Copyright
©The Author(s) 2020.
World J Gastroenterol. Aug 7, 2020; 26(29): 4218-4239
Published online Aug 7, 2020. doi: 10.3748/wjg.v26.i29.4218
Published online Aug 7, 2020. doi: 10.3748/wjg.v26.i29.4218
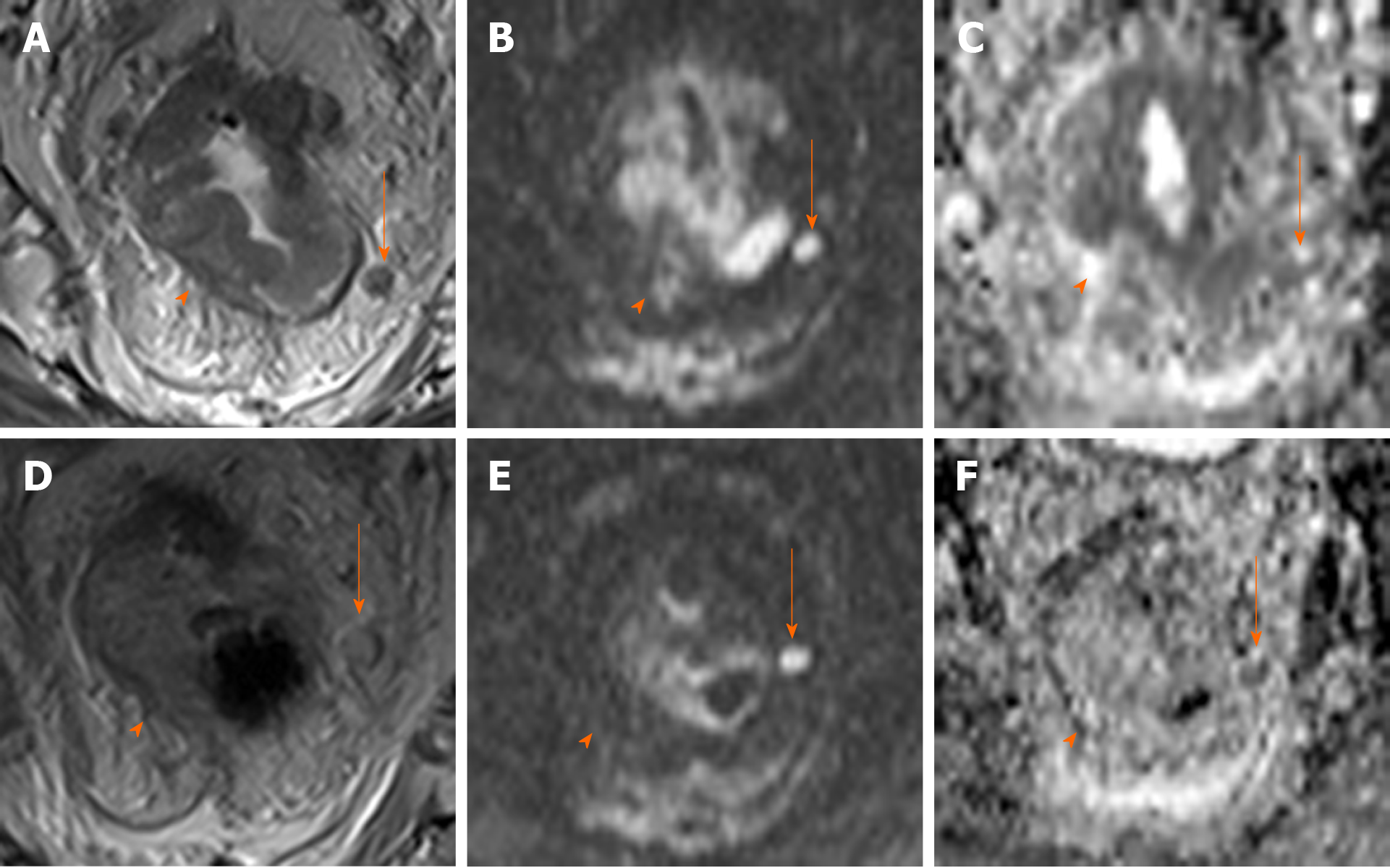
Figure 1 Discrepancies in magnetic resonance sequences in follow-up imaging after neoadjuvant therapy.
Magnetic resonance imaging (MRI) of the rectum for initial staging (upper row): High-resolution T2 sequences (A), high b value diffusion-weighted imaging (DWI) (B) and apparent diffusion coefficient (ADC) map (C). Protuberant wall thickening (arrow) with an adjacent enlarged, heterogeneous lymph node (arrow); signs of restricted diffusion are observed in both sequences (hyperintensity in DWI and hypointensity in ADC). MRI after neoadjuvant treatment in the same patient (bottom row) reveals near complete resolution of the main mass on the various imaging sequences. In the affected node, fewer morphological alterations are visible, but with no decrease in size (D) and with signs of restricted diffusion (E and F), suggesting persistent malignancy. No evidence of nodal malignancy is evidenced on the histological analysis of the surgical specimen.
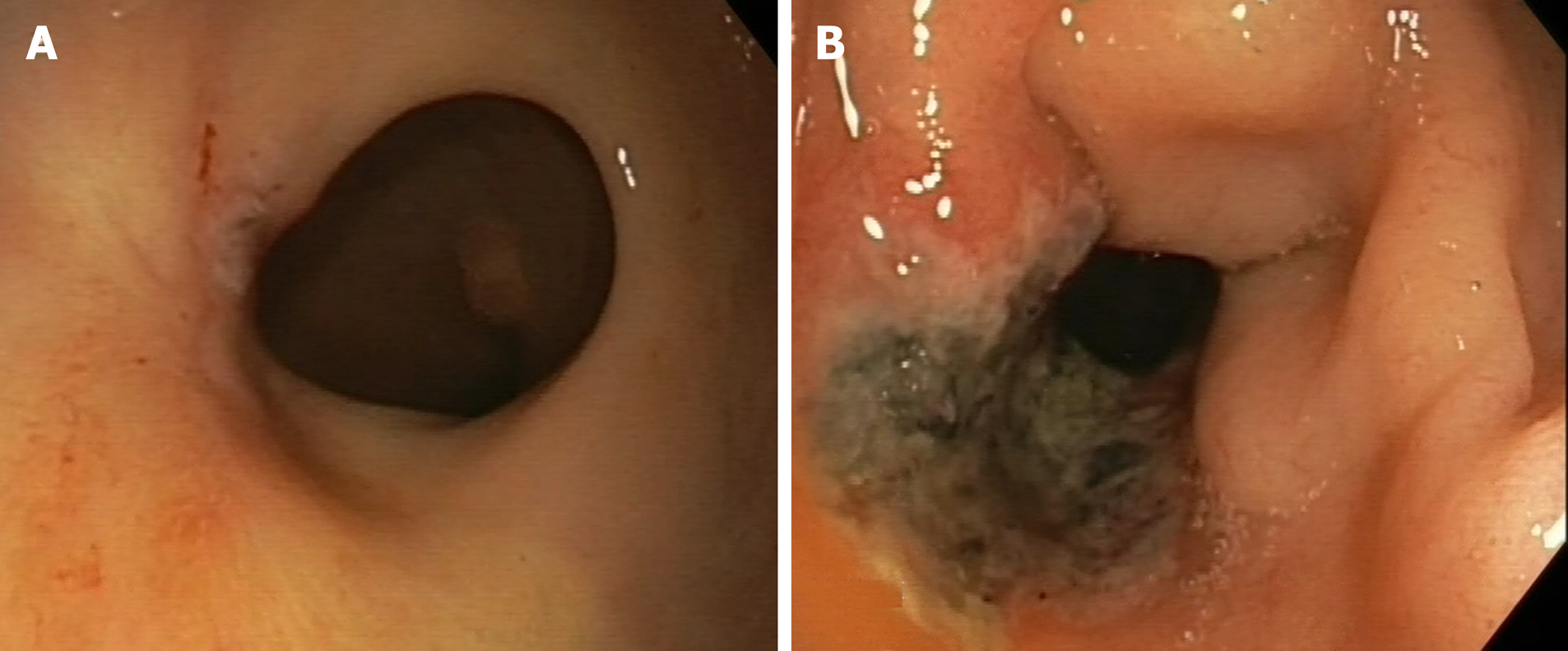
Figure 2 Clinical incomplete response.
A: Endoscopic evaluation after 9 wk of chemoradiotherapy completion, detecting a small, but irregular, residual ulcer. B: Regrowth is more evident 12 wk later, as a deep, irregular and necrotic ulcer.
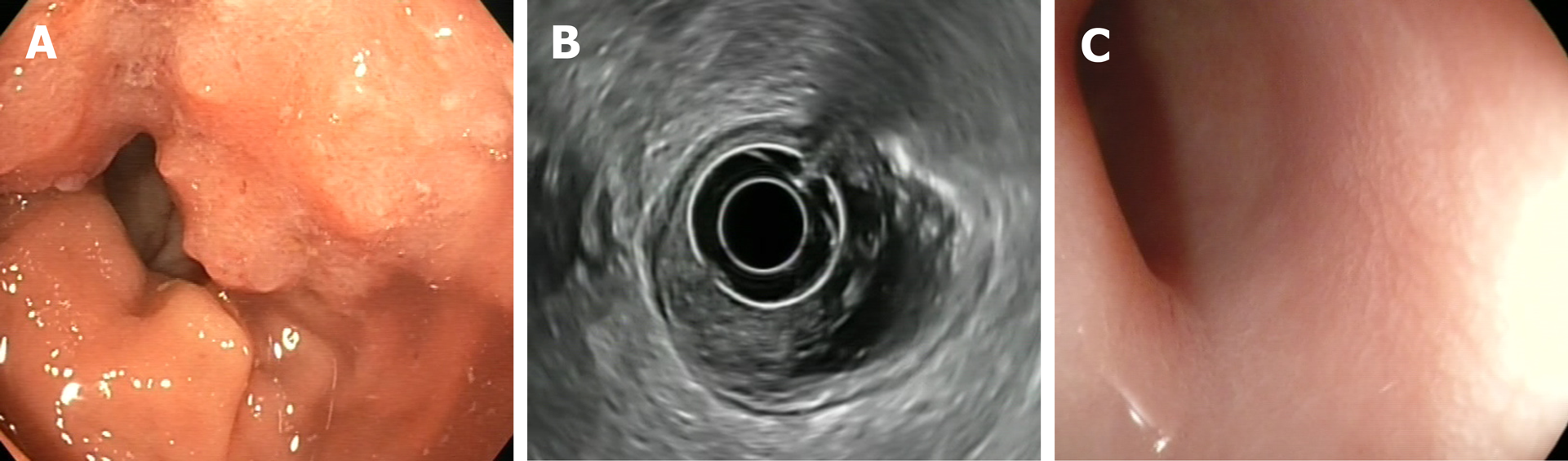
Figure 3 Clinical complete response.
A: Endoscopic view of a rectal tumor prior to the neoadjuvant chemoradiotherapy; B: Endoscopic ultrasound with radial probe, showing that the tumor (T) is located within the mucosa, submucosa and muscular layers (uT2N0); C: Flat scar 10 wk after treatment completion: An endoscopic response feature.
- Citation: López-Campos F, Martín-Martín M, Fornell-Pérez R, García-Pérez JC, Die-Trill J, Fuentes-Mateos R, López-Durán S, Domínguez-Rullán J, Ferreiro R, Riquelme-Oliveira A, Hervás-Morón A, Couñago F. Watch and wait approach in rectal cancer: Current controversies and future directions. World J Gastroenterol 2020; 26(29): 4218-4239
- URL: https://www.wjgnet.com/1007-9327/full/v26/i29/4218.htm
- DOI: https://dx.doi.org/10.3748/wjg.v26.i29.4218