mutations (80%): KIT exon 11 is the most common mutation and may be observed in approximately 75% of all mutation-positive tumors primarily affecting codons 557-559. These mutations are most commonly observed in gastric GIST. In the Z9001 trial, patients with exon 11 mutation proved to experience greater benefits from adjuvant Imatinib with higher rates of relapse-free survival although these mutations indicate poorer prognosis and high metastatic risk[17,93,94]. Exon 9 mutations (approximately 10%) are associated with poor Imatinib response. Mutations in exons 8, 13, and 17 are infrequent and seem to be < 3%[24].
PDGFRA gene mutations (5%-8%): GISTs with PDGFRA mutations are regularly located in stomach[17]. The D842V mutation in PDGFRA exon 18 is the most common mutation found (65%-75% of PDGFRA mutations)[94]; this mutation is associated with Imatinib and Sunitinib resistance[95,96]. Non-D842V exon 18, 12, and 14 mutations are rare and sensitive to Imatinib.
Wild-type GISTs (12%-15%; 90% of pediatric GISTs): In these cases, there are no detectable mutations in KIT or PDGFRA genes that are resistant to treatment with Imatinib although tyrosine kinases are still activated. Wild-type GISTs represent a heterogeneous group that includes several oncogenic mutations such as BRAF V600E substitution, NF1 mutation, and defects in the succinate dehydrogenase complex[97-99]. Second line TKI are recommended despite poor response by these tumors.
KIT-negative GISTs (CD117-negative): Approximately 5% of GISTs do not express CD117 by immunoreactivity but 30%-50% of cases have KIT or PDGFRA mutations[100].
When patients present primary or secondary resistance to Imatinib, second-line treatment with Sunitinib and third-line treatment with Regorafenib are recommended.
In spite of performing a complete resection of the tumor without tumor rupture and appearance of negative margins, GISTs still have some malignant potential and may recur or metastasize. It is necessary to identify those patients who may derive benefits from the adjuvant Imatinib-Mesylate because of their high risk of recurrence or metastases following resection. Several risk stratification models have been proposed to estimate the risk of recurrence and identify high risk GISTs after resection, so the indication of adjuvant Imatinib can be individualized. In multiples models, the main predictors of recurrence established were tumor mitotic rate, size, and location[47,101]. Increased tumor size, high mitotic activity, or extragastric location such as small bowel, colon, rectum, or mesentery is associated with an increased risk of poor outcomes. The oldest risk stratification model is the consensus from the National Institutes of Health (NIH) which stratifies risk on the basis of tumor size and mitotic count and has demonstrated its usefulness in predicting GIST behavior[8,102]. On the other hand, Miettinen et al[103] emphasized the importance of location to the risk of recurrence. The revised NIH consensus criteria by Joensuu et al[104] in 2008 included the presence of either spontaneous tumor rupture or that occurring, which worsens the prognosis and location because of the better prognosis of gastric location versus extra gastric GISTs (Table 2)[105]. Incomplete resection has demonstrated to adversely affect overall survival (OS)[106].
| Risk category | Tumour size (cm) | Mitotic index (per 50 HPF) | Primary tumour site |
| Very low risk | ≤ 2.0 | ≤ 5 | Any |
| Low risk | 2.1-5.0 | ≤ 5 | Any |
| Intermediate risk | ≤ 5.0 | 6-10 | Gastric |
| 5.1-10.0 | ≤ 5 | Gastric | |
| High risk | Any | Any | Tumour rupture |
| > 10.0 | Any | Any | |
| Any | > 10 | Any | |
| > 5.0 | > 5 | Any | |
| ≤ 5.0 | > 5 | Non-gastric | |
| 5.1-10.0 | ≤ 5 | Non-gastric |
In a phase II US Intergroup trial ACOSOG Z9000[107], 106 patients with resected high-risk GIST were included. High risk was defined as tumors >10 cm, evidence of capsular rupture, hemorrhage, or multifocal disease with > 5 tumor foci. Patients were treated after a complete resection with daily oral 400 mg Imatinib for one year. The primary endpoint was OS with 1-, 2-, and 3-year OS of 99%, 97%, and 83%, respectively. One-, 2-, and 3-year recurrence-free survival was 96%, 60%, and 40%, respectively.
In the ACOSOG Z9001 randomized phase III multicenter trial, 713 patients with complete gross resection of a primary GIST at least 3 cm in size and showing positive staining for KIT protein were randomly assigned to one year of adjuvant Imatinib (400 mg daily) or placebo[108]. Primary endpoint was recurrence-free survival (RFS). Imatinib was shown to increase RFS compared with placebo (98% versus 83% at one year; hazard ratio [HR] 0.35; P < 0.0001). Although no differences in the case of OS (99.2% vs 99.7% at one year; HR 0.66; P = 0.47), it was considered justified because of short follow-up time and the crossover study design, which allowed patients with tumor recurrence assigned to the placebo arm to receive Imatinib-Mesylate. In this study, patients with exon 11 mutations showed the longest progression-free survival (PFS), while those with an exon 9 mutation had the worst outcomes; however, those patients with exon 9 mutations treated with higher dose of Imatinib showed greater PFS.
In the EORTC 62024 phase III trial[109], 908 patients with intermediate- or high-risk GIST were included and assigned to two years of daily Imatinib 400 mg after complete resection compared to only surgery. The primary endpoint at the origin was OS; however, in 2009, the primary endpoint was changed to Imatinib failure-free survival (IFFS). With a median follow-up of 4.7 years, 5-year IFFS was 87% in those patients treated with Imatinib versus 84% in the control arm (HR = 0.79; 98.5%CI: 0.50-1.25; P = 0.21); RFS was 84% in the Imatinib group vs 66% at 3 years and 69% versus 63% at 5 years (log-rank P < 0.001).
In the Scandinavian Sarcoma Group (SSG) XVIII trial comparing 12 mo vs 36 mo of adjuvant 400 mg/d Imatinib, 400 patients with high-risk complete resected GIST were included. Patients who were treated with 36 months of Imatinib showed an increase in RFS compared with those treated 12 mo (HR = 0.46; 95%CI: 0.32-0.65; P < 0.001). Five-year RFS was 65.6% in the 36-mo group compared to 47.9% in the 12-mo group. Patients treated with 36 mo of Imatinib showed an increase in OS (HR = 0.45; 95%CI: 0.22-0.89; P = 0.02) with 5-year survival of 92.0% versus 81.7% in those patients treated for 12 mo[110]. In the 36-mo group, it was observed that a high number of patients discontinued Imatinib for reasons other than GIST recurrence (25.8% vs 12.6%). In this study, patients with KIT exon 11 deletion mutations benefitted most from the 36 mo of adjuvant Imatinib, while in the other mutational subgroups examined there were no significant benefits[111].
Adjuvant treatment is recommended in those patients who have R0 primary high risk GISTs; however, the optimal indication of adjuvant treatment in high risk patients is not clear, so each case must be approached individually in multidisciplinary specialized committees that balance beneficial and negative impacts. The standard treatment for high risk GIST is adjuvant therapy of 400 mg/d of Imatinib-Mesylate over three years. Two randomized trials comparing prolonged adjuvant therapy with Imatinib-Mesylate versus standard treatment (five versus three years in SSG XXII [NCT02413736] and six versus three years ImadGist [NCT02260505]) exist.
Neoadjuvant Imatinib-Mesylate should be, considered for shrinking the tumor in cases of locally advanced primary or recurrent disease, unresectable or potentially resectable metastasic tumors, and potentially resectable disease in complex anatomic locations to decrease the related morbidity[112]. There is no consensus about duration of the treatment with Imatinib-Mesylate; however, 3-12 mo of treatment with numerous imaging control studies would be an acceptable management[113]. Usually, maximal tumor response occurs after 4 to 12 mo of treatment[114].
Tumors located in complex anatomic locations such as the esophagus, duodenum, or rectum may show a major benefit of initial neoadjuvant treatment to produce less extensive organ disruption interventions[14,78,115].
Preoperative Imatinib has demonstrated to facilitate complete resection of locally advanced primary, recurrent, or metastatic GISTs. In Andtbacka et al[80], a series of 46 patients, who underwent surgery after neoadjuvant Imatinib, was retrospectively reviewed; 35 patients were treated for recurrent or metastatic GIST obtaining a complete resection in 11 patients. This study showed that those patients with a partial radiographic tumor response to neoadjuvant showed significantly higher complete resection rates than patients with progressive disease (91% vs 4%; P < 0.001).
In a study by Bonvalot et al[81], 22 of 180 patients with unresectable GIST treated with neoadjuvant Imatinib (19 received imatinib 400 mg/d and three received 800 mg/d) and no radiographic evidence of overall progression underwent surgery. There were five patients with metastases who underwent emergency surgery due to hemorrhaging and three of them died in the early postoperative period. When surgery was planned, 15 of 17 patients (88%) had a complete resection.
In the study by Chandrajit et al[30], those patients with advanced GISTs under neoadjuvant therapy with Imatinib showing stable disease or limited progression had an increase in OS rates after cytoreductive surgery.
The analysis realized by European Organization for Research and Treatment of Cancer-Soft Tissue and Bone Sarcoma Group (EORTC STBSG), which included databases from 10 EORTC STBSG sarcoma centers, indicated that the largest group of GIST patients (n = 161) were treated with neoadjuvant Imatinib. The most common location was the stomach (55%) followed by rectum (20%), duodenum (10%), ileum/jejunum/other (11%), and esophagus (3%). Median time on therapy with neoadjuvant Imatinib was 40 weeks, and R0 was obtained in 83% of patients. During follow-up, they observed 37 disease recurrences (23%) and only five patients (3%) presented a local relapse with a 5-year DFS rate of 65% (95%CI: 59.1%-70.9%). Five-year OS was 87% (95%CI: 78%-98%), and median OS was 104 mo. Patients who continued with Imatinib after surgery presented better rates of DFS.
In cases of patients with metastasic or recurrent disease under treatment with second-line sunitinib or third-line regorafenib, the role of debulking surgery is still not clear, and there is only a certain amount of information concerning emergency interventions. It is necessary to bear in mind that in these cases the tumors are advanced and resistant to standard treatment, so the potential benefit of the surgery is not known[112].
Pathologic diagnosis has a major impact on GIST management, both at the preoperative time and after complete surgical resection. Data obtained by pathologists need to be stratified according to risk, and prognoses and possible therapies based on primary and acquired secondary resistance to TKI need to be determined.
GISTs in GI tracts are normally found in the subepithelial layer; however, as they become larger, they may cause epithelial ulceration. Currently, GIST’s pathological diagnosis depends on the combination of morphology, immunohistochemistry (CD117 and/or DOG1), and molecular analysis (See Role of Oncologist).
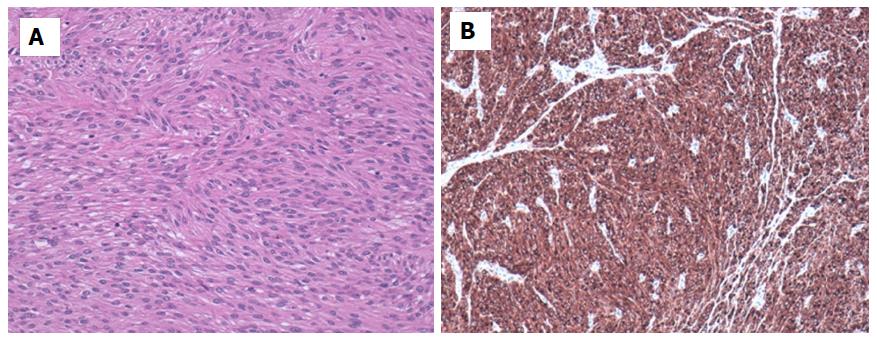
Morphologically, GISTs are subdivided into spindle (70%), epithelioid (20%), and mixed-type cells, but it is considered that cell type influence on the outcome is not relevant[8]. GIST may be divided into eight different subtypes[116]: (1) Spindle cell subtypes: sclerosing, palisading-vacuolated, hypercellular and sarcomatous spindle cell; and (2) Epithelioid cell subtypes: sclerosing, discohesive, hypercellular and epithelioid spindle cell.
The distinction between benign and malignant depends on the presence of nuclear atypia and presence of necrosis, hemorrhaging, and mitotic activity. It is necessary to determine mitotic rate, grade of dedifferentiation, size, location, tumor infiltration, grade of necrosis and hemorrhage, surgical margins, and whether a tumor ruptures because these factors are implicated in the risk of relapse[117]. Ki67 is an important prognostic factor that has been implicated in recurrence and survival and should be included in pathologist’s report[118,119] (See Table 3). The depth of tumor infiltration, including serosal penetration has been proposed as a prognostic factor for patients with GISTs with significantly poorer prognosis compared to its absence[120,121].
| Pathology report items |
| Localization |
| Size |
| Number of foci |
| Tumor infiltration |
| Histologic subtype |
| Depth of tumor infiltration |
| Grade of dedifferentation |
| Mitotic rate |
| Ki67 |
| Grade of necrosis |
| Grade of hemorrhage |
| Margins |
| Staging |
| Mutational study |
Most GIST (> 90%) shows overexpression of the receptor tyrosine kinase KIT (CD117) by immunohistochemistry. On the other hand, a proportion of GISTs (near 5%) which are CD117-negative exists; however, approximately one third of these cases stained with discovered on GIST (DOG)1, which is expressed strongly on GIST and is rarely expressed on other soft tissue tumors[122,123] (See Figure 7). PKC-θ has lower specificity than DOG-1, but it may be a useful biomarker when combined with DOG1. Using both as an important diagnostic tool in the diagnosis of KIT-negative GISTs, even in wild type GISTs may prove useful for diagnosing GIST[124].
GIST’s mutational study is becoming increasingly important. Mutational analyses allow correlations of sensitivity or resistance to molecular-targeted therapies and doses. These types of analyses have prognostic value, so that they play a major role in GIST management[122] (see Role of Oncologist).
The diagnosis of GIST has increased in recent years thanks to new imaging techniques which have increased the interest in the management of this type of tumors.
The clinical diagnosis is based on the CT, EDA and/or endoscopic US and staging diagnosis is obtained by CT and FDG-PET. The histological diagnosis is based on US-guided biopsy or percutaneous biopsy prior to surgery; In case of high suspicion in the imaging tests, surgical resection without previous biopsy would be justified.
The biological behavior of the GIST is explained according to the mitotic index, Ki67, anatomical location, size and mutational status.
Surgical resection with free margins of tumor disease R0 is the only potentially curative therapeutic option.
Therapies with TKI (Imatinib, Sunitinib and Regorafenib) have let a noteworthy improvement in the rates of disease-free survival and overall survival, even in recurrent or unresectable metastatic GISTs.
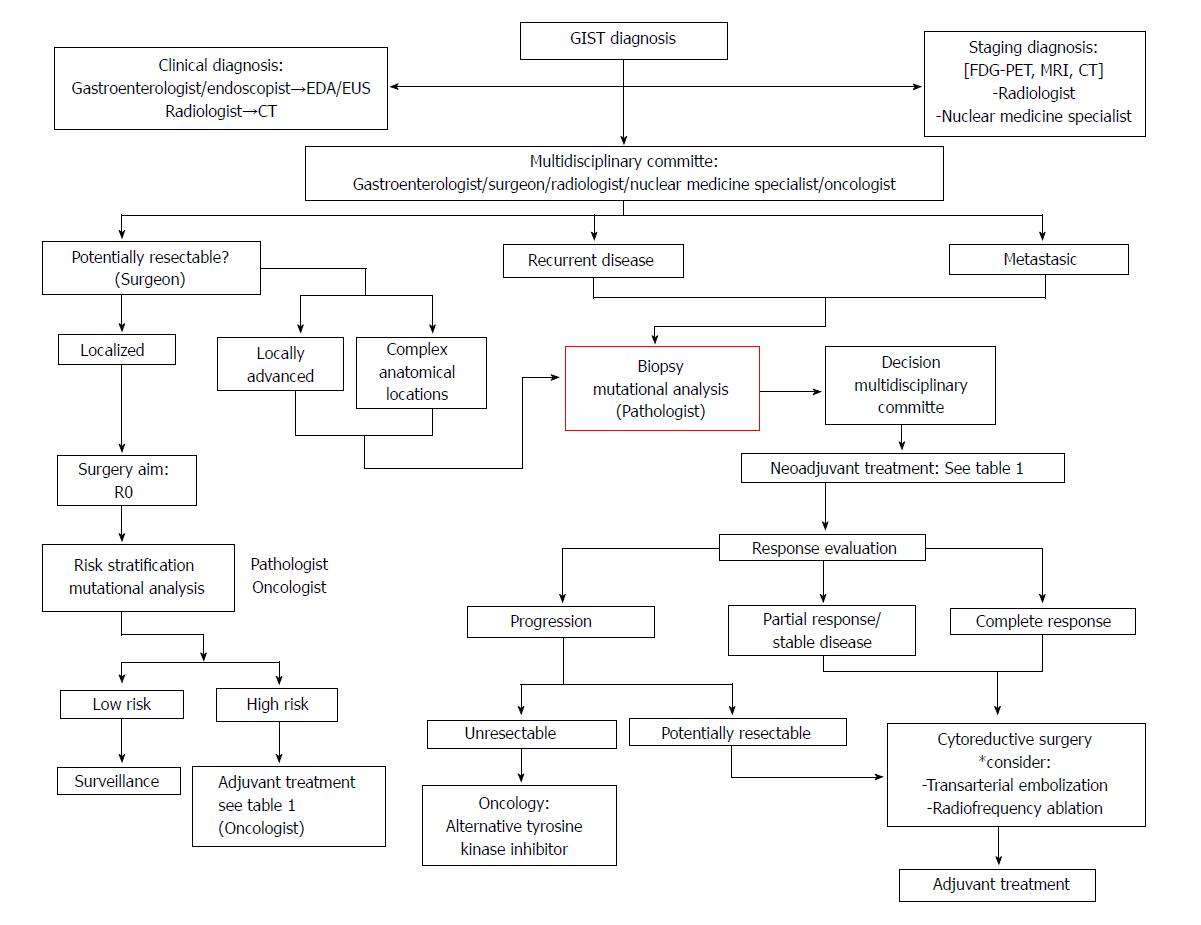
GISTs are the paradigm of a cancer with molecular targeted therapy and its management requires a multidisciplinary approach (See algorithm of management in Figure 8).
Manuscript source: Invited manuscript
Specialty type: Gastroenterology and hepatology
Country of origin: Spain
Peer-review report classification
Grade A (Excellent): 0
Grade B (Very good): B
Grade C (Good): C
Grade D (Fair): 0
Grade E (Poor): 0
P- Reviewer: Guner A, Oymaci E S- Editor: Gong ZM L- Editor: A E- Editor: Huang Y
| 1. | Søreide K, Sandvik OM, Søreide JA, Giljaca V, Jureckova A, Bulusu VR. Global epidemiology of gastrointestinal stromal tumours (GIST): A systematic review of population-based cohort studies. Cancer Epidemiol. 2016;40:39-46. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 579] [Cited by in RCA: 518] [Article Influence: 57.6] [Reference Citation Analysis (1)] |
| 2. | Nilsson B, Bümming P, Meis-Kindblom JM, Odén A, Dortok A, Gustavsson B, Sablinska K, Kindblom LG. Gastrointestinal stromal tumors: the incidence, prevalence, clinical course, and prognostication in the preimatinib mesylate era--a population-based study in western Sweden. Cancer. 2005;103:821-829. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 803] [Cited by in RCA: 874] [Article Influence: 43.7] [Reference Citation Analysis (0)] |
| 3. | Ma GL, Murphy JD, Martinez ME, Sicklick JK. Epidemiology of gastrointestinal stromal tumors in the era of histology codes: results of a population-based study. Cancer Epidemiol Biomarkers Prev. 2015;24:298-302. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 142] [Cited by in RCA: 182] [Article Influence: 16.5] [Reference Citation Analysis (0)] |
| 4. | Harlan LC, Eisenstein J, Russell MC, Stevens JL, Cardona K. Gastrointestinal stromal tumors: treatment patterns of a population-based sample. J Surg Oncol. 2015;111:702-707. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 20] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 5. | DeMatteo RP, Lewis JJ, Leung D, Mudan SS, Woodruff JM, Brennan MF. Two hundred gastrointestinal stromal tumors: recurrence patterns and prognostic factors for survival. Ann Surg. 2000;231:51-58. [PubMed] |
| 6. | Kindblom LG, Remotti HE, Aldenborg F, Meis-Kindblom JM. Gastrointestinal pacemaker cell tumor (GIPACT): gastrointestinal stromal tumors show phenotypic characteristics of the interstitial cells of Cajal. Am J Pathol. 1998;152:1259-1269. [PubMed] |
| 7. | Sircar K, Hewlett BR, Huizinga JD, Chorneyko K, Berezin I, Riddell RH. Interstitial cells of Cajal as precursors of gastrointestinal stromal tumors. Am J Surg Pathol. 1999;23:377-389. [PubMed] |
| 8. | Fletcher CD, Berman JJ, Corless C, Gorstein F, Lasota J, Longley BJ, Miettinen M, O’Leary TJ, Remotti H, Rubin BP. Diagnosis of gastrointestinal stromal tumors: A consensus approach. Hum Pathol. 2002;33:459-465. [PubMed] |
| 9. | Rubin BP. Gastrointestinal stromal tumours: an update. Histopathology. 2006;48:83-96. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 139] [Cited by in RCA: 132] [Article Influence: 6.9] [Reference Citation Analysis (0)] |
| 10. | Demetri GD, von Mehren M, Blanke CD, Van den Abbeele AD, Eisenberg B, Roberts PJ, Heinrich MC, Tuveson DA, Singer S, Janicek M. Efficacy and safety of imatinib mesylate in advanced gastrointestinal stromal tumors. N Engl J Med. 2002;347:472-480. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 3203] [Cited by in RCA: 3107] [Article Influence: 135.1] [Reference Citation Analysis (0)] |
| 11. | Tran T, Davila JA, El-Serag HB. The epidemiology of malignant gastrointestinal stromal tumors: an analysis of 1,458 cases from 1992 to 2000. Am J Gastroenterol. 2005;100:162-168. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 436] [Cited by in RCA: 437] [Article Influence: 21.9] [Reference Citation Analysis (1)] |
| 12. | Miettinen M, Sobin LH, Lasota J. Gastrointestinal stromal tumors of the stomach: a clinicopathologic, immunohistochemical, and molecular genetic study of 1765 cases with long-term follow-up. Am J Surg Pathol. 2005;29:52-68. [PubMed] |
| 13. | Miettinen M, Makhlouf H, Sobin LH, Lasota J. Gastrointestinal stromal tumors of the jejunum and ileum: a clinicopathologic, immunohistochemical, and molecular genetic study of 906 cases before imatinib with long-term follow-up. Am J Surg Pathol. 2006;30:477-489. [PubMed] |
| 14. | Robb WB, Bruyere E, Amielh D, Vinatier E, Mabrut JY, Perniceni T, Piessen G, Mariette C; FREGAT Working Group--FRENCH. Esophageal gastrointestinal stromal tumor: is tumoral enucleation a viable therapeutic option? Ann Surg. 2015;261:117-124. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 23] [Cited by in RCA: 29] [Article Influence: 2.9] [Reference Citation Analysis (33)] |
| 15. | Heinrich MC, Corless CL. Gastric GI stromal tumors (GISTs): the role of surgery in the era of targeted therapy. J Surg Oncol. 2005;90:195-207; discussion 207. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 84] [Cited by in RCA: 83] [Article Influence: 4.2] [Reference Citation Analysis (0)] |
| 16. | Frankel TL, Chang AE, Wong SL. Surgical options for localized and advanced gastrointestinal stromal tumors. J Surg Oncol. 2011;104:882-887. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 25] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 17. | Martin-Broto J, Martinez-Marín V, Serrano C, Hindi N, López-Guerrero JA, Bisculoa M, Ramos-Asensio R, Vallejo-Benítez A, Marcilla-Plaza D, González-Cámpora R. Gastrointestinal stromal tumors (GISTs): SEAP-SEOM consensus on pathologic and molecular diagnosis. Clin Transl Oncol. 2017;19:536-545. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 10] [Cited by in RCA: 16] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 18. | Pink D, Schoeler D, Lindner T, Thuss-Patience PC, Kretzschmar A, Knipp H, Vanhoefer U, Reichardt P. Severe hypoglycemia caused by paraneoplastic production of IGF-II in patients with advanced gastrointestinal stromal tumors: a report of two cases. J Clin Oncol. 2005;23:6809-6811. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 54] [Article Influence: 2.7] [Reference Citation Analysis (0)] |
| 19. | Maynard MA, Marino-Enriquez A, Fletcher JA, Dorfman DM, Raut CP, Yassa L, Guo C, Wang Y, Dorfman C, Feldman HA. Thyroid hormone inactivation in gastrointestinal stromal tumors. N Engl J Med. 2014;370:1327-1334. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 40] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 20. | Gasparotto D, Rossi S, Bearzi I, Doglioni C, Marzotto A, Hornick JL, Grizzo A, Sartor C, Mandolesi A, Sciot R. Multiple primary sporadic gastrointestinal stromal tumors in the adult: an underestimated entity. Clin Cancer Res. 2008;14:5715-5721. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 40] [Cited by in RCA: 47] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 21. | Miettinen M, Fetsch JF, Sobin LH, Lasota J. Gastrointestinal stromal tumors in patients with neurofibromatosis 1: a clinicopathologic and molecular genetic study of 45 cases. Am J Surg Pathol. 2006;30:90-96. [PubMed] |
| 22. | Carney JA. Gastric stromal sarcoma, pulmonary chondroma, and extra-adrenal paraganglioma (Carney Triad): natural history, adrenocortical component, and possible familial occurrence. Mayo Clin Proc. 1999;74:543-552. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 321] [Cited by in RCA: 275] [Article Influence: 10.6] [Reference Citation Analysis (0)] |
| 23. | Carney JA, Stratakis CA. Familial paraganglioma and gastric stromal sarcoma: a new syndrome distinct from the Carney triad. Am J Med Genet. 2002;108:132-139. [PubMed] |
| 24. | Corless CL, Barnett CM, Heinrich MC. Gastrointestinal stromal tumours: origin and molecular oncology. Nat Rev Cancer. 2011;11:865-878. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 635] [Cited by in RCA: 621] [Article Influence: 44.4] [Reference Citation Analysis (0)] |
| 25. | Janeway KA, Weldon CB. Pediatric gastrointestinal stromal tumor. Semin Pediatr Surg. 2012;21:31-43. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 34] [Cited by in RCA: 38] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 26. | Scarpa M, Bertin M, Ruffolo C, Polese L, D’Amico DF, Angriman I. A systematic review on the clinical diagnosis of gastrointestinal stromal tumors. J Surg Oncol. 2008;98:384-392. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 86] [Cited by in RCA: 88] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 27. | Kim JS, Kim HJ, Park SH, Lee JS, Kim AY, Ha HK. Computed tomography features and predictive findings of ruptured gastrointestinal stromal tumours. Eur Radiol. 2017;27:2583-2590. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 20] [Article Influence: 2.2] [Reference Citation Analysis (0)] |
| 28. | Levy AD, Remotti HE, Thompson WM, Sobin LH, Miettinen M. Gastrointestinal stromal tumors: radiologic features with pathologic correlation. Radiographics. 2003;23:283-304, 456; quiz 532. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 355] [Cited by in RCA: 324] [Article Influence: 14.7] [Reference Citation Analysis (0)] |
| 29. | Eisenhauer EA, Therasse P, Bogaerts J, Schwartz LH, Sargent D, Ford R, Dancey J, Arbuck S, Gwyther S, Mooney M. New response evaluation criteria in solid tumours: revised RECIST guideline (version 1.1). Eur J Cancer. 2009;45:228-247. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15860] [Cited by in RCA: 21529] [Article Influence: 1345.6] [Reference Citation Analysis (1)] |
| 30. | Raut CP, Posner M, Desai J, Morgan JA, George S, Zahrieh D, Fletcher CD, Demetri GD, Bertagnolli MM. Surgical management of advanced gastrointestinal stromal tumors after treatment with targeted systemic therapy using kinase inhibitors. J Clin Oncol. 2006;24:2325-2331. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 311] [Cited by in RCA: 296] [Article Influence: 15.6] [Reference Citation Analysis (0)] |
| 31. | Choi H, Charnsangavej C, Faria SC, Macapinlac HA, Burgess MA, Patel SR, Chen LL, Podoloff DA, Benjamin RS. Correlation of computed tomography and positron emission tomography in patients with metastatic gastrointestinal stromal tumor treated at a single institution with imatinib mesylate: proposal of new computed tomography response criteria. J Clin Oncol. 2007;25:1753-1759. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1094] [Cited by in RCA: 1117] [Article Influence: 62.1] [Reference Citation Analysis (0)] |
| 32. | Choi H. Role of Imaging in Response Assessment and Individualised Treatment for Sarcomas. Clin Oncol (R Coll Radiol). 2017;29:481-488. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 15] [Cited by in RCA: 18] [Article Influence: 2.3] [Reference Citation Analysis (0)] |
| 33. | Koo HJ, Shin JH, Shin S, Yoon HK, Ko GY, Gwon DI. Efficacy and Clinical Outcomes of Transcatheter Arterial Embolization for Gastrointestinal Bleeding from Gastrointestinal Stromal Tumor. J Vasc Interv Radiol. 2015;26:1297-304.e1. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 28] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 34. | Eriksson M, Reichardt P, Sundby Hall K, Schütte J, Cameron S, Hohenberger P, Bauer S, Leinonen M, Reichardt A, Rejmyr Davis M. Needle biopsy through the abdominal wall for the diagnosis of gastrointestinal stromal tumour - Does it increase the risk for tumour cell seeding and recurrence? Eur J Cancer. 2016;59:128-133. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 25] [Article Influence: 2.8] [Reference Citation Analysis (0)] |
| 35. | Takaki H, Litchman T, Covey A, Cornelis F, Maybody M, Getrajdman GI, Sofocleous CT, Brown KT, Solomon SB, Alago W. Hepatic artery embolization for liver metastasis of gastrointestinal stromal tumor following imatinib and sunitinib therapy. J Gastrointest Cancer. 2014;45:494-499. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 24] [Article Influence: 2.4] [Reference Citation Analysis (0)] |
| 36. | Kobayashi K, Gupta S, Trent JC, Vauthey JN, Krishnamurthy S, Ensor J, Ahrar K, Wallace MJ, Madoff DC, Murthy R. Hepatic artery chemoembolization for 110 gastrointestinal stromal tumors: response, survival, and prognostic factors. Cancer. 2006;107:2833-2841. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 46] [Cited by in RCA: 46] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 37. | Pawlik TM, Vauthey JN, Abdalla EK, Pollock RE, Ellis LM, Curley SA. Results of a single-center experience with resection and ablation for sarcoma metastatic to the liver. Arch Surg. 2006;141:537-43; discussion 543-4. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 131] [Cited by in RCA: 122] [Article Influence: 6.4] [Reference Citation Analysis (0)] |
| 38. | Papanikolaou IS, Triantafyllou K, Kourikou A, Rösch T. Endoscopic ultrasonography for gastric submucosal lesions. World J Gastrointest Endosc. 2011;3:86-94. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 51] [Cited by in RCA: 77] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 39. | Tio TL, Tytgat GN, den Hartog Jager FC. Endoscopic ultrasonography for the evaluation of smooth muscle tumors in the upper gastrointestinal tract: an experience with 42 cases. Gastrointest Endosc. 1990;36:342-350. [PubMed] |
| 40. | Ando N, Goto H, Niwa Y, Hirooka Y, Ohmiya N, Nagasaka T, Hayakawa T. The diagnosis of GI stromal tumors with EUS-guided fine needle aspiration with immunohistochemical analysis. Gastrointest Endosc. 2002;55:37-43. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 247] [Cited by in RCA: 231] [Article Influence: 10.0] [Reference Citation Analysis (0)] |
| 41. | Watson RR, Binmoeller KF, Hamerski CM, Shergill AK, Shaw RE, Jaffee IM, Stewart L, Shah JN. Yield and performance characteristics of endoscopic ultrasound-guided fine needle aspiration for diagnosing upper GI tract stromal tumors. Dig Dis Sci. 2011;56:1757-1762. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 70] [Cited by in RCA: 73] [Article Influence: 5.2] [Reference Citation Analysis (0)] |
| 42. | Demetri GD, Benjamin RS, Blanke CD, Blay JY, Casali P, Choi H, Corless CL, Debiec-Rychter M, DeMatteo RP, Ettinger DS. NCCN Task Force report: management of patients with gastrointestinal stromal tumor (GIST)--update of the NCCN clinical practice guidelines. J Natl Compr Canc Netw. 2007;5 Suppl 2:S1-S29; quiz S30. [PubMed] |
| 43. | Kamiyama Y, Aihara R, Nakabayashi T, Mochiki E, Asao T, Kuwano H, Oriuchi N, Endo K. 18F-fluorodeoxyglucose positron emission tomography: useful technique for predicting malignant potential of gastrointestinal stromal tumors. World J Surg. 2005;29:1429-1435. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 70] [Cited by in RCA: 62] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 44. | Van den Abbeele AD. The lessons of GIST--PET and PET/CT: a new paradigm for imaging. Oncologist. 2008;13 Suppl 2:8-13. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 213] [Cited by in RCA: 202] [Article Influence: 11.9] [Reference Citation Analysis (0)] |
| 45. | Hassanzadeh-Rad A, Yousefifard M, Katal S, Asady H, Fard-Esfahani A, Moghadas Jafari A, Hosseini M. The value of (18) F-fluorodeoxyglucose positron emission tomography for prediction of treatment response in gastrointestinal stromal tumors: a systematic review and meta-analysis. J Gastroenterol Hepatol. 2016;31:929-935. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 30] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 46. | Everett M, Gutman H. Surgical management of gastrointestinal stromal tumors: analysis of outcome with respect to surgical margins and technique. J Surg Oncol. 2008;98:588-593. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 44] [Cited by in RCA: 47] [Article Influence: 2.9] [Reference Citation Analysis (0)] |
| 47. | Dematteo RP, Gold JS, Saran L, Gönen M, Liau KH, Maki RG, Singer S, Besmer P, Brennan MF, Antonescu CR. Tumor mitotic rate, size, and location independently predict recurrence after resection of primary gastrointestinal stromal tumor (GIST). Cancer. 2008;112:608-615. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 317] [Cited by in RCA: 345] [Article Influence: 20.3] [Reference Citation Analysis (0)] |
| 48. | Gold JS, Dematteo RP. Combined surgical and molecular therapy: the gastrointestinal stromal tumor model. Ann Surg. 2006;244:176-184. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 187] [Cited by in RCA: 186] [Article Influence: 9.8] [Reference Citation Analysis (0)] |
| 49. | Koga T, Hirayama Y, Yoshiya S, Taketani K, Nakanoko T, Yoshida R, Minagawa R, Kai M, Kajiyama K, Akahoshi K. Necessity for resection of gastric gastrointestinal stromal tumors ≤ 20 mm. Anticancer Res. 2015;35:2341-2344. [PubMed] |
| 50. | Balde AI, Chen T, Hu Y, Redondo N JD, Liu H, Gong W, Yu J, Zhen L, Li G. Safety analysis of laparoscopic endoscopic cooperative surgery versus endoscopic submucosal dissection for selected gastric gastrointestinal stromal tumors: a propensity score-matched study. Surg Endosc. 2017;31:843-851. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 41] [Cited by in RCA: 41] [Article Influence: 5.1] [Reference Citation Analysis (1)] |
| 51. | Novitsky YW, Kercher KW, Sing RF, Heniford BT. Long-term outcomes of laparoscopic resection of gastric gastrointestinal stromal tumors. Ann Surg. 2006;243:738-745; discussion 745-747. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 278] [Cited by in RCA: 291] [Article Influence: 15.3] [Reference Citation Analysis (0)] |
| 52. | Milone M, Elmore U, Musella M, Parise P, Zotti MC, Bracale U, Di Lauro K, Manigrasso M, Milone F, Rosati R. Safety and efficacy of laparoscopic wedge gastrectomy for large gastrointestinal stromal tumors. Eur J Surg Oncol. 2017;43:796-800. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 24] [Cited by in RCA: 24] [Article Influence: 3.0] [Reference Citation Analysis (0)] |
| 53. | Honda M, Hiki N, Nunobe S, Ohashi M, Kiyokawa T, Sano T, Yamaguchi T. Long-term and surgical outcomes of laparoscopic surgery for gastric gastrointestinal stromal tumors. Surg Endosc. 2014;28:2317-2322. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 35] [Cited by in RCA: 39] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 54. | Masoni L, Gentili I, Maglio R, Meucci M, D’Ambra G, Di Giulio E, Di Nardo G, Corleto VD. Laparoscopic resection of large gastric GISTs: feasibility and long-term results. Surg Endosc. 2014;28:2905-2910. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 17] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 55. | Piessen G, Lefèvre JH, Cabau M, Duhamel A, Behal H, Perniceni T, Mabrut JY, Regimbeau JM, Bonvalot S, Tiberio GA. Laparoscopic Versus Open Surgery for Gastric Gastrointestinal Stromal Tumors: What Is the Impact on Postoperative Outcome and Oncologic Results? Ann Surg. 2015;262:831-9; discussion 829-40. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 50] [Cited by in RCA: 55] [Article Influence: 5.5] [Reference Citation Analysis (0)] |
| 56. | Bischof DA, Kim Y, Dodson R, Carolina Jimenez M, Behman R, Cocieru A, Blazer DG 3rd, Fisher SB, Squires MH 3rd, Kooby DA, Maithel SK, Groeschl RT, Clark Gamblin T, Bauer TW, Karanicolas PJ, Law C, Quereshy FA, Pawlik TM. Open versus minimally invasive resection of gastric GIST: a multi-institutional analysis of short- and long-term outcomes. Ann Surg Oncol. 2014;21:2941-2948. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 39] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 57. | Khoo CY, Goh BKP, Eng AKH, Chan WH, Teo MCC, Chung AYF, Ong HS, Wong WK. Laparoscopic wedge resection for suspected large (≥5 cm) gastric gastrointestinal stromal tumors. Surg Endosc. 2017;31:2271-2279. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 27] [Cited by in RCA: 27] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 58. | Qiu G, Wang J, Che X, He S, Wei C, Li X, Pang K, Fan L. Laparoscopic Versus Open Resection of Gastric Gastrointestinal Stromal Tumors Larger Than 5 cm: A Single-Center, Retrospective Study. Surg Innov. 2017;24:582-589. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 10] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 59. | Crouthamel MR, Kaufman JA, Billing JP, Billing PS, Landerholm RW. Incidental gastric mesenchymal tumors identified during laparoscopic sleeve gastrectomy. Surg Obes Relat Dis. 2015;11:1025-1028. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 19] [Cited by in RCA: 26] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 60. | Yuval JB, Khalaileh A, Abu-Gazala M, Shachar Y, Keidar A, Mintz Y, Nissan A, Elazary R. The true incidence of gastric GIST-a study based on morbidly obese patients undergoing sleeve gastrectomy. Obes Surg. 2014;24:2134-2137. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 36] [Cited by in RCA: 39] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 61. | Chiappetta S, Theodoridou S, Stier C, Weiner RA. Incidental finding of GIST during obesity surgery. Obes Surg. 2015;25:579-583. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 34] [Article Influence: 3.4] [Reference Citation Analysis (0)] |
| 62. | Tabrizian P, Sweeney RE, Uhr JH, Nguyen SQ, Divino CM. Laparoscopic resection of gastric and small bowel gastrointestinal stromal tumors: 10-year experience at a single center. J Am Coll Surg. 2014;218:367-373. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 12] [Cited by in RCA: 12] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 63. | Nguyen SQ, Divino CM, Wang JL, Dikman SH. Laparoscopic management of gastrointestinal stromal tumors. Surg Endosc. 2006;20:713-716. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 93] [Cited by in RCA: 101] [Article Influence: 5.3] [Reference Citation Analysis (0)] |
| 64. | Ihn K, Hyung WJ, Kim HI, An JY, Kim JW, Cheong JH, Yoon DS, Choi SH, Noh SH. Treatment Results of Small Intestinal Gastrointestinal Stromal Tumors Less than 10 cm in Diameter: A Comparison between Laparoscopy and Open Surgery. J Gastric Cancer. 2012;12:243-248. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 9] [Cited by in RCA: 15] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 65. | Cai W, Wang ZT, Wu L, Zhong J, Zheng MH. Laparoscopically assisted resections of small bowel stromal tumors are safe and effective. J Dig Dis. 2011;12:443-447. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 13] [Cited by in RCA: 13] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 66. | Tabrizian P, Nguyen SQ, Divino CM. Laparoscopic management and longterm outcomes of gastrointestinal stromal tumors. J Am Coll Surg. 2009;208:80-86. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 26] [Cited by in RCA: 29] [Article Influence: 1.7] [Reference Citation Analysis (0)] |
| 67. | Kukar M, Kapil A, Papenfuss W, Groman A, Grobmyer SR, Hochwald SN. Gastrointestinal stromal tumors (GISTs) at uncommon locations: a large population based analysis. J Surg Oncol. 2015;111:696-701. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 38] [Cited by in RCA: 47] [Article Influence: 4.7] [Reference Citation Analysis (0)] |
| 68. | Tai WC, Chuah SK, Lin JW, Chen HH, Huang HY, Kuo CM, Yi LN, Lee CM, Changchien CS, Hu TH. Colorectal mesenchymal tumors - from smooth muscle tumors to stromal tumors. Oncol Rep. 2008;20:1157-1164. [PubMed] |
| 69. | Amato A. Colorectal gastrointestinal stromal tumor. Tech Coloproctol. 2010;14 Suppl 1:S91-S95. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 11] [Cited by in RCA: 14] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 70. | Duffaud F, Meeus P, Bachet JB, Cassier P, Huynh TK, Boucher E, Bouché O, Moutardier V, le Cesne A, Landi B. Conservative surgery vs. duodeneopancreatectomy in primary duodenal gastrointestinal stromal tumors (GIST): a retrospective review of 114 patients from the French sarcoma group (FSG). Eur J Surg Oncol. 2014;40:1369-1375. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 18] [Cited by in RCA: 21] [Article Influence: 1.9] [Reference Citation Analysis (0)] |
| 71. | Shen C, Chen H, Yin Y, Chen J, Han L, Zhang B, Chen Z, Chen J. Duodenal gastrointestinal stromal tumors: clinicopathological characteristics, surgery, and long-term outcome. BMC Surg. 2015;15:98. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 28] [Cited by in RCA: 31] [Article Influence: 3.1] [Reference Citation Analysis (0)] |
| 72. | Johnston FM, Kneuertz PJ, Cameron JL, Sanford D, Fisher S, Turley R, Groeschl R, Hyder O, Kooby DA, Blazer D 3rd, Choti MA, Wolfgang CL, Gamblin TC, Hawkins WG, Maithel SK, Pawlik TM. Presentation and management of gastrointestinal stromal tumors of the duodenum: a multi-institutional analysis. Ann Surg Oncol. 2012;19:3351-3360. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 57] [Cited by in RCA: 58] [Article Influence: 4.5] [Reference Citation Analysis (0)] |
| 73. | Tien YW, Lee CY, Huang CC, Hu RH, Lee PH. Surgery for gastrointestinal stromal tumors of the duodenum. Ann Surg Oncol. 2010;17:109-114. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 50] [Cited by in RCA: 53] [Article Influence: 3.3] [Reference Citation Analysis (0)] |
| 74. | Chok AY, Koh YX, Ow MY, Allen JC Jr, Goh BK. A systematic review and meta-analysis comparing pancreaticoduodenectomy versus limited resection for duodenal gastrointestinal stromal tumors. Ann Surg Oncol. 2014;21:3429-3438. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 42] [Cited by in RCA: 47] [Article Influence: 4.3] [Reference Citation Analysis (0)] |
| 75. | Colombo C, Ronellenfitsch U, Yuxin Z, Rutkowski P, Miceli R, Bylina E, Hohenberger P, Raut CP, Gronchi A. Clinical, pathological and surgical characteristics of duodenal gastrointestinal stromal tumor and their influence on survival: a multi-center study. Ann Surg Oncol. 2012;19:3361-3367. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 48] [Article Influence: 3.7] [Reference Citation Analysis (0)] |
| 76. | Wilkinson MJ, Fitzgerald JE, Strauss DC, Hayes AJ, Thomas JM, Messiou C, Fisher C, Benson C, Tekkis PP, Judson I. Surgical treatment of gastrointestinal stromal tumour of the rectum in the era of imatinib. Br J Surg. 2015;102:965-971. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 67] [Article Influence: 6.7] [Reference Citation Analysis (0)] |
| 77. | Machlenkin S, Pinsk I, Tulchinsky H, Ziv Y, Sayfan J, Duek D, Rabau M, Walfisch S. The effect of neoadjuvant Imatinib therapy on outcome and survival after rectal gastrointestinal stromal tumour. Colorectal Dis. 2011;13:1110-1115. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 32] [Cited by in RCA: 35] [Article Influence: 2.5] [Reference Citation Analysis (0)] |
| 78. | Fujimoto Y, Akiyoshi T, Konishi T, Nagayama S, Fukunaga Y, Ueno M. Laparoscopic sphincter-preserving surgery (intersphincteric resection) after neoadjuvant imatinib treatment for gastrointestinal stromal tumor (GIST) of the rectum. Int J Colorectal Dis. 2014;29:111-116. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 39] [Cited by in RCA: 45] [Article Influence: 4.1] [Reference Citation Analysis (0)] |
| 79. | Pintor-Tortolero J, García JC, Cantero R. Transanal minimally invasive surgery approach for rectal GIST. Tech Coloproctol. 2016;20:321-322. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 8] [Article Influence: 0.9] [Reference Citation Analysis (0)] |
| 80. | Andtbacka RH, Ng CS, Scaife CL, Cormier JN, Hunt KK, Pisters PW, Pollock RE, Benjamin RS, Burgess MA, Chen LL. Surgical resection of gastrointestinal stromal tumors after treatment with imatinib. Ann Surg Oncol. 2007;14:14-24. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 175] [Cited by in RCA: 177] [Article Influence: 9.8] [Reference Citation Analysis (0)] |
| 81. | Bonvalot S, Eldweny H, Péchoux CL, Vanel D, Terrier P, Cavalcanti A, Robert C, Lassau N, Cesne AL. Impact of surgery on advanced gastrointestinal stromal tumors (GIST) in the imatinib era. Ann Surg Oncol. 2006;13:1596-1603. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 118] [Cited by in RCA: 131] [Article Influence: 7.3] [Reference Citation Analysis (0)] |
| 82. | Bamboat ZM, DeMatteo RP. Metastasectomy for gastrointestinal stromal tumors. J Surg Oncol. 2014;109:23-27. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 21] [Cited by in RCA: 22] [Article Influence: 1.8] [Reference Citation Analysis (0)] |
| 83. | Ye YJ, Gao ZD, Poston GJ, Wang S. Diagnosis and multi-disciplinary management of hepatic metastases from gastrointestinal stromal tumour (GIST). Eur J Surg Oncol. 2009;35:787-792. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 20] [Cited by in RCA: 24] [Article Influence: 1.5] [Reference Citation Analysis (0)] |
| 84. | Sugarbaker PH. Sarcomatosis and Imatinib-Resistant GISTosis: Diagnosis and Therapeutic Options. Cytoreductive Surgery Perioperative Chemotherapy for Peritoneal Surface Malignancy Textbook and Video Atlas. 1st ed. Woodbury, CT: Cine-Med Publishing, Inc 2012; 127-136. |
| 85. | Raut CP, Wang Q, Manola J, Morgan JA, George S, Wagner AJ, Butrynski JE, Fletcher CD, Demetri GD, Bertagnolli MM. Cytoreductive surgery in patients with metastatic gastrointestinal stromal tumor treated with sunitinib malate. Ann Surg Oncol. 2010;17:407-415. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 51] [Cited by in RCA: 57] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 86. | Gronchi A, Fiore M, Miselli F, Lagonigro MS, Coco P, Messina A, Pilotti S, Casali PG. Surgery of residual disease following molecular-targeted therapy with imatinib mesylate in advanced/metastatic GIST. Ann Surg. 2007;245:341-346. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 168] [Cited by in RCA: 172] [Article Influence: 9.6] [Reference Citation Analysis (0)] |
| 87. | DeMatteo RP, Maki RG, Singer S, Gonen M, Brennan MF, Antonescu CR. Results of tyrosine kinase inhibitor therapy followed by surgical resection for metastatic gastrointestinal stromal tumor. Ann Surg. 2007;245:347-352. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 226] [Cited by in RCA: 224] [Article Influence: 12.4] [Reference Citation Analysis (0)] |
| 88. | Bonvalot S, Cavalcanti A, Le Péchoux C, Terrier P, Vanel D, Blay JY, Le Cesne A, Elias D. Randomized trial of cytoreduction followed by intraperitoneal chemotherapy versus cytoreduction alone in patients with peritoneal sarcomatosis. Eur J Surg Oncol. 2005;31:917-923. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 67] [Cited by in RCA: 71] [Article Influence: 3.6] [Reference Citation Analysis (0)] |
| 89. | DeMatteo RP, Shah A, Fong Y, Jarnagin WR, Blumgart LH, Brennan MF. Results of hepatic resection for sarcoma metastatic to liver. Ann Surg. 2001;234:540-547; discussion 547-548. [PubMed] |
| 90. | Turley RS, Peng PD, Reddy SK, Barbas AS, Geller DA, Marsh JW, Tsung A, Pawlik TM, Clary BM. Hepatic resection for metastatic gastrointestinal stromal tumors in the tyrosine kinase inhibitor era. Cancer. 2012;118:3571-3578. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 45] [Cited by in RCA: 45] [Article Influence: 3.5] [Reference Citation Analysis (0)] |
| 91. | Husted TL, Neff G, Thomas MJ, Gross TG, Woodle ES, Buell JF. Liver transplantation for primary or metastatic sarcoma to the liver. Am J Transplant. 2006;6:392-397. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 55] [Cited by in RCA: 49] [Article Influence: 2.6] [Reference Citation Analysis (0)] |
| 92. | Serralta AS, Sanjuan FR, Moya AH, Orbis FC, López-Andújar R, Pareja EI, Vila JC, Rayón M, Juan MB, Mir JP. Combined liver transplantation plus imatinib for unresectable metastases of gastrointestinal stromal tumours. Eur J Gastroenterol Hepatol. 2004;16:1237-1239. [PubMed] |
| 93. | Corless CL, Ballman KV, Antonescu CR, Kolesnikova V, Maki RG, Pisters PW, Blackstein ME, Blanke CD, Demetri GD, Heinrich MC. Pathologic and molecular features correlate with long-term outcome after adjuvant therapy of resected primary GI stromal tumor: the ACOSOG Z9001 trial. J Clin Oncol. 2014;32:1563-1570. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 181] [Cited by in RCA: 221] [Article Influence: 20.1] [Reference Citation Analysis (0)] |
| 94. | Reichardt P, Hogendoorn PC, Tamborini E, Loda M, Gronchi A, Poveda A, Schöffski P. Gastrointestinal stromal tumors I: pathology, pathobiology, primary therapy, and surgical issues. Semin Oncol. 2009;36:290-301. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 30] [Cited by in RCA: 32] [Article Influence: 2.0] [Reference Citation Analysis (0)] |
| 95. | Lasota J, Miettinen M. Clinical significance of oncogenic KIT and PDGFRA mutations in gastrointestinal stromal tumours. Histopathology. 2008;53:245-266. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 305] [Cited by in RCA: 285] [Article Influence: 16.8] [Reference Citation Analysis (1)] |
| 96. | Blay JY, Heinrich MC, Hohenberger P, Casali PG, Rutkowski P, Serrano-Garcia C, Jones RL, Hall KS, Eckardt JR, von Mehren M. A randomized, double-blind, placebo-controlled, phase III study of crenolanib in advanced or metastatic GIST patients bearing a D842V mutation in PDGFRA: The CrenoGIST study. J Clin Oncol. 2017;35:published online before print. [RCA] [DOI] [Full Text] [Cited by in Crossref: 9] [Cited by in RCA: 10] [Article Influence: 1.3] [Reference Citation Analysis (0)] |
| 97. | Hostein I, Faur N, Primois C, Boury F, Denard J, Emile JF, Bringuier PP, Scoazec JY, Coindre JM. BRAF mutation status in gastrointestinal stromal tumors. Am J Clin Pathol. 2010;133:141-148. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 152] [Cited by in RCA: 152] [Article Influence: 10.1] [Reference Citation Analysis (0)] |
| 98. | Janeway KA, Kim SY, Lodish M, Nosé V, Rustin P, Gaal J, Dahia PL, Liegl B, Ball ER, Raygada M. Defects in succinate dehydrogenase in gastrointestinal stromal tumors lacking KIT and PDGFRA mutations. Proc Natl Acad Sci U S A. 2011;108:314-318. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 436] [Cited by in RCA: 462] [Article Influence: 30.8] [Reference Citation Analysis (0)] |
| 99. | Ricci R. Syndromic gastrointestinal stromal tumors. Hered Cancer Clin Pract. 2016;14:15. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 48] [Cited by in RCA: 63] [Article Influence: 7.0] [Reference Citation Analysis (0)] |
| 100. | Casali PG, Zalcberg J, Le Cesne A, Reichardt P, Blay JY, Lindner LH, Judson IR, Schöffski P, Leyvraz S, Italiano A. Ten-Year Progression-Free and Overall Survival in Patients With Unresectable or Metastatic GI Stromal Tumors: Long-Term Analysis of the European Organisation for Research and Treatment of Cancer, Italian Sarcoma Group, and Australasian Gastrointestinal Trials Group Intergroup Phase III Randomized Trial on Imatinib at Two Dose Levels. J Clin Oncol. 2017;35:1713-1720. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 90] [Cited by in RCA: 100] [Article Influence: 12.5] [Reference Citation Analysis (0)] |
| 101. | Sanchez Hidalgo JM, Rufian Peña S, Ciria Bru R, Naranjo Torres A, Muñoz Casares C, Ruiz Rabelo J, Briceño Delgado J. Gastrointestinal stromal tumors (GIST): a prospective evaluation of risk factors and prognostic scores. J Gastrointest Cancer. 2010;41:27-37. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 4] [Cited by in RCA: 6] [Article Influence: 0.4] [Reference Citation Analysis (0)] |
| 102. | Rutkowski P, Nowecki ZI, Michej W, Debiec-Rychter M, Woźniak A, Limon J, Siedlecki J, Grzesiakowska U, Kakol M, Osuch C. Risk criteria and prognostic factors for predicting recurrences after resection of primary gastrointestinal stromal tumor. Ann Surg Oncol. 2007;14:2018-2027. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 173] [Cited by in RCA: 184] [Article Influence: 10.2] [Reference Citation Analysis (0)] |
| 103. | Miettinen M, Lasota J. Gastrointestinal stromal tumors: Pathology and prognosis at different sites. Semin Diagn Pathol. 2006;23:70-83. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 1244] [Cited by in RCA: 1300] [Article Influence: 72.2] [Reference Citation Analysis (33)] |
| 104. | Joensuu H. Risk stratification of patients diagnosed with gastrointestinal stromal tumor. Hum Pathol. 2008;39:1411-1419. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 699] [Cited by in RCA: 862] [Article Influence: 50.7] [Reference Citation Analysis (0)] |
| 105. | Hohenberger P, Ronellenfitsch U, Oladeji O, Pink D, Ströbel P, Wardelmann E, Reichardt P. Pattern of recurrence in patients with ruptured primary gastrointestinal stromal tumour. Br J Surg. 2010;97:1854-1859. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 149] [Cited by in RCA: 149] [Article Influence: 9.9] [Reference Citation Analysis (0)] |
| 106. | Besana-Ciani I, Boni L, Dionigi G, Benevento A, Dionigi R. Outcome and long term results of surgical resection for gastrointestinal stromal tumors (GIST). Scand J Surg. 2003;92:195-199. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 28] [Cited by in RCA: 34] [Article Influence: 1.6] [Reference Citation Analysis (0)] |
| 107. | DeMatteo RP, Ballman KV, Antonescu CR, Corless C, Kolesnikova V, von Mehren M, McCarter MD, Norton J, Maki RG, Pisters PW, Demetri GD, Brennan MF, Owzar K; American College of Surgeons Oncology Group (ACOSOG) Intergroup Adjuvant GIST Study Team for the Alliance for Clinical Trials in Oncology. Long-term results of adjuvant imatinib mesylate in localized, high-risk, primary gastrointestinal stromal tumor: ACOSOG Z9000 (Alliance) intergroup phase 2 trial. Ann Surg. 2013;258:422-429. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 121] [Cited by in RCA: 124] [Article Influence: 10.3] [Reference Citation Analysis (0)] |
| 108. | Dematteo RP, Ballman KV, Antonescu CR, Maki RG, Pisters PW, Demetri GD, Blackstein ME, Blanke CD, von Mehren M, Brennan MF, Patel S, McCarter MD, Polikoff JA, Tan BR, Owzar K; American College of Surgeons Oncology Group (ACOSOG) Intergroup Adjuvant GIST Study Team. Adjuvant imatinib mesylate after resection of localised, primary gastrointestinal stromal tumour: a randomised, double-blind, placebo-controlled trial. Lancet. 2009;373:1097-1104. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 1075] [Cited by in RCA: 967] [Article Influence: 60.4] [Reference Citation Analysis (1)] |
| 109. | Casali PG, Le Cesne A, Poveda Velasco A, Kotasek D, Rutkowski P, Hohenberger P, Fumagalli E, Judson IR, Italiano A, Gelderblom H. Time to Definitive Failure to the First Tyrosine Kinase Inhibitor in Localized GI Stromal Tumors Treated With Imatinib As an Adjuvant: A European Organisation for Research and Treatment of Cancer Soft Tissue and Bone Sarcoma Group Intergroup Randomized Trial in Collaboration With the Australasian Gastro-Intestinal Trials Group, UNICANCER, French Sarcoma Group, Italian Sarcoma Group, and Spanish Group for Research on Sarcomas. J Clin Oncol. 2015;33:4276-4283. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 102] [Cited by in RCA: 122] [Article Influence: 12.2] [Reference Citation Analysis (0)] |
| 110. | Joensuu H, Eriksson M, Sundby Hall K, Hartmann JT, Pink D, Schütte J, Ramadori G, Hohenberger P, Duyster J, Al-Batran SE. One vs three years of adjuvant imatinib for operable gastrointestinal stromal tumor: a randomized trial. JAMA. 2012;307:1265-1272. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 758] [Cited by in RCA: 681] [Article Influence: 52.4] [Reference Citation Analysis (0)] |
| 111. | Joensuu H, Wardelmann E, Sihto H, Eriksson M, Sundby Hall K, Reichardt A, Hartmann JT, Pink D, Cameron S, Hohenberger P. Effect of KIT and PDGFRA Mutations on Survival in Patients With Gastrointestinal Stromal Tumors Treated With Adjuvant Imatinib: An Exploratory Analysis of a Randomized Clinical Trial. JAMA Oncol. 2017;3:602-609. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 92] [Cited by in RCA: 135] [Article Influence: 16.9] [Reference Citation Analysis (0)] |
| 112. | von Mehren M, Joensuu H. Gastrointestinal Stromal Tumors. J Clin Oncol. 2018;36:136-143. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 139] [Cited by in RCA: 219] [Article Influence: 27.4] [Reference Citation Analysis (0)] |
| 113. | ESMO/European Sarcoma Network Working Group. Gastrointestinal stromal tumours: ESMO Clinical Practice Guidelines for diagnosis, treatment and follow-up. Ann Oncol. 2014;25 Suppl 3:iii21-iii26. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 228] [Cited by in RCA: 264] [Article Influence: 26.4] [Reference Citation Analysis (0)] |
| 114. | Poveda A, Martinez V, Serrano C, Sevilla I, Lecumberri MJ, de Beveridge RD, Estival A, Vicente D, Rubió J, Martin-Broto J. SEOM Clinical Guideline for gastrointestinal sarcomas (GIST) (2016). Clin Transl Oncol. 2016;18:1221-1228. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in Crossref: 14] [Cited by in RCA: 11] [Article Influence: 1.2] [Reference Citation Analysis (0)] |
| 115. | Duffaud F, Meeus P, Bertucci F, Delhorme JB, Stoeckle E, Isambert N, Bompas E, Gagniere J, Bouché O, Toulmonde M. Patterns of care and clinical outcomes in primary oesophageal gastrointestinal stromal tumours (GIST): A retrospective study of the French Sarcoma Group (FSG). Eur J Surg Oncol. 2017;43:1110-1116. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 6] [Cited by in RCA: 11] [Article Influence: 1.4] [Reference Citation Analysis (1)] |
| 116. | Miettinen M, Lasota J. Gastrointestinal stromal tumors: review on morphology, molecular pathology, prognosis, and differential diagnosis. Arch Pathol Lab Med. 2006;130:1466-1478. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 27] [Reference Citation Analysis (0)] |
| 117. | Rubin BP, Blanke CD, Demetri GD, Dematteo RP, Fletcher CD, Goldblum JR, Lasota J, Lazar A, Maki RG, Miettinen M. Protocol for the examination of specimens from patients with gastrointestinal stromal tumor. Arch Pathol Lab Med. 2010;134:165-170. [RCA] [PubMed] [DOI] [Full Text] [Cited by in RCA: 3] [Reference Citation Analysis (0)] |
| 118. | Sánchez Hidalgo JM, Muñoz Casares FC, Rufian Peña S, Naranjo Torres A, Ciria Bru R, Briceño Delgado J, López Cillero P. [Gastrointestinal stromal tumors (GIST): factors predictive of survival after R0-cytoreduction]. Rev Esp Enferm Dig. 2007;99:703-708. [PubMed] |
| 119. | Belev B, Brčić I, Prejac J, Golubić ZA, Vrbanec D, Božikov J, Alerić I, Boban M, Razumović JJ. Role of Ki-67 as a prognostic factor in gastrointestinal stromal tumors. World J Gastroenterol. 2013;19:523-527. [RCA] [PubMed] [DOI] [Full Text] [Full Text (PDF)] [Cited by in CrossRef: 39] [Cited by in RCA: 40] [Article Influence: 3.3] [Reference Citation Analysis (1)] |
| 120. | Cananzi FC, Lorenzi B, Belgaumkar A, Benson C, Judson I, Mudan S. Prognostic factors for primary gastrointestinal stromal tumours: are they the same in the multidisciplinary treatment era? Langenbecks Arch Surg. 2014;399:323-332. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 8] [Cited by in RCA: 11] [Article Influence: 1.0] [Reference Citation Analysis (0)] |
| 121. | Vallböhmer D, Marcus HE, Baldus SE, Brabender J, Drebber U, Metzger R, Hölscher AH, Schneider PM. Serosal penetration is an important prognostic factor for gastrointestinal stromal tumors. Oncol Rep. 2008;20:779-783. [PubMed] |
| 122. | Dei Tos AP, Laurino L, Bearzi I, Messerini L, Farinati F; Gruppo Italiano Patologi Apparato Digerente (GIPAD); Società Italiana di Anatomia Patologica e Citopatologia Diagnostica/International Academy of Pathology, Italian division (SIAPEC/IAP). Gastrointestinal stromal tumors: the histology report. Dig Liver Dis. 2011;43 Suppl 4:S304-S309. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 16] [Cited by in RCA: 16] [Article Influence: 1.1] [Reference Citation Analysis (0)] |
| 123. | West RB, Corless CL, Chen X, Rubin BP, Subramanian S, Montgomery K, Zhu S, Ball CA, Nielsen TO, Patel R. The novel marker, DOG1, is expressed ubiquitously in gastrointestinal stromal tumors irrespective of KIT or PDGFRA mutation status. Am J Pathol. 2004;165:107-113. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 462] [Cited by in RCA: 456] [Article Influence: 21.7] [Reference Citation Analysis (0)] |
| 124. | Kang GH, Srivastava A, Kim YE, Park HJ, Park CK, Sohn TS, Kim S, Kang DY, Kim KM. DOG1 and PKC-θ are useful in the diagnosis of KIT-negative gastrointestinal stromal tumors. Mod Pathol. 2011;24:866-875. [RCA] [PubMed] [DOI] [Full Text] [Cited by in Crossref: 49] [Cited by in RCA: 43] [Article Influence: 3.1] [Reference Citation Analysis (0)] |