Copyright
©The Author(s) 2020.
World J Gastroenterol. Oct 7, 2020; 26(37): 5561-5596
Published online Oct 7, 2020. doi: 10.3748/wjg.v26.i37.5561
Published online Oct 7, 2020. doi: 10.3748/wjg.v26.i37.5561
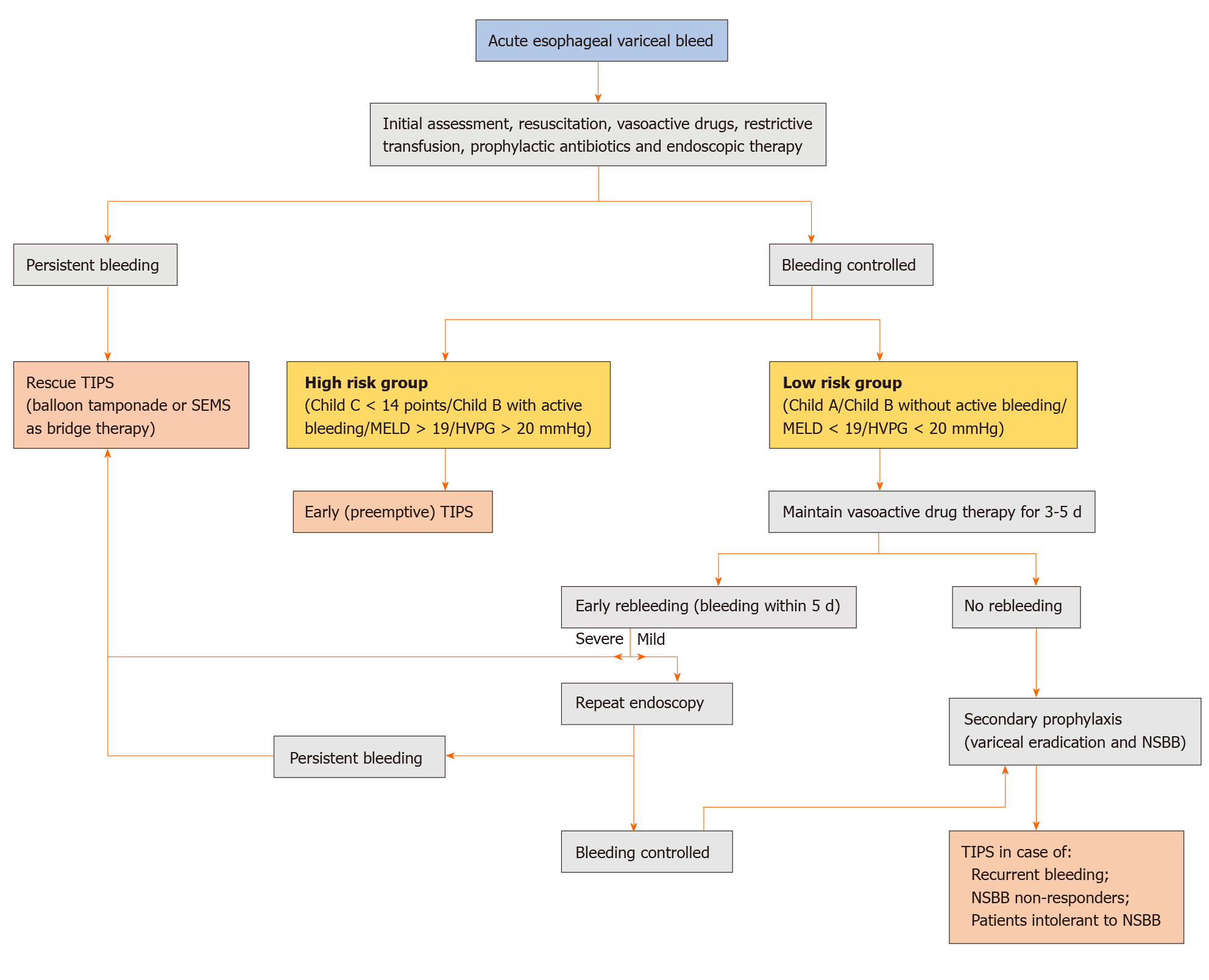
Figure 1 Proposed algorithm for the management of index acute esophageal variceal hemorrhage.
Mild rebleeding is defined as clinical symptoms of bleeding only while severe rebleeding is bleeding associated with hemodynamic compromise or requirement of blood transfusion. TIPS: Transjugular intrahepatic portosystemic shunt; SEMS: Self-expandable metal stents; MELD: Model for end-stage liver disease; HVPG: Hepatic venous pressure gradient; NSBB: Non-selective beta-blockers.
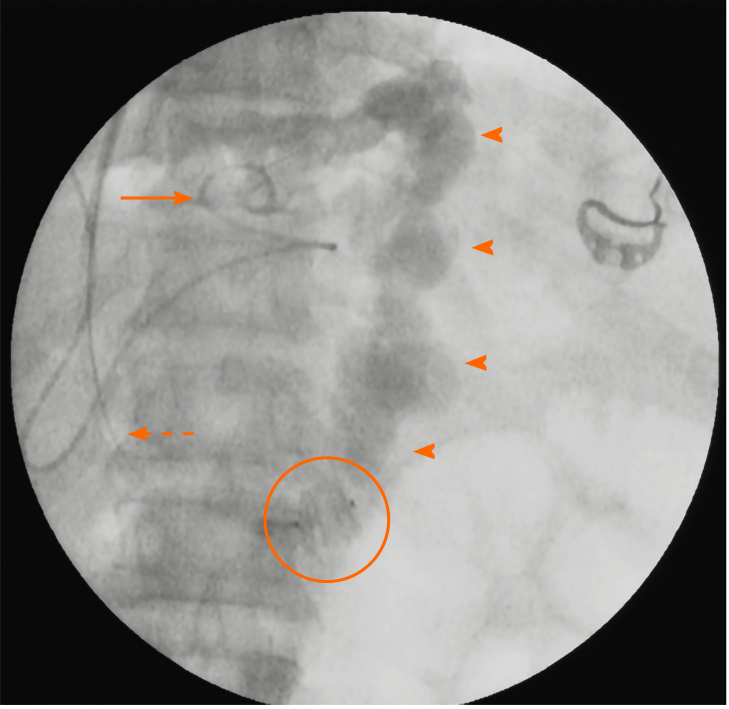
Figure 2 Fluoroscopic spot image demonstrating the “combined approach” to management of a patient with intractable gastric variceal bleeding due to IGV1 and severely attenuated portal vein.
A type-II amplatzer vascular plug (encircled) has been deployed within the gastrorenal shunt retrogradely through the jugular route with vascular access sheath (dashed arrow) in situ. Subsequently, a catheter (solid arrow) was used to inject the sclerosant mixture into the shunt (arrowheads) antegrade through the transjugular intrahepatic route. The transjugular intrahepatic portosystemic shunt stent was then placed in the usual way within the intrahepatic tract after ensuring stasis of sclerosant mixture within the shunt and detachment of the vascular plug.
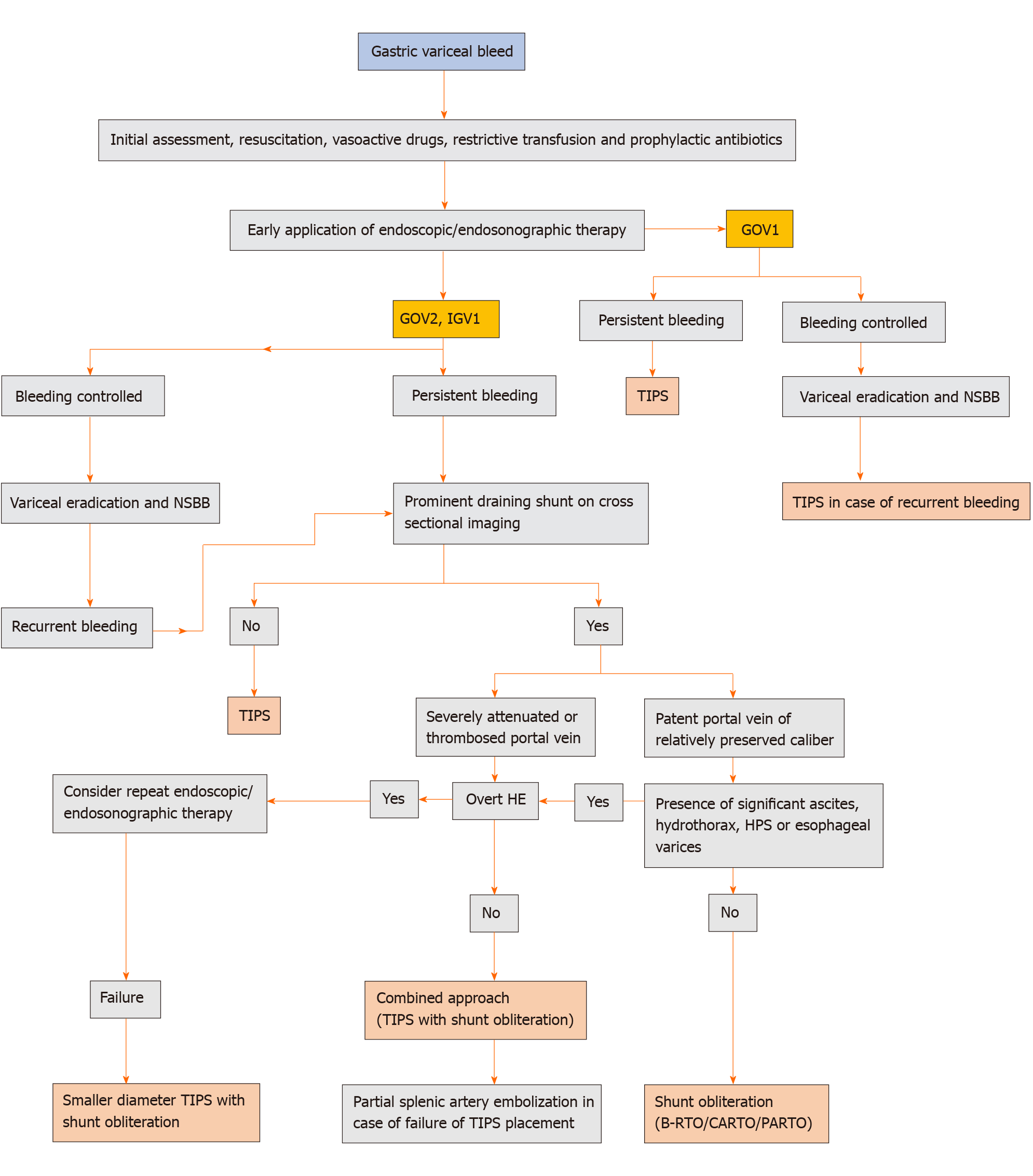
Figure 3 Proposed algorithm for the management of acute gastric variceal hemorrhage.
TIPS: Transjugular intrahepatic portosystemic shunt; NSBB: Non-selective beta-blockers; HE: Hepatic encephalopathy; HPS: Hepatopulmonary syndrome; B-RTO: Balloon-occluded retrograde transvenous obliteration; CARTO: Coil-assisted retrograde transvenous obliteration; PARTO: Plug-assisted retrograde transvenous obliteration.
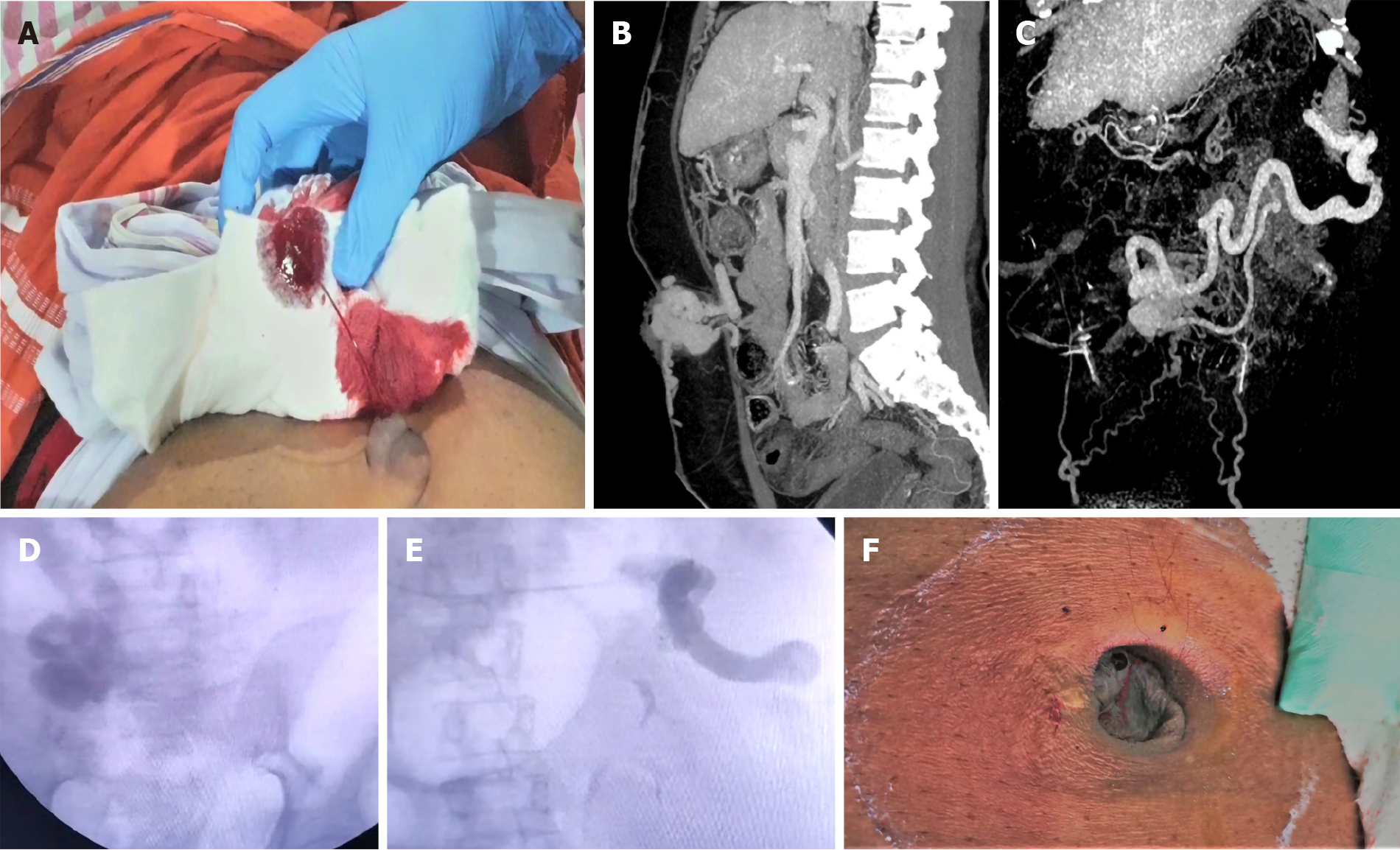
Figure 4 Ectopic umbilical variceal bleeding controlled using TIPS procedure and adjuvant percutaneous intravariceal glue injection.
A: The patient with cirrhosis and portal hypertension presented with spontaneous blood soakage of clothes associated with painless spurting of blood from umbilical region; B: Contrast imaging of abdomen revealed large umbilical varix with extracutaneous component; C: The umbilical varix supply was from the splenic vein; D and E: Fluroscopy guided transjugular intrahepatic portosystemc shunt placement, shunt embolization with multiple coils followed by percutaneous glue injection for variceal obliteration was performed; F: Complete resolution of the variceal complex was noted clinically post transjugular intrahepatic portosystemc shunt procedure.
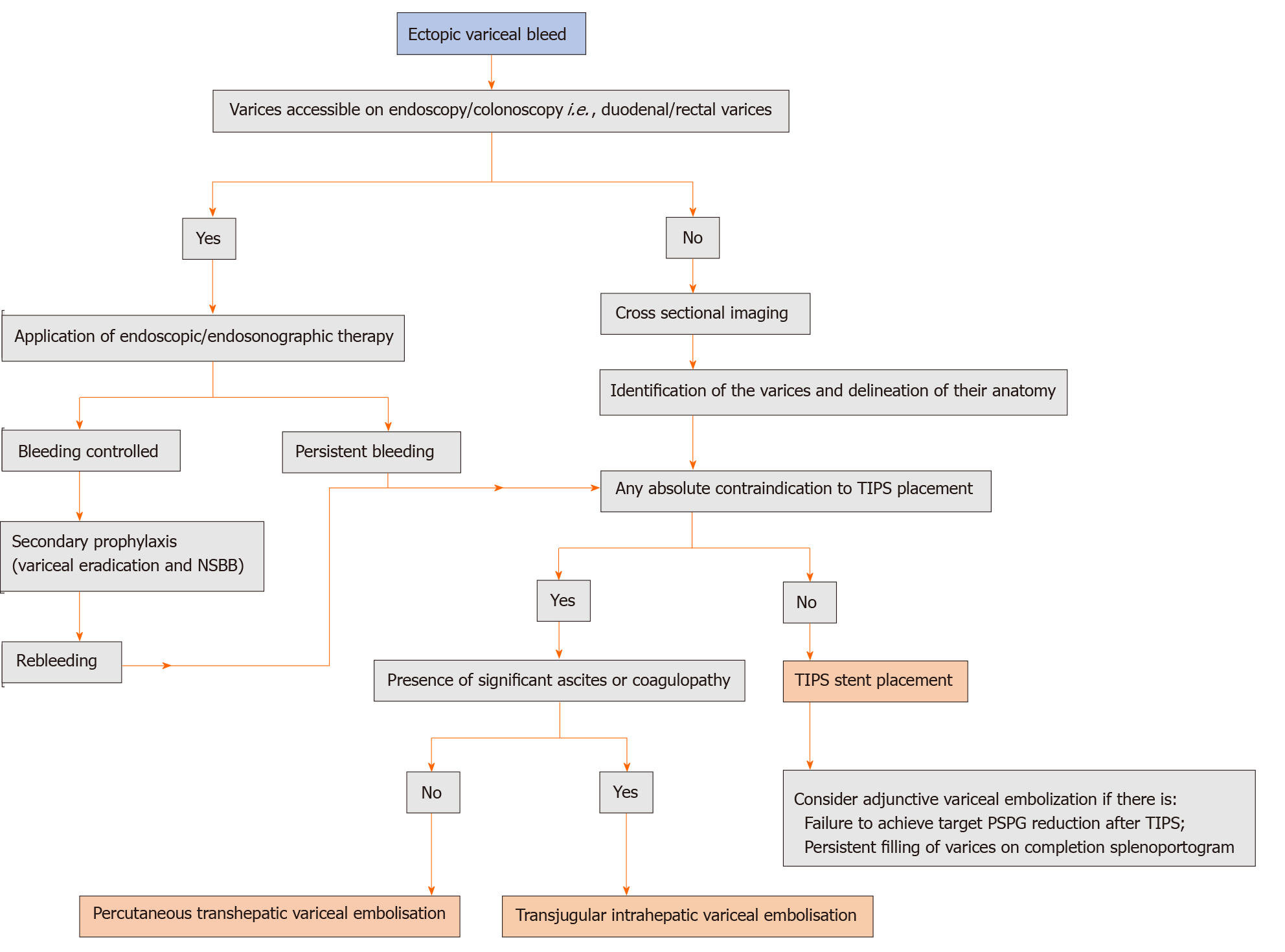
Figure 5 Proposed algorithm for the management of ectopic variceal bleeding.
NSBB: Non-selective beta-blockers; TIPS: Transjugular intrahepatic portosystemic shunt; PSPG: Portosystemic gradient.
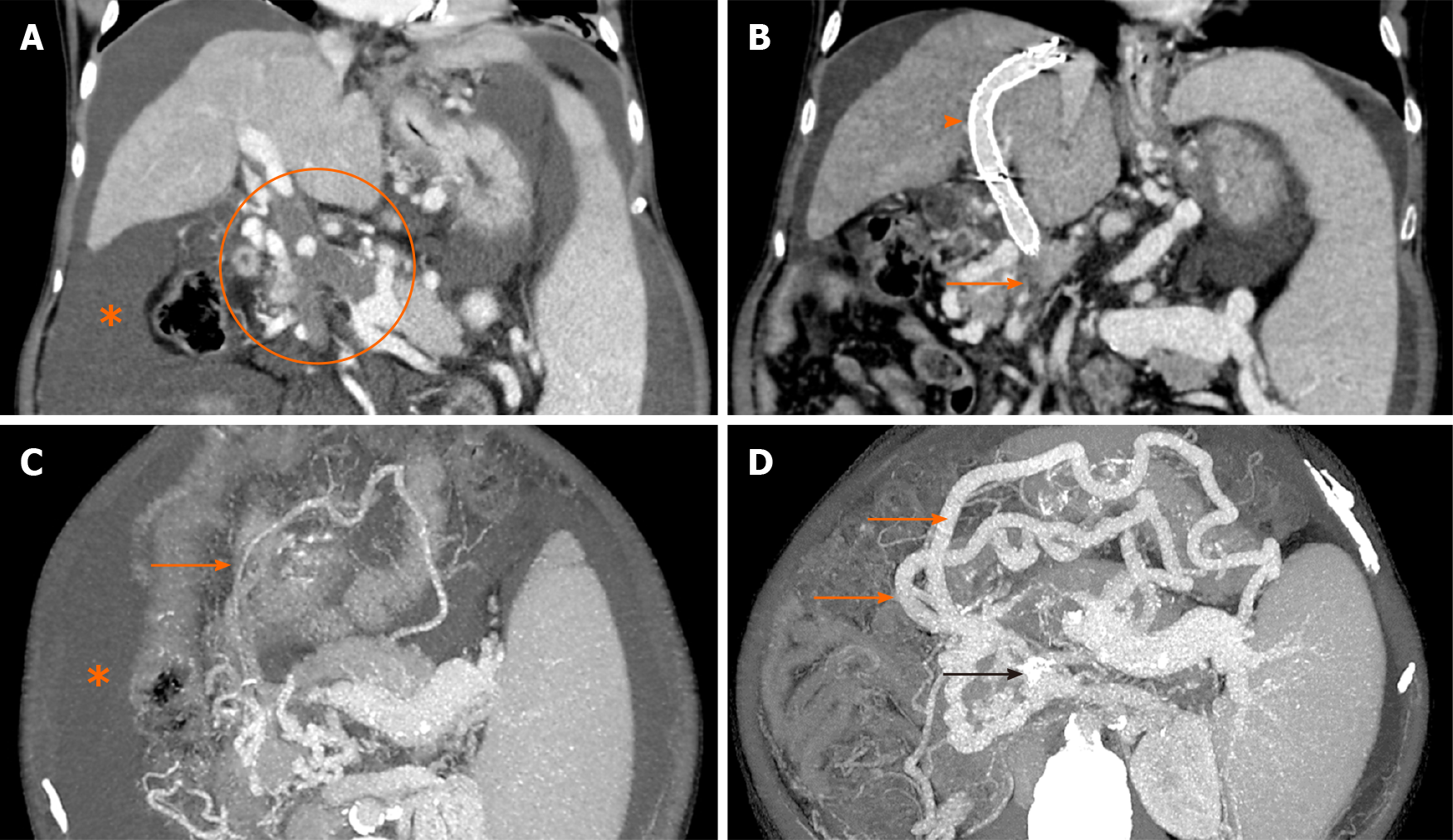
Figure 6 Contrast-enhanced computed tomography image.
A: Coronal image showing bland occlusive thrombus involving the main portal vein, superior mesenteric vein (SMV) and splenic vein (encircled) with gross ascites (asterisk); B: Image taken 2 wk after transjugular intrahepatic portosystemic shunt (TIPS) shows the stent in situ (arrowhead) with its distal end in one of the major tributaries of SMV. The main trunk of SMV (solid arrow) and splenic vein could not be fully recanalized during TIPS. Trans-splenic access was not taken due to gross ascites; C and D: Corresponding axial images show marked enlargement of the gastroepiploic collaterals (solid orange arrows) arising from the patent portion of splenic vein at splenic hilum draining through the TIPS stent (black arrow in D) into the portal venous system. Note the significant regression of ascites on the follow up scans.
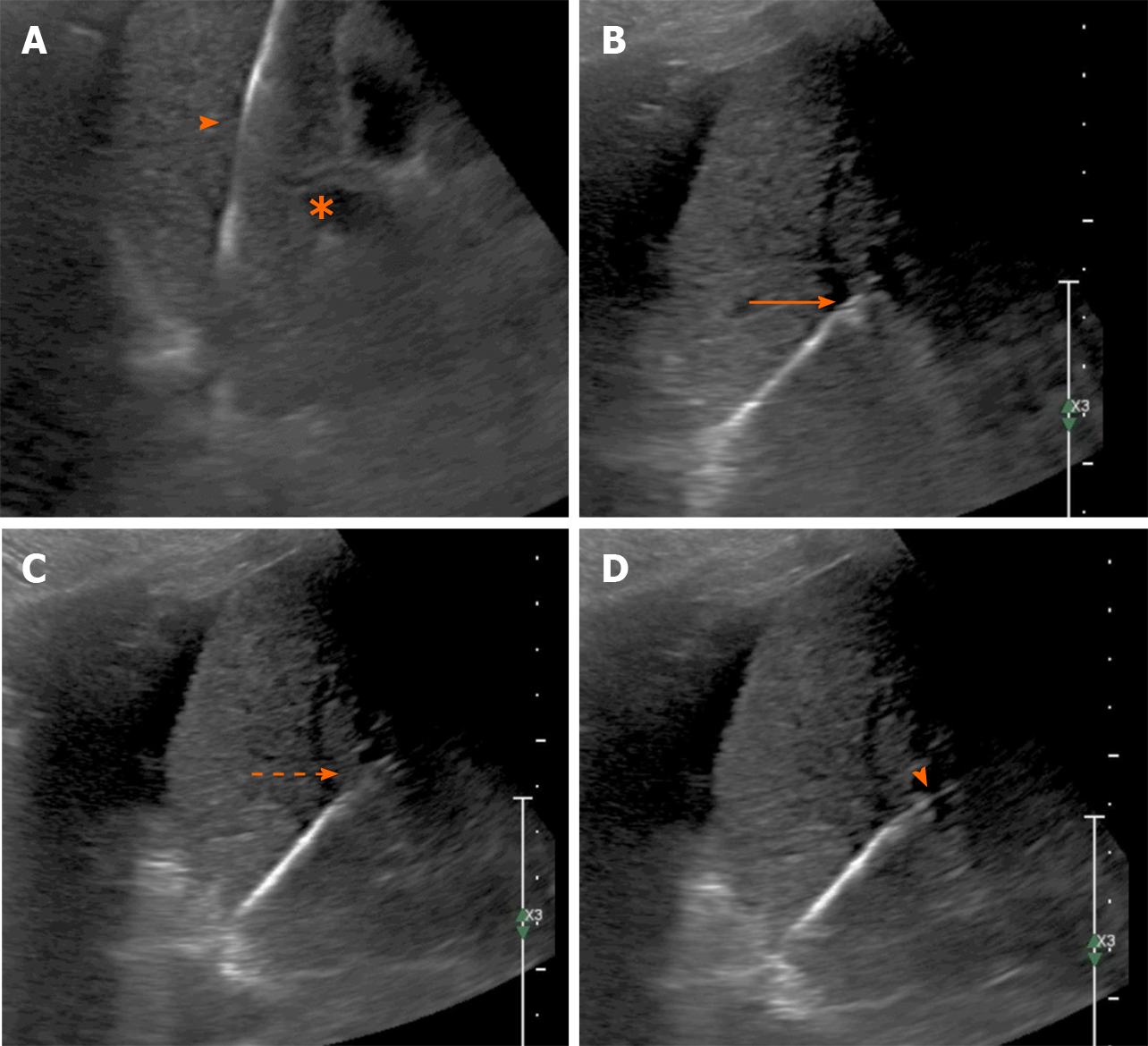
Figure 7 Ultrasound image.
A: Gray scale ultrasound image showing the stiff guidewire in the right hepatic vein (arrowhead) with the right portal vein branch in the same image (asterisk); B: The needle-catheter combination advancing towards the portal vein branch (arrow); C: Indentation of the needle (arrow); D: The needle is seen entering the portal vein (arrowhead).
- Citation: Rajesh S, George T, Philips CA, Ahamed R, Kumbar S, Mohan N, Mohanan M, Augustine P. Transjugular intrahepatic portosystemic shunt in cirrhosis: An exhaustive critical update. World J Gastroenterol 2020; 26(37): 5561-5596
- URL: https://www.wjgnet.com/1007-9327/full/v26/i37/5561.htm
- DOI: https://dx.doi.org/10.3748/wjg.v26.i37.5561