Copyright
©2012 Baishideng Publishing Group Co.
World J Gastroenterol. Nov 14, 2012; 18(42): 6036-6059
Published online Nov 14, 2012. doi: 10.3748/wjg.v18.i42.6036
Published online Nov 14, 2012. doi: 10.3748/wjg.v18.i42.6036
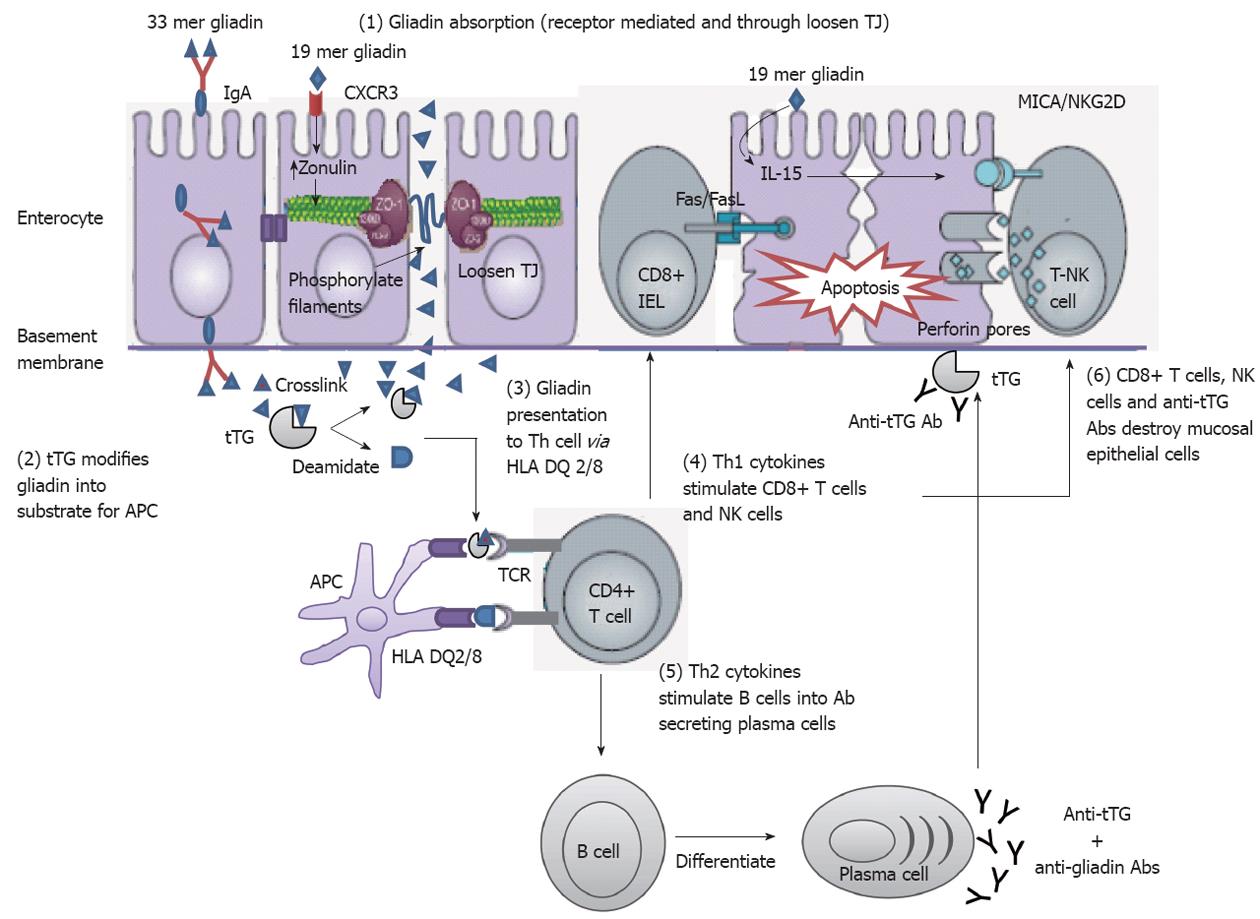
Figure 3 Mechanisms of mucosal damage in celiac disease[80] (adapted).
Gliadin peptides crosses the enterocyte by paracellular tight junctions (TJ) as a consequence of increased release of zonulin leading to impaired mucosal integrity upon 19 mer gliadin binding to chemokine (C-X-C motif) receptor 3 (CXCR3) receptor, or via transcytosis, or retrotranscytosis of secretory immunoglobulin A (IgA) through transferrin receptor CD71. Tissue transglutaminase (tTG) deamidates or crosslinks 33 mer gliadin which is then recognized by human leukocyte antigen (HLA)-DQ2 or -DQ8 molecules of antigen presenting cell (APC). APC presents the toxic peptide to CD4+ T cells. Activated gluten-reactive CD4+ T-cells produce high levels of pro-inflammatory cytokines. T helper 1 (Th1) cytokines promote increased cytotoxicity of intraepithelial lymphocytes (IELs) and natural killer (NK) T cells which cause apoptotic death of enterocytes by the Fas/Fas ligand (FasL) system, or interleukin 15 (IL-15)-induced perforin/granzyme and homodimeric natural killer-activating receptor-major histocompatibility-classIchain-related gene A comple (NKG2D–MICA) signaling pathways. The production of T-helper2 (Th2) cytokines activate and induce clonal expansion of B cells, which differentiate into (antigliadin and anti-tTG) antibody secreting plasma cells. Interaction between with the extracellular tTG and anti-tTG-autoantibody may induce epithelial damage. TCR: T cell receptor.
- Citation: Gujral N, Freeman HJ, Thomson AB. Celiac disease: Prevalence, diagnosis, pathogenesis and treatment. World J Gastroenterol 2012; 18(42): 6036-6059
- URL: https://www.wjgnet.com/1007-9327/full/v18/i42/6036.htm
- DOI: https://dx.doi.org/10.3748/wjg.v18.i42.6036