Published online Jan 28, 2009. doi: 10.3748/wjg.15.496
Revised: November 20, 2008
Published online: January 28, 2009
AIM: To investigate the feasibility of fast track clinical pathway for esophageal tumor resections.
METHODS: One hundred and fourteen patients with esophageal carcinoma who underwent esophagogastrectomy from January 2006 to October 2007 in our department were studied. Fast track clinical pathway included analgesia control, fluid infusion volume control, early ambulation and enteral nutrition. Nasogastric tube was removed 3 d after operation and chest tube was removed 4 d after operation as a routine, and full liquid diet 5 d after operation.
RESULTS: Among 114 patients (84 men and 30 women), 26 patients underwent fast track surgery, including 17 patients over 65 years old and 9 under 65 (P = 0.014); 18 patients who had preoperative complications could not bear fast track surgery (P < 0.001). No significant differences in tolerance of fast track surgery were attributed to differences in gender, differentiated degree or stage of tumor, pathological type of tumor, or operative incision. The median length of hospital stay was 7 d (5-28 d), 4% patients were readmitted to hospital within 30 d of discharge. Three patients died and postoperative mortality was 2.6%. All 3 patients had no determinacy to fast track surgery approach.
CONCLUSION: The majority of patients with esophageal carcinoma can tolerate fast track surgery. Patients younger than 65 or who have no preoperative diseases have the best results. Median length of hospital stay has been reduced to 7 d.
- Citation: Jiang K, Cheng L, Wang JJ, Li JS, Nie J. Fast track clinical pathway implications in esophagogastrectomy. World J Gastroenterol 2009; 15(4): 496-501
- URL: https://www.wjgnet.com/1007-9327/full/v15/i4/496.htm
- DOI: https://dx.doi.org/10.3748/wjg.15.496
Recently, a new surgical model, fast track surgery, appears[12]. Fast track surgery combines various new techniques and new theories used in pre-operative, peri-operative and post-operative care of patients. The methods include anaesthesia, nutritional monitoring, optimal pain control and surgical techniques[3]. The combination of these approaches lowers the stress response, morbidity as well as mortality rates, thus greatly reducing the time required for full recovery. Fast track surgery has significantly changed many clinical therapeiutic modes.
To date, few existing data can prove whether such concept could also be safely applied to esophageal surgery such as esophageal tumor resection[4]. This study reviews the outcome of a single-center survey regarding the application of the new “fast-track surgery” model and its effects in patients undergoing esophagus tumor resection.
The records of patients with esophageal carcinoma who underwent esophagogastrectomy from January 2006 to October 2007 in our department were studied. All the patients received preoperative examinations including gastroscope, barium meal of upper gastrointestine, abdominal ultrasonography, chest CT, pulmonary function and hematological examinations.
The diagnosis of esophageal carcinoma was identified, and no obvious surgical contraindications were detected. There was no evidence of metastasis in intrathoracic lymph nodes, such as the signs of recurrent laryngeal nerve paralysis, diaphragmatic paralysis or Horner’s syndrome. There was no supraclavicular and cervical lymphadenectasis. If distant metastasis had been found or resection was impossible temporarily, neoadjuvant chemotherapy or radiotherapy was suggested preoperatively. One hundred and fourteen cases were selected according to the surgical criteria. All these patients received preoperative healthy education: (1) respiratory function exercise to improve pulmonary ventilation function; (2) effective cough and expectoration to promote lung re-ventilation postoperatively; and (3) diet guide to help patients switch from full liquid diet to semiliquid diet after operation. Preoperative preparations: Patients were fasted for 8 h and supplemented with sugar and salt through intravenous infusion 2 h before operation to increase energy. Anesthesia: Double channel lumen intubation general anesthesia combined with epidural block was used. Anesthetists actively removed sputum, closely controlled the intake and output liquid to maintain the stabilization of effective circulation. A classic radical correction of esophageal carcinoma was performed through opening the chest between ribs and preserving rib bed. Intercostal nerves were removed for assisted analgesic effect. A mechanical anastomosis was performed between the end of the esophagus and the side of the stomach. Jejunal tube was placed at 20-30 cm away from distal Treitz ligament. Both thoracic and celiac lymph nodes were excised referring to the Korst’s profile of lymph nodes of esophageal carcinoma[5]. Patients were transferred to anesthesia recovery room after operation. The tracheal intubations were removed when their spontaneous breath, stable circulation, cough reflex, swallowing reflex, and oxygen saturation recovered. But patients with histories of severe diseases such as coronary artery diseases or ventilation dysfunction would be sent to the ICU for tracheal extubation. Enteral feedings combined with parenteral alimentation were used for postoperative patients. Parenteral alimentation was supported with enteral feedings via the jejunostomy tube, primarily with a rate of 20 mL/h in the first 48 h after operation and 65 mL/h 2 d later and then with parenteral alimentation. If swallow showed no leak, full liquid diet was started on the fifth day after operation. Patient controlled analgesia was suggested to be a common practice for 48-72 h after operation. Discharge standard: taking food totally through mouth without intravenous infusion and walking freely in rehabilitation home. The first telephone follow-up was carried out in 72 h after the patients discharged from hospital, with regular visits one week after the operation as the clinical follow-up. Later telephone follow-up was done once every week, until 30 d after operation.
Major complications were defined as any complication excluding transient atrial arrhythmias, urinary retention, or nonoperatively managed air leak. Mortality was defined as any death occurring during the hospital stay or within 30 d postoperatively. Outcome data were analyzed by SPSS 13.0 package using Chi-square test or Fisher exact test. P < 0. 05 was considered to be significant.
There were 114 patients, 84 men and 30 women. The ratio of male to female was 2.8: 1. The average age was 58.6 years, ranging from 38 to 85. Lesions were located in distal thoracic esophagus in 60 cases (52.6%), in mid-thoracic esophagus in 35 cases (31.6%), and in upper thoracic esophagus in 18 cases (15.8%). Twenty-eight of 114 cases had histories of various diseases: 14 with respiratory diseases (12.3%), 9 with cardiocerebrovascular disease (7.9%), 8 with other diseases (7.0%), and 3 with more than two kinds of diseases. Twenty-six patients could not undergo the fast track surgery. Seventeen patients were over 65 years old and nine were under 65 (P = 0.014); 18 patients who had a preoperative complication could not bear fast track surgery (P < 0.001). No significant differences in tolerance of fast track surgery were attributed to differences in gender, degree of differentiation, stage of tumor, pathological type, or operative incision (Table 1).
| Characteristics | Patients | Complications | Failed fast track | P value |
| Overall | 114 | 19 | 26 | |
| Gender | 0.80 | |||
| Male | 84 | 14 | 20 | |
| Female | 30 | 5 | 6 | |
| Age (yr) | 0.014 | |||
| ≥ 65 | 50 | 11 | 17 | |
| < 65 | 64 | 8 | 9 | |
| Differentiation | 1.00 | |||
| Low | 18 | 4 | 4 | |
| Moderate | 56 | 8 | 13 | |
| High | 40 | 7 | 9 | |
| Stage of cancer at time of surgery | 0.58 | |||
| I | 8 | 0 | 0 | |
| II | 16 | 2 | 4 | |
| III | 78 | 14 | 18 | |
| IV | 12 | 3 | 4 | |
| Preoperative complication | < 0.001 | |||
| Yes | 28 | 12 | 18 | |
| No | 86 | 7 | 8 | |
| Pathology | 1.00 | |||
| Squamous cell carcinoma | 87 | 15 | 20 | |
| Adenocarcinoma | 18 | 3 | 4 | |
| Other | 9 | 1 | 2 | |
| Operative incision | 0.73 | |||
| One | 60 | 9 | 12 | |
| Two | 36 | 6 | 9 | |
| Three | 18 | 4 | 5 | |
| Tolerated fast track surgery | 0.001 | |||
| Yes | 88 | 5 | ||
| No | 26 | 14 |
Sixty percent of the patients received tracheal extubation immediately at the end of the operation, 30% received tracheal extubation a few hours later in recovery room, and 10% demanded mechanical ventilation. The fluid infusion was controlled between 1.5 L and 2.5 L, between 2.5 L and 3.5 L and above 3.5 L for 71%, 25% and 4% of the total number of patients, respectively. A total of 109 (96%) patients accepted PCA, including vein PCA (44%), epidural PCA analgesia (52%) and 5 patients refused PCA for various reasons. PCA lasted 48-72 h ordinarily (Table 2).
| Variables | Data |
| Extubation | 114 |
| Immediate | 68 |
| Operation day | 34 |
| Later | 12 |
| Pain management | 109 |
| Epidural PCA | 59 |
| Vein PCA | 50 |
| Operative transfusion | 114 |
| 1.5-2.5 L | 81 |
| 2.5-3.5 L | 28 |
| > 3.5 L | 5 |
| Day | Daily guideline of postoperative care |
| POD 1 | Jejunal tube feeding 500 mL (20 mL/h);physical therapy four times per day;chest tube and nasogastric tube draining patency; head of bed put at 45-60 degree; supply albumin |
| POD 2 | Jejunal tube feeding 1000 mL (40 mL/h) ;remove urinary catheter and epidural (Or pod3 remove);encourage patient to ambulate; chest tube and nasogastric tube draining patency; continue physical therapy, promoted to lung recruitment |
| POD 3 | Jejunal tube feeding 1500 mL (65 mL/h); remove nasogastric tube; continue physical therapy |
| POD 4 | Jejunal tube feeding 1500 mL (65 mL/h); X-ray; remove chest tube (drainage < 100 mL) |
| POD 5 | Jejunal tube feeding 1500 mL (65 mL/h); gastrograffin swallow; anastomosis showed no leak; advice patient to take a little liquid diet; education on aspiration precaution |
| POD 6 | Increase liquid diet; continue to jejunal tube feeding |
| POD 7 | Remove jejunal tube; full liquid diet |
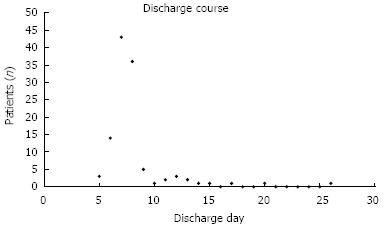
Postoperative patients relied mainly on enteral feedings and assisted by parenteral alimentation. During the first 48 h after operation, parenteral alimentation was primarily supported with enteral feedings via the jejunostomy tube with a rate of 20 mL/h 2 d later, jejunostomy tube feedings with a rate of 65 mL/h were given priority with supplement of parenteral alimentation. If swallow showed no leak, full liquid diet was started on postoperative day 5. All the patients were educated to prevent aspiration. Nasogastric tube was removed on postoperative day 3 and chest tube was routinely removed on postoperative day 4. Patients were encouraged to walk and cough effectively. Respiratory tract care was strengthened in order to promote lung reventilation postoperatively. The average length of hospital stay was 7 d (5-28 d), and 4% of the patients were readmitted within 30 d of discharge (Figure 1).
Postoperative mortality was 2.6% (3 cases). Nevertheless, all 3 patients had no relation to fast track surgery. The causes of death: respiratory failure in two patients and multiple organ failure in one. Nineteen patients had a variety of 34 major complications: 38% with pulmonary complications, 26% with cardiac complications, 15% with anastomotic complications, and 21% with other complications (Table 4).
| Variables | Data |
| Pulmonary | 13 |
| Empyema | 2 |
| Atelectasis | 2 |
| Pulmonary edema | 1 |
| Pulmonary infection | 3 |
| Respiratory insufficiency | 5 |
| Anastomotic | 5 |
| Leak | 4 |
| Hemorrhage | 1 |
| Cardiac | 9 |
| Atrial arrhythmia | 4 |
| Supraventricular arrhythmia | 3 |
| Ventricular arrhythmia | 2 |
| Other | 7 |
| Chylothorax | 3 |
| Hoarseness | 2 |
| Gastric perforation | 1 |
| Ileus | 1 |
| Mortality | 3 |
| Respiratory failure | 2 |
| Multiple organs failure | 1 |
Fast track surgery was suggested by Henrik Kehlet et al[12] who thought postoperative degression process of body function could be shortened from a few weeks to a few days. One hundred and fourteen patients undergoing fast-track rehabilitation got good therapeutic effect, compared with the traditional surgery of esophageal cancer[6789] (Table 5) .Fast track surgery were successful in many general surgical patients, especially in colorectal surgery patients[101112]. In our study, postoperative hospital stay was significantly shortened and cost of hospitalization was reduced without increase of morbidity or mortality. Postoperative hospital stay was declined from traditionally 12-14 d to now 7 d through the use of fast track surgery. Multivariate analysis showed that age (> 65 years) and preoperative complications were the main factors that determined whether patients could bear fast track surgery clinical pathway.
In brief, fast track surgery uses multiple modes to control pathophysiological process of perioperative patients. It can improve the prognosis and promote their recovery. How to attenuate the stimulation is the basis of reduction of stress response. Basically, the approaches include three aspects: (1) make good physical and mental preparation preoperatively; (2) minimize therapeutic stress; and block nerve conduction to stress signal[13]. In a wide view of these measures, there are not many higher demands of surgical skills. Fast track surgery approach mainly optimizes perioperative management on the basis of various effective methods confirmed by evidence-based medicine. As a result, fast track surgery reduces common complications, relieves patients’ pain and accelerates patients’ recovery.
Intravenous nutrition, gastrointestinal decompression and chest tube are all necessary for traditional esophagogastrectomy. Postoperative pain is common. We used fast track surgery to optimize traditional measures. It is known that gastrointestinal decompression and delayed eating are conventional means. However, nasogastric tube made 88% patients discomfort to a moderate to severe degree, and 70% patients with even more severe feelings[1415]. It is obvious that functional restoration of gastrointestine was delayed. Some studies found that cancellation of gastrointestinal decompression might be a vital step for faster functional restoration of gastrointestine and decrease of hospital stay. A recent meta-analysis showed that gastrointestinal decompression had not reduced the complications of operation on digestive tract[16]. Nevertheless, our research indicated that function of gastrointestine was in the stage of overall recovery during 48 after operation, therefore, gastrointestinal decompression would be helpful. In our opinion, gastrointestinal decompression is essential in the early postoperative stage, and the discomfort can be relieved by drugs.
Pulmonary complications are not only the most common but also the main death cause after operation[17]. So how to effectively prevent pulmonary complications becomes the focus of fast track surgery. Satisfying health education could relieve patients’ anxiety and fear, and partially reduce postoperative pain. Patients could benefit from good partner treatment and sufficient cardiorespiratory function exercise preoperatively. Full communication with anesthetist perioperatively is very helpful for anesthetist to grasp patient’s condition. On the premise of ensuring effective circulation, anesthetist controlled the fluid infusion volume, actively sucked sputum, and gave early tracheal extubation to promote lung reventilation postoperatively. Recently, the evidence shows that the reduction of fluid volume in the operation would help reduce postoperative complications and shorten the hospital stay[1819]. After operation, anesthetist performed a various kinds of patient control analgesia. Postoperative analgesia is not only the demanding of humanism but also the vital component of fast track surgery. It is very helpful for patients to ambulate earlier so that muscles will not be hypertrophied because of long-term bed-ridden. It is also very helpful for patients to cough and expectorate effectively to recruit their lungs. This could reduce thrombogenesis and pulmonary infection. Epidural analgesia has advantages in the early recovery of pulmonary function and early physical therapy. And effective cough for the effect of epidural analgesia was regional and weaker compared with vein analgesia. But the manipulation of epidural analgesia is complex. It is hard to control anesthesia plane and its effect is instable. We have found that the cooperation of surgeons, anesthestists, and dietitian is very important because they can work together with multiple means to effectively decrease the complications of lung and heart.
Early enteral nutrition not only gurantee the structure and function of intestinal mucosa cells, maintain intestinal mechanical, chemical and biological barrier, but also increase portal circulation, activate intestinal digestive secretary system and accelerate organ recovery. Enteral nutrition has also been an important measure for fast-track. Now perioperative nutritional support contains the full regulation of pathophysiological process as well as simple nutritional regulation. In the past decade, advantage of diversion from parenteral nutrition to enteral nutrition has been generally accepted. Enteral nutrition is more suitable for physiological demanding with less complications and lower price. Enteral alimentation should be small in amounts and short in time. Parentral nutrition is the major supplement and the whole enteral nutrition should be given 48 h later. Immunological enteral nutrition could be used for some indicated patients. A recent meta-analysis demonstrated that immunological enteral nutrition could reduce postoperative infection complications[20].
Enteroparalysis and anastomotic leakage have been two major puzzles for early eating after operation. Enteroparalysis was considered to be inevitable in the past. There are a few factors related to enteroparalysis which could be ameliorated by intestinal rest and gastrointestinal decompression. However, some studies indicated that intestinal rest and nasogastric tube decompression were not indispensable[2122]. That fast track encourages patients to have a diet early did not increase discomfort but promoted the intestinal recovery. Postoperative anastomotic leakage was a dangerous complication in the past. Late diet was thought to prevent leakage. However, with the development of evidence-based medicine, there has been no proof that late diet can reduce this kind of complication. Recent research showed that severe complications were mainly related to the condition of patients before operation and surgical techniques[23]. In our study, 4 cases had leakage in neck and 1 case had leakage in the chest. But no evidence indicated leakage related to early diet.
Age and preoperative disorders are also the key factors influencing whether patients can tolerate fast track surgery. Organic functions of patients over 65 years of age are in the degenerating stage. They had intense stress caused by the operation and so their recovery was relatively slow. Fast track surgery would increase their complications and had a disadvantage in early restoration. Patients with preoperative disorders especially heart and lung diseases might fail in the fast-tracking protocol. So it is suggested that the primary diseases should be ameliorated actively and cardiac-pulmonary functions should improve before operation. If organ disorders and nutrition status achieve good improvement, patients can accept fast track surgery mode.
Our research demonstrated that the majority of patients with esophageal carcinoma can tolerate fast track surgery clinical pathway. Patients less than 65 years or without preoperative diseases have the best effect. Average length of hospital stay has been reduced to 7 d. The major goal of fast track surgery is to control pathophysiological process and improve patients’ prognosis, not only for early discharge, but also for early recovery. Fast track surgery is not only the responsibility of surgeons, it also needs a team that could cooperate effectively. This involves surgeons, anesthestists, dietitians, and nurses[24]. Fast track surgery clinical pathway increases patients’ satisfaction and reduce costs. It can also use medical resources in the most efficient way. As a result, fast track surgery will be the tendency of surgery development.
The first author appreciate the help of his wife for her careful proofreading of the manuscript.
A new surgical model, fast track surgery, has appeared recently. Many clinical therapeutic modes have been significantly changed due to fast track surgery. However, the mechanism of this treatment in esophageal tumor resection is still unclear.
To date, few existing data can prove whether such concept in fast track surgery could be safely applied to esophageal surgery such as esophageal tumor resection. This study reviews the outcome of a single-center survey regarding the application of the new “fast-track surgery” clinical pathway and its effects in patients undergoing esophagal tumor resections.
Patients were preoperatively fasted for 8 h only and supplemented with sugar and salt by intravenous infusion 2 h before operation to increase energy. Postoperative patients relied mainly on enteral feedings and were assisted by parenteral alimentation. Nasogastric tube was removed on postoperative day 3 and chest tube was removed on postoperative day 4.
The majority of patients with esophageal carcinoma can tolerate fast track surgery clinical pathway. Patients less than 65 years of age or without preoperative diseases have the best effect in the treatment.
FTS stands for fast-track surgery, a combination of various new techniques which reduce the stress response as well as morbidity and mortality rates, thus greatly shortening the time required for full recovery.
Several articles have evaluated fast-tracking pathways. The primary objective of this study was to determine if fast-tracking pathway can be applied with satisfaction without increasing morbidity or mortality as compared to other reports. The initial observation is interesting.
| 2. | Kehlet H, Wilmore DW. Multimodal strategies to improve surgical outcome. Am J Surg. 2002;183:630-641. |
| 3. | Kehlet H, Dahl JB. Anaesthesia, surgery, and challenges in postoperative recovery. Lancet. 2003;362:1921-1928. |
| 4. | Cerfolio RJ, Bryant AS, Bass CS, Alexander JR, Bartolucci AA. Fast tracking after Ivor Lewis esophagogastrectomy. Chest. 2004;126:1187-1194. |
| 5. | Korst RJ, Rusch VW, Venkatraman E, Bains MS, Burt ME, Downey RJ, Ginsberg RJ. Proposed revision of the staging classification for esophageal cancer. J Thorac Cardiovasc Surg. 1998;115:660-669; discussion 669-670. |
| 6. | Low DE, Kunz S, Schembre D, Otero H, Malpass T, Hsi A, Song G, Hinke R, Kozarek RA. Esophagectomy--it’s not just about mortality anymore: standardized perioperative clinical pathways improve outcomes in patients with esophageal cancer. J Gastrointest Surg. 2007;11:1395-1402; discussion 1402. |
| 7. | Goan YG, Chang HC, Hsu HK, Chou YP. An audit of surgical outcomes of esophageal squamous cell carcinoma. Eur J Cardiothorac Surg. 2007;31:536-544. |
| 8. | Ancona E, Cagol M, Epifani M, Cavallin F, Zaninotto G, Castoro C, Alfieri R, Ruol A. Surgical complications do not affect longterm survival after esophagectomy for carcinoma of the thoracic esophagus and cardia. J Am Coll Surg. 2006;203:661-669. |
| 9. | Atkins BZ, Shah AS, Hutcheson KA, Mangum JH, Pappas TN, Harpole DH Jr, D’Amico TA. Reducing hospital morbidity and mortality following esophagectomy. Ann Thorac Surg. 2004;78:1170-1176; discussion 1170-1176. |
| 10. | Basse L, Hjort Jakobsen D, Billesbolle P, Werner M, Kehlet H. A clinical pathway to accelerate recovery after colonic resection. Ann Surg. 2000;232:51-57. |
| 11. | Basse L, Jacobsen DH, Billesbolle P, Kehlet H. Colostomy closure after Hartmann’s procedure with fast-track rehabilitation. Dis Colon Rectum. 2002;45:1661-1664. |
| 12. | Basse L, Jakobsen DH, Bardram L, Billesbolle P, Lund C, Mogensen T, Rosenberg J, Kehlet H. Functional recovery after open versus laparoscopic colonic resection: a randomized, blinded study. Ann Surg. 2005;241:416-423. |
| 13. | Wilmore DW. From Cuthbertson to fast-track surgery: 70 years of progress in reducing stress in surgical patients. Ann Surg. 2002;236:643-648. |
| 14. | Cutillo G, Maneschi F, Franchi M, Giannice R, Scambia G, Benedetti-Panici P. Early feeding compared with nasogastric decompression after major oncologic gynecologic surgery: a randomized study. Obstet Gynecol. 1999;93:41-45. |
| 15. | Koukouras D, Mastronikolis NS, Tzoracoleftherakis E, Angelopoulou E, Kalfarentzos F, Androulakis J. The role of nasogastric tube after elective abdominal surgery. Clin Ter. 2001;152:241-244. |
| 16. | Nelson R, Tse B, Edwards S. Systematic review of prophylactic nasogastric decompression after abdominal operations. Br J Surg. 2005;92:673-680. |
| 17. | Lanuti M, de Delva PE, Maher A, Wright CD, Gaissert HA, Wain JC, Donahue DM, Mathisen DJ. Feasibility and outcomes of an early extubation policy after esophagectomy. Ann Thorac Surg. 2006;82:2037-2041. |
| 18. | Brandstrup B. Fluid therapy for the surgical patient. Best Pract Res Clin Anaesthesiol. 2006;20:265-283. |
| 19. | Brandstrup B, Tonnesen H, Beier-Holgersen R, Hjortso E, Ording H, Lindorff-Larsen K, Rasmussen MS, Lanng C, Wallin L, Iversen LH. Effects of intravenous fluid restriction on postoperative complications: comparison of two perioperative fluid regimens: a randomized assessor-blinded multicenter trial. Ann Surg. 2003;238:641-648. |
| 20. | Heys SD, Walker LG, Smith I, Eremin O. Enteral nutritional supplementation with key nutrients in patients with critical illness and cancer: a meta-analysis of randomized controlled clinical trials. Ann Surg. 1999;229:467-477. |
| 21. | Mangesi L, Hofmeyr GJ. Early compared with delayed oral fluids and food after caesarean section. Cochrane Database Syst Rev. 2002;229:CD003516. |
| 22. | Johnson Casto C, Krammer J, Drake J. Postoperative feeding: a clinical review. Obstet Gynecol Surv. 2000;55:571-573. |
| 23. | Pettigrew RA, Hill GL. Indicators of surgical risk and clinical judgement. Br J Surg. 1986;73:47-51. |
| 24. | Kehlet H. Future perspectives and research initiatives in fast-track surgery. Langenbecks Arch Surg. 2006;391:495-498. |