INTRODUCTION
The concept of natural orifice translumenal endoscopic surgery (NOTES) was introduced in 2004, when Kaloo et al[1] reported a successful transgastric peritoneoscopy performed in an in vivo porcine model. Since then, the variety of NOTES interventions using the porcine survival model has expanded to include splenectomy[2], gastrojejunostomy[3], hysterectomy[4], ligation of fallopian tubes[5], oophorectomy[6,7], cholecystectomy[8], appendectomy[9], hernia repair[10], pancreatectomy[11], and lymphadenectomy[12]. Human trials are currently under way[13].
From the beginning, two of the main scientific endoscopic societies have been involved in assessing and promoting research related to the NOTES procedures, namely the North American Natural Orifice Surgery Consortium for Assessment and Research (NOSCAR) group[14] and the European EURO-NOTES group[15]. In 2006, NOSCAR published a White Paper outlining twelve critical features that can impact the safety of NOTES to guide its appropriate usage and highlighted the need for increased research and analysis of data[16]. Gastric (intestinal) closure was designated as a very important area of research, and the group mandated a strict objective of the NOTES procedure to achieve closure with absolutely no leaks.
To date, the reported closure methods for the various NOTES interventions have used dedicated suture and anchor tools[17], such as T tags[18], purse string-modified T tags[19], Eagle Claw VIII[20], flexible endoscopic stapler[21], purse string suturing device[22], and flexible Endostitch[17]. All of these devices are cumbersome and have not yet received approval for use in clinical settings.
Therefore, this study was designed to investigate the feasibility of performing a surgical suture of a stomach opening by using common endoscopy devices.
MATERIALS AND METHODS
A modified version of the in vitro porcine stomach model described by Hon et al[23] was used. Briefly, a trocar with radiolucent sleeve and 10-15 mm seal (Versaport Plus; Tyco Healthcare, Gosport, United Kingdom) was fixed onto a plastic rectangular box. A fresh pig stomach was tightly attached to the trocar on the inner side of the box via the esophageal opening. The duodenum was closed with a pair of Kocher forceps (Figure 1A). A standard gastroscope (GIF 160; Olympus, Rungis, France) fitted with a transparent straight plastic cap was inserted through the trocar (emulating passage through the esophagus) into the lumen of the stomach. The lumen was inflated and the procedure was performed as detailed in the Results.
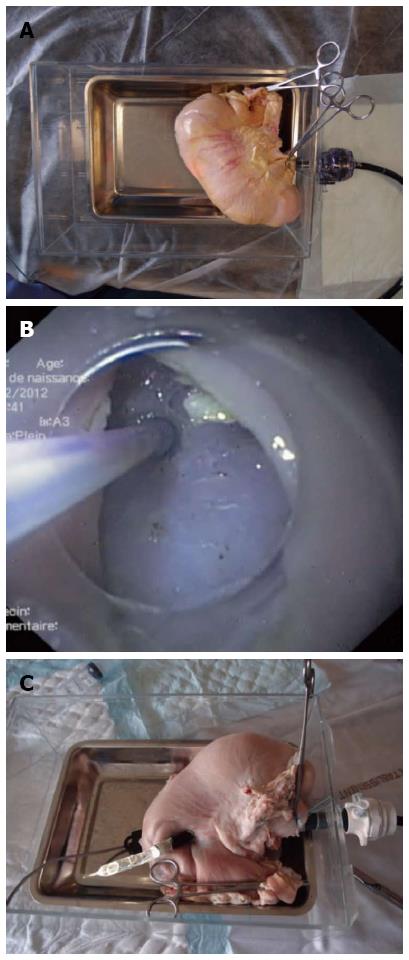
Figure 1 Endoscope.
A: The “in vitro” pig stomach model with the endoscope in place; B: View over muscularis propria from the gastric lumen in the submucosal space created by endoscopic submucosal dissection. Muscularis propria is about to be punctured (“peritoneoscopy”); C: Endoscope outside of the stomach simulating peritoneoscopy, with the dilated balloon in the working channel.
RESULTS
The gastroscope-assisted knotting procedure was carried out with the following nine steps: (1) A 20 mm gastric submucosal bleb was created by injecting saline (25G 1-JectS; ABS Bolton Medical, Saint Michel/Meurthe, France) into the anterior inner face of the stomach, near the angle. A 15 mm linear incision was then made at the top of the submucosal elevation using a Dual Knife (KD650U; Olympus) coupled with a standard electrosurgical unit (Erbotom ICC200; ERBE, Tübingen, Germany); (2) The submucosal space was dissected at about 10 mm on both sides of the incision by introducing the cap-fitted endoscope inside the submucosal space (Figure 1B); (3) Peritoneoscopy was performed by the standard technique[1]. First, the Dual Knife was used to puncture the muscular layer from the submucosal space into the middle of the initial incision. A 0.025” guidewire (Jagwire/450 cm; Boston Scientific, Nanterre, France) was introduced into this orifice, followed by a 10 mm dilating balloon (Quantum TT; Cook Medical, Charenton le Pont, France) that was inflated to facilitate the scope’s passage out of the stomach (Figure 1C). Finally, the balloon was deflated and the scope was retracted into the stomach; (4) On one incision side, a puncture was made in the mucosa from the submucosal space towards the lumen. A guiding catheter (HGC-6; Cook Medical) was introduced into this puncture to facilitate introduction of a 0.025” guidewire on the luminal side of the mucosa, traversing into the gastric lumen (Figure 2A); (5) After creating several loops in the stomach with the guidewire from Step (4), the endoscope was withdrawn, leaving the guidewire in place, and then reintroduced near it. The guidewire’s distal end was captured with forceps (Radial Jaw; Boston Scientific) and pulled outside of the stomach (Figure 2B). Both ends of the guidewire were now outside the stomach, with the guidewire passing through an orifice from the submucosal space into the gastric lumen; (6) A 120 cm 4-0 surgical suture (Prolene; Ethicon, Issy les Moulineaux, France) was tied to one end of the guidewire. The other end of the guidewire was then pulled out, effectively dragging the surgical wire into the previously occupied position. The extracted guidewire was detached from the in-place surgical wire; (7) Steps (4), (5), and (6) were repeated on the second incision side, with minor modification. At step (6), the submucosal end of the guidewire was tied outside the stomach, with the submucosal end of the surgical wire remaining in place on the first incision side. The guidewire was again pulled out, so that the surgical wire passed through both sides of the submucosal incision (Figure 2C); (8) A single loop had formed on the outside, and one wire end was fixed into place. Biopsy forceps were used to pull the other end through the working channel of the endoscope, simultaneously introducing the endoscope into the stomach and pushing the loop with the endoscope tip towards the incision line (Figure 2D). In this manner, the incision mucosal sides were brought towards one another as the loop was tightened. Three alternating loops were made to form the final surgical knot; and (9) The wire ends were cut with a reusable loop cutter (FS-5Q-1; Olympus) (Figure 2E). A photograph of the completed surgical knot is shown in Figure 2F.
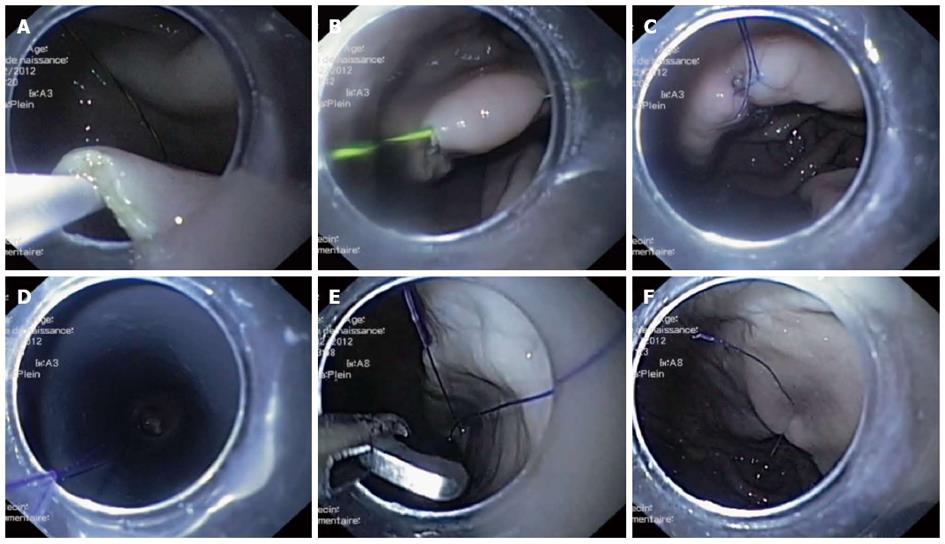
Figure 2 Natural orifice translumenal endoscopic surgery.
A: Puncture of the mucosa from the submucosal space on the right side of the incision and passing a guidewire into the gastric lumen; B: The guidewire traverses the mucosa on the right side of the incision, both ends are outside; C: Surgical wire replaces the guidewire first on the right side, then is passed through both sides after replacing the guidewire on the left side; D: A loop formed outside is pushed with the endoscope (here at the rim of the transparent cap) at the mucosal incision so as to tighten the knot; E Cutting the wire ends; F: The final aspect of the surgical knot.
DISCUSSION
The aim of this study was purely theoretical, by which we sought to prove that a surgical suture may be created using only commonplace endoscopy suite materials, without metallic clips, to close a hole in the wall of a hollow digestive organ. As such, the study has several important limitations.
Since the study was based on an in vitro model, neither the strength of the suture, its resistance nor tightness was evaluated. Moreover, other treatment-related quality parameters, such as infection rate and histological response, were not evaluated. Although infectious complications may be prevented in the in vivo model by antibiotic lavage of the stomach before gastric NOTES procedures[24]. Another limitation is that only a single knot was used to close a 15 mm incision, which would be insufficient for a surgical closure. We speculate that two or more suture wires may be passed through both incision sides and tightened at the end, so as to form two or more surgical knots and increase the fidelity of the closure. However, this may prove unfeasible since surgical wires could tangle or form spontaneous knots inside the stomach, beyond the operator’s control.
Nonetheless, the endoscopic method does have an important safety advantage. The endoscopic surgical suturing reduces the risk of injury to organs adjacent to the stomach, which is a significant concern when using T-tags[25]. The method itself may also prove useful as a feasibility model for future development of safer suturing devices that work within a previously dissected submucosal space. In fact, some researchers have already attempted to investigate the utility and safety of an artificially generated submucosal tunnel, but the mucosal incision site had been closed with metallic clips[26]. Testing of this method in an in vivo animal model is necessary to better understand not only its clinical significance with NOTES interventions but also to help realize its potential for other applications.
ACKNOWLEDGMENTS
The authors would like to thank the endoscopy nurses Virginie Dispard, Alice Gâla and Cezarina Vasile.
COMMENTS
Background
Traditionally, surgery has been the only method available for removing pathological tissue from the inner abdomen. Laparoscopic surgery and digestive endoscopy have made diagnostic and therapeutic procedures less invasive. Laparoscopic surgery requires creation of orifices in the abdominal wall to access the peritoneal space, while digestive endoscopy travels along and is confined to the digestive tract. In the last 10 years, however, the natural orifice translumenal endoscopic surgery (NOTES) approach passed the endoscope into the peritoneal cavity through a created orifice in the wall of the digestive tract.
Research frontiers
The NOTES approach has not yet been fully developed. Questions remain about how to prevent peritoneal infection, how to accurately stabilize the endoscope in the peritoneal cavity and obtain a good grip and orientation (triangulation), and how to finally close the parietal access point. The simplest way to close the orifice is to use endoscopic metallic clips, which are already used for closing accidental perforations, for hemostasis, or for marking. More elaborate methods have been proposed, including endoscopic suture machines and staplers, or trans-parietal metallic tags tightened together. Yet, these methods are complicated, costly, high risk, and not approved for clinical practice.
Innovations and breakthroughs
The authors have described a method to close the digestive wall orifice with a surgical knot using only common endoscopy suite materials. This approach avoids the use of additional devices and reproduces the gold standard surgical closure method-the surgical knot.
Applications
The method may be used as a model for creating simple suturing devices that work within the submucosal space. It must first be validated by in vivo survival animal experiments.
Terminology
NOTES: Natural orifice translumenal endoscopic surgery, a method to perform abdominal surgery by entering the peritoneal space through small orifices made into hollow organs (i.e., stomach, colon, vagina, urinary bladder).
Peer review
The case is interesting and extremely rare. It is well written and is describing a new method of endoscopic suture. It can be accepted for publication an intra operative image during laparotomy would be of added value.
P- Reviewers Rotondano G, Akyuz F, Iglesias-Garcia J S- Editor Song XX L- Editor A E- Editor Zhang DN